Hospitals Face Increased Risk of Data Breaches
|
By HospiMedica International staff writers Posted on 26 Apr 2017 |
A new study suggests that as health providers adopt health information technology, they increasingly suffer from data breaches.
Researchers at Michigan State University, Ball State University, and Johns Hopkins University conducted a retrospective data analysis of data breaches reported to the U.S. Department of Health and Human Services between October 2009 and December 2016. By law, U.S. hospitals covered by the Health Insurance Portability and Accountability Act (HIPPA), must notify the HHS of any breach affecting 500 or more individuals within 60 days of the discovery of the breach.
The results revealed that during the study period, healthcare providers reported 1,225 of the 1,798 recorded breaches, while business associates, health plans, and healthcare clearinghouses reported the remaining 573 data breaches. Of these, 257 breaches were reported by 216 hospitals; importantly, 33 hospitals experienced more than one breach, many of them large, major teaching hospitals, such as UC Davis Medical Center (CA, USA) and Henry Ford Hospital (Detroit, MI, USA). The study was published on April 3, 2017, in JAMA Internal Medicine.
“This research reinforces the critical trade-off patient’s face: healthcare systems having access to information they need, versus a hacker planning to spend your savings at Best Buy,” said lead author Xuefeng Jiang, PhD, of MSU, and colleagues. “While the law requires health care professionals and systems to cross-share patient data, the more people who can access data, the less secure it is.”
A data breach is defined as a security incident in which sensitive, protected, or confidential data is copied, transmitted, viewed, stolen or used by an individual unauthorized to do so. Data breaches may involve financial information such as credit card or bank details, personal health information, personally identifiable information, trade secrets of corporations, or intellectual property.
Researchers at Michigan State University, Ball State University, and Johns Hopkins University conducted a retrospective data analysis of data breaches reported to the U.S. Department of Health and Human Services between October 2009 and December 2016. By law, U.S. hospitals covered by the Health Insurance Portability and Accountability Act (HIPPA), must notify the HHS of any breach affecting 500 or more individuals within 60 days of the discovery of the breach.
The results revealed that during the study period, healthcare providers reported 1,225 of the 1,798 recorded breaches, while business associates, health plans, and healthcare clearinghouses reported the remaining 573 data breaches. Of these, 257 breaches were reported by 216 hospitals; importantly, 33 hospitals experienced more than one breach, many of them large, major teaching hospitals, such as UC Davis Medical Center (CA, USA) and Henry Ford Hospital (Detroit, MI, USA). The study was published on April 3, 2017, in JAMA Internal Medicine.
“This research reinforces the critical trade-off patient’s face: healthcare systems having access to information they need, versus a hacker planning to spend your savings at Best Buy,” said lead author Xuefeng Jiang, PhD, of MSU, and colleagues. “While the law requires health care professionals and systems to cross-share patient data, the more people who can access data, the less secure it is.”
A data breach is defined as a security incident in which sensitive, protected, or confidential data is copied, transmitted, viewed, stolen or used by an individual unauthorized to do so. Data breaches may involve financial information such as credit card or bank details, personal health information, personally identifiable information, trade secrets of corporations, or intellectual property.
Latest Health IT News
- AI-Native EHR Achieves EU Medical Device Certification
- EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
- AI System Detects and Quantifies Chronic Subdural Hematoma
- Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
- Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Channels
Artificial Intelligence
view channel
AI Platform Supports Noninvasive Remote Hemodynamic Monitoring in Heart Failure
Heart failure remains a leading cause of hospitalization in adults over 65, affecting more than 6.7 million people in the U.S. Clinicians often lose visibility into hemodynamic deterioration once patients... Read more
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read moreCritical Care
view channel
Smartphone Heart Rhythm App Reduces Unnecessary Cardioversion Procedures
Atrial fibrillation, an irregular and often rapid heart rhythm, is the most common arrhythmia in adults. Elective electrical cardioversion is frequently canceled on the day of treatment when patients revert... Read more
New Practice Guidance Supports Prostatic Artery Embolization for BPH Symptoms
Benign prostatic hyperplasia is a noncancerous enlargement of the prostate that can cause lower urinary tract symptoms and impair daily functioning. These symptoms erode sleep, productivity, and sexual... Read more
Bedside CSF Monitor Detects Early Infection in Fluid Drains
External drainage of cerebrospinal fluid (CSF) after traumatic brain injury, hydrocephalus, or hemorrhage carries a significant risk of infection. These infections can prolong intensive care, cause severe... Read more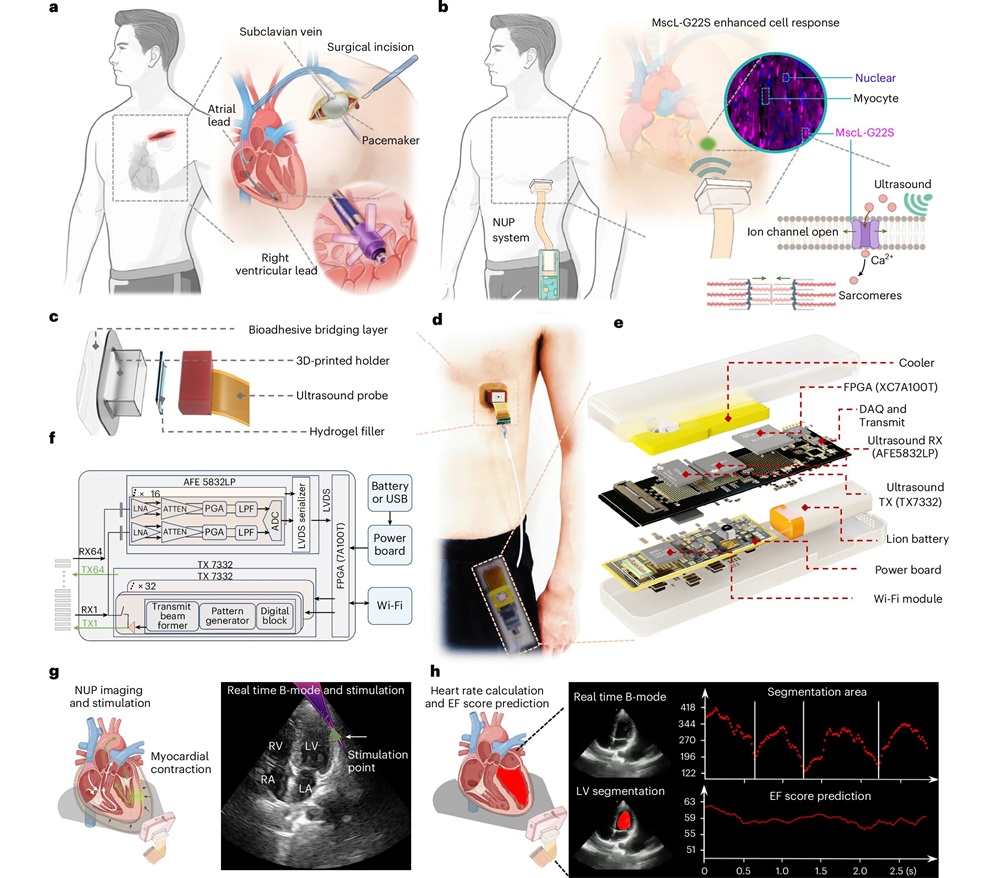
Wearable Ultrasound Patch Noninvasively Paces Heart to Stabilize Arrhythmias
Cardiac arrhythmias, including slow and irregular heart rhythms, often require pacemakers that are surgically implanted. While effective, implants carry procedural risks and long-term device maintenance burdens.... Read moreSurgical Techniques
view channel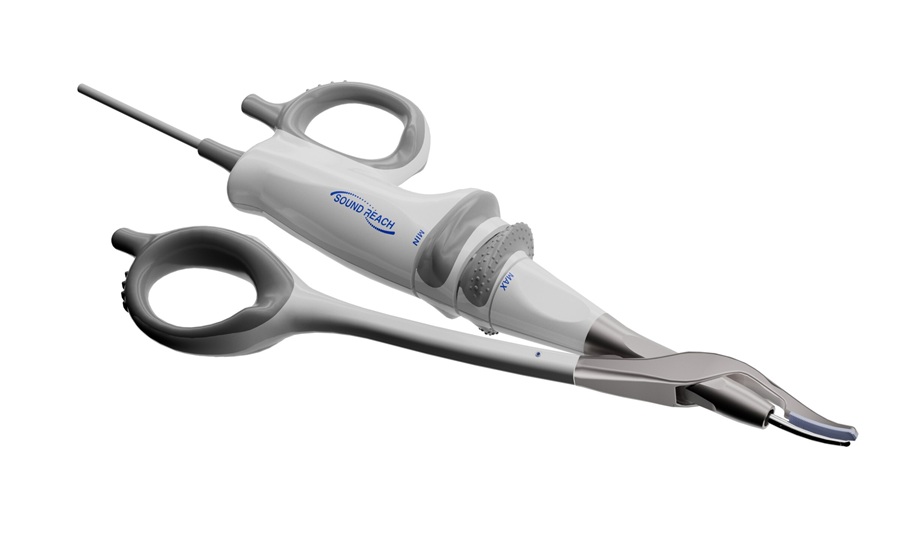
CE-Marked Ultrasonic Shears Streamline Breast and Thyroid Surgery
Thyroid and breast surgeries are often performed in confined anatomical spaces near critical structures, making precise dissection and controlled thermal management essential. As the global disease burden... Read more
3D Map of Heart Electrical Wiring Aims to Guide Congenital Heart Repair
Tetralogy of Fallot is one of the most common congenital heart problems and often requires surgery in infancy. Many survivors later develop conduction abnormalities because the cardiac electrical system... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read morePoint of Care
view channel
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more