New AI Method Predicts Breast Cancer Five Years in Advance
|
By HospiMedica International staff writers Posted on 18 May 2019 |
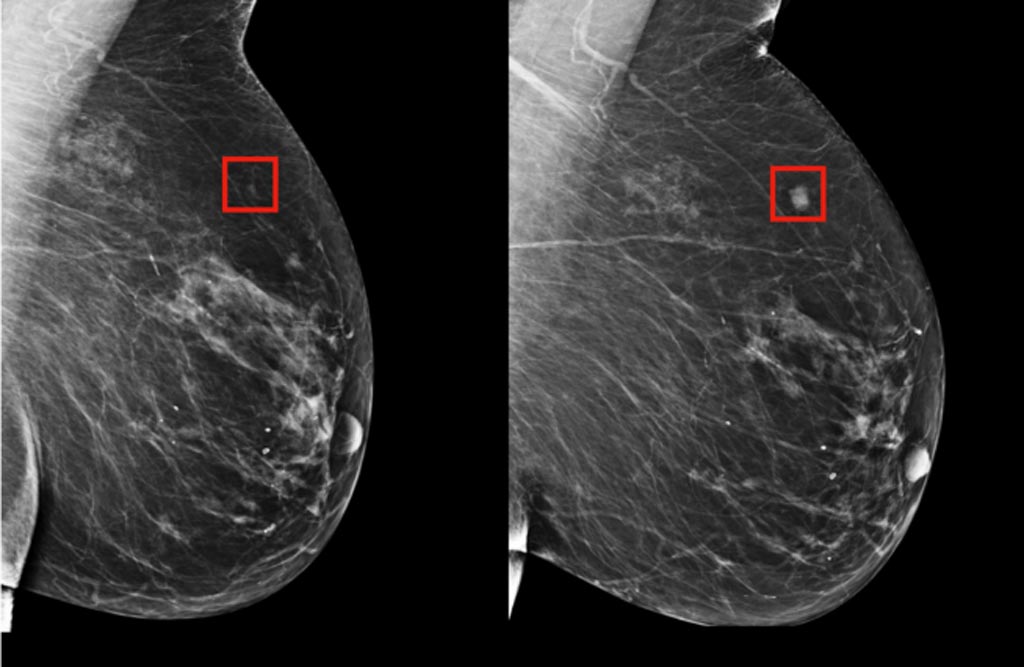
Image: A new AI method for detecting breast cancer is expected to surpass existing methods that fall short in their predictions (Photo courtesy of MIT).
Researchers from two major institutions have developed a new tool with advanced artificial intelligence (AI) methods to predict a woman’s future risk of breast cancer. The currently available models that use factors such as family history and genetics fall far short in predicting an individual woman’s likelihood of being diagnosed with breast cancer.
In some models, breast density—the amount of dense tissue compared to the amount of fatty tissue in the breast on a mammogram— has been added to improve risk assessment as it is an independent risk factor for breast cancer. Since it is based on subjective assessment that can vary across radiologists, deep learning, a subset of AI in which computers learn by example, has been studied as a way to standardize and automate these measurements.
Adam Yala, a Ph.D. candidate at the Massachusetts Institute of Technology (MIT), in collaboration with Regina Barzilay, Ph.D., an AI expert and professor at MIT, and Constance Lehman, M.D, Ph.D., chief of breast imaging at Massachusetts General Hospital and professor of radiology at Harvard Medical School, recently compared three different risk assessment approaches.
The first model relied on traditional risk factors, the second on deep learning that used the mammogram alone, and the third on a hybrid approach that incorporated both the mammogram and traditional risk factors into the deep learning model. The researchers used nearly 90,000 full-resolution screening mammograms from about 40,000 women to train, validate and test the deep learning model. They were able to obtain cancer outcomes through linkage to a regional tumor registry.
The deep learning models yielded substantially improved risk discrimination over the Tyrer-Cuzick model, a current clinical standard that uses breast density in factoring risk. When comparing the hybrid deep learning model against breast density, the researchers found that patients with non-dense breasts and model-assessed high risk had 3.9 times the cancer incidence of patients with dense breasts and model-assessed low risk. The advantages held across different subgroups of women.
“There’s much more information in a mammogram than just the four categories of breast density. By using the deep learning model, we learn subtle cues that are indicative of future cancer,” said Yala. “There’s a very large amount of information in a full-resolution mammogram that breast cancer risk models have not been able to use until recently. Using deep learning, we can learn to leverage that information directly from the data and create models that are significantly more accurate across diverse populations.”
“Unlike traditional models, our deep learning model performs equally well across diverse races, ages and family histories,” Dr. Barzilay said. “Until now, African-American women were at a distinct disadvantage in having accurate risk assessment of future breast cancer. Our AI model has changed that.”
“A missing element to support more effective, more personalized screening programs has been risk-assessment tools that are easy to implement and that work across the full diversity of women whom we serve,” Dr. Lehman said. “We are thrilled with our results and eager to work closely with our health care systems, our providers and, most importantly, our patients to incorporate this discovery into improved outcomes for all women.”
Related Links:
MIT
In some models, breast density—the amount of dense tissue compared to the amount of fatty tissue in the breast on a mammogram— has been added to improve risk assessment as it is an independent risk factor for breast cancer. Since it is based on subjective assessment that can vary across radiologists, deep learning, a subset of AI in which computers learn by example, has been studied as a way to standardize and automate these measurements.
Adam Yala, a Ph.D. candidate at the Massachusetts Institute of Technology (MIT), in collaboration with Regina Barzilay, Ph.D., an AI expert and professor at MIT, and Constance Lehman, M.D, Ph.D., chief of breast imaging at Massachusetts General Hospital and professor of radiology at Harvard Medical School, recently compared three different risk assessment approaches.
The first model relied on traditional risk factors, the second on deep learning that used the mammogram alone, and the third on a hybrid approach that incorporated both the mammogram and traditional risk factors into the deep learning model. The researchers used nearly 90,000 full-resolution screening mammograms from about 40,000 women to train, validate and test the deep learning model. They were able to obtain cancer outcomes through linkage to a regional tumor registry.
The deep learning models yielded substantially improved risk discrimination over the Tyrer-Cuzick model, a current clinical standard that uses breast density in factoring risk. When comparing the hybrid deep learning model against breast density, the researchers found that patients with non-dense breasts and model-assessed high risk had 3.9 times the cancer incidence of patients with dense breasts and model-assessed low risk. The advantages held across different subgroups of women.
“There’s much more information in a mammogram than just the four categories of breast density. By using the deep learning model, we learn subtle cues that are indicative of future cancer,” said Yala. “There’s a very large amount of information in a full-resolution mammogram that breast cancer risk models have not been able to use until recently. Using deep learning, we can learn to leverage that information directly from the data and create models that are significantly more accurate across diverse populations.”
“Unlike traditional models, our deep learning model performs equally well across diverse races, ages and family histories,” Dr. Barzilay said. “Until now, African-American women were at a distinct disadvantage in having accurate risk assessment of future breast cancer. Our AI model has changed that.”
“A missing element to support more effective, more personalized screening programs has been risk-assessment tools that are easy to implement and that work across the full diversity of women whom we serve,” Dr. Lehman said. “We are thrilled with our results and eager to work closely with our health care systems, our providers and, most importantly, our patients to incorporate this discovery into improved outcomes for all women.”
Related Links:
MIT
Latest AI News
- Machine Learning Approach Enhances Liver Cancer Risk Stratification
- New AI Approach Monitors Brain Health Using Passive Wearable Data
- AI Tool Maps Early Risk Patterns in Bloodstream Infections
- AI Model Identifies Rare Endocrine Disorder from Hand Images
- AI Tool Promises to Reduce Length of Hospital Stays and Free Up Beds
- Machine Learning Model Cuts Canceled Liver Transplants By 60%
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreCritical Care
view channel
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read more
First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
Pulmonary hypertension is a progressive, life‑threatening disease that is frequently missed early because symptoms such as dyspnea are nonspecific and diagnostic delays can exceed two years.... Read moreSurgical Techniques
view channel
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read more
New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
Volumetric muscle loss is a traumatic loss of skeletal muscle that often leads to permanent functional impairment and limited reconstructive options. Current experimental strategies struggle to deliver... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel