HPV Positive Throat Cancer Patients Need Less Neck Surgery
|
By HospiMedica International staff writers Posted on 29 Sep 2014 |
Patients with oropharyngeal cancer (OPC) resulting from human papillomavirus (HPV) show significantly higher rates of complete response on a post-radiation neck dissection, according to a new study.
Researchers at the Fox Chase Cancer Center (FCCC; Philadelphia, PA, USA) reviewed the medical records of 396 patients whose oropharyngeal tumors had spread to at least one lymph node. Within 180 days of completing radiation therapy, 146 of the patients underwent neck surgery to remove persistent lumps in their neck; of these, 99 patients had records that indicated whether or not their tumors had likely been triggered by HPV.
The researchers found that patients with HPV often responded better to treatment for OPC than those without. The same trend suggested that those that tested positive for HPV—measured by the presence of a protein called p16—were less likely to have a recurrence of their cancers, regardless of whether or not the tumors had completely disappeared following treatment. Patients’ HPV status was also the strongest predictor of whether or not they were alive at the end of the study. The study was presented at the American Society for Radiation Oncology (ASRO) annual meeting, held during September 2014 in Chicago (IL, USA).
“Among the patients who underwent neck surgery, any lingering bumps were more likely to be benign if patients were infected with HPV,” said lead author and study presenter Thomas Galloway, MD, director of clinical research at FCCC. “For patients that achieve a complete response, neck surgery is probably unnecessary. The bump might have become a permanent scar, or in some cases, it would have eventually disappeared.”
HPV oral infection precedes the development of the related OPC. Slight injury to the mucous membrane serves as an entry gate for HPV, which thus works into the basal layer of the epithelium. An earlier prospective study found that increased HPV+ OPC risk was observed more than 15 years after HPV exposure, pointing to a slow development of the disease, much like cervical cancer.
Related Links:
Fox Chase Cancer Center
Researchers at the Fox Chase Cancer Center (FCCC; Philadelphia, PA, USA) reviewed the medical records of 396 patients whose oropharyngeal tumors had spread to at least one lymph node. Within 180 days of completing radiation therapy, 146 of the patients underwent neck surgery to remove persistent lumps in their neck; of these, 99 patients had records that indicated whether or not their tumors had likely been triggered by HPV.
The researchers found that patients with HPV often responded better to treatment for OPC than those without. The same trend suggested that those that tested positive for HPV—measured by the presence of a protein called p16—were less likely to have a recurrence of their cancers, regardless of whether or not the tumors had completely disappeared following treatment. Patients’ HPV status was also the strongest predictor of whether or not they were alive at the end of the study. The study was presented at the American Society for Radiation Oncology (ASRO) annual meeting, held during September 2014 in Chicago (IL, USA).
“Among the patients who underwent neck surgery, any lingering bumps were more likely to be benign if patients were infected with HPV,” said lead author and study presenter Thomas Galloway, MD, director of clinical research at FCCC. “For patients that achieve a complete response, neck surgery is probably unnecessary. The bump might have become a permanent scar, or in some cases, it would have eventually disappeared.”
HPV oral infection precedes the development of the related OPC. Slight injury to the mucous membrane serves as an entry gate for HPV, which thus works into the basal layer of the epithelium. An earlier prospective study found that increased HPV+ OPC risk was observed more than 15 years after HPV exposure, pointing to a slow development of the disease, much like cervical cancer.
Related Links:
Fox Chase Cancer Center
Latest Surgical Techniques News
- 3D Map of Heart Electrical Wiring Aims to Guide Congenital Heart Repair
- Small Cryoprobe Outperforms Forceps in Lung Biopsy Trial
- Natural Bypass Score May Guide Care in Chronic Coronary Blockages
- Navigation Instruments Cleared for Posterior Cervical Fusion Procedures
- Bioengineered Heart Patch Improves Cardiac Function in Advanced Heart Failure
- Fracture Plating System Combines Anatomical Fit with Streamlined Instrumentation
- Surgical Robotic System Gains CE Mark for Minimally Invasive Procedures
- Pink Noise Stimulation Approach Could Support Safer Anesthesia
- BD Launches Elyra Laser Platform for Kidney Stone and Soft Tissue Procedures
- Anesthesia-Sparing System Targets Faster Ureteral Stone Treatment
- Stretchable Bioelectronic Implant Lowers Blood Pressure in Preclinical Study
- FDA-Cleared Nerve Stimulator Advances Intraoperative Peripheral Nerve Assessment
- Intravascular Lithotripsy Catheter Advances Treatment of Calcified Coronary Disease
- Handheld AI Endomicroscope Enables Real-Time Precancer Detection at Point of Care
- Photoacoustic Imaging System Maps Hidden Nerves and Vessels in Robotic Laparoscopy
- Smart Soft Sensors Provide Real-Time Force Feedback in Minimally Invasive Surgery
Channels
Artificial Intelligence
view channel
AI Platform Supports Noninvasive Remote Hemodynamic Monitoring in Heart Failure
Heart failure remains a leading cause of hospitalization in adults over 65, affecting more than 6.7 million people in the U.S. Clinicians often lose visibility into hemodynamic deterioration once patients... Read more
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read moreCritical Care
view channel
Bedside CSF Monitor Detects Early Infection in Fluid Drains
External drainage of cerebrospinal fluid (CSF) after traumatic brain injury, hydrocephalus, or hemorrhage carries a significant risk of infection. These infections can prolong intensive care, cause severe... Read more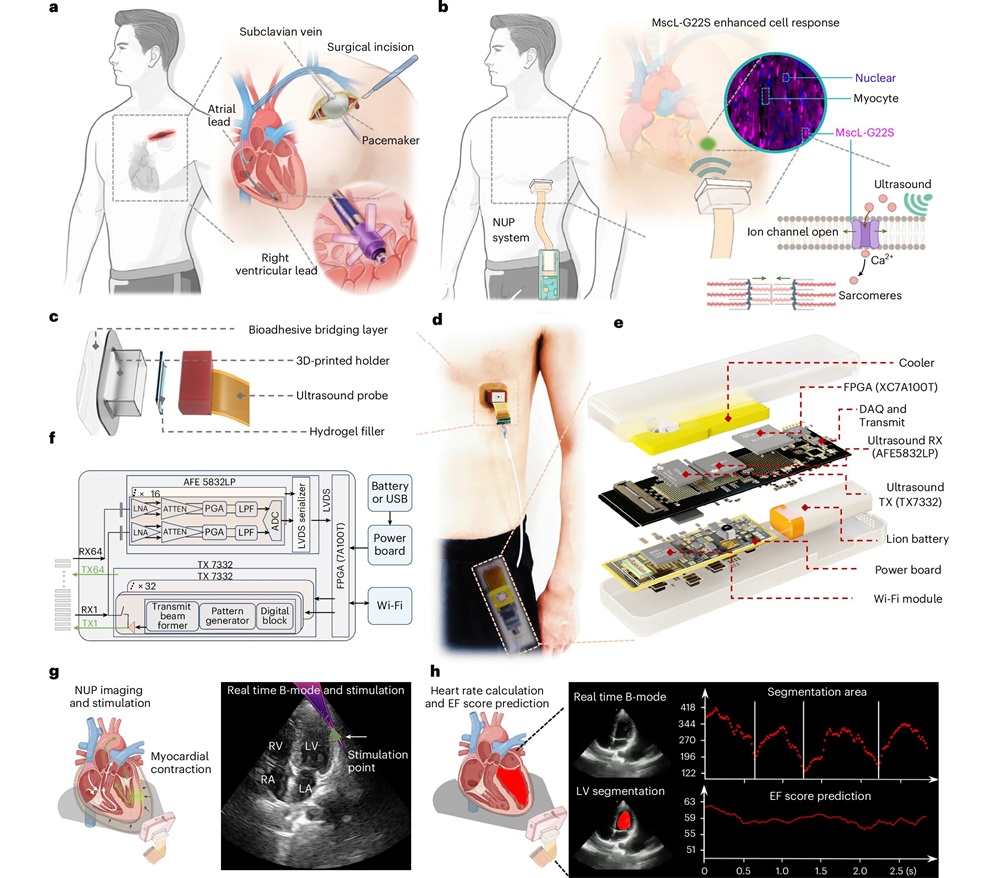
Wearable Ultrasound Patch Noninvasively Paces Heart to Stabilize Arrhythmias
Cardiac arrhythmias, including slow and irregular heart rhythms, often require pacemakers that are surgically implanted. While effective, implants carry procedural risks and long-term device maintenance burdens.... Read more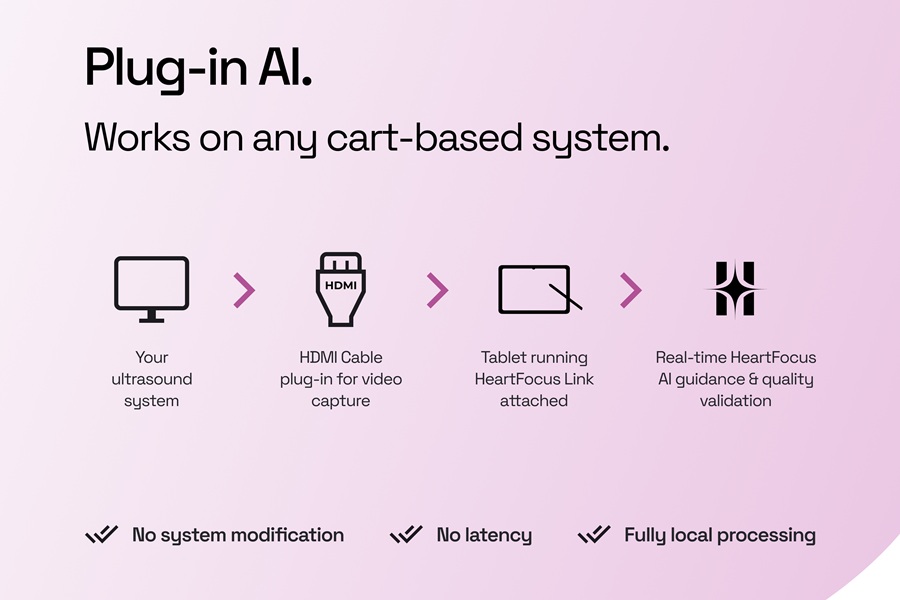
AI-Guided System Supports Cardiac Ultrasound Training on Cart-Based Systems
Cardiac ultrasound adoption in frontline settings often lags despite widespread investment in ultrasound equipment. Many systems sit underused for cardiac imaging because acquiring standard views requires... Read more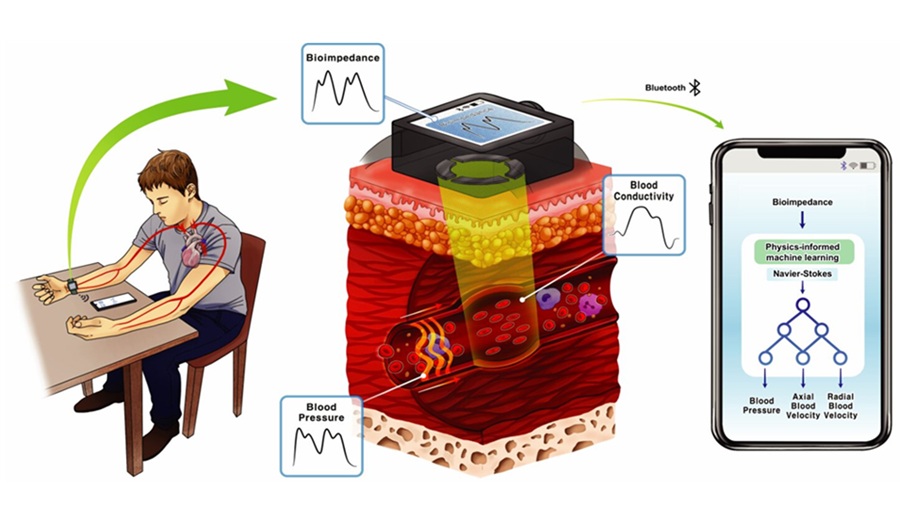
Cuffless Wearable Enables Continuous Blood Pressure Monitoring for Hypertension Care
Hypertension, or chronically elevated blood pressure, drives major risks for heart attack and stroke yet is typically assessed with intermittent cuff readings. These snapshots miss rapid physiologic changes... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read moreHealth IT
view channel
AI-Native EHR Achieves EU Medical Device Certification
InterSystems (Boston, MA, USA) announced that its IntelliCare electronic health record (EHR) solutions have been certified as Class IIa medical devices under the European Union Medical Device Regulation... Read more
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read morePoint of Care
view channel
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more