Longer Anesthesia Duration Tied to Surgical Complications
|
By HospiMedica International staff writers Posted on 16 Oct 2017 |
Image: A new study suggests anesthesia time should be kept to the minimum to avoid surgical complications (Photo courtesy of Alamy).
A new study suggests that extended anesthesia is associated with significantly increased rates of surgical complications, especially due to postoperative transfusion requirements.
Researchers at Rutgers New Jersey Medical School (NJMS; Newark, USA) conducted a study involving 630 patients who underwent head and neck microvascular reconstruction between 2005 and 2014 to examine the association of anesthesia duration with surgical complications. The patients were stratified into five quintiles based on mean anesthesia duration; group 1 - 358.1 minutes; group 2 - 563.2 minutes; group 3 - 648.9 minutes; group 4 - 736.5 minutes; and group 5 - 922.1 minutes. The main outcomes included rates of postoperative medical and surgical complications and mortality.
The results showed that increasing anesthesia duration was associated with higher 30-day complication rates, 30-day postoperative surgical complications, increased rates of postoperative transfusion, and more wound disruptions. Anesthesia duration was not associated with specific medical complications, overall medical complication rate, or mortality. When accounting for demographics and significant preoperative factors, including free flap type, increased anesthesia duration remained significantly associated with overall complications, surgical complications, and postoperative transfusion. The study was published on October 5, 2017, in JAMA Facial Plastic Surgery.
“These results highlight the need for an awareness of the perioperative and nonsurgical factors that may extend anesthesia time and tactics that promote intraoperative efficiency. One such strategy involves selection of a donor site amenable to concurrent harvesting and implementation of a 2-team approach,” concluded lead author Jacob Brady, MD, and colleagues. “The number of microvascular anastomoses and defect closure that will be required should also be considered in donor site selection. Ultimately, meticulous preoperative planning and preparation should allow surgeons to reduce operating room time, regardless of other nonsurgical factors out of their control.”
General anesthesia is a state produced when a patient receives intravenous and inhaled agents to allow adequate surgical access to the operative site. It is intended to promote amnesia, analgesia, muscle paralysis, and sedation in a controlled, reversible, state of unconsciousness that enables a patient to tolerate surgical procedures that would otherwise inflict unbearable pain, potentiate extreme physiologic exacerbations, and result in unpleasant memories.
Related Links:
Rutgers New Jersey Medical School
Researchers at Rutgers New Jersey Medical School (NJMS; Newark, USA) conducted a study involving 630 patients who underwent head and neck microvascular reconstruction between 2005 and 2014 to examine the association of anesthesia duration with surgical complications. The patients were stratified into five quintiles based on mean anesthesia duration; group 1 - 358.1 minutes; group 2 - 563.2 minutes; group 3 - 648.9 minutes; group 4 - 736.5 minutes; and group 5 - 922.1 minutes. The main outcomes included rates of postoperative medical and surgical complications and mortality.
The results showed that increasing anesthesia duration was associated with higher 30-day complication rates, 30-day postoperative surgical complications, increased rates of postoperative transfusion, and more wound disruptions. Anesthesia duration was not associated with specific medical complications, overall medical complication rate, or mortality. When accounting for demographics and significant preoperative factors, including free flap type, increased anesthesia duration remained significantly associated with overall complications, surgical complications, and postoperative transfusion. The study was published on October 5, 2017, in JAMA Facial Plastic Surgery.
“These results highlight the need for an awareness of the perioperative and nonsurgical factors that may extend anesthesia time and tactics that promote intraoperative efficiency. One such strategy involves selection of a donor site amenable to concurrent harvesting and implementation of a 2-team approach,” concluded lead author Jacob Brady, MD, and colleagues. “The number of microvascular anastomoses and defect closure that will be required should also be considered in donor site selection. Ultimately, meticulous preoperative planning and preparation should allow surgeons to reduce operating room time, regardless of other nonsurgical factors out of their control.”
General anesthesia is a state produced when a patient receives intravenous and inhaled agents to allow adequate surgical access to the operative site. It is intended to promote amnesia, analgesia, muscle paralysis, and sedation in a controlled, reversible, state of unconsciousness that enables a patient to tolerate surgical procedures that would otherwise inflict unbearable pain, potentiate extreme physiologic exacerbations, and result in unpleasant memories.
Related Links:
Rutgers New Jersey Medical School
Latest Critical Care News
- New Nasal Spray Enables Prehospital Neuroprotection in Ischemic Stroke
- AI-Enhanced ECG Screens for Heart Failure Risk in Resource-Limited Settings
- Single-Lead AI ECG Tool Detects Moderate-to-Severe Hyperkalemia Outside Clinic
- Reduced-Intensity Transplant Regimen Expands Donor Access in Sickle Cell Disease
- Battery-Free ECG Patch Enables Continuous Arrhythmia Monitoring
- Spinal Cord Interface Restores Bladder Control in Preclinical Study
- Rapid Clotting Gel Improves Emergency Bleeding Control
- AI Tool Predicts In-Hospital Cardiac Arrest Minutes in Advance
- Magnetic Control System Enables Precise Navigation of Miniature Medical Devices
- Shelf-Stable Synthetic Platelets Could Enable Prehospital Hemorrhage Control
- Noninvasive AI Test Aims to Enable Earlier Pulmonary Hypertension Detection
- Blood-Filtering Device May Prolong Pregnancy in Severe Early Preeclampsia
- Noninvasive Skull Sensor Detects Early Deterioration in Acute Brain Injury
- Automated Robotic Imaging System Enhances Full-Body Skin Cancer Screening
- Bacteria-Resistant Urinary Catheter Coating Reduces Infections and Antibiotic Use
- New Brain-Computer Interface Targets Treatment-Resistant Depression
Channels
Artificial Intelligence
view channelFacial Image Analysis Tracks Biological Aging, Predicts Cancer Outcomes
Biological aging is the progressive loss of physiological function that may diverge from chronological age. In cancer care, clinicians need simple tools that reflect dynamic changes in patient resilience... Read more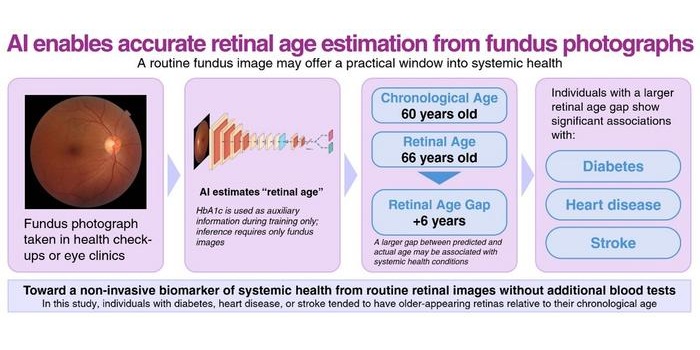
AI Model Uses Eye Imaging to Identify Risk of Major Systemic Diseases
Early detection of systemic disease risk remains a persistent challenge in population health screening. Cardiometabolic conditions such as diabetes, heart disease, and stroke often progress without symptoms... Read moreCritical Care
view channel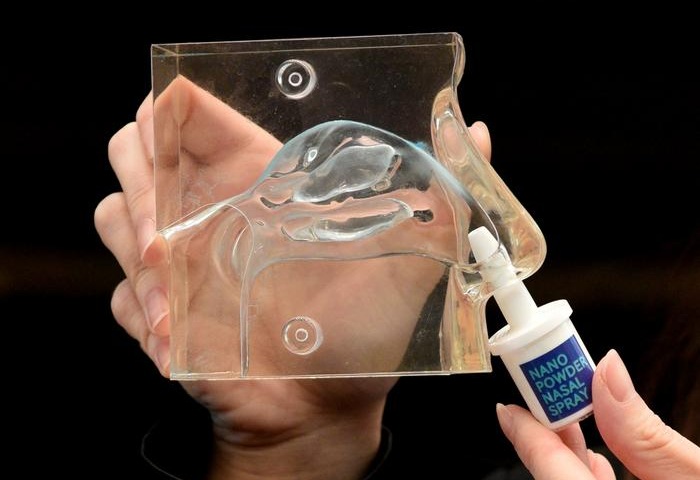
New Nasal Spray Enables Prehospital Neuroprotection in Ischemic Stroke
Ischemic stroke, caused by arterial occlusion in the brain, requires time‑critical intervention to limit neuronal loss. Many patients arrive outside the narrow window for thrombolysis or thrombectomy,... Read more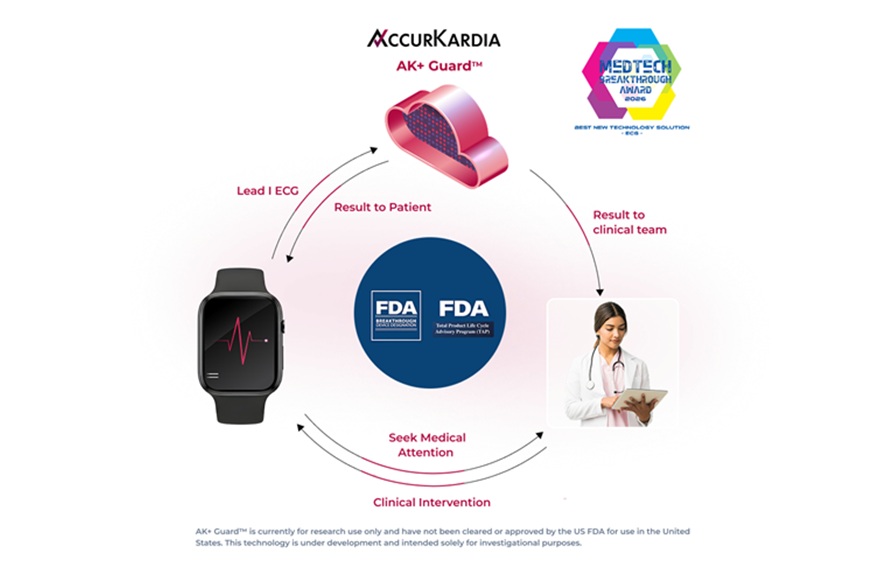
Single-Lead AI ECG Tool Detects Moderate-to-Severe Hyperkalemia Outside Clinic
Hyperkalemia can escalate quickly and is commonly monitored through laboratory blood draws, leaving risk between clinic visits. Clinicians need timely, accessible tools to identify moderate to severe elevations... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channel
Point-of-Care Viscoelastic Testing System Supports Obstetric Bleeding Management
HemoSonics (Durham, NC, USA) announced on May 5, 2026 that the company's Quantra Hemostasis System for Obstetric Procedures won Silver in the 2026 Edison Awards in the Women’s Health and Reproductive Innovations... Read moreBusiness
view channel
Olympus Partnership Aims to Expand Access to Robot-Assisted Endoscopic Therapy
Olympus has signed an exclusive global distribution agreement with EndoRobotics Co., Ltd., under which robot-assisted technologies developed by EndoRobotics will be distributed worldwide as part of the... Read more