Antibiotics Could Avert Surgery in Uncomplicated Appendicitis
|
By HospiMedica International staff writers Posted on 28 Jun 2015 |
A new study suggests most patients with an inflamed appendix could be treated with antibiotics and avoid an appendectomy.
Researchers at the University of Eastern Finland (Joensuu, Finland), Turku University Hospital (Finland), and other institutions conducted a study involving 530 patients (18–60 years of age) in Finland with uncomplicated acute appendicitis, as confirmed by computed tomography (CT). Patients were randomly assigned to standard open appendectomy or to an antibiotic regimen that involved intravenous ertapenem for three days, followed by seven days of oral levofloxacin and metronidazole. End points were surgical success or hospital discharge without the need for surgery, and no recurrent appendicitis during the follow-up period.
The results showed that of the 273 patients in the surgical group, all but one underwent successful appendectomy, resulting in a success rate of 99.6%. Of the 256 patients available for follow-up in the antibiotic group, 72.7% did not require subsequent surgery. Of those that did require surgery, 82.9% had uncomplicated appendicitis, 10% had complicated acute appendicitis, and 7.1% did not have appendicitis but received appendectomy for suspected recurrence. There were no intra-abdominal abscesses or other major complications associated with delayed appendectomy. The study was published on June 16, 2015, in the Journal of the American Medical Association (JAMA).
“For more than a century, appendectomy has been the standard treatment; but about 80% of patients with an inflamed appendix don't need to have their appendix surgically removed, and those who ultimately do need the surgery aren't hurt by waiting,” said lead author Paulina Salminen, MD, PhD, of Turku University Hospital. “Now we know that only a small proportion of appendicitis patients need an emergency operation.”
“It's kind of lost to history why people started doing appendectomies, but it has become so routine that when someone comes in with appendicitis they get whisked into the operating room. However, a lot has changed in 130 years, for example the ability to diagnose appendicitis; it's almost perfect with CT scans,” said Edward Livingston, MD, coauthor of an accompanying editorial and deputy editor of JAMA. “I am a surgeon and I hope to get through life without ever having an operation. So if I were given the option of taking antibiotics and not have surgery, I would take antibiotics in a heartbeat.”
Appendectomy is the surgical removal of the vermiform appendix. The procedure is normally performed as an emergency procedure, when the patient is suffering from acute appendicitis. In the absence of surgical facilities, intravenous antibiotics are used to delay or avoid the onset of sepsis. In some cases the appendicitis resolves completely; more often, an inflammatory mass forms around the appendix, causing transruptural flotation.
Related Links:
University of Eastern Finland
Turku University Hospital
Researchers at the University of Eastern Finland (Joensuu, Finland), Turku University Hospital (Finland), and other institutions conducted a study involving 530 patients (18–60 years of age) in Finland with uncomplicated acute appendicitis, as confirmed by computed tomography (CT). Patients were randomly assigned to standard open appendectomy or to an antibiotic regimen that involved intravenous ertapenem for three days, followed by seven days of oral levofloxacin and metronidazole. End points were surgical success or hospital discharge without the need for surgery, and no recurrent appendicitis during the follow-up period.
The results showed that of the 273 patients in the surgical group, all but one underwent successful appendectomy, resulting in a success rate of 99.6%. Of the 256 patients available for follow-up in the antibiotic group, 72.7% did not require subsequent surgery. Of those that did require surgery, 82.9% had uncomplicated appendicitis, 10% had complicated acute appendicitis, and 7.1% did not have appendicitis but received appendectomy for suspected recurrence. There were no intra-abdominal abscesses or other major complications associated with delayed appendectomy. The study was published on June 16, 2015, in the Journal of the American Medical Association (JAMA).
“For more than a century, appendectomy has been the standard treatment; but about 80% of patients with an inflamed appendix don't need to have their appendix surgically removed, and those who ultimately do need the surgery aren't hurt by waiting,” said lead author Paulina Salminen, MD, PhD, of Turku University Hospital. “Now we know that only a small proportion of appendicitis patients need an emergency operation.”
“It's kind of lost to history why people started doing appendectomies, but it has become so routine that when someone comes in with appendicitis they get whisked into the operating room. However, a lot has changed in 130 years, for example the ability to diagnose appendicitis; it's almost perfect with CT scans,” said Edward Livingston, MD, coauthor of an accompanying editorial and deputy editor of JAMA. “I am a surgeon and I hope to get through life without ever having an operation. So if I were given the option of taking antibiotics and not have surgery, I would take antibiotics in a heartbeat.”
Appendectomy is the surgical removal of the vermiform appendix. The procedure is normally performed as an emergency procedure, when the patient is suffering from acute appendicitis. In the absence of surgical facilities, intravenous antibiotics are used to delay or avoid the onset of sepsis. In some cases the appendicitis resolves completely; more often, an inflammatory mass forms around the appendix, causing transruptural flotation.
Related Links:
University of Eastern Finland
Turku University Hospital
Latest Surgical Techniques News
- Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
- Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
- Ultrasound Technology Aims to Replace Invasive BPH Procedures
- Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
- New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
- Robot-Assisted Brain Angiography Improves Procedural Outcomes
- Brain Mapping Technology Enhances Precision in Brain Tumor Resection
- Handheld Robotic System Expands Options for Total Knee Surgery
- VR Experience Reduces Patient Anxiety Before Kidney Stone Procedure
- Injectable Mini Livers Offer Hope for Patients Awaiting Transplant
- Pulsed Field Ablation Technology Cleared in Europe for Persistent AFib
- AI-Powered Imaging Brings Real-Time Margin Clarity to Breast Cancer Surgery
- Minimally Invasive Device Safely Treats Challenging Brain Aneurysms
- Surgical Robot Makes Complex Liver Tumor Surgery Safer and Less Invasive
- Neurostimulation Implant Reduces Seizure Burden in Drug-Resistant Epilepsy
- Minimally Invasive Procedure Effectively Treats Small Kidney Cancers
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel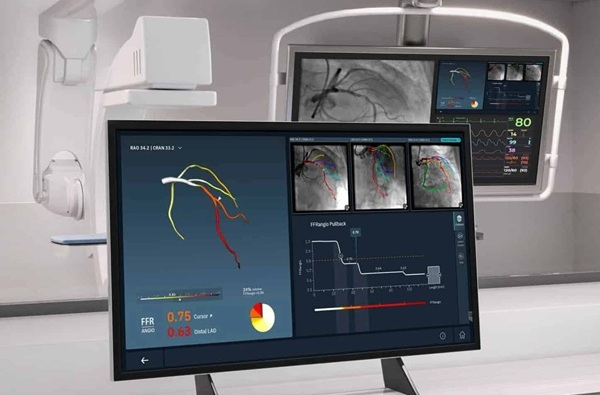
Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
Accurately determining whether a coronary stenosis limits blood flow is essential to guide percutaneous coronary intervention, yet wire-based physiologic testing remains underused due to added procedural... Read more
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel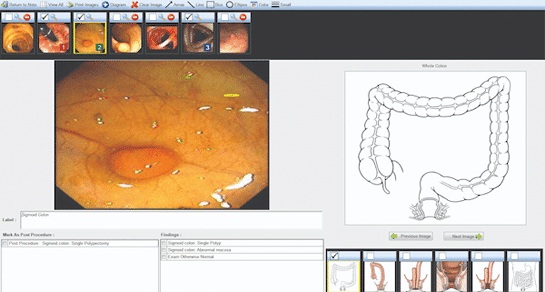
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel




















