Preventive PCI for High-Risk Coronary Plaques Reduces Cardiac Events
Posted on 09 Apr 2024
Plaques building up in the heart’s arteries that comprise fats, cholesterol, and other substances, can lead to heart attacks and serious cardiac events if they break off and travel through the blood vessel to cause a blockage. Percutaneous coronary intervention (PCI) is used to open blocked arteries for treating myocardial ischemia, a condition where the heart muscle fails to receive enough oxygenated blood. During PCI, a stent is inserted through a catheter into the blocked artery from the groin or arm, which not only keeps the artery open for blood to flow freely but also releases medications to prevent further plaque buildup. The concept of preventive PCI is based on the view that a stent could stabilize high-risk plaque lesions, thus lowering the chance of rupture and a potential heart attack. Now, a new study has found that individuals with a buildup of fatty atherosclerotic plaque in the heart’s arteries considered at risk of rupturing can benefit significantly from PCI, reducing the likelihood of severe cardiac events compared to treatment with medication alone.
The findings of the new research presented at the American College of Cardiology’s Annual Scientific Session by the University of Ulsan (Seoul, South Korea) suggest that individuals having high-risk plaques that are likely to rupture stand to benefit from preventive PCI instead of waiting for a heart attack or other serious reduction in blood flow to happen. The PREVENT trial is notably the most extensive study on preventive PCI to date as it focuses on patients with non-symptomatic or non-ischemic blockages that typically wouldn't warrant PCI under current care standards. It is also the first study with a large enough sample size to examine the clinical outcomes of using preventive PCI for treating vulnerable plaques. The trial found that, after two years, participants who underwent preventive PCI had an 89% lower risk of experiencing serious cardiac outcomes such as cardiac death, heart attack in the targeted vessel, revascularization due to ischemia in the target vessel, or hospitalization for unstable or progressive chest pain, compared to those on medication alone.
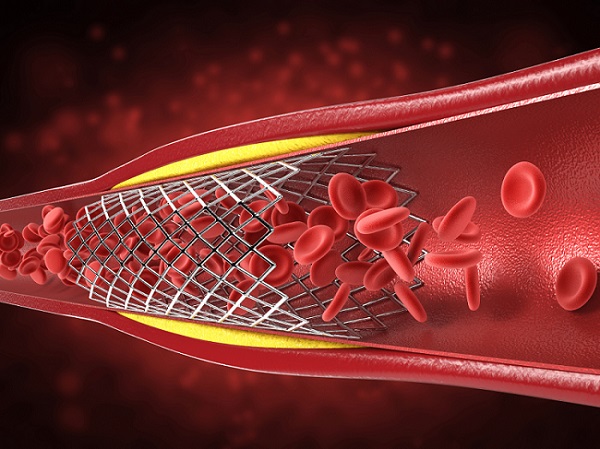
The study involved 1,606 coronary artery disease patients from 15 centers across four countries, all with plaques identified as vulnerable to rupture through intravascular imaging but not significantly obstructing blood flow. Participants, averaging 64 years old, were either assigned to PCI combined with medical therapy or to medical therapy only, which included lifestyle changes and intensive pharmacologic treatment per secondary prevention guidelines, with a strong emphasis on high-dose statin therapy for both groups. Two years into the study, the composite primary endpoint occurred in three patients who underwent PCI (0.4% of the PCI group) and in 27 patients who were administered only medications (3.4% of the controls), marking an 89% lower risk of the composite primary endpoint among those who received PCI. The cumulative incidence of this composite endpoint was found to be significantly lower in the PCI group through long-term follow-up over a median of 4.4 years (maximum up to 7.9 years), with patients receiving PCI demonstrating a 46% lower risk of the composite endpoint across this period. Additionally, the rates for each component of the composite primary endpoint were also found to be lower in the PCI group, in line with the composite rate of death from any cause or heart attack in the target vessel or any revascularization.
“PREVENT has now shown that preventive PCI may reduce the two-year and long-term risks of major cardiac events arising from vessels containing vulnerable plaques,” said Seung-Jung Park, MD, the study’s lead author. “These findings demonstrate that the focal treatment of high-risk vulnerable plaques may improve patient prognosis beyond optimal medical therapy alone.”
Related Links:
University of Ulsan