Chemotherapy Poses Notable Risks to Healthcare Workers
|
By HospiMedica International staff writers Posted on 19 Mar 2019 |

Image: Many oncology nurses do take necessary precautions when handling chemotherapy (Photo courtesy of U-M).
A new study concludes that the use of personal protective equipment (PPE) use among oncology nurses who handle hazardous drugs is suboptimal at best.
Researchers at the University of Michigan (U-M; Ann Arbor, USA) conducted a cluster randomized trial that included 257 nurses from 12 ambulatory oncology settings between 2015 and 2017 across the United States. In one arm, 136 nurses received a one-hour educational module on PPE use with quarterly reminders; in the other, 121 nurses received a one-hour educational module, tailored messages to address perceived barriers, and quarterly data gathered on chemotherapy drugs spills and plasma samples for analysis. The primary outcome was nurse-reported PPE use.
The results revealed that after two years, both control and intervention sites reported suboptimal PPE use, with no significant differences observed in PPE use knowledge or perceived barriers. Conversely, study participants reported high satisfaction with the study experience. The study was published in the March 2019 edition of Oncology Nursing Forum.
“This is an invisible threat. It’s unlike the needle stick, where you know when you’ve been stuck by a needle. Early on we could understand that a needle stick conveyed serious health risks. With chemotherapy exposure, we don’t have that smoking gun,” said lead author Professor Christopher Friese, PhD, RN, of the U-M Rogel Cancer Center. “This is a subtle threat, but it’s a daily threat. As a practicing nurse it’s disappointing; we were hoping we could develop a bundled intervention that cancer centers and others can use.”
Guidelines from professional societies recommend handling chemotherapy drugs using protective gear that includes double gloving, eye protection, respirators, and a thick, disposable gown made from a fabric of low permeability with back closure. Eye and face protection is also advised when splashing is a risk. However, not using protective gear is common, according to an anonymous poll conducted at the 2016 Oncology Nursing Society annual meeting. More than one third of respondents said they did not change their gown or double-glove, because the equipment was not conveniently located. Others said they skipped wearing the gear because it was too uncomfortable.
Related Links:
University of Michigan
Researchers at the University of Michigan (U-M; Ann Arbor, USA) conducted a cluster randomized trial that included 257 nurses from 12 ambulatory oncology settings between 2015 and 2017 across the United States. In one arm, 136 nurses received a one-hour educational module on PPE use with quarterly reminders; in the other, 121 nurses received a one-hour educational module, tailored messages to address perceived barriers, and quarterly data gathered on chemotherapy drugs spills and plasma samples for analysis. The primary outcome was nurse-reported PPE use.
The results revealed that after two years, both control and intervention sites reported suboptimal PPE use, with no significant differences observed in PPE use knowledge or perceived barriers. Conversely, study participants reported high satisfaction with the study experience. The study was published in the March 2019 edition of Oncology Nursing Forum.
“This is an invisible threat. It’s unlike the needle stick, where you know when you’ve been stuck by a needle. Early on we could understand that a needle stick conveyed serious health risks. With chemotherapy exposure, we don’t have that smoking gun,” said lead author Professor Christopher Friese, PhD, RN, of the U-M Rogel Cancer Center. “This is a subtle threat, but it’s a daily threat. As a practicing nurse it’s disappointing; we were hoping we could develop a bundled intervention that cancer centers and others can use.”
Guidelines from professional societies recommend handling chemotherapy drugs using protective gear that includes double gloving, eye protection, respirators, and a thick, disposable gown made from a fabric of low permeability with back closure. Eye and face protection is also advised when splashing is a risk. However, not using protective gear is common, according to an anonymous poll conducted at the 2016 Oncology Nursing Society annual meeting. More than one third of respondents said they did not change their gown or double-glove, because the equipment was not conveniently located. Others said they skipped wearing the gear because it was too uncomfortable.
Related Links:
University of Michigan
Latest Critical Care News
- Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
- Eye Imaging AI Identifies Elevated Cardiovascular Risk
- Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreSurgical Techniques
view channel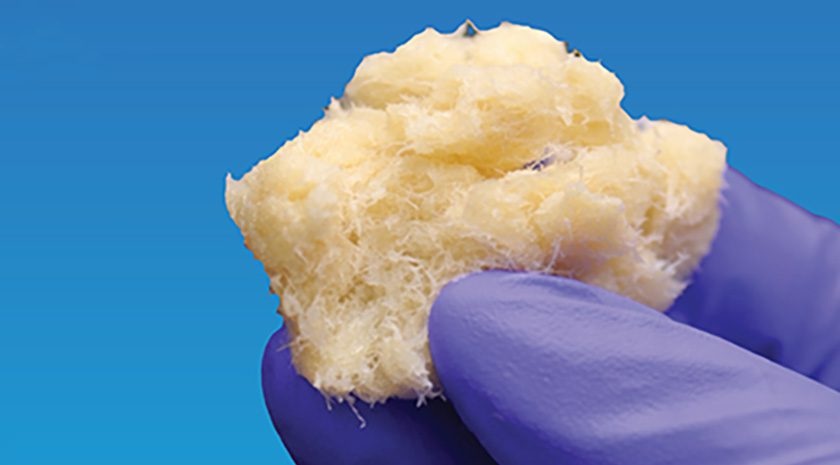
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel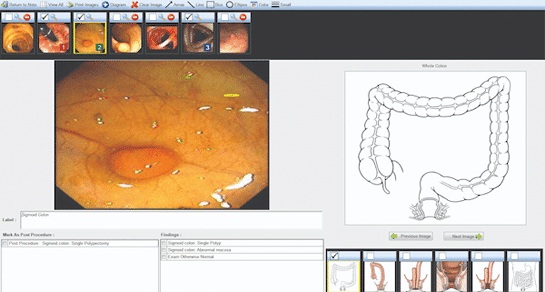
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel