Heart Association Issues Statement on Understanding Radiation Risks Before Cardiac Imaging
|
By HospiMedica International staff writers Posted on 16 Oct 2014 |
Image: The American Heart Association issued a statement that patients need to be informed on radiation risks before undergoing cardiac imaging (Photo courtesy of AHA - The American Heart Association).
People should understand why a heart-imaging test is needed before undergoing the procedure, including the benefits and risks involved, such as the potential long-term risk from radiation exposure, advises a new scientific statement.
The statement was published online, before print, on September 29, 2014, in the American Heart Association’s (AHA; Dallas, TX, USA) journal Circulation. “When medical imaging is being considered, patients should feel very comfortable asking how the test will help them and the possible risks, including radiation-related risks,” said Reza Fazel, MD, MSc, chair of the writing committee for the statement and an AHA volunteer currently serving on the Joint Cardiac Imaging Committee of the AHA’s Council on Clinical Cardiology and Council on Cardiovascular Radiology.
As technology has evolved, imaging modalities have become an increasingly important application in diagnosing and treating patients with heart disease. However, the rising use has resulted in higher radiation exposure during the last 20 years. Heart imaging now accounts for nearly 40% of the radiation exposure patients receive from medical tests, according to the statement.
“In general, the radiation-related risk of any imaging test to an individual patient is very small and, when the test is clinically appropriate, the benefits of the test typically far outweigh any potential risks,” said Dr. Fazel, a cardiologist at Beth Israel Deaconess Medical Center (Boston, MA, USA).
Some questions that may help a patient understand the risks and benefits are: (1) how will this test help diagnose or treat my heart problem? (2) Will the results of this test change the recommended treatment? (3) Are there other techniques to get the information without using radiation? (4) How much radiation exposure may occur? (5) How could that affect my chance of developing cancer later in life? (6) Lastly, how does that risk compare to the risk from other common activities?
The most typically used heart and blood vessel imaging procedures using radiation are nuclear stress tests, cardiac computed tomography (CT) scans and fluoroscopy (a real-time X-ray technology used to guide catheter and device placement during heart catheterization and tests for heart rhythm abnormalities). Echocardiography and cardiac magnetic resonance imaging do not expose patients to ionizing radiation.
The new statement also provides guidance for the training of professionals who order or administer cardiac imaging tests. Clinicians planning imaging tests should understand when each type of test is appropriate, the typical average radiation dose and the potential risks. In deciding the best imaging method to use, the clinician should also consider the test’s diagnostic accuracy, potential risks, cost, availability, and the patient’s convenience.
“Radiation-related risk is one of the factors that should be considered in the decision to use cardiovascular imaging with ionizing radiation, particularly in younger patients in whom the potential risk of radiation exposure is thought to be higher,” Dr. Fazel said.
Clinicians who perform cardiac imaging should understand current methods required to select the optimal dose of radiation—using enough to produce high-quality imaged, not significantly more than that. They should also know how to minimize radiation exposure to staff, according to the statement.
Related Links:
American Heart Association
Beth Israel Deaconess Medical Center
The statement was published online, before print, on September 29, 2014, in the American Heart Association’s (AHA; Dallas, TX, USA) journal Circulation. “When medical imaging is being considered, patients should feel very comfortable asking how the test will help them and the possible risks, including radiation-related risks,” said Reza Fazel, MD, MSc, chair of the writing committee for the statement and an AHA volunteer currently serving on the Joint Cardiac Imaging Committee of the AHA’s Council on Clinical Cardiology and Council on Cardiovascular Radiology.
As technology has evolved, imaging modalities have become an increasingly important application in diagnosing and treating patients with heart disease. However, the rising use has resulted in higher radiation exposure during the last 20 years. Heart imaging now accounts for nearly 40% of the radiation exposure patients receive from medical tests, according to the statement.
“In general, the radiation-related risk of any imaging test to an individual patient is very small and, when the test is clinically appropriate, the benefits of the test typically far outweigh any potential risks,” said Dr. Fazel, a cardiologist at Beth Israel Deaconess Medical Center (Boston, MA, USA).
Some questions that may help a patient understand the risks and benefits are: (1) how will this test help diagnose or treat my heart problem? (2) Will the results of this test change the recommended treatment? (3) Are there other techniques to get the information without using radiation? (4) How much radiation exposure may occur? (5) How could that affect my chance of developing cancer later in life? (6) Lastly, how does that risk compare to the risk from other common activities?
The most typically used heart and blood vessel imaging procedures using radiation are nuclear stress tests, cardiac computed tomography (CT) scans and fluoroscopy (a real-time X-ray technology used to guide catheter and device placement during heart catheterization and tests for heart rhythm abnormalities). Echocardiography and cardiac magnetic resonance imaging do not expose patients to ionizing radiation.
The new statement also provides guidance for the training of professionals who order or administer cardiac imaging tests. Clinicians planning imaging tests should understand when each type of test is appropriate, the typical average radiation dose and the potential risks. In deciding the best imaging method to use, the clinician should also consider the test’s diagnostic accuracy, potential risks, cost, availability, and the patient’s convenience.
“Radiation-related risk is one of the factors that should be considered in the decision to use cardiovascular imaging with ionizing radiation, particularly in younger patients in whom the potential risk of radiation exposure is thought to be higher,” Dr. Fazel said.
Clinicians who perform cardiac imaging should understand current methods required to select the optimal dose of radiation—using enough to produce high-quality imaged, not significantly more than that. They should also know how to minimize radiation exposure to staff, according to the statement.
Related Links:
American Heart Association
Beth Israel Deaconess Medical Center
Latest Critical Care News
- Bedside CSF Monitor Detects Early Infection in Fluid Drains
- Wearable Ultrasound Patch Noninvasively Paces Heart to Stabilize Arrhythmias
- AI ECG Tool Detects Cardiac Amyloidosis for Early Screening
- Cuffless Wearable Enables Continuous Blood Pressure Monitoring for Hypertension Care
- AI-Guided System Supports Cardiac Ultrasound Training on Cart-Based Systems
- AI ECG Index Tracks Pubertal Maturation in Children and Adolescents
- Noninvasive AI Tool Enables Pressure-Guided Heart Failure Management
- Regenerative Therapies Aim to Support Recovery After Traumatic Brain Injury
- Ring-Type Cuffless Monitor Becomes First Added to Official Hypertension Guidelines
- “Intelligent Tattoo” Method Detects Early Melanoma Signals
- Implantable Wireless Light Device Advances Bladder Cancer Treatment
- Reusable Intermittent Catheters Reduce Antibiotic Use Without Increasing Urinary Tract Infections
- Smart Wristband Technology Detects Cardiac Arrest and Alerts Responders
- FDA-Cleared Home Sleep Test Enables Multi-Night Diagnosis of Sleep Apnea
- AI-Enabled Wearable Patches Reveal Undetected Hormone Disruption in Infertility
- AI Method Turns Toe Scan into Rapid PAD Screening Tool
Channels
Artificial Intelligence
view channel
AI Platform Supports Noninvasive Remote Hemodynamic Monitoring in Heart Failure
Heart failure remains a leading cause of hospitalization in adults over 65, affecting more than 6.7 million people in the U.S. Clinicians often lose visibility into hemodynamic deterioration once patients... Read more
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read moreCritical Care
view channel
Bedside CSF Monitor Detects Early Infection in Fluid Drains
External drainage of cerebrospinal fluid (CSF) after traumatic brain injury, hydrocephalus, or hemorrhage carries a significant risk of infection. These infections can prolong intensive care, cause severe... Read more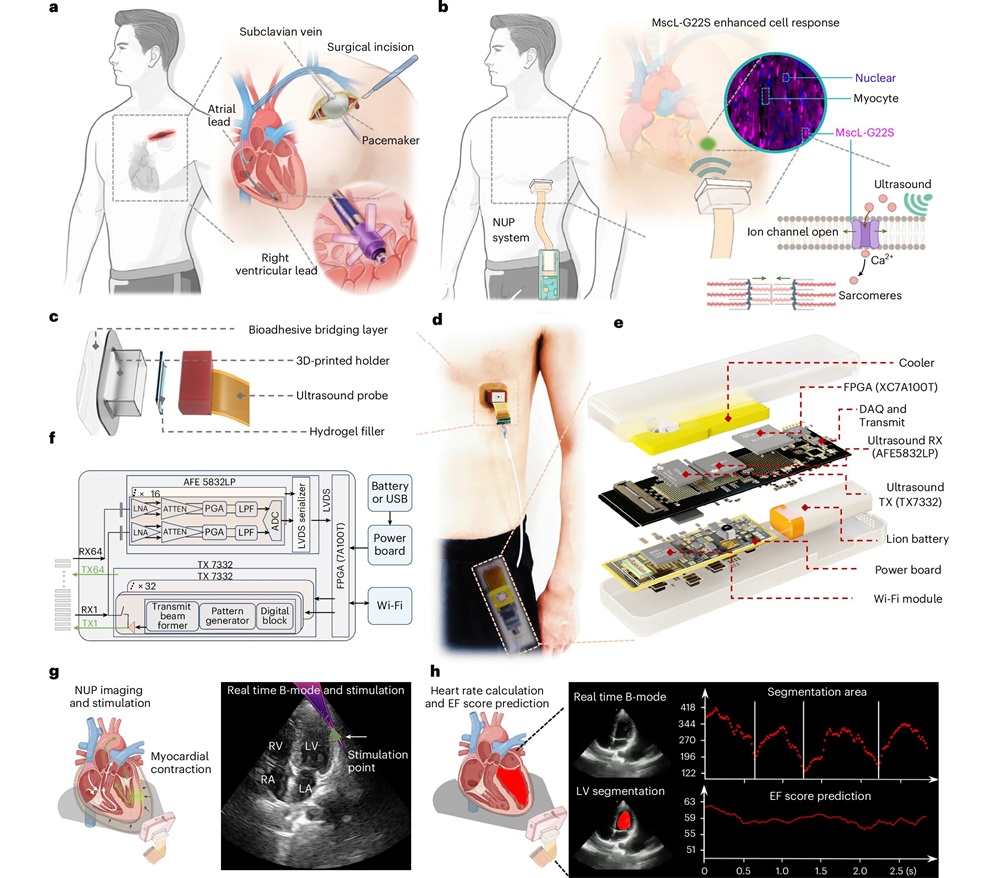
Wearable Ultrasound Patch Noninvasively Paces Heart to Stabilize Arrhythmias
Cardiac arrhythmias, including slow and irregular heart rhythms, often require pacemakers that are surgically implanted. While effective, implants carry procedural risks and long-term device maintenance burdens.... Read more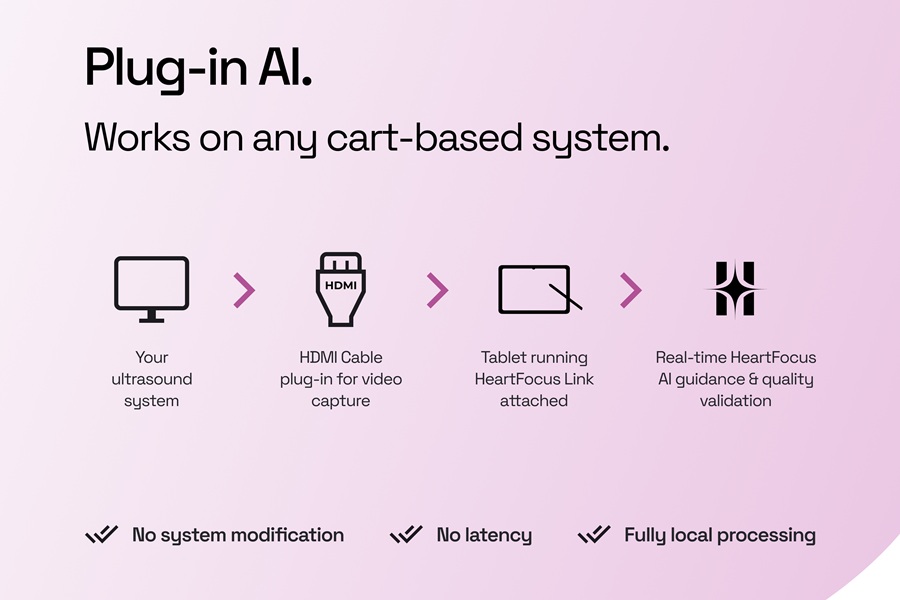
AI-Guided System Supports Cardiac Ultrasound Training on Cart-Based Systems
Cardiac ultrasound adoption in frontline settings often lags despite widespread investment in ultrasound equipment. Many systems sit underused for cardiac imaging because acquiring standard views requires... Read more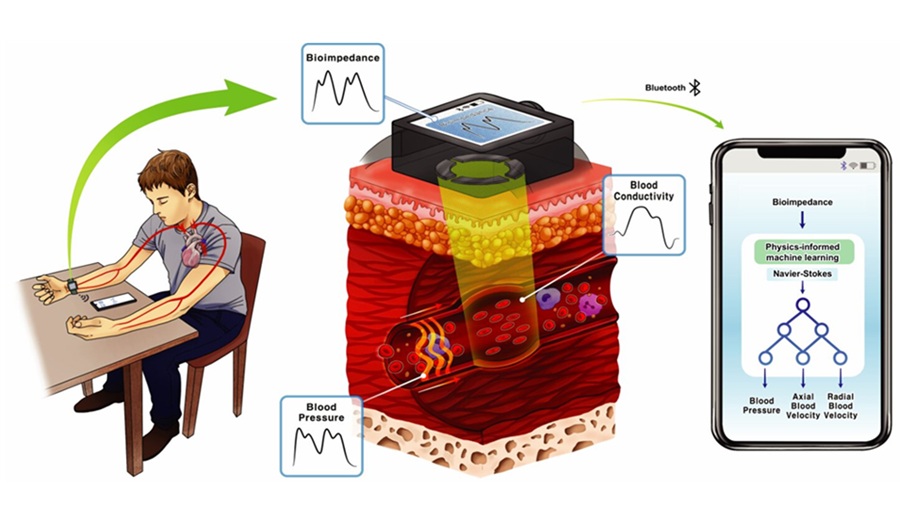
Cuffless Wearable Enables Continuous Blood Pressure Monitoring for Hypertension Care
Hypertension, or chronically elevated blood pressure, drives major risks for heart attack and stroke yet is typically assessed with intermittent cuff readings. These snapshots miss rapid physiologic changes... Read moreSurgical Techniques
view channel
3D Map of Heart Electrical Wiring Aims to Guide Congenital Heart Repair
Tetralogy of Fallot is one of the most common congenital heart problems and often requires surgery in infancy. Many survivors later develop conduction abnormalities because the cardiac electrical system... Read more
Small Cryoprobe Outperforms Forceps in Lung Biopsy Trial
Accurate diagnosis of pulmonary nodules, post-transplant allograft dysfunction, and diffuse parenchymal lung disease depends on high-quality tissue obtained during bronchoscopy. Conventional forceps biopsy... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read moreHealth IT
view channel
AI-Native EHR Achieves EU Medical Device Certification
InterSystems (Boston, MA, USA) announced that its IntelliCare electronic health record (EHR) solutions have been certified as Class IIa medical devices under the European Union Medical Device Regulation... Read more
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read morePoint of Care
view channel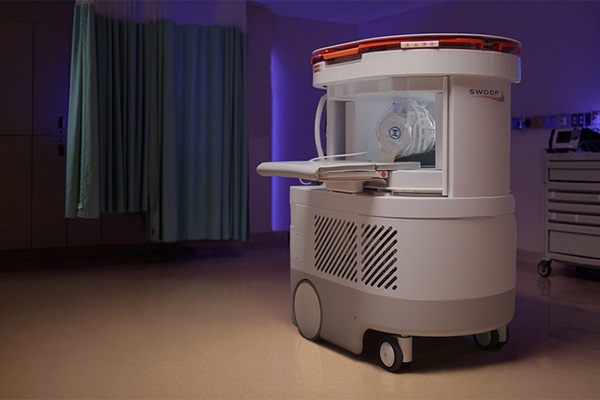
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more