Laparoscopic Approach Cuts Pancreatitis Complication Rates
|
By HospiMedica International staff writers Posted on 18 Jul 2017 |
Minimally invasive transplant surgery reduces operative times, length of stay, and promises quicker opioid independence for patients suffering from chronic pancreatitis (CP).
Developed at Johns Hopkins University (JHU, Baltimore, MD, USA), laparoscopic total pancreatectomy with islet cell auto transplantation (TPIAT) involves surgically removing the pancreas and reconstructing the gastrointestinal tract. While removing the pancreas often relieves the severe abdominal pain that accompanies CP, it also causes the patient to develop insulin-dependent diabetes. To counter this eventuality, islet cells from the diseased pancreas are isolated and injected into the patient’s liver.
To examine the feasibility of using a laparoscopic TPIAT approach in the treatment of CP, 32 patients were offered to undergo the procedure between January 1, 2013, and December 31, 2015. Of the 22 patients who eventually underwent laparoscopic TPIAT, two patients converted to an open procedure because of difficult anatomy and prior surgery. Average operating time was 493 minutes, average islet isolation took 185 minutes, and average length of hospital stay was 11 days. Pain and glycemic outcomes were recorded at follow-up visits every 3’6 months postoperatively.
The results showed that that laparoscopic TPIAT (compared to open TPIAT) resulted in shorter average operative time, islet isolation time, warm ischemia time, and length of stay. No patients experienced postoperative surgical site infection (SSI), hernia, or small-bowel obstruction, and none died. In all, 90% of the patients experienced a decrease or complete resolution of pain, with 60% no longer requiring opioid therapy. At one-year follow-up, 25% were insulin independent, 45% required 1-10 daily units (U/d) of insulin, 25% required 11-20 U/d, and one patient required greater than 20 U/d of basal insulin. The study was published on June 1, 2017, in JAMA Surgery.
“Chronic pancreatitis can be a very painful and debilitating condition. In an era of opioid addiction, performing a major operation through a minimally invasive technique can mean less pain for patients, reducing the need for opioids and their complications,” said senior author professor of surgery Martin Makary, MD, MPH. “Benefits of laparoscopic approaches can include vastly reduced risk of surgical wound and other infection, a quicker recovery, and better pain management.”
CP is an inflammation of the pancreas that does not heal or improve, eventually impairing a patient’s ability to digest food and make pancreatic hormones. The prevalence of CP is 50 people per 100,000, often developing between the ages of 30 and 40, and is more common in men than women. Symptoms include upper abdominal pain, nausea, vomiting, weight loss, diarrhea, and oily, clay-colored stools. Patients who have CP may have a decreased quality of life due to pain and often require admission to the hospital for treatment of symptoms.
Related Links:
Johns Hopkins University
Developed at Johns Hopkins University (JHU, Baltimore, MD, USA), laparoscopic total pancreatectomy with islet cell auto transplantation (TPIAT) involves surgically removing the pancreas and reconstructing the gastrointestinal tract. While removing the pancreas often relieves the severe abdominal pain that accompanies CP, it also causes the patient to develop insulin-dependent diabetes. To counter this eventuality, islet cells from the diseased pancreas are isolated and injected into the patient’s liver.
To examine the feasibility of using a laparoscopic TPIAT approach in the treatment of CP, 32 patients were offered to undergo the procedure between January 1, 2013, and December 31, 2015. Of the 22 patients who eventually underwent laparoscopic TPIAT, two patients converted to an open procedure because of difficult anatomy and prior surgery. Average operating time was 493 minutes, average islet isolation took 185 minutes, and average length of hospital stay was 11 days. Pain and glycemic outcomes were recorded at follow-up visits every 3’6 months postoperatively.
The results showed that that laparoscopic TPIAT (compared to open TPIAT) resulted in shorter average operative time, islet isolation time, warm ischemia time, and length of stay. No patients experienced postoperative surgical site infection (SSI), hernia, or small-bowel obstruction, and none died. In all, 90% of the patients experienced a decrease or complete resolution of pain, with 60% no longer requiring opioid therapy. At one-year follow-up, 25% were insulin independent, 45% required 1-10 daily units (U/d) of insulin, 25% required 11-20 U/d, and one patient required greater than 20 U/d of basal insulin. The study was published on June 1, 2017, in JAMA Surgery.
“Chronic pancreatitis can be a very painful and debilitating condition. In an era of opioid addiction, performing a major operation through a minimally invasive technique can mean less pain for patients, reducing the need for opioids and their complications,” said senior author professor of surgery Martin Makary, MD, MPH. “Benefits of laparoscopic approaches can include vastly reduced risk of surgical wound and other infection, a quicker recovery, and better pain management.”
CP is an inflammation of the pancreas that does not heal or improve, eventually impairing a patient’s ability to digest food and make pancreatic hormones. The prevalence of CP is 50 people per 100,000, often developing between the ages of 30 and 40, and is more common in men than women. Symptoms include upper abdominal pain, nausea, vomiting, weight loss, diarrhea, and oily, clay-colored stools. Patients who have CP may have a decreased quality of life due to pain and often require admission to the hospital for treatment of symptoms.
Related Links:
Johns Hopkins University
Latest Surgical Techniques News
- Handheld Probe Enables Real-Time Tumor Mapping in Breast-Conserving Surgery
- Optical Wireless Link Enables Cable-Free 4K Endoscopic Imaging
- Glasses-Free 3D Imaging Software Receives FDA Clearance for Surgical Planning
- Noninvasive Cardiac Radiotherapy Reduces Ventricular Tachycardia Events
- Augmented Reality System for Knee Replacement Receives FDA Clearance
- New AI Tool Predicts Complications Before Lung Cancer Surgery
- First Automated Insulin Delivery System Cleared for Type 1 Diabetes in Pregnancy
- Novel Ablation Technology Reduces Ventricular Tachycardia Recurrence
- Dual-Energy Ablation and Conduction System Pacing Show Positive Early Outcomes
- Less Invasive Microcurrent Cardiac Device Improves Heart Failure Outcomes
- Partial Heart Transplantation Enables Growing Valve Replacement for Children
- Torqueable Microcatheters Enhance Navigation in Complex Coronary Lesions
- Early “Heart Training” Surgery Promotes Regeneration in Pediatric Heart Failure
- Transcatheter Venous Arterialization Improves Outcomes in No-Option Limb Ischemia Patients
- CE-Marked Stapler Designed to Improve Staple Line Integrity
- Smart Fracture Implant Monitors Healing and Delivers Adaptive Support
Channels
Artificial Intelligence
view channelFacial Image Analysis Tracks Biological Aging, Predicts Cancer Outcomes
Biological aging is the progressive loss of physiological function that may diverge from chronological age. In cancer care, clinicians need simple tools that reflect dynamic changes in patient resilience... Read more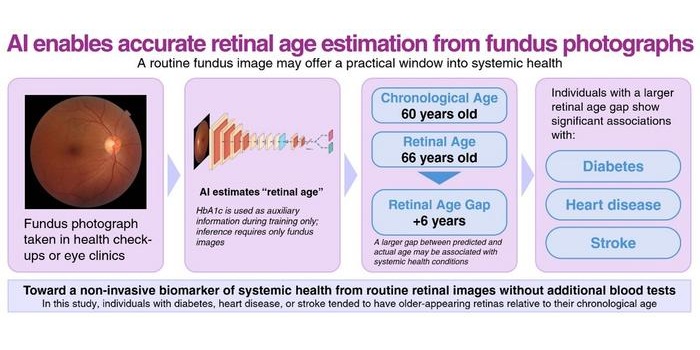
AI Model Uses Eye Imaging to Identify Risk of Major Systemic Diseases
Early detection of systemic disease risk remains a persistent challenge in population health screening. Cardiometabolic conditions such as diabetes, heart disease, and stroke often progress without symptoms... Read moreCritical Care
view channel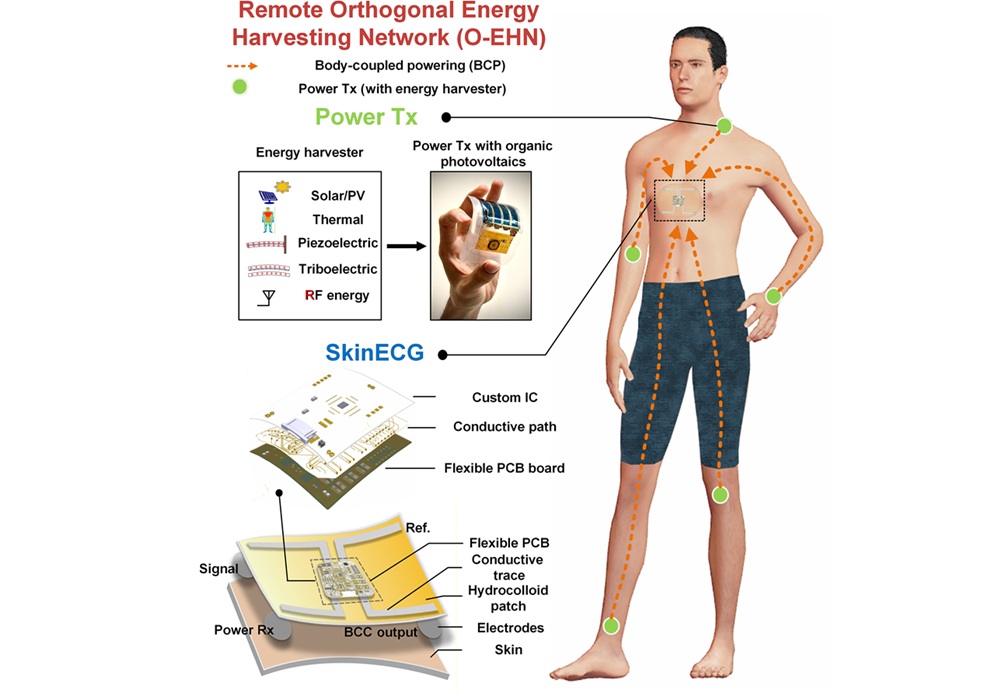
Battery-Free ECG Patch Enables Continuous Arrhythmia Monitoring
Continuous electrocardiogram (ECG) monitoring supports early detection of arrhythmias and enables timely intervention, yet many wearables depend on bulky batteries that interrupt care when depleted.... Read more
Rapid Clotting Gel Improves Emergency Bleeding Control
Uncontrolled hemorrhage remains a leading cause of preventable death in trauma and major surgery. Conventional clots can form too slowly and fail under mechanical stress, limiting hemostasis and impairing... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channel
Point-of-Care Viscoelastic Testing System Supports Obstetric Bleeding Management
HemoSonics (Durham, NC, USA) announced on May 5, 2026 that the company's Quantra Hemostasis System for Obstetric Procedures won Silver in the 2026 Edison Awards in the Women’s Health and Reproductive Innovations... Read moreBusiness
view channel
Johnson & Johnson Launches AI-Driven Cardiac Mapping System
Johnson & Johnson has introduced the CARTOSOUND SONATA Module for the CARTO System at the Heart Rhythm Society (HRS) 2026 meeting in Chicago. The module uses artificial intelligence with the CARTO... Read more