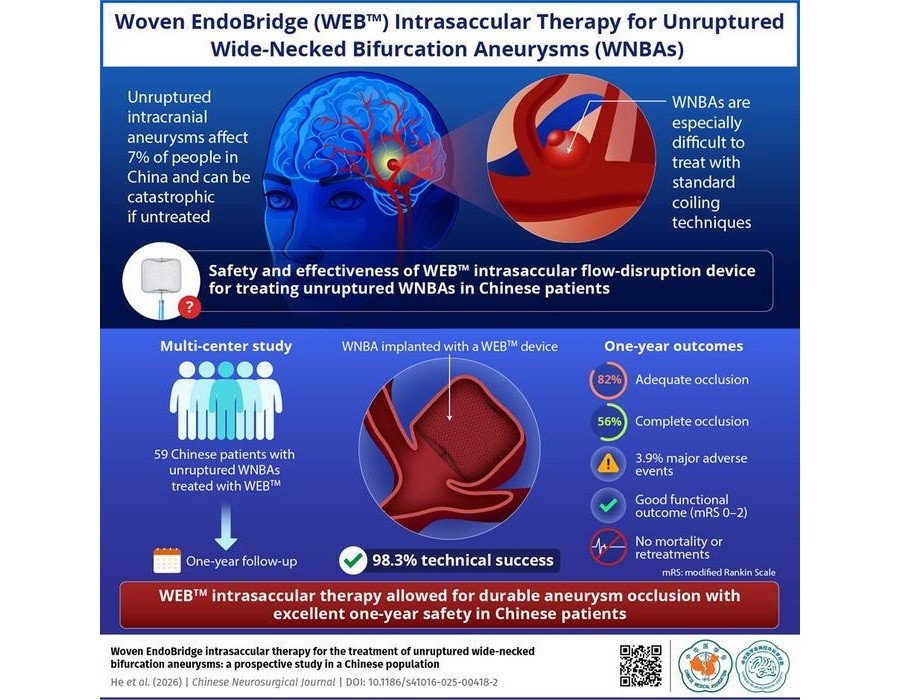
Catheters in Dialysis Linked to High Risk of Infection
|
By HospiMedica International staff writers Posted on 03 Mar 2013 |
A new study shows that dialysis patients using catheters for blood access have the highest risks for death, infections, and cardiovascular (CV) events.
Researchers at the University of Calgary (Canada), the University of Otago (Christchurch, New Zealand), and other institutions conducted a systematic review of cohort studies to evaluate the associations between type of vascular access (arteriovenous fistula, arteriovenous graft, and central venous catheter) and risk for death, infection, and major CV events. The researchers searched MEDLINE, EMBASE, and other article reference lists and extracted data describing study design, participants, vascular access type, clinical outcomes, and risk for bias. In all, 62 cohort studies comprising 586,337 participants met the inclusion criteria.
The results showed that when compared with patients with an arteriovenous fistula, those using catheters had a 38% higher risk of experiencing a major heart-related event, a 53% higher risk of dying, and more than twice the risk of developing fatal infections. Patients with arteriovenous grafts had an 18% increased risk of dying and a 36% increased risk of developing fatal infections compared to those with an arteriovenous fistula, but they did not have an increased risk of experiencing a major heart-related event. The study was published early online on February 21, 2013, in the Journal of the American Society of Nephrology (JASN).
“Our findings are reflected in current clinical practice guidelines, which promote fistulas as the preferred form of bloodstream access in hemodialysis patients,” said lead author Pietro Ravani, MD, of the University of Calgary, and colleagues. “Better quality data are needed, but not from studies with the same design as those already available. In fact, our cumulative meta-analysis shows that this information was already available 10 years ago.”
An arteriovenous fistula is currently the most recommended access for kidney disease patients who must undergo dialysis, created by connecting a patient's vein and artery to form a long-lasting site through which blood can be removed and returned. Alternatively, in patients who are unsuitable for a fistula, an arteriovenous graft—a plastic conduit between an artery and a vein—may be used. Many patients, however, prefer a catheter, for reasons that include inadequate preparation for dialysis, avoidance of surgery, or fear of needles (since the connection to the dialysis machine via a catheter does not require needles).
Related Links:
University of Calgary
University of Otago
Researchers at the University of Calgary (Canada), the University of Otago (Christchurch, New Zealand), and other institutions conducted a systematic review of cohort studies to evaluate the associations between type of vascular access (arteriovenous fistula, arteriovenous graft, and central venous catheter) and risk for death, infection, and major CV events. The researchers searched MEDLINE, EMBASE, and other article reference lists and extracted data describing study design, participants, vascular access type, clinical outcomes, and risk for bias. In all, 62 cohort studies comprising 586,337 participants met the inclusion criteria.
The results showed that when compared with patients with an arteriovenous fistula, those using catheters had a 38% higher risk of experiencing a major heart-related event, a 53% higher risk of dying, and more than twice the risk of developing fatal infections. Patients with arteriovenous grafts had an 18% increased risk of dying and a 36% increased risk of developing fatal infections compared to those with an arteriovenous fistula, but they did not have an increased risk of experiencing a major heart-related event. The study was published early online on February 21, 2013, in the Journal of the American Society of Nephrology (JASN).
“Our findings are reflected in current clinical practice guidelines, which promote fistulas as the preferred form of bloodstream access in hemodialysis patients,” said lead author Pietro Ravani, MD, of the University of Calgary, and colleagues. “Better quality data are needed, but not from studies with the same design as those already available. In fact, our cumulative meta-analysis shows that this information was already available 10 years ago.”
An arteriovenous fistula is currently the most recommended access for kidney disease patients who must undergo dialysis, created by connecting a patient's vein and artery to form a long-lasting site through which blood can be removed and returned. Alternatively, in patients who are unsuitable for a fistula, an arteriovenous graft—a plastic conduit between an artery and a vein—may be used. Many patients, however, prefer a catheter, for reasons that include inadequate preparation for dialysis, avoidance of surgery, or fear of needles (since the connection to the dialysis machine via a catheter does not require needles).
Related Links:
University of Calgary
University of Otago
Latest Critical Care News
- Simple 5-Minute Questionnaire Test Speeds Endometriosis Diagnosis
- Nanohydrogels Guide Medicine to Tumors Without Damaging Healthy Tissue
- Magnetic Gel Offers Safer and More Effective Atrial Fibrillation Treatment
- Hydrogel Biosensor Detects and Differentiates Blood Circulation Complications
- Spray-Type Technology Coats Transplant Organs with Immunosuppressants to Prevent Rejection
- Single Heart Attack Shot to Revolutionize Cardiac Care
- Machine-Learning Model Predicts Preeclampsia in Late Pregnancy
- Single Mid-Wave Infrared Thermal Camera Enables Noncontact Vital Signs Monitoring
- 3D-Printed Bandage to Help Heal Chronic Wounds
- Ultrasound-Activated Nanoagents Kill Superbugs Hiding in Biofilms
- Painless Microneedle Skin Patch Monitors Immune Health

- Smart T-Shirt Uses AI to Enhance Detection of Heart Rhythm Disorders
- Aptamers Enable Real-Time Biomarker Tracking Without Blood Draws
- Specialized Dressing with Sensor Monitors pH Levels in Chronic Wounds
- AI Model Could Help Diagnose Spinal Cord Disease Up To 30 Months Earlier
- 3D-Printed Swallowable Robot Could Perform Gastrointestinal Procedures
Channels
Artificial Intelligence
view channel
AI Model Identifies Rare Endocrine Disorder from Hand Images
Acromegaly is a rare, intractable disease that typically begins in middle age and causes enlargement of the hands and feet, changes in facial appearance, and abnormal bone and organ growth.... Read moreSurgical Techniques
view channel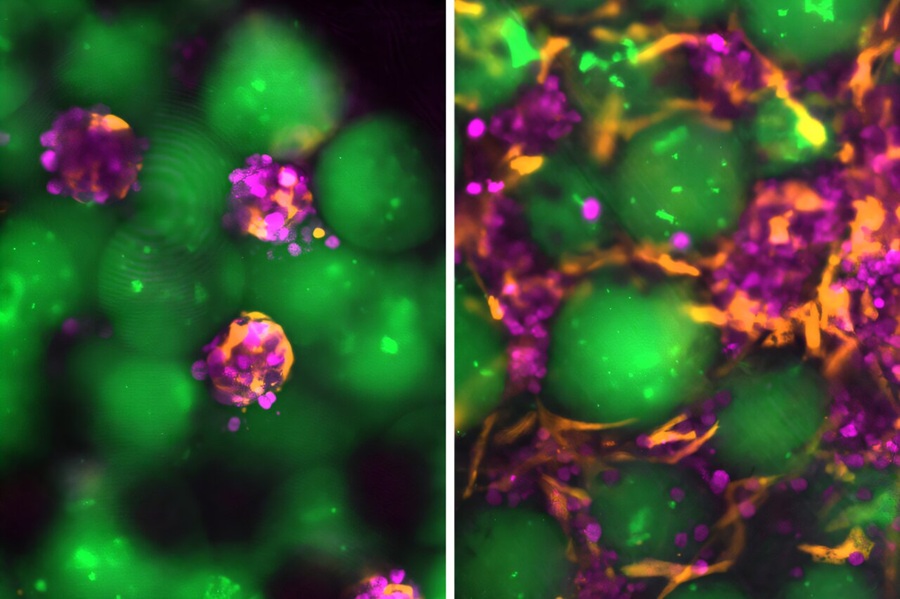
Injectable Mini Livers Offer Hope for Patients Awaiting Transplant
Chronic liver disease and acute liver failure leave thousands dependent on transplantation, yet donor organs remain scarce and many patients are too frail for major surgery. The resulting treatment gap... Read more
Pulsed Field Ablation Technology Cleared in Europe for Persistent AFib
Atrial fibrillation is a common heart rhythm disorder that can cause dizziness, fatigue, and shortness of breath and is associated with an increased risk of stroke. Persistent atrial fibrillation, defined... Read morePatient Care
view channel
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read more
VR Training Tool Combats Contamination of Portable Medical Equipment
Healthcare-associated infections (HAIs) impact one in every 31 patients, cause nearly 100,000 deaths each year, and cost USD 28.4 billion in direct medical expenses. Notably, up to 75% of these infections... Read more
Portable Biosensor Platform to Reduce Hospital-Acquired Infections
Approximately 4 million patients in the European Union acquire healthcare-associated infections (HAIs) or nosocomial infections each year, with around 37,000 deaths directly resulting from these infections,... Read moreFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel
Quantum Surgical Acquires NeuWave from Johnson & Johnson
Quantum Surgical announced that it has acquired NeuWave Medical from Johnson & Johnson. NeuWave’s microwave ablation system is used in percutaneous tumor ablation procedures, and the acquisition supports... Read more
Medtronic to Acquire Coronary Artery Medtech Company CathWorks
Medtronic plc (Galway, Ireland) has announced that it will exercise its option to acquire CathWorks (Kfar Saba, Israel), a privately held medical device company, which aims to transform how coronary artery... Read more








.jpg)