Tele-ICU Supports Improved Patient Care
|
By HospiMedica International staff writers Posted on 10 Aug 2011 |
A new study shows that using a tele-intensive care unit (tele-ICU) favorably affects hospital mortality, length of stay, best practice adherence, and preventable complications.
Researchers at the University of Massachusetts Medical School (UMMS; Worcester, USA) conducted a prospective pre- and post-study of 6,290 adults admitted to any of 7 ICUs (3 medical, 3 surgical, and 1 mixed cardiovascular) on two campuses of an academic medical center from April 2005 through September 2007. Electronically supported and monitored processes for best practice adherence, care plan creation, and clinician response times to alarms were evaluated. The main outcome measures were case-mix and severity-adjusted hospital mortality; other outcomes included hospital and ICU length of stay, best practice adherence, and complication rates.
The results showed that the hospital mortality rate was 13.6% during the preintervention period, and 11.8% during the tele-ICU period. The tele-ICU intervention period was also associated with higher rates of best clinical practice adherence for cardiovascular protection and prevention of deep vein thrombosis (DVT), stress ulcers, and ventilator-associated pneumonia (VAP), resulting in lower rates of preventable complications. Patients in the tele-ICU period had shorter hospital lengths of stay (9.8 versus 13.3 days), and the results were comparable for medical, surgical, and cardiovascular ICUs.
"It's a very, very, strong clear signal that tele-ICU technology works. Places that are giving pretty good critical care can produce even better critical care with it,” said lead author Craig Lilly, MD, director of the Tele-ICU program at UMMS. “The system leverages technology as well as clinical expertise to provide expert care at 3 am. The problem is, you just can't be there 24/7 because you've got to sleep, and you've got a family.”
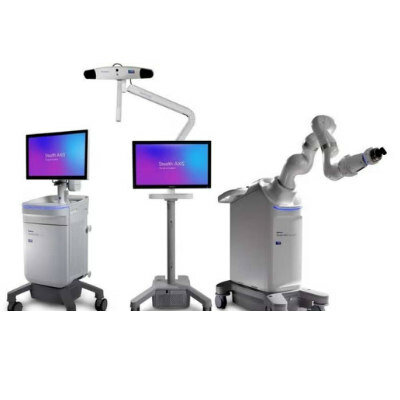
The off-site tele-ICU team, which included an intensivist, had the ability to communicate with bedside clinicians or directly manage patients by recording clinician orders for tests, treatments, consultations, and management of life-support devices. Among the responsibilities of the team were reviewing the care of individual patients; performing real-time audits of best practice adherence; monitoring system-generated electronic alerts; auditing bedside clinician responses to in-room alarms; and intervening when the responses of bedside clinicians were delayed and patients were deemed physiologically unstable.
Related Links:
University of Massachusetts Medical School
Researchers at the University of Massachusetts Medical School (UMMS; Worcester, USA) conducted a prospective pre- and post-study of 6,290 adults admitted to any of 7 ICUs (3 medical, 3 surgical, and 1 mixed cardiovascular) on two campuses of an academic medical center from April 2005 through September 2007. Electronically supported and monitored processes for best practice adherence, care plan creation, and clinician response times to alarms were evaluated. The main outcome measures were case-mix and severity-adjusted hospital mortality; other outcomes included hospital and ICU length of stay, best practice adherence, and complication rates.
The results showed that the hospital mortality rate was 13.6% during the preintervention period, and 11.8% during the tele-ICU period. The tele-ICU intervention period was also associated with higher rates of best clinical practice adherence for cardiovascular protection and prevention of deep vein thrombosis (DVT), stress ulcers, and ventilator-associated pneumonia (VAP), resulting in lower rates of preventable complications. Patients in the tele-ICU period had shorter hospital lengths of stay (9.8 versus 13.3 days), and the results were comparable for medical, surgical, and cardiovascular ICUs.
"It's a very, very, strong clear signal that tele-ICU technology works. Places that are giving pretty good critical care can produce even better critical care with it,” said lead author Craig Lilly, MD, director of the Tele-ICU program at UMMS. “The system leverages technology as well as clinical expertise to provide expert care at 3 am. The problem is, you just can't be there 24/7 because you've got to sleep, and you've got a family.”
The off-site tele-ICU team, which included an intensivist, had the ability to communicate with bedside clinicians or directly manage patients by recording clinician orders for tests, treatments, consultations, and management of life-support devices. Among the responsibilities of the team were reviewing the care of individual patients; performing real-time audits of best practice adherence; monitoring system-generated electronic alerts; auditing bedside clinician responses to in-room alarms; and intervening when the responses of bedside clinicians were delayed and patients were deemed physiologically unstable.
Related Links:
University of Massachusetts Medical School
Latest Health IT News
- AI-Native EHR Achieves EU Medical Device Certification
- EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
- AI System Detects and Quantifies Chronic Subdural Hematoma
- Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
- Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Channels
Artificial Intelligence
view channel
AI Platform Supports Noninvasive Remote Hemodynamic Monitoring in Heart Failure
Heart failure remains a leading cause of hospitalization in adults over 65, affecting more than 6.7 million people in the U.S. Clinicians often lose visibility into hemodynamic deterioration once patients... Read more
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read moreCritical Care
view channel
Smartphone Heart Rhythm App Reduces Unnecessary Cardioversion Procedures
Atrial fibrillation, an irregular and often rapid heart rhythm, is the most common arrhythmia in adults. Elective electrical cardioversion is frequently canceled on the day of treatment when patients revert... Read more
New Practice Guidance Supports Prostatic Artery Embolization for BPH Symptoms
Benign prostatic hyperplasia is a noncancerous enlargement of the prostate that can cause lower urinary tract symptoms and impair daily functioning. These symptoms erode sleep, productivity, and sexual... Read more
Bedside CSF Monitor Detects Early Infection in Fluid Drains
External drainage of cerebrospinal fluid (CSF) after traumatic brain injury, hydrocephalus, or hemorrhage carries a significant risk of infection. These infections can prolong intensive care, cause severe... Read more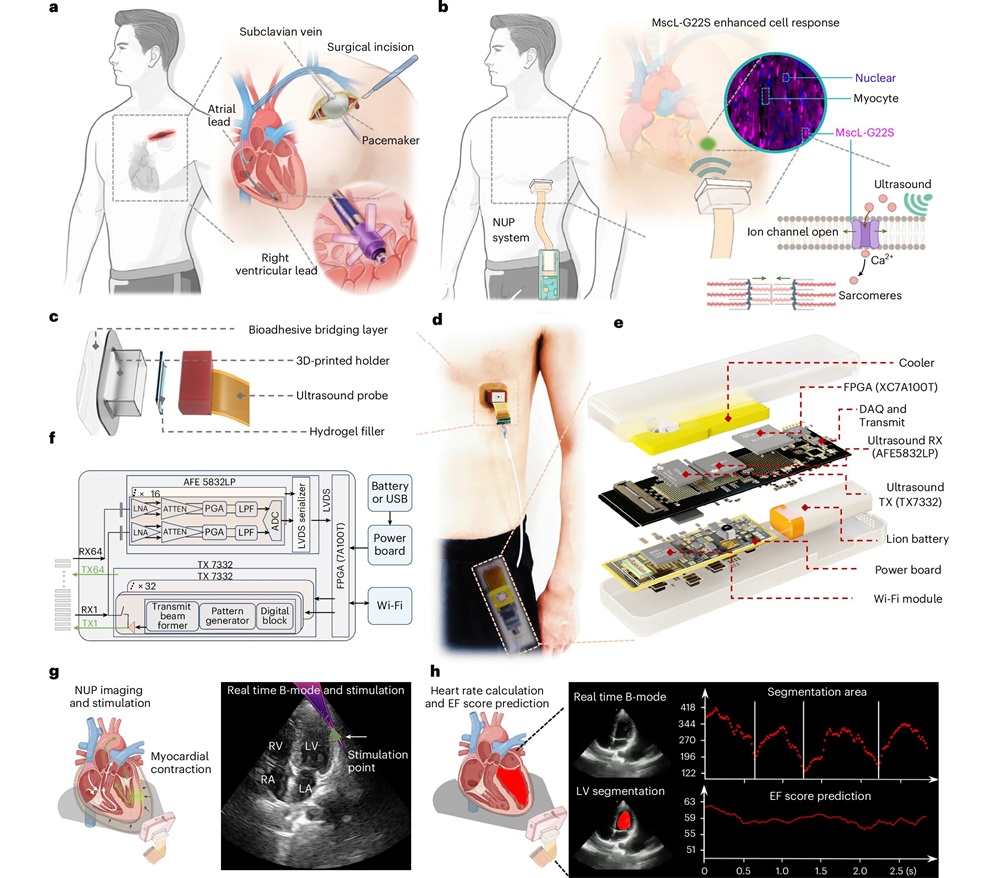
Wearable Ultrasound Patch Noninvasively Paces Heart to Stabilize Arrhythmias
Cardiac arrhythmias, including slow and irregular heart rhythms, often require pacemakers that are surgically implanted. While effective, implants carry procedural risks and long-term device maintenance burdens.... Read moreSurgical Techniques
view channel
CE-Marked Ultrasonic Shears Streamline Breast and Thyroid Surgery
Thyroid and breast surgeries are often performed in confined anatomical spaces near critical structures, making precise dissection and controlled thermal management essential. As the global disease burden... Read more
3D Map of Heart Electrical Wiring Aims to Guide Congenital Heart Repair
Tetralogy of Fallot is one of the most common congenital heart problems and often requires surgery in infancy. Many survivors later develop conduction abnormalities because the cardiac electrical system... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read morePoint of Care
view channel
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more