Nerve Block Procedure Safe for Children
|
By HospiMedica International staff writers Posted on 25 Nov 2014 |
Caudal nerve block in children has a low complication rate, with little or no risk of long-term adverse effects, according to a new study.
Researchers at Northwestern University (Chicago, IL, USA) conducted an observational study involving 18,650 children to estimate the overall and specific incidence of complications associated with the performance of caudal block; the data were retrieved from the pediatric regional anesthesia network (PRAN) database. A complication was defined by the presence of block failure, vascular puncture, intravascular test dose, dural puncture, seizure, cardiac arrest, sacral pain, or neurologic symptoms. In addition, the presence of temporary or permanent sequela was evaluated.
The procedures were performed at 18 children's hospitals from 2007 to 2012, with average patient age being 14 months. The complication rate was 1.9%, with the most common complications being block failure, blood aspiration, and intravascular injection, but none of the reported complications led to lasting or permanent adverse effects. Serious complications such as cardiac arrest and seizure were rare, occurring in just four children. The study was published in the October 2014 issue of Anesthesia & Analgesia.
“The results draw attention to variations in the local anesthetic doses used for caudal block, potentially increasing the risk of toxic effects,” warned lead author Santhanam Suresh, MD, and colleagues. “Further studies are needed to define the optimal local anesthetic dosage, as well as the pain-relieving effectiveness of caudal block for specific types of surgery.”
“The PRAN database was a lot of work to create, but it is an important contribution to the safety of children undergoing anesthesia,” commented Steven Shafer, MD, of Stanford University (CA, USA), editor-in-chief of Anesthesia & Analgesia. “This paper shows that caudal blocks for postoperative pain control are safe in children. It will help to guide physicians, and parents, in selecting the anesthetic that provides the best outcome for their kids.”
The caudal block is the most commonly performed regional anesthesia technique in pediatric patients undergoing surgical procedures, involving a small dose of local anesthetic injected into the base of the spine to numb feeling in the lower body. It is usually added to general anesthesia, with the aim of controlling pain after surgery while reducing the required dose of general anesthetic.
Related Links:
Northwestern University
Researchers at Northwestern University (Chicago, IL, USA) conducted an observational study involving 18,650 children to estimate the overall and specific incidence of complications associated with the performance of caudal block; the data were retrieved from the pediatric regional anesthesia network (PRAN) database. A complication was defined by the presence of block failure, vascular puncture, intravascular test dose, dural puncture, seizure, cardiac arrest, sacral pain, or neurologic symptoms. In addition, the presence of temporary or permanent sequela was evaluated.
The procedures were performed at 18 children's hospitals from 2007 to 2012, with average patient age being 14 months. The complication rate was 1.9%, with the most common complications being block failure, blood aspiration, and intravascular injection, but none of the reported complications led to lasting or permanent adverse effects. Serious complications such as cardiac arrest and seizure were rare, occurring in just four children. The study was published in the October 2014 issue of Anesthesia & Analgesia.
“The results draw attention to variations in the local anesthetic doses used for caudal block, potentially increasing the risk of toxic effects,” warned lead author Santhanam Suresh, MD, and colleagues. “Further studies are needed to define the optimal local anesthetic dosage, as well as the pain-relieving effectiveness of caudal block for specific types of surgery.”
“The PRAN database was a lot of work to create, but it is an important contribution to the safety of children undergoing anesthesia,” commented Steven Shafer, MD, of Stanford University (CA, USA), editor-in-chief of Anesthesia & Analgesia. “This paper shows that caudal blocks for postoperative pain control are safe in children. It will help to guide physicians, and parents, in selecting the anesthetic that provides the best outcome for their kids.”
The caudal block is the most commonly performed regional anesthesia technique in pediatric patients undergoing surgical procedures, involving a small dose of local anesthetic injected into the base of the spine to numb feeling in the lower body. It is usually added to general anesthesia, with the aim of controlling pain after surgery while reducing the required dose of general anesthetic.
Related Links:
Northwestern University
Latest Surgical Techniques News
- Noninvasive Cardiac Radiotherapy Reduces Ventricular Tachycardia Events
- Augmented Reality System for Knee Replacement Receives FDA Clearance
- New AI Tool Predicts Complications Before Lung Cancer Surgery
- First Automated Insulin Delivery System Cleared for Type 1 Diabetes in Pregnancy
- Novel Ablation Technology Reduces Ventricular Tachycardia Recurrence
- Dual-Energy Ablation and Conduction System Pacing Show Positive Early Outcomes
- Less Invasive Microcurrent Cardiac Device Improves Heart Failure Outcomes
- Partial Heart Transplantation Enables Growing Valve Replacement for Children
- Torqueable Microcatheters Enhance Navigation in Complex Coronary Lesions
- Early “Heart Training” Surgery Promotes Regeneration in Pediatric Heart Failure
- Transcatheter Venous Arterialization Improves Outcomes in No-Option Limb Ischemia Patients
- CE-Marked Stapler Designed to Improve Staple Line Integrity
- Smart Fracture Implant Monitors Healing and Delivers Adaptive Support
- Pulsed Field Ablation Technology Showcases One-Year AF Outcomes
- Novel GERD Device Demonstrates Long-Term Safety in Real-World Study
- Flexible Graphene Cortical Interface Enables Real-Time Mapping During Tumor Surgery
Channels
Artificial Intelligence
view channel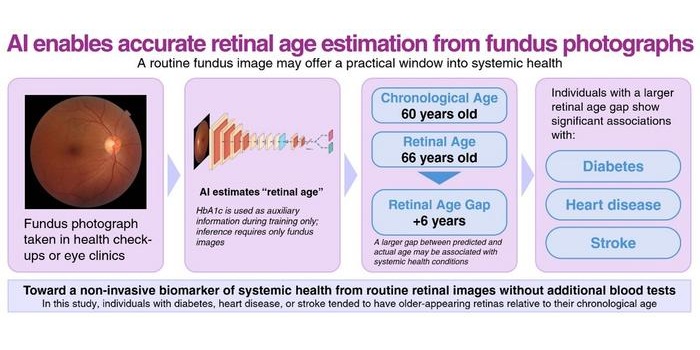
AI Model Uses Eye Imaging to Identify Risk of Major Systemic Diseases
Early detection of systemic disease risk remains a persistent challenge in population health screening. Cardiometabolic conditions such as diabetes, heart disease, and stroke often progress without symptoms... Read more
AI Platform Interprets Real-Time Wearable Data for Parkinson’s Management
Parkinson’s disease presents fluctuating motor and non-motor symptoms that complicate day-to-day self-management and clinical decision-making. Care teams require timely, longitudinal insight into medication... Read moreCritical Care
view channel
Blood-Filtering Device May Prolong Pregnancy in Severe Early Preeclampsia
Preeclampsia is a hypertensive disorder of pregnancy that can progress rapidly and threaten the lives of both mother and fetus. In its severe early form, often before 34 weeks’ gestation, clinicians frequently... Read more
AI Tool Predicts In-Hospital Cardiac Arrest Minutes in Advance
Sudden cardiac arrest, the abrupt loss of heart function, often arises without clear warning in hospitalized patients. Clinicians must sift through faint signals from routine monitoring while limiting... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channelBusiness
view channel
Johnson & Johnson Launches AI-Driven Cardiac Mapping System
Johnson & Johnson has introduced the CARTOSOUND SONATA Module for the CARTO System at the Heart Rhythm Society (HRS) 2026 meeting in Chicago. The module uses artificial intelligence with the CARTO... Read more