Minimal Oxygen Supplementation Recommended for Most Inpatients
|
By HospiMedica International staff writers Posted on 13 Nov 2018 |
A new guidance statement reports that supplemental oxygen is not always indicated for acutely ill patients, and may contribute to higher mortality.
An expert panel from McMaster University (Hamilton, ON, Canada), Stellenbosch University (SU, South Africa), University Hospitals of Geneva (Switzerland), and other institutions convened to evaluated a recent systematic review and meta-analysis of 25 randomized controlled trials in order to develop recommendations for supplemental oxygen therapy in critically ill patients, surgical patients with sepsis, hospitalized patients, or patients en-route to hospital in an ambulance. Postoperative, obstetric, and pediatric patients were not included in the review.
The systematic review, which was published in The Lancet in April 2018, found that supplemental oxygen in inpatients with normal oxygen saturation increases mortality, and recommended that oxygen should be administered conservatively. The international panel of experts made several key recommendations, including maintaining peripheral oxygen saturation (SpO2) at or below 96% in patients on supplemental oxygen; in patients with acute myocardial infarction (MI) or stroke, oxygen should not be administered if the initial SpO2 is higher 92%. The guidance recommendations were published on October 24, 2018, in BMJ.
“It is a longstanding cultural norm to provide supplemental oxygen to sick patients, regardless of their blood oxygen saturation. A recent systematic review and meta-analysis has shown that too much supplemental oxygen increases mortality for medical patients in hospital,” concluded lead author Reed Siemieniuk, MD, PhD, of McMaster University, and colleagues. “A target SpO2 range of 90-94% seems reasonable for most patients, and 88-92% for patients at risk of hypercapnic respiratory failure seems wide enough to allow for normal fluctuation, and is likely low enough to avoid harm.”
The reasons as to why excessive supplemental oxygen increases mortality remain uncertain. Excessive oxygen can lead to reduced cardiac output, vasoconstriction, inflammation, and oxidative stress. In addition, excessive oxygen might lead to falsely reassuring SpO2 values and make it difficult to recognize when a patient’s condition worsens.
Related Links:
McMaster University
Stellenbosch University
University Hospitals of Geneva
An expert panel from McMaster University (Hamilton, ON, Canada), Stellenbosch University (SU, South Africa), University Hospitals of Geneva (Switzerland), and other institutions convened to evaluated a recent systematic review and meta-analysis of 25 randomized controlled trials in order to develop recommendations for supplemental oxygen therapy in critically ill patients, surgical patients with sepsis, hospitalized patients, or patients en-route to hospital in an ambulance. Postoperative, obstetric, and pediatric patients were not included in the review.
The systematic review, which was published in The Lancet in April 2018, found that supplemental oxygen in inpatients with normal oxygen saturation increases mortality, and recommended that oxygen should be administered conservatively. The international panel of experts made several key recommendations, including maintaining peripheral oxygen saturation (SpO2) at or below 96% in patients on supplemental oxygen; in patients with acute myocardial infarction (MI) or stroke, oxygen should not be administered if the initial SpO2 is higher 92%. The guidance recommendations were published on October 24, 2018, in BMJ.
“It is a longstanding cultural norm to provide supplemental oxygen to sick patients, regardless of their blood oxygen saturation. A recent systematic review and meta-analysis has shown that too much supplemental oxygen increases mortality for medical patients in hospital,” concluded lead author Reed Siemieniuk, MD, PhD, of McMaster University, and colleagues. “A target SpO2 range of 90-94% seems reasonable for most patients, and 88-92% for patients at risk of hypercapnic respiratory failure seems wide enough to allow for normal fluctuation, and is likely low enough to avoid harm.”
The reasons as to why excessive supplemental oxygen increases mortality remain uncertain. Excessive oxygen can lead to reduced cardiac output, vasoconstriction, inflammation, and oxidative stress. In addition, excessive oxygen might lead to falsely reassuring SpO2 values and make it difficult to recognize when a patient’s condition worsens.
Related Links:
McMaster University
Stellenbosch University
University Hospitals of Geneva
Latest Critical Care News
- Battery-Free ECG Patch Enables Continuous Arrhythmia Monitoring
- Spinal Cord Interface Restores Bladder Control in Preclinical Study
- Rapid Clotting Gel Improves Emergency Bleeding Control
- AI Tool Predicts In-Hospital Cardiac Arrest Minutes in Advance
- Magnetic Control System Enables Precise Navigation of Miniature Medical Devices
- Shelf-Stable Synthetic Platelets Could Enable Prehospital Hemorrhage Control
- Noninvasive AI Test Aims to Enable Earlier Pulmonary Hypertension Detection
- Blood-Filtering Device May Prolong Pregnancy in Severe Early Preeclampsia
- Noninvasive Skull Sensor Detects Early Deterioration in Acute Brain Injury
- Automated Robotic Imaging System Enhances Full-Body Skin Cancer Screening
- Bacteria-Resistant Urinary Catheter Coating Reduces Infections and Antibiotic Use
- New Brain-Computer Interface Targets Treatment-Resistant Depression
- Sensor-Integrated Airway Stent Enables Continuous Remote Monitoring
- Graphene-Based Material Selectively Eliminates Bacteria While Sparing Human Cells
- Flexible Plastic Film Uses Nanostructures to Destroy Viruses
- Finger Cuff Algorithm Enables Noninvasive Screening for Aortic Stenosis
Channels
Artificial Intelligence
view channelFacial Image Analysis Tracks Biological Aging, Predicts Cancer Outcomes
Biological aging is the progressive loss of physiological function that may diverge from chronological age. In cancer care, clinicians need simple tools that reflect dynamic changes in patient resilience... Read more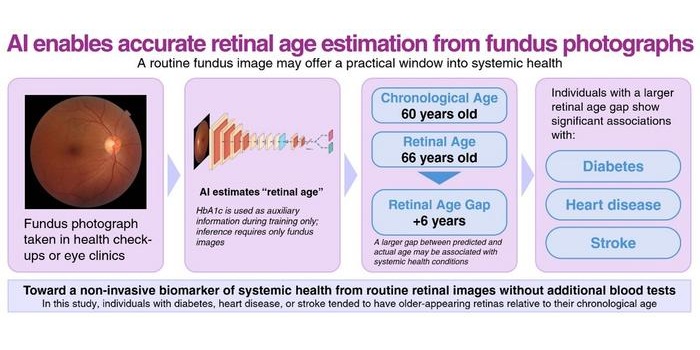
AI Model Uses Eye Imaging to Identify Risk of Major Systemic Diseases
Early detection of systemic disease risk remains a persistent challenge in population health screening. Cardiometabolic conditions such as diabetes, heart disease, and stroke often progress without symptoms... Read moreSurgical Techniques
view channel
Optical Wireless Link Enables Cable-Free 4K Endoscopic Imaging
Cabled endoscopes can hamper workflow in minimally invasive surgery and complicate infection control in the operating room. Power, lighting, and data lines drape across patients and floors, creating hygiene... Read moreGlasses-Free 3D Imaging Software Receives FDA Clearance for Surgical Planning
Clinicians often make three-dimensional decisions from two-dimensional scans, which can limit depth perception and slow shared understanding of complex anatomy during planning and consultation.... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channelBusiness
view channel
Johnson & Johnson Launches AI-Driven Cardiac Mapping System
Johnson & Johnson has introduced the CARTOSOUND SONATA Module for the CARTO System at the Heart Rhythm Society (HRS) 2026 meeting in Chicago. The module uses artificial intelligence with the CARTO... Read more