US Announces Agreement on Health Data Interoperability
|
By HospiMedica International staff writers Posted on 13 Mar 2016 |
The US Department of Health and Human Services (HHS; Washington DC, USA) has fostered an agreement on health data interoperability between providers and healthcare information technology (IT) firms.
More than a dozen leading professional associations and stakeholder groups pledged to implement three core commitments that will improve the flow of health information to consumers and healthcare providers. The first commitment is to help consumers easily and securely access their electronic health record (EHR) information, direct it to any desired location, learn how their information can be shared and used, and be assured that this information will be effectively and safely used to benefit their health and that of their community.
The second commitment is no information blocking by helping providers share personal EHR information with other providers and their patients whenever permitted by law, and not block EHR information, defined as knowingly and unreasonably interfering with information sharing.
The third commitment is to implement federally recognized, national interoperability standards, policies, guidance, and practices for electronic health information, and adopt best practices including those related to privacy and security. Many of the market leaders are embracing the Office of the National Coordinator for Health IT (ONC) Interoperability Standards Advisory, a coordinated catalog of existing and emerging standards and implementation specifications that is updated annually in order to keep pace with developments in the health IT industry.
“Today I am announcing that companies providing 90% of electronic health records used by hospitals have made a public commitment to make data work better for consumers and providers,” said Sylvia Burwell, secretary of the HHS, at the annual meeting of the Healthcare Information and Management Systems Society (HIMSS). “Consumer access remains a challenge; it's great to have an electronic record, but if that record can't be easily accessed by doctors and patients because of funky technology, then we aren't consistently seeing the benefit.”
“We commend HHS for bringing so many stakeholders together, all of whom have an interest in using technology to result in a healthier and more efficient health care system,” said Steven Stack, MD, president of the American Medical Association (AMA; Chicago, IL, USA). “Patients and physicians are in this effort together because patients need easy access to their electronic health information, confident that it is secure and can be shared to benefit their health, and physicians need these electronic records to be interoperable to ensure that patients are receiving the best care possible.”
Many of the biggest health IT developers have already committed to using standardized application programming interfaces and Health Level 7 (HL7) fast health care interoperability resources (FHIR), so that user-friendly devices, such as smartphone and tablet apps, can quickly be made market-ready and compatible with one another. The use of a single shared standard for communicating among devices will make it easier for consumers to access their test results, track progress in their care, and communicate with their providers.
Related Links:
US Department of Health and Human Services
American Medical Association
More than a dozen leading professional associations and stakeholder groups pledged to implement three core commitments that will improve the flow of health information to consumers and healthcare providers. The first commitment is to help consumers easily and securely access their electronic health record (EHR) information, direct it to any desired location, learn how their information can be shared and used, and be assured that this information will be effectively and safely used to benefit their health and that of their community.
The second commitment is no information blocking by helping providers share personal EHR information with other providers and their patients whenever permitted by law, and not block EHR information, defined as knowingly and unreasonably interfering with information sharing.
The third commitment is to implement federally recognized, national interoperability standards, policies, guidance, and practices for electronic health information, and adopt best practices including those related to privacy and security. Many of the market leaders are embracing the Office of the National Coordinator for Health IT (ONC) Interoperability Standards Advisory, a coordinated catalog of existing and emerging standards and implementation specifications that is updated annually in order to keep pace with developments in the health IT industry.
“Today I am announcing that companies providing 90% of electronic health records used by hospitals have made a public commitment to make data work better for consumers and providers,” said Sylvia Burwell, secretary of the HHS, at the annual meeting of the Healthcare Information and Management Systems Society (HIMSS). “Consumer access remains a challenge; it's great to have an electronic record, but if that record can't be easily accessed by doctors and patients because of funky technology, then we aren't consistently seeing the benefit.”
“We commend HHS for bringing so many stakeholders together, all of whom have an interest in using technology to result in a healthier and more efficient health care system,” said Steven Stack, MD, president of the American Medical Association (AMA; Chicago, IL, USA). “Patients and physicians are in this effort together because patients need easy access to their electronic health information, confident that it is secure and can be shared to benefit their health, and physicians need these electronic records to be interoperable to ensure that patients are receiving the best care possible.”
Many of the biggest health IT developers have already committed to using standardized application programming interfaces and Health Level 7 (HL7) fast health care interoperability resources (FHIR), so that user-friendly devices, such as smartphone and tablet apps, can quickly be made market-ready and compatible with one another. The use of a single shared standard for communicating among devices will make it easier for consumers to access their test results, track progress in their care, and communicate with their providers.
Related Links:
US Department of Health and Human Services
American Medical Association
Latest Health IT News
- AI-Native EHR Achieves EU Medical Device Certification
- EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
- AI System Detects and Quantifies Chronic Subdural Hematoma
- Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
- Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Channels
Artificial Intelligence
view channel
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read more
Automated Phone Speech Test Identifies Alzheimer’s Pathology for Prescreening
Alzheimer’s disease assessment and trial recruitment often rely on costly, invasive biomarker testing and clinic-based cognitive evaluations, limiting scalability as populations age. Providers and trial... Read moreCritical Care
view channel
Ring-Type Cuffless Monitor Becomes First Added to Official Hypertension Guidelines
Detecting nocturnal and morning hypertension often requires out-of-office assessment, but conventional cuff-type monitors can disrupt sleep. New national guidance in South Korea expands 24-hour monitoring... Read more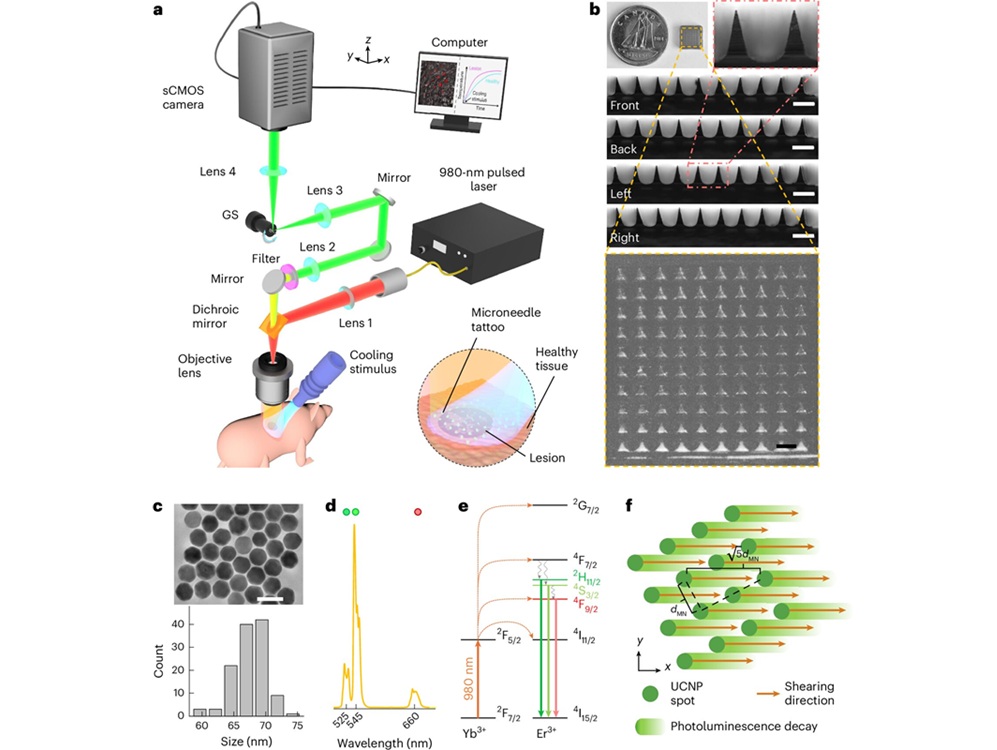
“Intelligent Tattoo” Method Detects Early Melanoma Signals
Melanoma is a lethal skin cancer in which earlier detection drives better outcomes. Current evaluation relies on visual inspection followed by biopsy, which can miss nascent lesions and lead to unnecessary... Read more
Reusable Intermittent Catheters Reduce Antibiotic Use Without Increasing Urinary Tract Infections
Intermittent self-catheterization, used to empty the bladder several times a day, can leave patients vulnerable to recurrent urinary tract infections and repeated antibiotic use. Reliance on single-use... Read moreSurgical Techniques
view channel
Fracture Plating System Combines Anatomical Fit with Streamlined Instrumentation
Fracture management involves diverse anatomies and injury patterns that can make plate fit and fixation strategy challenging. Surgeons need both intraoperative efficiency and flexibility, while hospitals... Read more
Pink Noise Stimulation Approach Could Support Safer Anesthesia
Maintaining stable unconsciousness during general anesthesia while minimizing drug exposure remains a core perioperative challenge. Sudden nociceptive surges can disrupt anesthetic depth, increasing neurological... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read morePoint of Care
view channel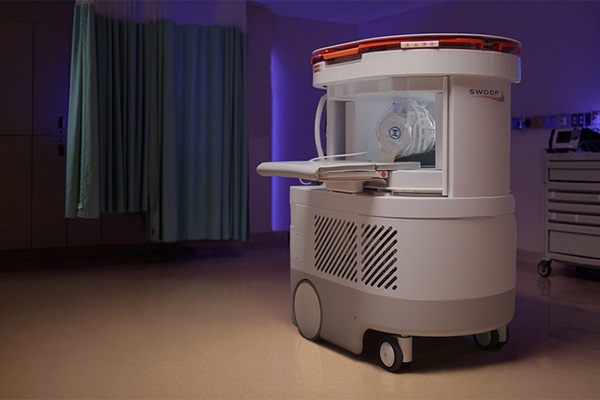
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more