Cross-Checking between ED Physicians Reduces Harm
|
By HospiMedica International staff writers Posted on 08 May 2018 |

Image: A new study suggests a few minutes of consultation can avoid adverse ED events (Photo courtesy of Dreamstime).
A new study suggests that systematic cross-checking between doctors may be a key to reducing the high rate of adverse events in the emergency department (ED).
Researchers at the Sorbonne University (Paris, France), Pitie-Salpetriere Hospital (Paris, France), and other institutions conducted a cluster randomized crossover trial that included a random sample of 1,680 patients attended to in six EDs in France during two 10-day periods. The intervention included systematic cross-checking between ED physicians three times a day, which included a brief presentation of one physician’s case to another, followed by the second physician’s feedback. The main outcome was medical error, defined as either a near miss or a serious adverse event.
The results showed that there were 54 adverse events among 840 patients (6.4%) during the cross-check intervention, compared with 90 adverse events among 840 patients (10.7%) during the control period, a relative reduction of 40%. Most of the reductions occurred in adverse events defined as near misses, with a reduction of 47%. Errors in sepsis management accounted for more than 40% of the preventable serious adverse events. The median duration of cross-checking sessions was nine minutes, during which about seven patients were discussed. The study was published on April 23, 2018, in JAMA Internal Medicine.
“The reduction in preventable serious adverse events with systematic cross-checking did not reach statistical significance; only reductions in near misses did,” explained lead author Yonathan Freund, MD, PhD, of Hôpital Pitié-Salpêtrière. “Whether an adverse event resulted from a misdiagnosis or from the implementation of an inappropriate plan for the correct diagnosis could not be determined decisively. This included sepsis-associated medical errors, which may be particularly relevant, because the most commonly occurring serious adverse events were violations of the surviving sepsis campaign guidelines.”
An adverse event is defined as a preventable or non-preventable injury that was caused by medical management (rather than the underlying disease) and that prolonged hospitalization, produced a disability at the time of discharge, or both. Adverse event also include errors, defined as acts of commission or omission leading to an undesirable outcome or significant potential for such an outcome, and near misses, in which an error was committed, but the patient did not experience clinical harm, either through early detection or sheer luck.
Related Links:
Sorbonne University
Pitie-Salpetriere Hospital
Researchers at the Sorbonne University (Paris, France), Pitie-Salpetriere Hospital (Paris, France), and other institutions conducted a cluster randomized crossover trial that included a random sample of 1,680 patients attended to in six EDs in France during two 10-day periods. The intervention included systematic cross-checking between ED physicians three times a day, which included a brief presentation of one physician’s case to another, followed by the second physician’s feedback. The main outcome was medical error, defined as either a near miss or a serious adverse event.
The results showed that there were 54 adverse events among 840 patients (6.4%) during the cross-check intervention, compared with 90 adverse events among 840 patients (10.7%) during the control period, a relative reduction of 40%. Most of the reductions occurred in adverse events defined as near misses, with a reduction of 47%. Errors in sepsis management accounted for more than 40% of the preventable serious adverse events. The median duration of cross-checking sessions was nine minutes, during which about seven patients were discussed. The study was published on April 23, 2018, in JAMA Internal Medicine.
“The reduction in preventable serious adverse events with systematic cross-checking did not reach statistical significance; only reductions in near misses did,” explained lead author Yonathan Freund, MD, PhD, of Hôpital Pitié-Salpêtrière. “Whether an adverse event resulted from a misdiagnosis or from the implementation of an inappropriate plan for the correct diagnosis could not be determined decisively. This included sepsis-associated medical errors, which may be particularly relevant, because the most commonly occurring serious adverse events were violations of the surviving sepsis campaign guidelines.”
An adverse event is defined as a preventable or non-preventable injury that was caused by medical management (rather than the underlying disease) and that prolonged hospitalization, produced a disability at the time of discharge, or both. Adverse event also include errors, defined as acts of commission or omission leading to an undesirable outcome or significant potential for such an outcome, and near misses, in which an error was committed, but the patient did not experience clinical harm, either through early detection or sheer luck.
Related Links:
Sorbonne University
Pitie-Salpetriere Hospital
Latest Critical Care News
- Implantable Wireless Light Device Advance Bladder Cancer Treatment
- Smart Wristband Technology Detects Cardiac Arrest and Alerts Responders
- FDA-Cleared Home Sleep Test Enables Multi-Night Diagnosis of Sleep Apnea
- AI-Enabled Wearable Patches Reveal Undetected Hormone Disruption in Infertility
- AI Method Turns Toe Scan into Rapid PAD Screening Tool
- Integrated AI Pulmonary Workflow System Streamlines Detection and Follow-Up
- AI Model Predicts 10-Year Stroke Risk from Standard ECG
- Portable Ultrasound Tool Quantifies Liver Fat with MRI-Like Accuracy
- AI Tool Predicts Risk of Out-of-Hospital Cardiac Arrest
- Implantable Cytokine Device Enables Localized Immunotherapy for Ovarian Cancer
- Wearable Defibrillator Supports Quicker Beta-Blocker Optimization in Women
- High-Frequency Ultrasound Disables Viruses While Sparing Human Cells
- New Nasal Spray Enables Prehospital Neuroprotection in Ischemic Stroke
- AI-Enhanced ECG Screens for Heart Failure Risk in Resource-Limited Settings
- Single-Lead AI ECG Tool Detects Moderate-to-Severe Hyperkalemia Outside Clinic
- Reduced-Intensity Transplant Regimen Expands Donor Access in Sickle Cell Disease
Channels
Artificial Intelligence
view channel
Automated Phone Speech Test Identifies Alzheimer’s Pathology for Prescreening
Alzheimer’s disease assessment and trial recruitment often rely on costly, invasive biomarker testing and clinic-based cognitive evaluations, limiting scalability as populations age. Providers and trial... Read more
FDA-Cleared AI System Detects Sepsis Earlier and Reduces Mortality
Sepsis remains one of the deadliest complications for hospitalized patients, in part because its early signs overlap with other conditions. Each hour of delayed recognition measurably decreases survival,... Read moreSurgical Techniques
view channel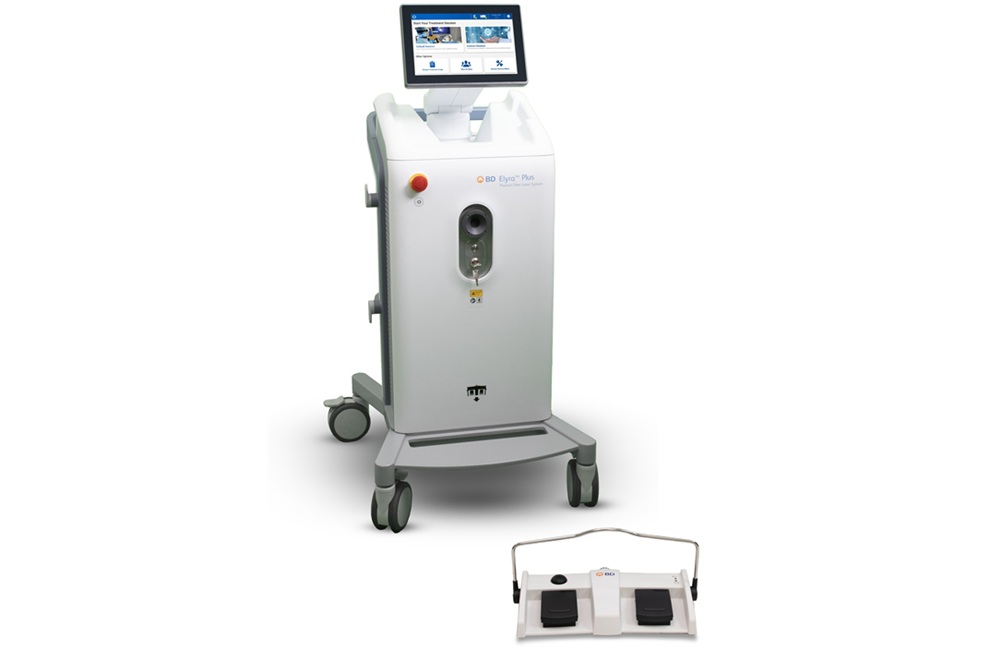
BD Launches Elyra Laser Platform for Kidney Stone and Soft Tissue Procedures
BD (Becton, Dickinson and Company) has introduced the Elyra Thulium Fiber Laser (TFL) System, an advanced laser platform developed to complete its kidney stone care portfolio for urology teams.... Read more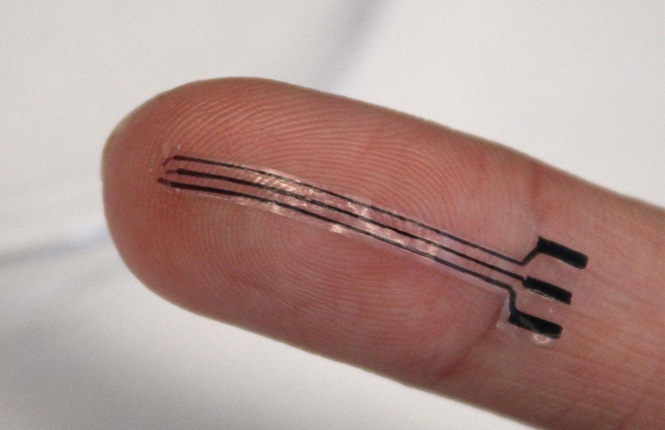
Stretchable Bioelectronic Implant Lowers Blood Pressure in Preclinical Study
Hypertension, or high blood pressure, drives major cardiovascular morbidity and affects nearly half of adults in the United States. About one in ten patients develop drug‑resistant hypertension that persists... Read more
FDA-Cleared Nerve Stimulator Advances Intraoperative Peripheral Nerve Assessment
The Evala Nerve Stimulator from Epineuron (Mississauga, ON, Canada) is a handheld, intraoperative electrical stimulation system designed to provide surgeons with a rapid and accurate method for nerve identification... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channel
Point-of-Care Viscoelastic Testing System Supports Obstetric Bleeding Management
HemoSonics (Durham, NC, USA) announced on May 5, 2026 that the company's Quantra Hemostasis System for Obstetric Procedures won Silver in the 2026 Edison Awards in the Women’s Health and Reproductive Innovations... Read moreBusiness
view channel
Olympus Partnership Aims to Expand Access to Robot-Assisted Endoscopic Therapy
Olympus has signed an exclusive global distribution agreement with EndoRobotics Co., Ltd., under which robot-assisted technologies developed by EndoRobotics will be distributed worldwide as part of the... Read more