Sensing Tool Measures Lung Function over the Phone
|
By HospiMedica International staff writers Posted on 12 May 2016 |

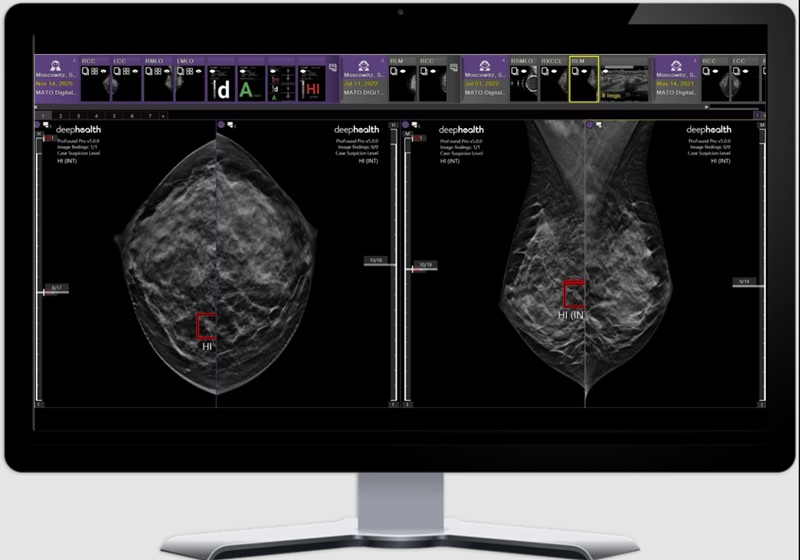
Image: A person using SpiroCall on a phone with and without a SpiroCall whistle (Photo courtesy of the University of Washington).
A new device allows lung function to be assessed from any phone, using the voice channel to transmit the sound of the spirometry effort.
Developed by researchers at the University of Washington (UW; Seattle, USA), the SpiroCall is a service that transmits an audio signal using the standard voice telephony channel. A server receives the data of degraded audio quality, calculates clinically relevant lung function measures using multiple regression algorithms, and reports the results using an audio message, text message, or both. The researchers also found several significant usability challenges more difficult to mitigate, such as how a user holds the phone, the distance from the user’s mouth to the phone, and how wide a user opens their mouth.
The researchers therefore designed a simple, low-cost 3D printed whistle accessory, which generates vortices as the user exhales through it, changing its resonating pitch in proportion to the flow rate. The whistle does not have any moving parts and is as simple as any spirometer mouthpiece. Advantages of the whistle include more consistent acoustic properties, audible sound at lower flow rates, removing the effect of distance from the user’s mouth, and precisely controlling mouth shape and phone orientation.
In a study to investigate viability of the call-in service approach with and without the whistle, the researchers evaluated SpiroCall in 50 patients, comparing it to approved spirometers and evaluating the effect of using the voice communication channel on performance. Each patient performed spirometry efforts with and without the whistle on two different phones, recording the audio through the cell phone network, and two smartphones recording the audio locally through an app. Participants also used two different sizes of vortex whistles to determine if different sizes work better for different individuals.
The results show that without a whistle, SpiroCall has a mean error of 7.2% for the four major clinically relevant lung function measures; for forced expiratory volume percentage (FEV1%), the mean error is 6.2%. With a whistle, SpiroCall has a mean error of 8.3% for the four measures, and 7.3% for FEV1%. Although the whistle shows higher average error in lung function estimates, it is more consistent for people with lower lung function and produces fewer overestimations. The study was presented at the Association for Computing Machinery conference, held during May 2016 in San Jose (CA, USA).
"People have to manage chronic lung diseases for their entire lives, so there's a real need to have a device that allows patients to accurately monitor their condition at home without having to constantly visit a medical clinic,” said lead author Mayank Goel, MSc, a computer science and engineering doctoral student. “Because this project has been around for four years, we've been able to talk to a lot of patients about how they're able to use the technology, and that feedback has really helped us make smart improvement.”
Related Links:
University of Washington
Developed by researchers at the University of Washington (UW; Seattle, USA), the SpiroCall is a service that transmits an audio signal using the standard voice telephony channel. A server receives the data of degraded audio quality, calculates clinically relevant lung function measures using multiple regression algorithms, and reports the results using an audio message, text message, or both. The researchers also found several significant usability challenges more difficult to mitigate, such as how a user holds the phone, the distance from the user’s mouth to the phone, and how wide a user opens their mouth.
The researchers therefore designed a simple, low-cost 3D printed whistle accessory, which generates vortices as the user exhales through it, changing its resonating pitch in proportion to the flow rate. The whistle does not have any moving parts and is as simple as any spirometer mouthpiece. Advantages of the whistle include more consistent acoustic properties, audible sound at lower flow rates, removing the effect of distance from the user’s mouth, and precisely controlling mouth shape and phone orientation.
In a study to investigate viability of the call-in service approach with and without the whistle, the researchers evaluated SpiroCall in 50 patients, comparing it to approved spirometers and evaluating the effect of using the voice communication channel on performance. Each patient performed spirometry efforts with and without the whistle on two different phones, recording the audio through the cell phone network, and two smartphones recording the audio locally through an app. Participants also used two different sizes of vortex whistles to determine if different sizes work better for different individuals.
The results show that without a whistle, SpiroCall has a mean error of 7.2% for the four major clinically relevant lung function measures; for forced expiratory volume percentage (FEV1%), the mean error is 6.2%. With a whistle, SpiroCall has a mean error of 8.3% for the four measures, and 7.3% for FEV1%. Although the whistle shows higher average error in lung function estimates, it is more consistent for people with lower lung function and produces fewer overestimations. The study was presented at the Association for Computing Machinery conference, held during May 2016 in San Jose (CA, USA).
"People have to manage chronic lung diseases for their entire lives, so there's a real need to have a device that allows patients to accurately monitor their condition at home without having to constantly visit a medical clinic,” said lead author Mayank Goel, MSc, a computer science and engineering doctoral student. “Because this project has been around for four years, we've been able to talk to a lot of patients about how they're able to use the technology, and that feedback has really helped us make smart improvement.”
Related Links:
University of Washington
Latest Health IT News
- EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
- AI System Detects and Quantifies Chronic Subdural Hematoma
- Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
- Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
- Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
- Smartwatches Could Detect Congestive Heart Failure
Channels
Artificial Intelligence
view channel
FDA-Cleared AI System Detects Sepsis Earlier and Reduces Mortality
Sepsis remains one of the deadliest complications for hospitalized patients, in part because its early signs overlap with other conditions. Each hour of delayed recognition measurably decreases survival,... Read moreFacial Image Analysis Tracks Biological Aging, Predicts Cancer Outcomes
Biological aging is the progressive loss of physiological function that may diverge from chronological age. In cancer care, clinicians need simple tools that reflect dynamic changes in patient resilience... Read moreSurgical Techniques
view channel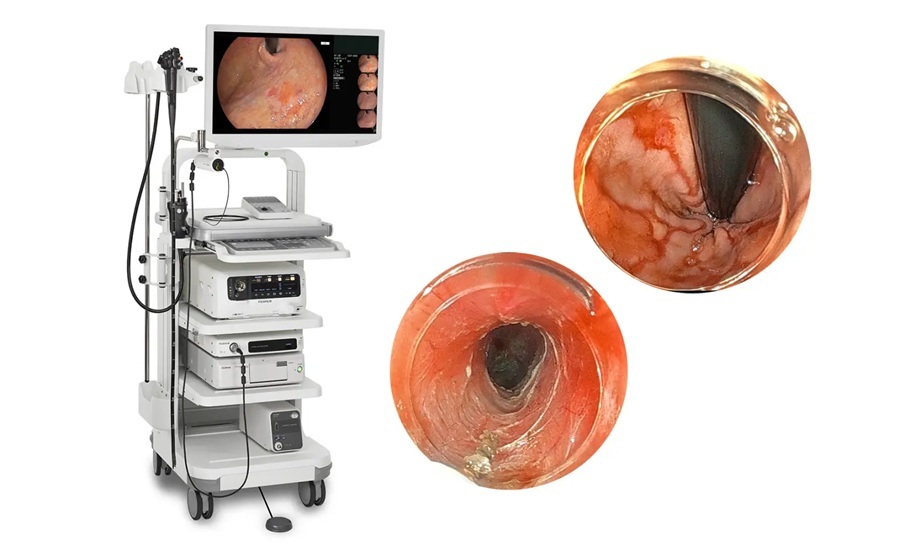
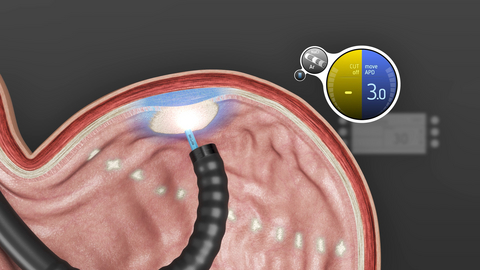
Advanced Endoscopy Platform Targets Challenging Upper GI Procedures
Fujifilm’s ELUXEO 8000 Endoscopic Imaging System, used with the EG-840TP ultra‑slim therapeutic gastroscope, was named “Best New Endoscopy Technology Solution” in the 10th annual MedTech Breakthrough Awards program.... Read more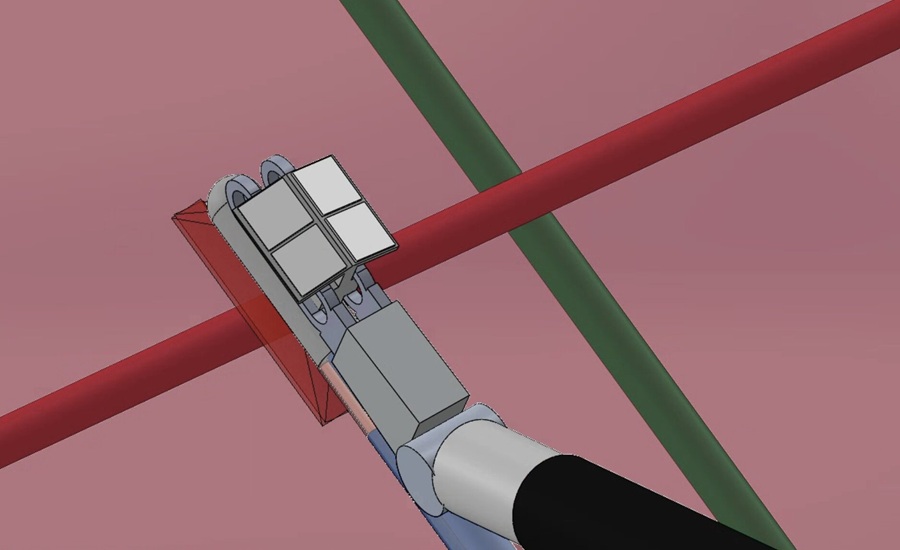
Photoacoustic Imaging System Maps Hidden Nerves and Vessels in Robotic Laparoscopy
Hidden neurovascular structures can be difficult to visualize during robot-assisted laparoscopy, increasing the risk of iatrogenic injury. Such injuries can cause hemorrhage, neurological deficits, and... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channel
Point-of-Care Viscoelastic Testing System Supports Obstetric Bleeding Management
HemoSonics (Durham, NC, USA) announced on May 5, 2026 that the company's Quantra Hemostasis System for Obstetric Procedures won Silver in the 2026 Edison Awards in the Women’s Health and Reproductive Innovations... Read moreBusiness
view channel
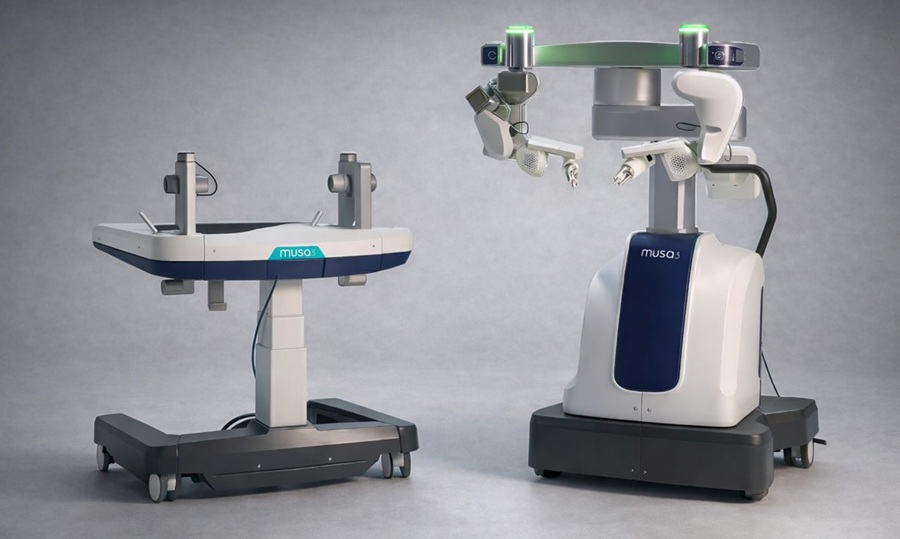
Olympus Partnership Aims to Expand Access to Robot-Assisted Endoscopic Therapy
Olympus has signed an exclusive global distribution agreement with EndoRobotics Co., Ltd., under which robot-assisted technologies developed by EndoRobotics will be distributed worldwide as part of the... Read more