“Black Box” Recorder Monitors Operating Rooms 
|
By HospiMedica International staff writers Posted on 29 Jul 2014 |

Image: The PESA Xstream “Black box” for operating rooms (Photo courtesy of PESA).
A “black box,” similar to that used in the airline industry, could improve patient safety and outcomes by identifying where errors occur in the operating room (OR) and teaching surgeons how to prevent them.
Developed at St. Michael’s Hospital (Toronto, ON, Canada), in collaboration with Air Canada (Montreal, Canada) the “black box” records almost everything that is happening in the OR, such as vital signs, a video of the OR, a video feed from the endoscope used in the surgical procedure, conversations among health care workers, room temperature, and decibel levels. Based on the PESA (Huntsville, AL, USA) X-stream multipath streaming media recorder, the technology is currently being used for minimally invasive surgery (MIS), but could be expanded for open surgeries as well.
Patients must give their consent before the black box is used during their surgery, as do members of the surgical team, including theater nurses. In a preliminary review of the data recorded on the device, the researchers have found that 84% of errors during gastric bypass MIS procedures occurred during the same two stages - suturing and grafting the bowel. The device has been in use at St. Michael’s since April 2014, and is also being tested at two hospitals in Copenhagen (Denmark), with more international sites to be involved soon.
“We want to see where errors happen in surgery so that we can understand how errors lead to adverse events and develop training curricula to prevent these errors from ever happening again,” said device developer surgeon Teodor Grantcharov, MD. “It doesn’t mean that we will have perfect surgeries, because we are not perfect. But it means we will learn from our errors, which will make us safer. We will train future surgeons better because we can show them what the most critical situations are and how to avoid them.”
“For surgeons, we will have data that will allow better coaching and improvements, and therefore better patient care. We will reduce the risk and complications and show how to make the OR more efficient, which will also allow us to save money and do more cases,” added Dr. Grantcharov. He also added that he hoped his black box would bring more transparency to the OR for patients, and help change the “blame-and-shame” culture that traditionally has made doctors and nurses reluctant to report mistakes.
Related Links:
St. Michael’s Hospital
Air Canada
PESA
Developed at St. Michael’s Hospital (Toronto, ON, Canada), in collaboration with Air Canada (Montreal, Canada) the “black box” records almost everything that is happening in the OR, such as vital signs, a video of the OR, a video feed from the endoscope used in the surgical procedure, conversations among health care workers, room temperature, and decibel levels. Based on the PESA (Huntsville, AL, USA) X-stream multipath streaming media recorder, the technology is currently being used for minimally invasive surgery (MIS), but could be expanded for open surgeries as well.
Patients must give their consent before the black box is used during their surgery, as do members of the surgical team, including theater nurses. In a preliminary review of the data recorded on the device, the researchers have found that 84% of errors during gastric bypass MIS procedures occurred during the same two stages - suturing and grafting the bowel. The device has been in use at St. Michael’s since April 2014, and is also being tested at two hospitals in Copenhagen (Denmark), with more international sites to be involved soon.
“We want to see where errors happen in surgery so that we can understand how errors lead to adverse events and develop training curricula to prevent these errors from ever happening again,” said device developer surgeon Teodor Grantcharov, MD. “It doesn’t mean that we will have perfect surgeries, because we are not perfect. But it means we will learn from our errors, which will make us safer. We will train future surgeons better because we can show them what the most critical situations are and how to avoid them.”
“For surgeons, we will have data that will allow better coaching and improvements, and therefore better patient care. We will reduce the risk and complications and show how to make the OR more efficient, which will also allow us to save money and do more cases,” added Dr. Grantcharov. He also added that he hoped his black box would bring more transparency to the OR for patients, and help change the “blame-and-shame” culture that traditionally has made doctors and nurses reluctant to report mistakes.
Related Links:
St. Michael’s Hospital
Air Canada
PESA
Latest Health IT News
- AI-Native EHR Achieves EU Medical Device Certification
- EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
- AI System Detects and Quantifies Chronic Subdural Hematoma
- Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
- Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
- Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
Channels
Artificial Intelligence
view channel
Automated Phone Speech Test Identifies Alzheimer’s Pathology for Prescreening
Alzheimer’s disease assessment and trial recruitment often rely on costly, invasive biomarker testing and clinic-based cognitive evaluations, limiting scalability as populations age. Providers and trial... Read more
FDA-Cleared AI System Detects Sepsis Earlier and Reduces Mortality
Sepsis remains one of the deadliest complications for hospitalized patients, in part because its early signs overlap with other conditions. Each hour of delayed recognition measurably decreases survival,... Read moreCritical Care
view channel
Ring-Type Cuffless Monitor Becomes First Added to Official Hypertension Guidelines
Detecting nocturnal and morning hypertension often requires out-of-office assessment, but conventional cuff-type monitors can disrupt sleep. New national guidance in South Korea expands 24-hour monitoring... Read more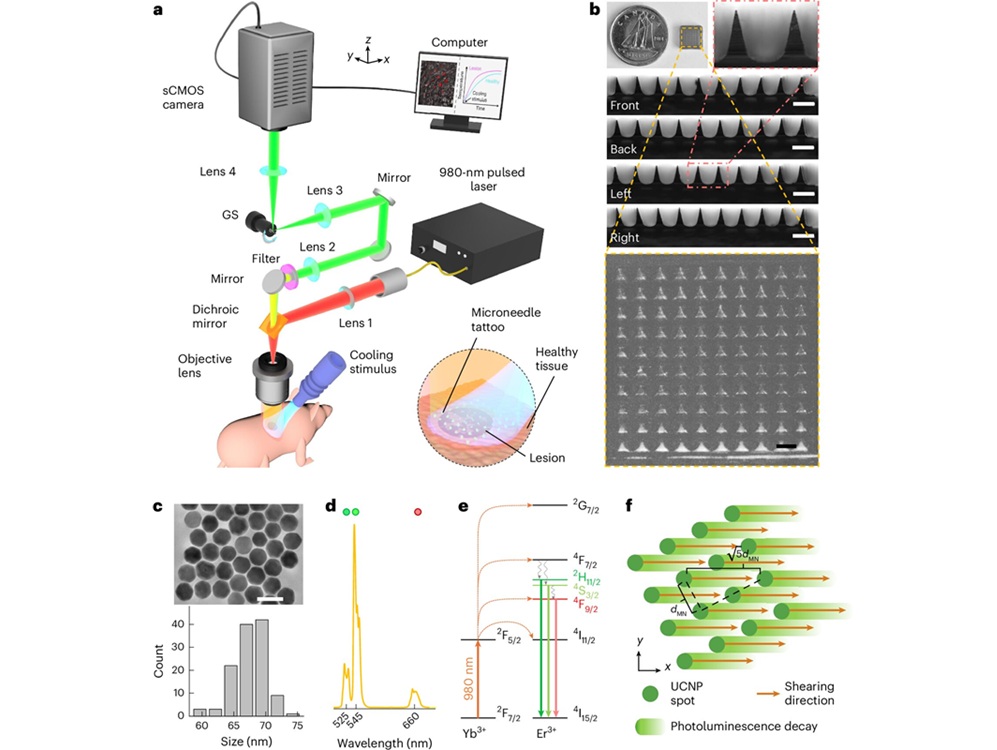
“Intelligent Tattoo” Method Detects Early Melanoma Signals
Melanoma is a lethal skin cancer in which earlier detection drives better outcomes. Current evaluation relies on visual inspection followed by biopsy, which can miss nascent lesions and lead to unnecessary... Read more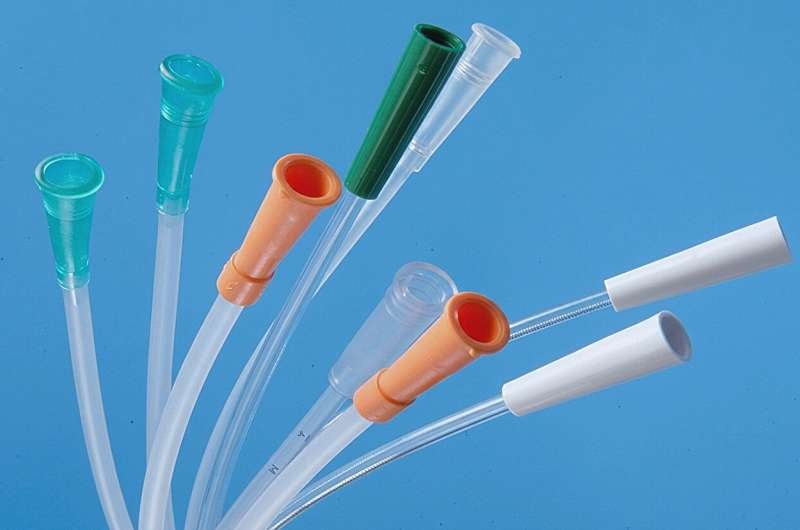
Reusable Intermittent Catheters Reduce Antibiotic Use Without Increasing Urinary Tract Infections
Intermittent self-catheterization, used to empty the bladder several times a day, can leave patients vulnerable to recurrent urinary tract infections and repeated antibiotic use. Reliance on single-use... Read moreSurgical Techniques
view channel
Pink Noise Stimulation Approach Could Support Safer Anesthesia
Maintaining stable unconsciousness during general anesthesia while minimizing drug exposure remains a core perioperative challenge. Sudden nociceptive surges can disrupt anesthetic depth, increasing neurological... Read more
Surgical Robotic System Gains CE Mark for Minimally Invasive Procedures
Cornerstone Robotics’ (CSR; Hong Kong, China) Sentire Endoscopic Surgical System (Sentire Surgical System) has received European Union CE mark certification under the Medical Device Regulation (MDR) for... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read morePoint of Care
view channel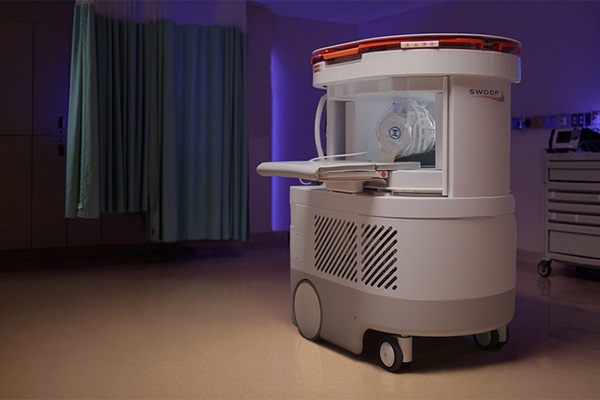
Portable MRI System Accelerates Emergency Brain Imaging and Supports Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more