Mortality Risk Higher Following Early Stroke
|
By HospiMedica International staff writers Posted on 18 Aug 2014 |
A new study reveals that nearly one in six teens and adults who initially survive a stroke before age 50 die over the next decade.
Researchers at Helsinki University Central Hospital (HUS; Finland) conducted a study to assess the risk of mortality and recurrent stroke rate in 970 consecutive patients (15–49 years of age) that survived 30 days following a first-ever ischemic stroke. Prospective follow-up data (from 1994 to 2007) from the Finnish Care Register for Health Care and Statistics was reviewed to compare survival between clinical subgroups. Mortality ratio for demographic and pathogenetic subgroups was calculated using mortality data of the general population matched with age, sex, calendar year, and geographical area.
The results showed that at the end of follow-up, 15.7% of the patients had died, representing a cumulative risk of 23%, while 13.6% of the patients had experienced a recurrent stroke. After adjusting for baseline characteristics, recurrent stroke was statistically the most important risk factor for mortality after first-ever ischemic stroke. Observed mortality was 7-fold higher than the expected mortality, and particularly high among patients who experienced a recurrent stroke. The study was published on July 24, 2014, in Stroke.
“The high mortality rates and the striking impact of recurrent stroke on the risk of death should lead to development of more robust primary and secondary prevention strategies for young patients with stroke,” concluded lead author Karoliina Aarnio, MD, and colleagues.
The rate of stroke is increasing faster in individuals 40–60 of age than in any other age group. Although the primary causes of stroke—obesity, diabetes, high blood pressure, smoking, and excess alcohol consumption—are still primary contributors, an increasing number of strokes are related to atypical causes such as migraine, drug use, and carotid dissection. Other causes, such as congenital heart disease (CHD), patent foramen ovale (PFO), and blood clotting abnormalities, as well as family history, need to be considered in the younger population of stroke sufferers.
Related Links:
Helsinki University Central Hospital
Researchers at Helsinki University Central Hospital (HUS; Finland) conducted a study to assess the risk of mortality and recurrent stroke rate in 970 consecutive patients (15–49 years of age) that survived 30 days following a first-ever ischemic stroke. Prospective follow-up data (from 1994 to 2007) from the Finnish Care Register for Health Care and Statistics was reviewed to compare survival between clinical subgroups. Mortality ratio for demographic and pathogenetic subgroups was calculated using mortality data of the general population matched with age, sex, calendar year, and geographical area.
The results showed that at the end of follow-up, 15.7% of the patients had died, representing a cumulative risk of 23%, while 13.6% of the patients had experienced a recurrent stroke. After adjusting for baseline characteristics, recurrent stroke was statistically the most important risk factor for mortality after first-ever ischemic stroke. Observed mortality was 7-fold higher than the expected mortality, and particularly high among patients who experienced a recurrent stroke. The study was published on July 24, 2014, in Stroke.
“The high mortality rates and the striking impact of recurrent stroke on the risk of death should lead to development of more robust primary and secondary prevention strategies for young patients with stroke,” concluded lead author Karoliina Aarnio, MD, and colleagues.
The rate of stroke is increasing faster in individuals 40–60 of age than in any other age group. Although the primary causes of stroke—obesity, diabetes, high blood pressure, smoking, and excess alcohol consumption—are still primary contributors, an increasing number of strokes are related to atypical causes such as migraine, drug use, and carotid dissection. Other causes, such as congenital heart disease (CHD), patent foramen ovale (PFO), and blood clotting abnormalities, as well as family history, need to be considered in the younger population of stroke sufferers.
Related Links:
Helsinki University Central Hospital
Latest Critical Care News
- Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
- Eye Imaging AI Identifies Elevated Cardiovascular Risk
- Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreSurgical Techniques
view channel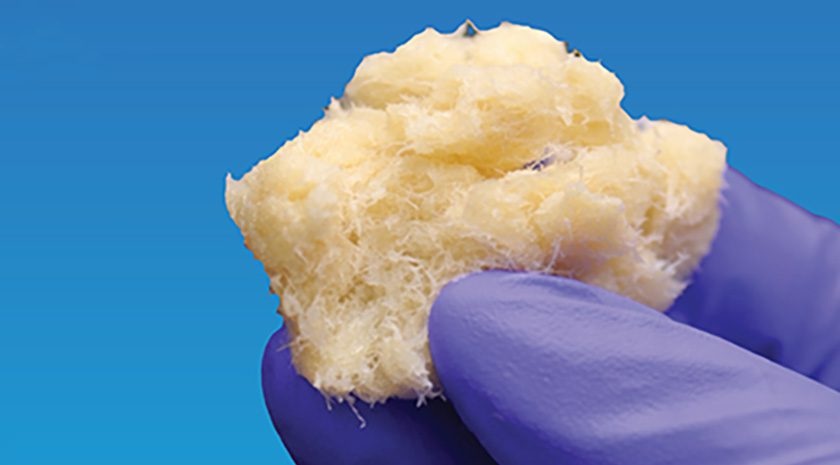
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more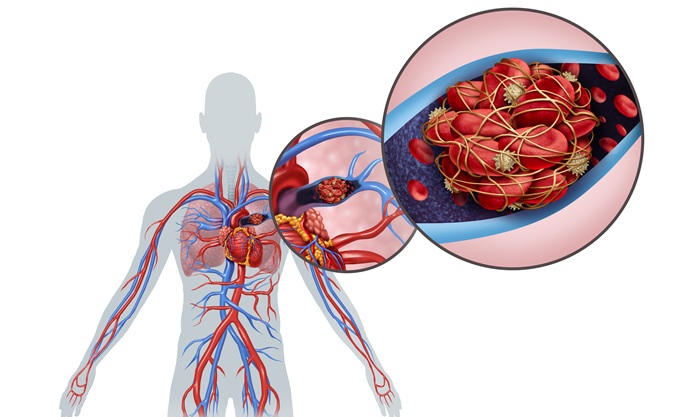
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel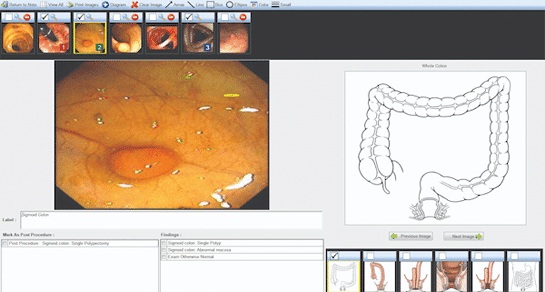
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel




















