Speech-Recognition Alone Cannot Sustain Transcription Process
|
By HospiMedica International staff writers Posted on 09 Aug 2018 |

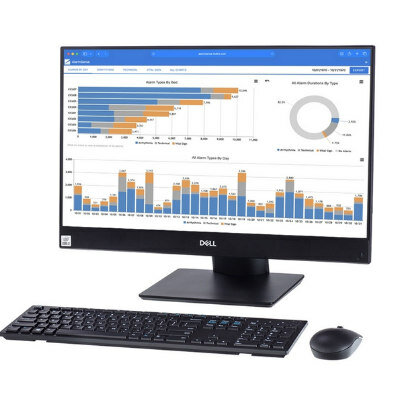
Image: Speech recognition notes are not enough for accurate documentation, according to a new study (Photo courtesy of Nuance).
While speech recognition (SR) software serves as a valuable tool for annotating clinical notes, it does not appear capable of serving as the sole component of the transcription process, claims a new study.
Researchers at Brigham and Women’s Hospital (BWH; Boston, MA, USA), Massachusetts General Hospital (MGH; Boston, USA), the University of Colorado (Aurora, USA), and other institutions conducted a study to examine the quality of SR-assisted documentation throughout the dictation process. To do so, they collected a random sample of 83 office notes, 75 discharge summaries, and 59 operative notes dictated by 144 physicians using the Nuance Communications Dragon Medical 360 | eScription platform.
They then identified transcription errors in the SR generated document, the medical transcriptionist edited document (MT), and the physician’s signed note (SN). Each document was compared with a criterion standard created from the original audio recording (OA) and the medical record review. Outcomes and measures included error rate; mean errors per document; error frequency by general type (such as deletion), semantic type (such as medication), and clinical significance. The researchers also reviewed variations by physician characteristics, note type, and institution.
The researchers then reviewed the documents at four separate stages (OA, SR, MT, SN), noting the time taken to dictate and review each note. In each stage, error rates involved clinical information in 15.8%, 26.9%, and 25.9% of cases, respectively; 5.7%, 8.9%, and 6.4% were deemed clinically significant. In the 217 clinical notes, 7.4% of the words were incorrectly transcribed by automated SR, but the error rate fell to 0.4% after MT review of the clinical notes, and dropped to just 0.3% after the physician signed off on the notes. The study was published on July 6, 2018, in JAMA Network Open.
Clinical documentation is among the most time-consuming and costly aspects of using an electronic health record (EHR) system. SR technology, the automatic translation of voice into text, has been used for clinical documentation since the 1980s. There are two types of SR systems - front-end SR, in which physicians dictate directly into free-text fields of the electronic health record (HER) and edit them before saving the document, and back-end SR systems, in which the SR text is edited by a professional MT and sent back to the physician for review.
Related Links:
Brigham and Women’s Hospital
Massachusetts General Hospital
University of Colorado
Researchers at Brigham and Women’s Hospital (BWH; Boston, MA, USA), Massachusetts General Hospital (MGH; Boston, USA), the University of Colorado (Aurora, USA), and other institutions conducted a study to examine the quality of SR-assisted documentation throughout the dictation process. To do so, they collected a random sample of 83 office notes, 75 discharge summaries, and 59 operative notes dictated by 144 physicians using the Nuance Communications Dragon Medical 360 | eScription platform.
They then identified transcription errors in the SR generated document, the medical transcriptionist edited document (MT), and the physician’s signed note (SN). Each document was compared with a criterion standard created from the original audio recording (OA) and the medical record review. Outcomes and measures included error rate; mean errors per document; error frequency by general type (such as deletion), semantic type (such as medication), and clinical significance. The researchers also reviewed variations by physician characteristics, note type, and institution.
The researchers then reviewed the documents at four separate stages (OA, SR, MT, SN), noting the time taken to dictate and review each note. In each stage, error rates involved clinical information in 15.8%, 26.9%, and 25.9% of cases, respectively; 5.7%, 8.9%, and 6.4% were deemed clinically significant. In the 217 clinical notes, 7.4% of the words were incorrectly transcribed by automated SR, but the error rate fell to 0.4% after MT review of the clinical notes, and dropped to just 0.3% after the physician signed off on the notes. The study was published on July 6, 2018, in JAMA Network Open.
Clinical documentation is among the most time-consuming and costly aspects of using an electronic health record (EHR) system. SR technology, the automatic translation of voice into text, has been used for clinical documentation since the 1980s. There are two types of SR systems - front-end SR, in which physicians dictate directly into free-text fields of the electronic health record (HER) and edit them before saving the document, and back-end SR systems, in which the SR text is edited by a professional MT and sent back to the physician for review.
Related Links:
Brigham and Women’s Hospital
Massachusetts General Hospital
University of Colorado
Latest Health IT News
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
- Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
- Smartwatches Could Detect Congestive Heart Failure
- Versatile Smart Patch Combines Health Monitoring and Drug Delivery
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read more
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read moreSurgical Techniques
view channel
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreBusiness
view channel