New AI System Can Diagnose and Classify Intracranial Hemorrhage
|
By HospiMedica International staff writers Posted on 23 Jan 2019 |
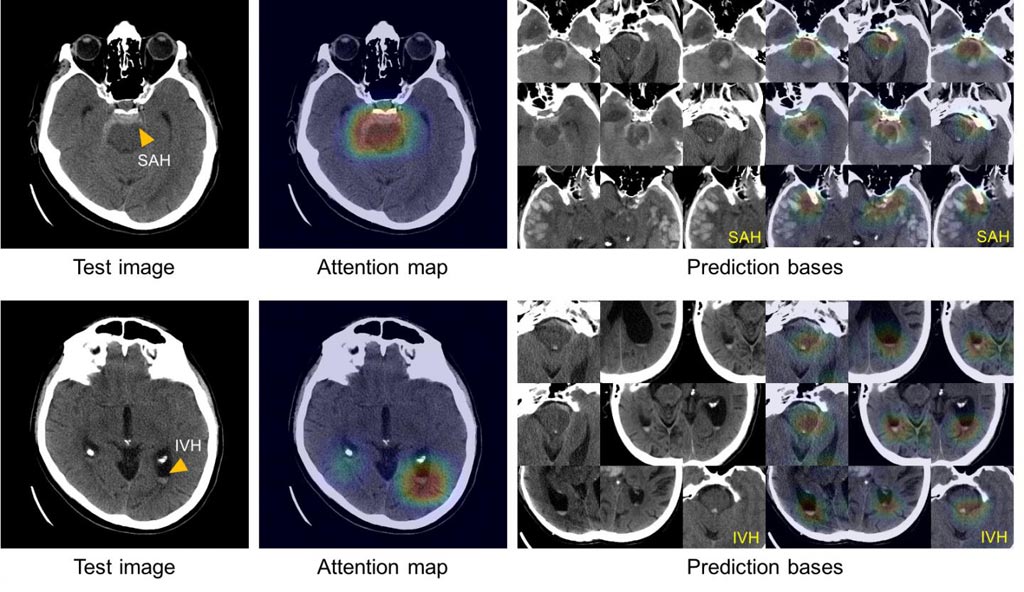
Image: These images show the system’s ability to explain its diagnosis of subarachnoid (left above) and intraventricular (left below) hemorrhage by displaying images with similar appearances (right) from an atlas of images used to train the system (Photo courtesy of Hyunkwang Lee, Harvard School of Engineering and Applied Sciences, and Sehyo Yune, MD, Massachusetts General Hospital Department of Radiology).
Researchers from the Massachusetts General Hospital (Boston, MA, USA) have developed an artificial intelligence (AI) system that can quickly diagnose and classify brain hemorrhages, as well as provide the basis of its decisions from relatively small image datasets. The system could help hospital emergency departments in evaluating patients with symptoms of a potentially life-threatening stroke, allowing rapid application of the correct treatment.
The researchers trained the system with 904 head CT scans, each consisting of around 40 individual images, that were labeled by neuroradiologists as to whether they depicted one of five hemorrhage subtypes, based on the location within the brain, or no hemorrhage. The team improved the accuracy of the deep-learning system by building in steps mimicking the way radiologists analyze images. These included adjusting factors such as contrast and brightness to reveal subtle differences not immediately apparent and scrolling through adjacent CT scan slices to determine whether or not something that appears on a single image reflects a real problem or is a meaningless artifact.
After the model system was created, the investigators tested it on two separate sets of CT scans – a retrospective set taken before the system was developed, consisting of 100 scans with and 100 without intracranial hemorrhage, and a prospective set of 79 scans with and 117 without hemorrhage, taken after the model was created. In its analysis of the retrospective set, the model system was as accurate in detecting and classifying intracranial hemorrhages as the radiologists that had reviewed the scans had been. In its analysis of the prospective set, the system proved to be even better than non-expert human readers.
To solve the “black box” problem, or the inability of systems to explain how they arrived at a decision, the team had the system review and save the images from the training dataset that most clearly represented the classic features of each of the five hemorrhage subtypes. Using this atlas of distinguishing features, the system is able to display a group of images similar to those of the CT scan being analyzed in order to explain the basis of its decisions.
“Rapid recognition of intracranial hemorrhage, leading to prompt appropriate treatment of patients with acute stroke symptoms, can prevent or mitigate major disability or death,” said co-author Michael Lev, MD, MGH Radiology. “Many facilities do not have access to specially trained neuroradiologists – especially at night or over weekends – which can require non-expert providers to determine whether or not a hemorrhage is the cause of a patient’s symptoms. The availability of a reliable, ‘virtual second opinion’ – trained by neuroradiologists – could make those providers more efficient and confident and help ensure that patients get the right treatment.”
“In addition to providing that much needed virtual second opinion, this system also could be deployed directly onto scanners, alerting the care team to the presence of a hemorrhage and triggering appropriate further testing before the patient is even off the scanner,” added co-author Shahein Tajmir, MD, MGH Radiology. “The next step will be to deploy the system into clinical areas and further validate its performance with many more cases. We are currently building a platform to allow for the widespread application of such tools throughout the department. Once we have this running in the clinical setting, we can evaluate its impact on turnaround time, clinical accuracy and the time to diagnosis.”
Related Links:
Massachusetts General Hospital
The researchers trained the system with 904 head CT scans, each consisting of around 40 individual images, that were labeled by neuroradiologists as to whether they depicted one of five hemorrhage subtypes, based on the location within the brain, or no hemorrhage. The team improved the accuracy of the deep-learning system by building in steps mimicking the way radiologists analyze images. These included adjusting factors such as contrast and brightness to reveal subtle differences not immediately apparent and scrolling through adjacent CT scan slices to determine whether or not something that appears on a single image reflects a real problem or is a meaningless artifact.
After the model system was created, the investigators tested it on two separate sets of CT scans – a retrospective set taken before the system was developed, consisting of 100 scans with and 100 without intracranial hemorrhage, and a prospective set of 79 scans with and 117 without hemorrhage, taken after the model was created. In its analysis of the retrospective set, the model system was as accurate in detecting and classifying intracranial hemorrhages as the radiologists that had reviewed the scans had been. In its analysis of the prospective set, the system proved to be even better than non-expert human readers.
To solve the “black box” problem, or the inability of systems to explain how they arrived at a decision, the team had the system review and save the images from the training dataset that most clearly represented the classic features of each of the five hemorrhage subtypes. Using this atlas of distinguishing features, the system is able to display a group of images similar to those of the CT scan being analyzed in order to explain the basis of its decisions.
“Rapid recognition of intracranial hemorrhage, leading to prompt appropriate treatment of patients with acute stroke symptoms, can prevent or mitigate major disability or death,” said co-author Michael Lev, MD, MGH Radiology. “Many facilities do not have access to specially trained neuroradiologists – especially at night or over weekends – which can require non-expert providers to determine whether or not a hemorrhage is the cause of a patient’s symptoms. The availability of a reliable, ‘virtual second opinion’ – trained by neuroradiologists – could make those providers more efficient and confident and help ensure that patients get the right treatment.”
“In addition to providing that much needed virtual second opinion, this system also could be deployed directly onto scanners, alerting the care team to the presence of a hemorrhage and triggering appropriate further testing before the patient is even off the scanner,” added co-author Shahein Tajmir, MD, MGH Radiology. “The next step will be to deploy the system into clinical areas and further validate its performance with many more cases. We are currently building a platform to allow for the widespread application of such tools throughout the department. Once we have this running in the clinical setting, we can evaluate its impact on turnaround time, clinical accuracy and the time to diagnosis.”
Related Links:
Massachusetts General Hospital
Latest AI News
- Machine Learning Approach Enhances Liver Cancer Risk Stratification
- New AI Approach Monitors Brain Health Using Passive Wearable Data
- AI Tool Maps Early Risk Patterns in Bloodstream Infections
- AI Model Identifies Rare Endocrine Disorder from Hand Images
- AI Tool Promises to Reduce Length of Hospital Stays and Free Up Beds
- Machine Learning Model Cuts Canceled Liver Transplants By 60%
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreCritical Care
view channel
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read more
First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
Pulmonary hypertension is a progressive, life‑threatening disease that is frequently missed early because symptoms such as dyspnea are nonspecific and diagnostic delays can exceed two years.... Read moreSurgical Techniques
view channel
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read more
New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
Volumetric muscle loss is a traumatic loss of skeletal muscle that often leads to permanent functional impairment and limited reconstructive options. Current experimental strategies struggle to deliver... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel






















