Implantable Sensor Relays Real-Time Health Data
|
By HospiMedica International staff writers Posted on 28 Mar 2018 |
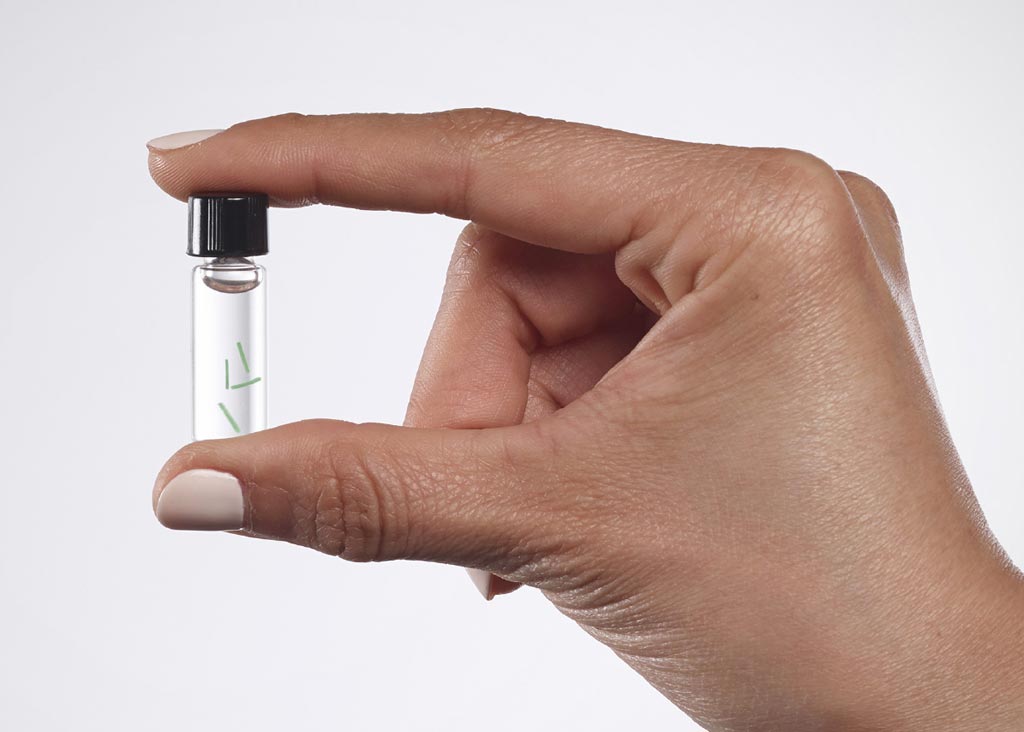
Image: Implantable biosensors continuously measure body chemistries (Photo courtesy of Profusa).
Tissue-integrating biosensors may soon allow continuous monitoring of body chemistries and provide early warning of developing health problems.
Under development at Profusa (San Francisco, CA, USA), the sensors, which are smaller than a grain of rice, are made of a proprietary hydrogel scaffold based on poly(2-hydroxyethyl methacrylate), a polymer used to make soft contact lenses. The sensors also lack flat surfaces, allowing cells and capillaries to grow into its porous structure without causing an undesirable immune response. The hydrogel scaffold is festooned with dye molecules that respond to various analytes in the blood, such as oxygen, carbon dioxide, glucose or lactate.
A small detector held against the skin shines near-infrared (nIR) light through the skin, causing the dye molecules to fluoresce in concordance with analyte concentration. The fluorescence is captured by a nIR optical reader, which wirelessly transmits the data to a computer or cell phone so as to record analyte concentrations over time. The data can also be shared securely via digital networks with healthcare providers. A study describing the new sensors was presented at the 255th National Meeting & Exposition of the American Chemical Society (ACS), held during March 2018 in New Orleans (LA, USA).
“While fitness trackers and other wearables provide insights into our heart rate, respiration, and other physical measures, they don’t provide information on the most important aspect of our health: our body’s chemistry,” said study presenter Natalie Wisniewski, PhD, chief technology officer (CTO) and co-founder of Profusa. “Based on our ongoing studies, tissue-integrated sensor technology has the potential to enable wearables to live up to the promise of personalized medicine, revolutionizing the management of health in wellness and disease.”
“The sensors would provide a continuous record of your analytes relative to your personal baseline. Then, if something goes off kilter, it's flagged early, before you feel symptoms, so you can get to the doctor in time for treatment,” concluded Dr. Wisniewski. “Other implantable sensors currently on the market have a significant drawback; they often provoke a 'foreign body' immune response that coats the sensor with inflammatory cells or scar tissue. That coating can wall off the device from capillaries and prevent it from sensing chemical changes accurately, so it stops working after a few weeks or months.”
The Lumee Oxygen Platform, the first medical application of Profusa biosensor technology, was approved for sale in Europe in 2017, helping wound-healing specialists track oxygen in the lower extremities of patients undergoing treatment for chronic limb ischemia (CLI).
Related Links:
Profusa
Under development at Profusa (San Francisco, CA, USA), the sensors, which are smaller than a grain of rice, are made of a proprietary hydrogel scaffold based on poly(2-hydroxyethyl methacrylate), a polymer used to make soft contact lenses. The sensors also lack flat surfaces, allowing cells and capillaries to grow into its porous structure without causing an undesirable immune response. The hydrogel scaffold is festooned with dye molecules that respond to various analytes in the blood, such as oxygen, carbon dioxide, glucose or lactate.
A small detector held against the skin shines near-infrared (nIR) light through the skin, causing the dye molecules to fluoresce in concordance with analyte concentration. The fluorescence is captured by a nIR optical reader, which wirelessly transmits the data to a computer or cell phone so as to record analyte concentrations over time. The data can also be shared securely via digital networks with healthcare providers. A study describing the new sensors was presented at the 255th National Meeting & Exposition of the American Chemical Society (ACS), held during March 2018 in New Orleans (LA, USA).
“While fitness trackers and other wearables provide insights into our heart rate, respiration, and other physical measures, they don’t provide information on the most important aspect of our health: our body’s chemistry,” said study presenter Natalie Wisniewski, PhD, chief technology officer (CTO) and co-founder of Profusa. “Based on our ongoing studies, tissue-integrated sensor technology has the potential to enable wearables to live up to the promise of personalized medicine, revolutionizing the management of health in wellness and disease.”
“The sensors would provide a continuous record of your analytes relative to your personal baseline. Then, if something goes off kilter, it's flagged early, before you feel symptoms, so you can get to the doctor in time for treatment,” concluded Dr. Wisniewski. “Other implantable sensors currently on the market have a significant drawback; they often provoke a 'foreign body' immune response that coats the sensor with inflammatory cells or scar tissue. That coating can wall off the device from capillaries and prevent it from sensing chemical changes accurately, so it stops working after a few weeks or months.”
The Lumee Oxygen Platform, the first medical application of Profusa biosensor technology, was approved for sale in Europe in 2017, helping wound-healing specialists track oxygen in the lower extremities of patients undergoing treatment for chronic limb ischemia (CLI).
Related Links:
Profusa
Latest Critical Care News
- Eye Imaging AI Identifies Elevated Cardiovascular Risk
- Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
- Combined Infection Control Strategy Limits Drug-Resistant Outbreak in NICU
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreSurgical Techniques
view channel
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more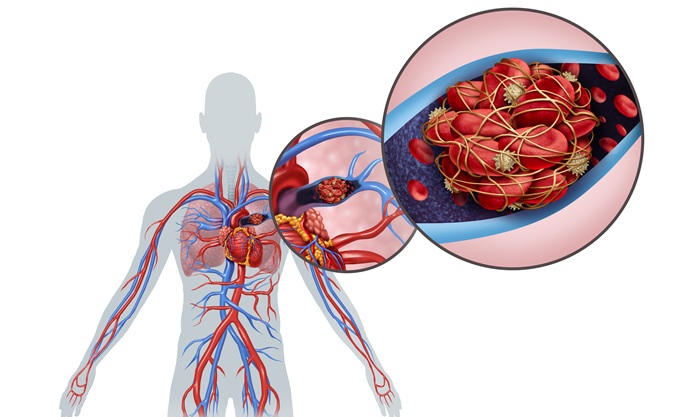
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel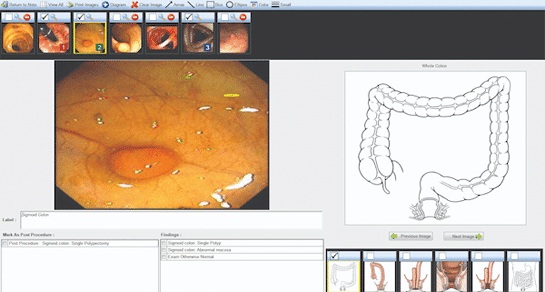
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel