CLND Fails to Improve Melanoma Survival Rates
|
By HospiMedica International staff writers Posted on 19 Jun 2017 |
A new study shows that immediate completion lymph-node dissection (CLND) does not increase survival among patients with melanoma and sentinel-node metastases.
Researchers at the John Wayne Cancer Institute (JWCI; Santa Monica, CA, USA), Sentara CarePlex Hospital (Hampton, VA, USA), and other institutions worldwide conducted a study that randomly assigned 1,934 patients with sentinel-node metastases--detected via standard pathological assessment or a multimarker molecular assay--to immediate CLND or to an observation group monitored with ultrasonography. Main outcomes and measures were melanoma-specific survival, disease-free survival, and cumulative rate of non-sentinel-node metastasis.
The results showed that Immediate CLND was not associated with increased melanoma-specific survival. In the per-protocol analysis, the mean three-year rate of melanoma-specific survival was similar in the dissection group and the observation group (86%) at a median follow-up of 43 months. The mean rate of disease-free survival was slightly higher in the dissection group (68%) than in the observation group (63%) at three years. Lymphedema was observed in 24.1% of the patients in the dissection group and in 6.3% of those in the observation group. The study was published on June 8, 2017, in the New England Journal of Medicine (NEJM).
“Although the completion dissections did not help overall survival, they did have some value. By examining the dissected lymph nodes, physicians were able to better gauge how extensively the cancer had spread and to lengthen the time that their patients were disease-free. But those advantages did not translate into longer lives,” said lead author Mark Faries, MD, of JWCI. “The new findings likely will result in many fewer of these procedures being performed around the world. The results also will likely affect the design of many current and future clinical trials of medical therapies in melanoma.”
Lymph nodes, located throughout the body, serve as biologic filters that contain immune cells that fight infection and clean the blood. When cancer cells break away from a tumor, the cells can travel through the lymph system; sentinel node surgery allows the surgeon to remove the nodes to determine cancer spread. As human nodes are only 5 mm in size, they are difficult to discern from the surrounding tissue during surgery. Furthermore, even when surgeons are able to map the location of the nodes, there is no current technique that indicates whether or not the lymph nodes contain cancer, requiring removal of more lymph nodes than necessary.
Related Links:
John Wayne Cancer Institute
Sentara CarePlex Hospital
Researchers at the John Wayne Cancer Institute (JWCI; Santa Monica, CA, USA), Sentara CarePlex Hospital (Hampton, VA, USA), and other institutions worldwide conducted a study that randomly assigned 1,934 patients with sentinel-node metastases--detected via standard pathological assessment or a multimarker molecular assay--to immediate CLND or to an observation group monitored with ultrasonography. Main outcomes and measures were melanoma-specific survival, disease-free survival, and cumulative rate of non-sentinel-node metastasis.
The results showed that Immediate CLND was not associated with increased melanoma-specific survival. In the per-protocol analysis, the mean three-year rate of melanoma-specific survival was similar in the dissection group and the observation group (86%) at a median follow-up of 43 months. The mean rate of disease-free survival was slightly higher in the dissection group (68%) than in the observation group (63%) at three years. Lymphedema was observed in 24.1% of the patients in the dissection group and in 6.3% of those in the observation group. The study was published on June 8, 2017, in the New England Journal of Medicine (NEJM).
“Although the completion dissections did not help overall survival, they did have some value. By examining the dissected lymph nodes, physicians were able to better gauge how extensively the cancer had spread and to lengthen the time that their patients were disease-free. But those advantages did not translate into longer lives,” said lead author Mark Faries, MD, of JWCI. “The new findings likely will result in many fewer of these procedures being performed around the world. The results also will likely affect the design of many current and future clinical trials of medical therapies in melanoma.”
Lymph nodes, located throughout the body, serve as biologic filters that contain immune cells that fight infection and clean the blood. When cancer cells break away from a tumor, the cells can travel through the lymph system; sentinel node surgery allows the surgeon to remove the nodes to determine cancer spread. As human nodes are only 5 mm in size, they are difficult to discern from the surrounding tissue during surgery. Furthermore, even when surgeons are able to map the location of the nodes, there is no current technique that indicates whether or not the lymph nodes contain cancer, requiring removal of more lymph nodes than necessary.
Related Links:
John Wayne Cancer Institute
Sentara CarePlex Hospital
Latest Surgical Techniques News
- Stretchable Bioelectronic Implant Lowers Blood Pressure in Preclinical Study
- FDA-Cleared Nerve Stimulator Advances Intraoperative Peripheral Nerve Assessment
- Intravascular Lithotripsy Catheter Advances Treatment of Calcified Coronary Disease
- Handheld AI Endomicroscope Enables Real-Time Precancer Detection at Point of Care
- Photoacoustic Imaging System Maps Hidden Nerves and Vessels in Robotic Laparoscopy
- Smart Soft Sensors Provide Real-Time Force Feedback in Minimally Invasive Surgery
- Advanced Endoscopy Platform Targets Challenging Upper GI Procedures
- Ultrasonic Fine-Needle Biopsy Tool Improves Salivary Gland Tumor Diagnosis
- Robotic Microsurgery System Gains CE Mark for Clinical Use in Europe
- New Endoscopic Device Offers Minimally Invasive Approach to Obesity Management
- Handheld Probe Enables Real-Time Tumor Mapping in Breast-Conserving Surgery
- Robotic Surgical System Enables Gastric Bypass in Space-Constrained Operating Rooms
- Optical Wireless Link Enables Cable-Free 4K Endoscopic Imaging
- Patient-Specific 3D-Printed Guide Improves Precision in Breast-Conserving Surgery
- Glasses-Free 3D Imaging Software Receives FDA Clearance for Surgical Planning
- Noninvasive Cardiac Radiotherapy Reduces Ventricular Tachycardia Events
Channels
Artificial Intelligence
view channel
FDA-Cleared AI System Detects Sepsis Earlier and Reduces Mortality
Sepsis remains one of the deadliest complications for hospitalized patients, in part because its early signs overlap with other conditions. Each hour of delayed recognition measurably decreases survival,... Read moreFacial Image Analysis Tracks Biological Aging, Predicts Cancer Outcomes
Biological aging is the progressive loss of physiological function that may diverge from chronological age. In cancer care, clinicians need simple tools that reflect dynamic changes in patient resilience... Read moreCritical Care
view channel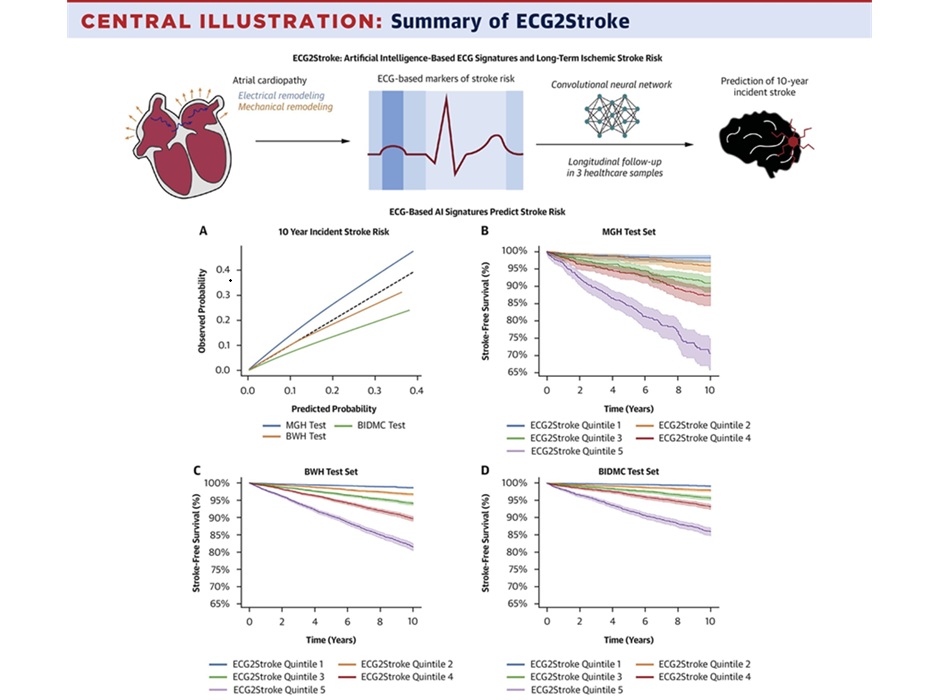
AI Model Predicts 10-Year Stroke Risk from Standard ECG
Stroke remains a major cause of death and long-term disability worldwide. Clinicians need scalable tools to identify people who face sustained risk years before an event occurs. Existing clinical scores... Read more
Implantable Cytokine Device Enables Localized Immunotherapy for Ovarian Cancer
High-grade serous ovarian carcinoma, the most lethal form of ovarian cancer, often disseminates throughout the peritoneal cavity and resists standard therapies. Systemic interleukin-2 (IL-2) can activate... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channel
Point-of-Care Viscoelastic Testing System Supports Obstetric Bleeding Management
HemoSonics (Durham, NC, USA) announced on May 5, 2026 that the company's Quantra Hemostasis System for Obstetric Procedures won Silver in the 2026 Edison Awards in the Women’s Health and Reproductive Innovations... Read moreBusiness
view channel
Olympus Partnership Aims to Expand Access to Robot-Assisted Endoscopic Therapy
Olympus has signed an exclusive global distribution agreement with EndoRobotics Co., Ltd., under which robot-assisted technologies developed by EndoRobotics will be distributed worldwide as part of the... Read more