Bioelectronic Therapy Device Exercises Heart Muscle
|
By HospiMedica International staff writers Posted on 22 Jul 2019 |
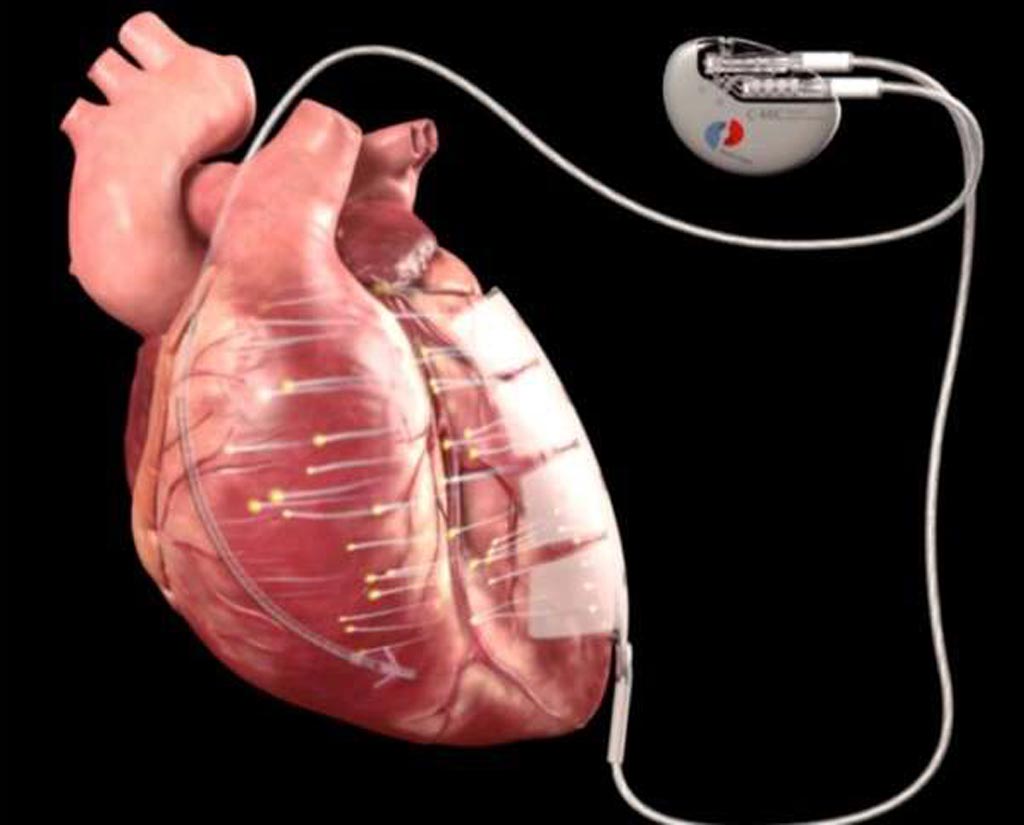
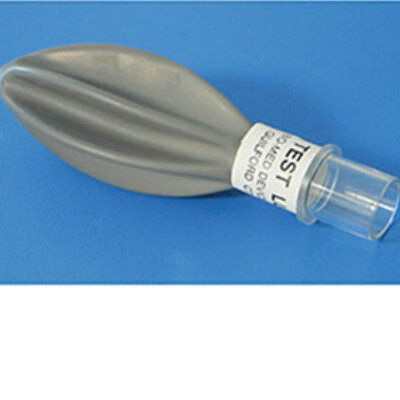
Image: The implanted device is designed to stimulate cell regeneration in cardiomyopathy (Photo courtesy of Berlin Heals).
A novel electroceutical device readjusts the myocardial electrical gradient in order to strengthen the weakened heart muscle of cardiomyopathy patients.
Under development by Berlin Heals (Berlin, Germany), C-MIC cardiac microcurrent therapy is based on an implanted pulse generator that exercises the heart muscle using electricity, thus stimulating it to renew itself. In a minimally invasive procedure, a small microcurrent pulse generator is implanted via two small incisions. Two electrodes exit the pulse generator, one taking the form of an extensive patch on the outside of the heart muscle, while the other is placed inside the left ventricle. The system is designed to stimulate the affected heart muscle, causing it to regenerate.
In a preclinical study at Hannover Medical School (Germany) involving 12 sheep with chronic systolic heart failure, the continuous microcurrent therapy was associated with a strong improvement of left ventricular ejection fraction (LVEF), indicating reversal of cardiac remodeling and reduced myocardial inflammation. A first in human study of the C-MIC device at the Medical University of Vienna (MedUni; Austria) revealed that after three months, the first patient treated showing initial signs of regeneration. The study was published in the April 2019 issue of The Journal of Heart and Lung Transplantation.
“The preliminary findings bring us real hope for cardiomyopathy patients. Microcurrent regeneration could bring us a step closer to the dream of being able to regenerate damaged organs,” said lead author Dominik Wiedemann, MD, of the MedUni division of cardiac surgery. “Particularly in times when donor organs are scarce, it is important to develop new effective treatment techniques to avoid major operations such as heart transplants as much as possible, as well as the subsequent immunosuppression that goes with them."
In dilative cardiomyopathy, the heart muscle becomes pathologically enlarged so that it can no longer contract sufficiently. Current treatments attempt to stabilize such heart failure patients for as long as possible by means of optimized drug treatment or specialized pacemakers. The treatment of last resort for terminal heart failure is a heart transplant or mechanical replacement using a left ventricular assist device (LVAD).
Related Links:
Berlin Heals
Hannover Medical School
Medical University of Vienna
Under development by Berlin Heals (Berlin, Germany), C-MIC cardiac microcurrent therapy is based on an implanted pulse generator that exercises the heart muscle using electricity, thus stimulating it to renew itself. In a minimally invasive procedure, a small microcurrent pulse generator is implanted via two small incisions. Two electrodes exit the pulse generator, one taking the form of an extensive patch on the outside of the heart muscle, while the other is placed inside the left ventricle. The system is designed to stimulate the affected heart muscle, causing it to regenerate.
In a preclinical study at Hannover Medical School (Germany) involving 12 sheep with chronic systolic heart failure, the continuous microcurrent therapy was associated with a strong improvement of left ventricular ejection fraction (LVEF), indicating reversal of cardiac remodeling and reduced myocardial inflammation. A first in human study of the C-MIC device at the Medical University of Vienna (MedUni; Austria) revealed that after three months, the first patient treated showing initial signs of regeneration. The study was published in the April 2019 issue of The Journal of Heart and Lung Transplantation.
“The preliminary findings bring us real hope for cardiomyopathy patients. Microcurrent regeneration could bring us a step closer to the dream of being able to regenerate damaged organs,” said lead author Dominik Wiedemann, MD, of the MedUni division of cardiac surgery. “Particularly in times when donor organs are scarce, it is important to develop new effective treatment techniques to avoid major operations such as heart transplants as much as possible, as well as the subsequent immunosuppression that goes with them."
In dilative cardiomyopathy, the heart muscle becomes pathologically enlarged so that it can no longer contract sufficiently. Current treatments attempt to stabilize such heart failure patients for as long as possible by means of optimized drug treatment or specialized pacemakers. The treatment of last resort for terminal heart failure is a heart transplant or mechanical replacement using a left ventricular assist device (LVAD).
Related Links:
Berlin Heals
Hannover Medical School
Medical University of Vienna
Latest Critical Care News
- Combined Infection Control Strategy Limits Drug-Resistant Outbreak in NICU
- Cancer-Seeking Microbubbles Make Tumor Cells Self-Destruct
- Eye Movement Tests Uncover Hidden Brain Changes Years After Concussion
- Simple 5-Minute Questionnaire Test Speeds Endometriosis Diagnosis
- Nanohydrogels Guide Medicine to Tumors Without Damaging Healthy Tissue
- Magnetic Gel Offers Safer and More Effective Atrial Fibrillation Treatment
- Hydrogel Biosensor Detects and Differentiates Blood Circulation Complications
- Spray-Type Technology Coats Transplant Organs with Immunosuppressants to Prevent Rejection
- Single Heart Attack Shot to Revolutionize Cardiac Care
- Machine-Learning Model Predicts Preeclampsia in Late Pregnancy
- Single Mid-Wave Infrared Thermal Camera Enables Noncontact Vital Signs Monitoring
- 3D-Printed Bandage to Help Heal Chronic Wounds
- Ultrasound-Activated Nanoagents Kill Superbugs Hiding in Biofilms
- Painless Microneedle Skin Patch Monitors Immune Health

- Smart T-Shirt Uses AI to Enhance Detection of Heart Rhythm Disorders
- Aptamers Enable Real-Time Biomarker Tracking Without Blood Draws
Channels
Artificial Intelligence
view channel
AI Model Identifies Rare Endocrine Disorder from Hand Images
Acromegaly is a rare, intractable disease that typically begins in middle age and causes enlargement of the hands and feet, changes in facial appearance, and abnormal bone and organ growth.... Read moreSurgical Techniques
view channel
VR Experience Reduces Patient Anxiety Before Kidney Stone Procedure
Many patients experience anxiety and limited comprehension when preparing for invasive or device-assisted care. Complex consent materials can leave people uncertain about risks, benefits, and what to expect... Read more
Robot-Assisted Brain Angiography Improves Procedural Outcomes
Digital subtraction angiography remains the gold standard for diagnosing cerebrovascular conditions such as intracranial aneurysms, arteriovenous malformations, and arterial stenosis. However, the procedure... Read morePatient Care
view channel
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read more
VR Training Tool Combats Contamination of Portable Medical Equipment
Healthcare-associated infections (HAIs) impact one in every 31 patients, cause nearly 100,000 deaths each year, and cost USD 28.4 billion in direct medical expenses. Notably, up to 75% of these infections... Read more
Portable Biosensor Platform to Reduce Hospital-Acquired Infections
Approximately 4 million patients in the European Union acquire healthcare-associated infections (HAIs) or nosocomial infections each year, with around 37,000 deaths directly resulting from these infections,... Read moreFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel
Quantum Surgical Acquires NeuWave from Johnson & Johnson
Quantum Surgical announced that it has acquired NeuWave Medical from Johnson & Johnson. NeuWave’s microwave ablation system is used in percutaneous tumor ablation procedures, and the acquisition supports... Read more
Medtronic to Acquire Coronary Artery Medtech Company CathWorks
Medtronic plc (Galway, Ireland) has announced that it will exercise its option to acquire CathWorks (Kfar Saba, Israel), a privately held medical device company, which aims to transform how coronary artery... Read more