Removing More Blood Improves Hemorrhagic Stroke Recovery
|
By HospiMedica International staff writers Posted on 26 Feb 2019 |
Image: Professor Issam Awad demonstrating the MISTIE procedure (Photo courtesy of University of Chicago).
The greater the volume of blood removed from the brain following cerebral hemorrhage, the greater the odds of better functional recovery, claims a new study.
Researchers at Johns Hopkins University (JHU; Baltimore, MD, USA), the University of Chicago (IL, USA), and 76 other hospitals in the USA, Canada, Europe, Australia, and Asia conducted a phase 3 clinical trial in order to assess if minimally invasive catheter evacuation of blood clots, followed by thrombolysis (with the aim of decreasing the clot size to 15 mL or less), could improve functional outcome in 242 patients (average age 62 years, 63% male) who underwent an intracerebral hemorrhage (ICH) event.
The procedure, called minimally invasive surgery plus alteplase for intracerebral hemorrhage evacuation (MISTIE) starts with computerized tomography (CT)-based navigation to develop a surgical approach plan, after which a rigid cannula is placed in the middle of the intracerebral blood clot. Surgeons then insert a soft drainage catheter, which facilitates up to nine injections of alteplase and passive clot removal. Evacuation is stopped when a hematoma size of 15 mL or less is achieved, as confirmed by daily CT scans.
Study results revealed that at one year, the proportion of patients with a modified Rankin Scale (mRS) score of 3 or less was not significantly higher in patients treated with the procedure (45%), compared to those who received standard medical care (41%). However, exploratory secondary analysis found that among the 58% of patients who had their hematoma reduced to a volume of 15 mL or less, there was a 10.5% difference in the likelihood of achieving a good functional outcome. The study was presented at the annual International Stroke Conference, held during January 2019 in Honolulu (Hawaii, USA).
“When assessing the results of surgery for brain hemorrhage, it is critical to consider how much blood was successfully evacuated. Unless a large majority of clot is removed and only a very small residual of blood is left, the full benefits of surgery will not be realized,” said senior author Professor Issam Awad, MD, MSc, of the University of Chicago. “This had never been considered as a factor in the success or failure of such surgeries, and cannot be taken for granted.”
Acute stroke due to supratentorial ICH is associated with high morbidity and mortality. Trials have not shown a benefit of hematoma evacuation with open craniotomy, and current guidelines have called for more evidence before making any recommendations about routine use of surgical interventions in this setting.
Related Links:
Johns Hopkins University
University of Chicago
Researchers at Johns Hopkins University (JHU; Baltimore, MD, USA), the University of Chicago (IL, USA), and 76 other hospitals in the USA, Canada, Europe, Australia, and Asia conducted a phase 3 clinical trial in order to assess if minimally invasive catheter evacuation of blood clots, followed by thrombolysis (with the aim of decreasing the clot size to 15 mL or less), could improve functional outcome in 242 patients (average age 62 years, 63% male) who underwent an intracerebral hemorrhage (ICH) event.
The procedure, called minimally invasive surgery plus alteplase for intracerebral hemorrhage evacuation (MISTIE) starts with computerized tomography (CT)-based navigation to develop a surgical approach plan, after which a rigid cannula is placed in the middle of the intracerebral blood clot. Surgeons then insert a soft drainage catheter, which facilitates up to nine injections of alteplase and passive clot removal. Evacuation is stopped when a hematoma size of 15 mL or less is achieved, as confirmed by daily CT scans.
Study results revealed that at one year, the proportion of patients with a modified Rankin Scale (mRS) score of 3 or less was not significantly higher in patients treated with the procedure (45%), compared to those who received standard medical care (41%). However, exploratory secondary analysis found that among the 58% of patients who had their hematoma reduced to a volume of 15 mL or less, there was a 10.5% difference in the likelihood of achieving a good functional outcome. The study was presented at the annual International Stroke Conference, held during January 2019 in Honolulu (Hawaii, USA).
“When assessing the results of surgery for brain hemorrhage, it is critical to consider how much blood was successfully evacuated. Unless a large majority of clot is removed and only a very small residual of blood is left, the full benefits of surgery will not be realized,” said senior author Professor Issam Awad, MD, MSc, of the University of Chicago. “This had never been considered as a factor in the success or failure of such surgeries, and cannot be taken for granted.”
Acute stroke due to supratentorial ICH is associated with high morbidity and mortality. Trials have not shown a benefit of hematoma evacuation with open craniotomy, and current guidelines have called for more evidence before making any recommendations about routine use of surgical interventions in this setting.
Related Links:
Johns Hopkins University
University of Chicago
Latest Critical Care News
- Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
- Combined Infection Control Strategy Limits Drug-Resistant Outbreak in NICU
- AI Helps Predict Which Heart-Failure Patients Will Worsen Within a Year
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read more
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel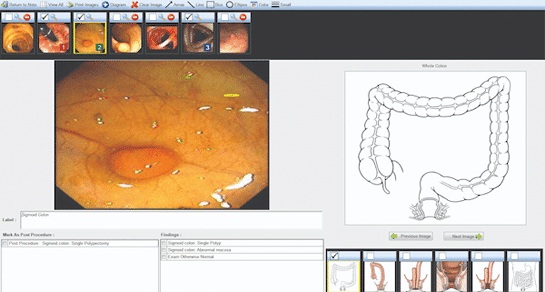
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel




















