Lung Simulations Could Improve Respiratory Treatment
|
By HospiMedica International staff writers Posted on 02 Aug 2015 |
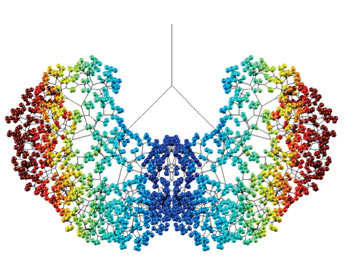
Image: Computer model of SRT delivered to an adult human lung; blue areas receive less (Photo courtesy of Prof. James Grotberg/U-M Engineering).
An innovative computer model that predicts the flow of liquids in human lungs could provide insight into the treatment of acute respiratory distress syndrome (ARDS).
ARDS is a life-threatening inflammation of the respiratory system that kills 74,000 adults each year in the United States alone. It is most common among patients with lung injury or sepsis, a whole-body inflammation caused by infection. Treatment involves surfactant replacement therapy (SRT) to make it easier for the lungs to inflate, similar to the therapy used in premature babies, who can lack the surfactant necessary to expand their lungs. While SRT has contributed to a dramatic reduction in mortality rates of premature babies, the attempt to implement the technology in adults has been largely unsuccessful.
To try and reveal why, researchers at the University of Michigan (U-M; Ann Arbor, USA) and Ecole Polytechnique (Palaiseau, France) developed a mathematical computer model that provided a three-dimensional (3D) image of exactly how SRT flowed through the lungs of patients in the three key trials that examined the technology. The first (1997) clinical study in adults showed promise, cutting mortality rate from 40% to 20%. But two larger studies in 2004 and 2011 showed no improvement in mortality, and the treatment was abandoned.
The computer model used fluid mechanical principals for 3-D modeling of the lung airway tree in both neonates and adults, showing how a liquid plug propagates through the tree from forced inspiration. In two separate modeling steps, they saw that the SRT plug deposits a coating film on the airway wall, and then splits unevenly at the bifurcation due to gravity. The model generates 3D images of the resulting acinar distribution and calculates two global indexes, efficiency and homogeneity.
When the researchers applied this engineering perspective to SRT, they saw one detail that set the successful 1997 study apart; a less concentrated version of medication was used. The SRT used in the 1997 study delivered the same dose of medication as the later studies, but it was dissolved in up to four times more liquid. The additional liquid helped the medication reach the tiny air sacs in the lungs. The study was published on July 13, 2015, in Proceedings of the National Academy of Sciences of the United States of America (PNAS).
“The medication needs to work its way from the trachea to tiny air sacs deep inside the lungs to be effective. This therapy is relatively straightforward in babies but more complex in adults, mostly because adult lungs are much bigger,” said lead author professor of biomedical engineering James Grotberg, MD, PhD, of the U-M College of Engineering. “The modeling technology could be used in other types of research as well, including more precise targeting of other medications in the lungs and projecting results from animal research to humans.”
Related Links:
University of Michigan
Ecole Polytechnique
ARDS is a life-threatening inflammation of the respiratory system that kills 74,000 adults each year in the United States alone. It is most common among patients with lung injury or sepsis, a whole-body inflammation caused by infection. Treatment involves surfactant replacement therapy (SRT) to make it easier for the lungs to inflate, similar to the therapy used in premature babies, who can lack the surfactant necessary to expand their lungs. While SRT has contributed to a dramatic reduction in mortality rates of premature babies, the attempt to implement the technology in adults has been largely unsuccessful.
To try and reveal why, researchers at the University of Michigan (U-M; Ann Arbor, USA) and Ecole Polytechnique (Palaiseau, France) developed a mathematical computer model that provided a three-dimensional (3D) image of exactly how SRT flowed through the lungs of patients in the three key trials that examined the technology. The first (1997) clinical study in adults showed promise, cutting mortality rate from 40% to 20%. But two larger studies in 2004 and 2011 showed no improvement in mortality, and the treatment was abandoned.
The computer model used fluid mechanical principals for 3-D modeling of the lung airway tree in both neonates and adults, showing how a liquid plug propagates through the tree from forced inspiration. In two separate modeling steps, they saw that the SRT plug deposits a coating film on the airway wall, and then splits unevenly at the bifurcation due to gravity. The model generates 3D images of the resulting acinar distribution and calculates two global indexes, efficiency and homogeneity.
When the researchers applied this engineering perspective to SRT, they saw one detail that set the successful 1997 study apart; a less concentrated version of medication was used. The SRT used in the 1997 study delivered the same dose of medication as the later studies, but it was dissolved in up to four times more liquid. The additional liquid helped the medication reach the tiny air sacs in the lungs. The study was published on July 13, 2015, in Proceedings of the National Academy of Sciences of the United States of America (PNAS).
“The medication needs to work its way from the trachea to tiny air sacs deep inside the lungs to be effective. This therapy is relatively straightforward in babies but more complex in adults, mostly because adult lungs are much bigger,” said lead author professor of biomedical engineering James Grotberg, MD, PhD, of the U-M College of Engineering. “The modeling technology could be used in other types of research as well, including more precise targeting of other medications in the lungs and projecting results from animal research to humans.”
Related Links:
University of Michigan
Ecole Polytechnique
Latest Critical Care News
- AI ECG Tool Detects Cardiac Amyloidosis for Early Screening
- Cuffless Wearable Enables Continuous Blood Pressure Monitoring for Hypertension Care
- AI ECG Index Tracks Pubertal Maturation in Children and Adolescents
- Noninvasive AI Tool Enables Pressure-Guided Heart Failure Management
- Regenerative Therapies Aim to Support Recovery After Traumatic Brain Injury
- Ring-Type Cuffless Monitor Becomes First Added to Official Hypertension Guidelines
- “Intelligent Tattoo” Method Detects Early Melanoma Signals
- Implantable Wireless Light Device Advances Bladder Cancer Treatment
- Reusable Intermittent Catheters Reduce Antibiotic Use Without Increasing Urinary Tract Infections
- Smart Wristband Technology Detects Cardiac Arrest and Alerts Responders
- FDA-Cleared Home Sleep Test Enables Multi-Night Diagnosis of Sleep Apnea
- AI-Enabled Wearable Patches Reveal Undetected Hormone Disruption in Infertility
- AI Method Turns Toe Scan into Rapid PAD Screening Tool
- Integrated AI Pulmonary Workflow System Streamlines Detection and Follow-Up
- AI Model Predicts 10-Year Stroke Risk from Standard ECG
- Portable Ultrasound Tool Quantifies Liver Fat with MRI-Like Accuracy
Channels
Artificial Intelligence
view channel
AI Platform Supports Noninvasive Remote Hemodynamic Monitoring in Heart Failure
Heart failure remains a leading cause of hospitalization in adults over 65, affecting more than 6.7 million people in the U.S. Clinicians often lose visibility into hemodynamic deterioration once patients... Read more
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read moreSurgical Techniques
view channel
Small Cryoprobe Outperforms Forceps in Lung Biopsy Trial
Accurate diagnosis of pulmonary nodules, post-transplant allograft dysfunction, and diffuse parenchymal lung disease depends on high-quality tissue obtained during bronchoscopy. Conventional forceps biopsy... Read more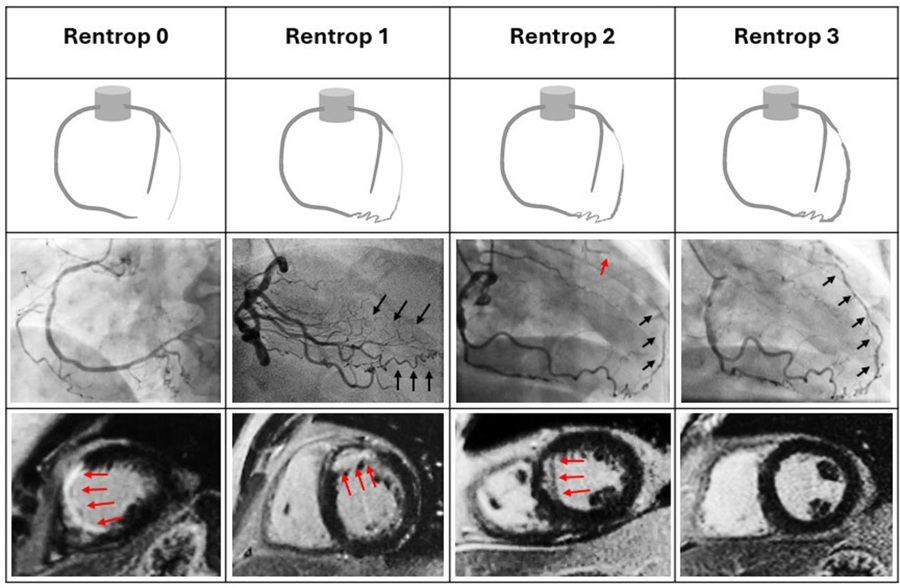
Natural Bypass Score May Guide Care in Chronic Coronary Blockages
Chronic total occlusion, a complete coronary artery blockage present for months, poses difficult treatment decisions in coronary artery disease. Opening these arteries is technically demanding and carries... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read moreHealth IT
view channel
AI-Native EHR Achieves EU Medical Device Certification
InterSystems (Boston, MA, USA) announced that its IntelliCare electronic health record (EHR) solutions have been certified as Class IIa medical devices under the European Union Medical Device Regulation... Read more
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read morePoint of Care
view channel
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more