Team-Based Approach Reduces Monitor Alarm Fatigue
|
By HospiMedica International staff writers Posted on 02 Dec 2014 |
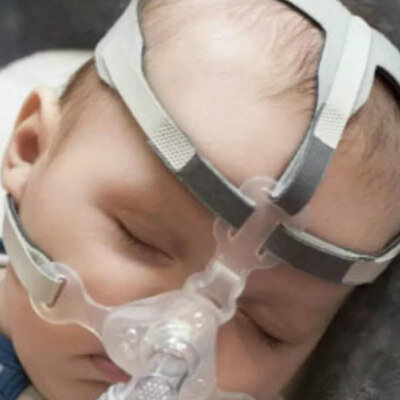
A new study describes a standardized, team-based approach to reduce cardiac monitor alarms and subsequent "alarm fatigue," in which caregivers become desensitized to the ever-present beeping.
Researchers at Cincinnati Children's Hospital Medical Center (OH, USA) developed a standardized cardiac monitor care process (CMCP) for a 24-bed pediatric bone marrow transplant unit. The project involved a process for initial ordering of monitor parameters based on age-appropriate standards, daily replacement of electrodes in a manner that was pain-free for patients, individualized daily assessment of monitor parameters, and an appropriate method for discontinuation of monitor use. They then used a model to design, test, and implement changes.
The results showed that from January to November 2013, compliance with each of the four individual components of the CMCP increased, with the overall compliance increasing from a median of 38% to 95%. During this time, the median number of alarms per patient-day decreased from 180 to just 40. The researchers therefore recommended a team-based approach to monitor care. The study was published online on November 10, 2104, in the journal Pediatrics.
“Cardiac monitors constitute the majority of alarms throughout the hospital. We think our approach to reducing monitor alarms can serve as a model for other hospitals throughout the country,” said lead author Christopher Dandoy, MD. “With fewer false alarms, the staff can address significant alarms more promptly. We believe the roles and responsibilities entailed in this process can be applied to most units with cardiac monitor care.”
The constant sounds of alarms and noises from blood pressure machines, ventilators, and cardiac monitors causes a "tuning out" of the sounds due to the brain adjusting to stimulation, an issue plaguing hospitals, home care providers, nursing homes, and other medical facilities alike. On April 18, 2013, the Joint Commission (Oakbrook Terrace, IL, USA) issued a sentinel event alert that highlighted the widespread problem of alarm fatigue. Recommendations issued included establishing guidelines to tailor alarm settings, training all members of the clinical team on safe use of alarms, and sharing information about alarm-related incidents.
Related Links:
Cincinnati Children's Hospital Medical Center
Joint Commission
Researchers at Cincinnati Children's Hospital Medical Center (OH, USA) developed a standardized cardiac monitor care process (CMCP) for a 24-bed pediatric bone marrow transplant unit. The project involved a process for initial ordering of monitor parameters based on age-appropriate standards, daily replacement of electrodes in a manner that was pain-free for patients, individualized daily assessment of monitor parameters, and an appropriate method for discontinuation of monitor use. They then used a model to design, test, and implement changes.
The results showed that from January to November 2013, compliance with each of the four individual components of the CMCP increased, with the overall compliance increasing from a median of 38% to 95%. During this time, the median number of alarms per patient-day decreased from 180 to just 40. The researchers therefore recommended a team-based approach to monitor care. The study was published online on November 10, 2104, in the journal Pediatrics.
“Cardiac monitors constitute the majority of alarms throughout the hospital. We think our approach to reducing monitor alarms can serve as a model for other hospitals throughout the country,” said lead author Christopher Dandoy, MD. “With fewer false alarms, the staff can address significant alarms more promptly. We believe the roles and responsibilities entailed in this process can be applied to most units with cardiac monitor care.”
The constant sounds of alarms and noises from blood pressure machines, ventilators, and cardiac monitors causes a "tuning out" of the sounds due to the brain adjusting to stimulation, an issue plaguing hospitals, home care providers, nursing homes, and other medical facilities alike. On April 18, 2013, the Joint Commission (Oakbrook Terrace, IL, USA) issued a sentinel event alert that highlighted the widespread problem of alarm fatigue. Recommendations issued included establishing guidelines to tailor alarm settings, training all members of the clinical team on safe use of alarms, and sharing information about alarm-related incidents.
Related Links:
Cincinnati Children's Hospital Medical Center
Joint Commission
Latest Critical Care News
- “Intelligent Tattoo” Method Detects Early Melanoma Signals
- Implantable Wireless Light Device Advances Bladder Cancer Treatment
- Reusable Intermittent Catheters Reduce Antibiotic Use Without Increasing Urinary Tract Infections
- Smart Wristband Technology Detects Cardiac Arrest and Alerts Responders
- FDA-Cleared Home Sleep Test Enables Multi-Night Diagnosis of Sleep Apnea
- AI-Enabled Wearable Patches Reveal Undetected Hormone Disruption in Infertility
- AI Method Turns Toe Scan into Rapid PAD Screening Tool
- Integrated AI Pulmonary Workflow System Streamlines Detection and Follow-Up
- AI Model Predicts 10-Year Stroke Risk from Standard ECG
- Portable Ultrasound Tool Quantifies Liver Fat with MRI-Like Accuracy
- AI Tool Predicts Risk of Out-of-Hospital Cardiac Arrest
- Implantable Cytokine Device Enables Localized Immunotherapy for Ovarian Cancer
- Wearable Defibrillator Supports Quicker Beta-Blocker Optimization in Women
- High-Frequency Ultrasound Disables Viruses While Sparing Human Cells
- New Nasal Spray Enables Prehospital Neuroprotection in Ischemic Stroke
- AI-Enhanced ECG Screens for Heart Failure Risk in Resource-Limited Settings
Channels
Artificial Intelligence
view channel
Automated Phone Speech Test Identifies Alzheimer’s Pathology for Prescreening
Alzheimer’s disease assessment and trial recruitment often rely on costly, invasive biomarker testing and clinic-based cognitive evaluations, limiting scalability as populations age. Providers and trial... Read more
FDA-Cleared AI System Detects Sepsis Earlier and Reduces Mortality
Sepsis remains one of the deadliest complications for hospitalized patients, in part because its early signs overlap with other conditions. Each hour of delayed recognition measurably decreases survival,... Read moreSurgical Techniques
view channel
Pink Noise Stimulation Approach Could Support Safer Anesthesia
Maintaining stable unconsciousness during general anesthesia while minimizing drug exposure remains a core perioperative challenge. Sudden nociceptive surges can disrupt anesthetic depth, increasing neurological... Read more
Surgical Robotic System Gains CE Mark for Minimally Invasive Procedures
Cornerstone Robotics’ (CSR; Hong Kong, China) Sentire Endoscopic Surgical System (Sentire Surgical System) has received European Union CE mark certification under the Medical Device Regulation (MDR) for... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read moreHealth IT
view channel
AI-Native EHR Achieves EU Medical Device Certification
InterSystems (Boston, MA, USA) announced that its IntelliCare electronic health record (EHR) solutions have been certified as Class IIa medical devices under the European Union Medical Device Regulation... Read more
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read morePoint of Care
view channel