New AR Device Helps Cardiologists Plan and Perform Complex Procedures
|
By HospiMedica International staff writers Posted on 12 Nov 2018 |
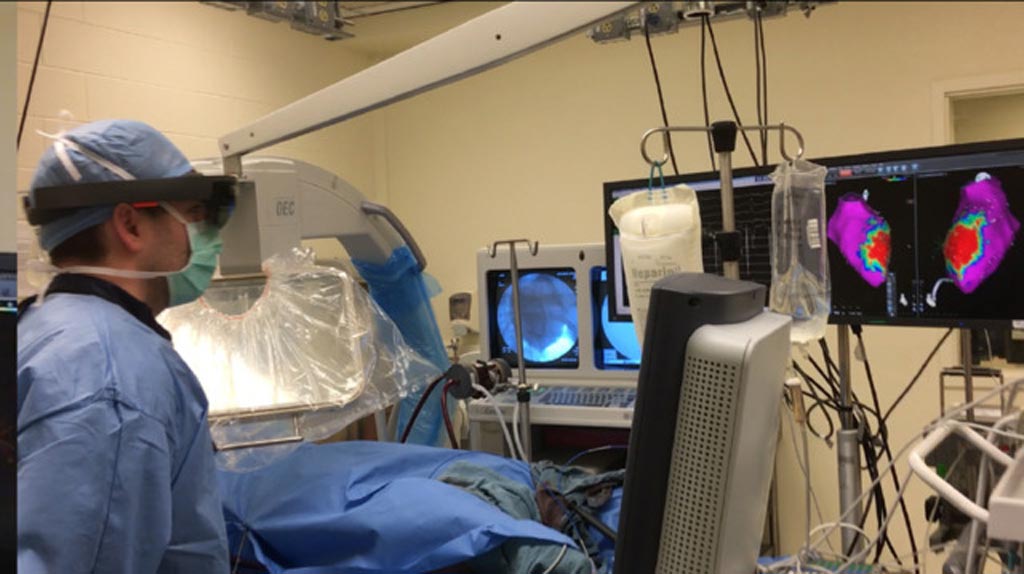
Image: The self-contained AR device is designed to provide an immersive AR experience in which surgeons can interactively explore data in three dimensions (Photo courtesy of Beth Israel Deaconess Medical Center).
Augmented Reality (AR), a technology that superimposes computer-generated information on a user's view of the real world, offers a new platform to help physicians better visualize complex medical data, particularly before and during medical procedures.
A new self-contained AR device aims to provide an immersive AR experience in which surgeons can interactively explore data in three dimensions (3D). By projecting 3D imagery onto a glass screen worn like a diving mask on the surgeon’s face, AR provides 3D depth perception and allows surgeons to interact with the medical data without physically touching a screen or computer mouse, maintaining a sterile environment and reducing the risk of infection.
Researchers at the Beth Israel Deaconess Medical Center (Boston, MA, USA) who conducted a study to assess the potential of AR for helping cardiologists visualize myocardial scarring in the heart as they perform ventricular tachycardia ablation or other electrophysiological interventions have found that the new technology confers a number of advantages.
In a pilot study, the researchers applied the AR technique as they generated holographic 3D scar in five animal models that underwent controlled infarction and electrophysiological study. 3D holographic visualization of the scar was performed to assist assessment of the complex 3D scar architecture. An operator and mapping specialist viewed the holographic 3D scar during electrophysiological study, and completed the perceived usefulness questionnaire in the six-item usefulness scale and found it useful to have scar information during the intervention. The user could interactively explore 3D myocardial scar in the AR environment that allows for the combination of holographic 3D LGE data interacting with any real-world environments, such as a surgical suite or patient’s body.
“Augmented reality allows physicians to superimpose images, such as MRI or CT scans, as a guide during therapeutic intervention,” said Jihye Jang, a PhD Candidate at the Cardiac Magnetic Resonance (MR) Center at Beth Israel Deaconess Medical Center. “Our report shows exciting potential that having this complex 3D scar information through augmented reality during the intervention may help guide treatment and ultimately improve patient care. Physicians can now use AR to view 3D cardiac MR information with a touchless interaction in sterile environment.”
Related Links:
Beth Israel Deaconess Medical Center
A new self-contained AR device aims to provide an immersive AR experience in which surgeons can interactively explore data in three dimensions (3D). By projecting 3D imagery onto a glass screen worn like a diving mask on the surgeon’s face, AR provides 3D depth perception and allows surgeons to interact with the medical data without physically touching a screen or computer mouse, maintaining a sterile environment and reducing the risk of infection.
Researchers at the Beth Israel Deaconess Medical Center (Boston, MA, USA) who conducted a study to assess the potential of AR for helping cardiologists visualize myocardial scarring in the heart as they perform ventricular tachycardia ablation or other electrophysiological interventions have found that the new technology confers a number of advantages.
In a pilot study, the researchers applied the AR technique as they generated holographic 3D scar in five animal models that underwent controlled infarction and electrophysiological study. 3D holographic visualization of the scar was performed to assist assessment of the complex 3D scar architecture. An operator and mapping specialist viewed the holographic 3D scar during electrophysiological study, and completed the perceived usefulness questionnaire in the six-item usefulness scale and found it useful to have scar information during the intervention. The user could interactively explore 3D myocardial scar in the AR environment that allows for the combination of holographic 3D LGE data interacting with any real-world environments, such as a surgical suite or patient’s body.
“Augmented reality allows physicians to superimpose images, such as MRI or CT scans, as a guide during therapeutic intervention,” said Jihye Jang, a PhD Candidate at the Cardiac Magnetic Resonance (MR) Center at Beth Israel Deaconess Medical Center. “Our report shows exciting potential that having this complex 3D scar information through augmented reality during the intervention may help guide treatment and ultimately improve patient care. Physicians can now use AR to view 3D cardiac MR information with a touchless interaction in sterile environment.”
Related Links:
Beth Israel Deaconess Medical Center
Latest Business News
- GE HealthCare Leads Major European Initiative to Advance Cardio-Oncology Care
- Medtronic and GE HealthCare Broaden Alliance Across Monitoring and Care Solutions
- Quantum Surgical Acquires NeuWave from Johnson & Johnson
- Medtronic to Acquire Coronary Artery Medtech Company CathWorks
- Medtronic and Mindray Expand Strategic Partnership to Ambulatory Surgery Centers in the U.S.
- FDA Clearance Expands Robotic Options for Minimally Invasive Heart Surgery
- WHX in Dubai (formerly Arab Health) to debut specialised Biotech & Life Sciences Zone as sector growth accelerates globally
- WHX in Dubai (formerly Arab Health) to bring together key UAE government entities during the groundbreaking 2026 edition
- Interoperability Push Fuels Surge in Healthcare IT Market
- Philips and Masimo Partner to Advance Patient Monitoring Measurement Technologies
- B. Braun Acquires Digital Microsurgery Company True Digital Surgery
- CMEF 2025 to Promote Holistic and High-Quality Development of Medical and Health Industry
- Bayer and Broad Institute Extend Research Collaboration to Develop New Cardiovascular Therapies
- Medtronic Partners with Corsano to Expand Acute Care & Monitoring Portfolio in Europe
- Expanded Collaboration to Transform OR Technology Through AI and Automation
- Becton Dickinson to Spin Out Biosciences and Diagnostic Solutions Business
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreCritical Care
view channel
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read more
First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
Pulmonary hypertension is a progressive, life‑threatening disease that is frequently missed early because symptoms such as dyspnea are nonspecific and diagnostic delays can exceed two years.... Read moreSurgical Techniques
view channel
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read more
New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
Volumetric muscle loss is a traumatic loss of skeletal muscle that often leads to permanent functional impairment and limited reconstructive options. Current experimental strategies struggle to deliver... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more