Cardiac Telemetry Improves AF Detection Following Stroke
|
By HospiMedica International staff writers Posted on 23 Jul 2019 |
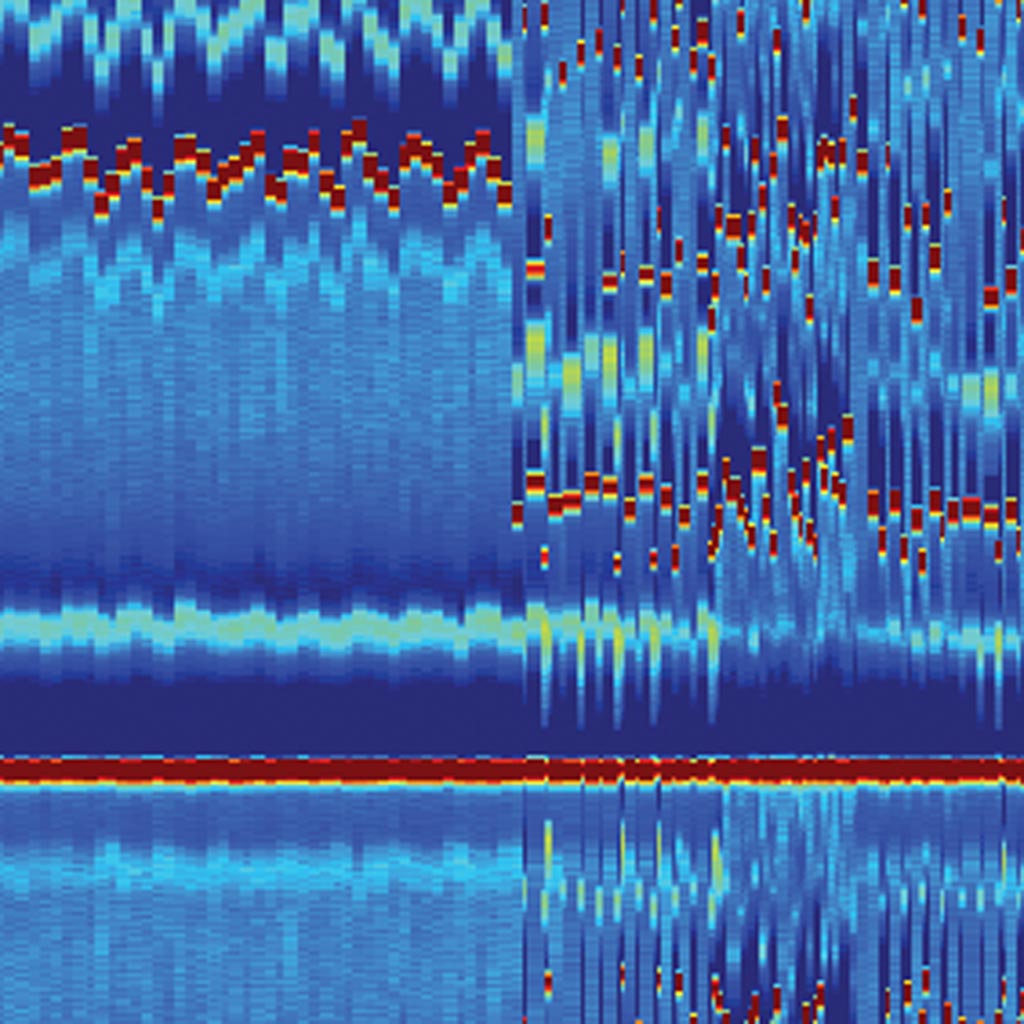
Image: An example of an electrocardiomatrix, with flagged events (Photo courtesy of U-M).
A new study describes how electrocardiogram (ECG) telemetry data is analyzed in a three-dimensional (3D) matrix to allow for more accurate P-wave analysis.
Developed at the University of Michigan (U-M; Ann Arbor, USA), electrocardiomatrix is designed to convert two-dimensional signals from a patient’s ECG into a 3D heatmap so as to provide fast, intuitive detection of cardiac arrhythmias. To test the technology, U-M researchers conducted a prospective, observational study that analyzed data from 265 ischemic stroke and transient ischemic attack (TIA) patients between April 2017 and January 2018. Atrial fibrillation (AF) episodes lasting more than 30 seconds were identified through review of electrocardiomatrix matrices by a non-cardiologist.
The electrocardiomatrix results were then compared with AF identified directly by a cardiologist through standard telemetry. The results revealed that electrocardiomatrix successfully identified AF in 260 (98%) of cases. The positive predictive value of electrocardiomatrix compared with the clinical documentation was 86% overall, and 100% among a subset of patients with no history of AF. For the five false-positive and five false-negative cases, expert overview disagreed with the clinical documentation and confirmed the electrocardiomatrix-based diagnosis. The study was published on July 1, 2019, in Stroke.
“Electrocardiomatrix goes further than standard cardiac telemetry by examining large amounts of telemetry data in a way that's so detailed it's impractical for individual clinicians to attempt,” said senior author and electrocardiomatrix co-inventor Jimo Borjigin, PhD, of the department of molecular and integrative physiology at U-M Medical School. “Importantly, the electrocardiomatrix identification method was highly accurate for the 212 patients who did not have a history of AF. This group is most clinically relevant, because of the importance of determining whether stroke patients have previously undetected AF.”
“After a stroke, neurologists are tasked with identifying which risk factors may have contributed in order to do everything possible to prevent another event. That makes detecting irregular heartbeat an urgent concern for these patients,” said lead author professor of neurology Devin Brown, MD. “As a physician can't reasonably review every single heartbeat, current monitoring technology flags heart rates that are too high. More accurate identification of AF should translate into more strokes prevented.”
Related Links:
University of Michigan
Developed at the University of Michigan (U-M; Ann Arbor, USA), electrocardiomatrix is designed to convert two-dimensional signals from a patient’s ECG into a 3D heatmap so as to provide fast, intuitive detection of cardiac arrhythmias. To test the technology, U-M researchers conducted a prospective, observational study that analyzed data from 265 ischemic stroke and transient ischemic attack (TIA) patients between April 2017 and January 2018. Atrial fibrillation (AF) episodes lasting more than 30 seconds were identified through review of electrocardiomatrix matrices by a non-cardiologist.
The electrocardiomatrix results were then compared with AF identified directly by a cardiologist through standard telemetry. The results revealed that electrocardiomatrix successfully identified AF in 260 (98%) of cases. The positive predictive value of electrocardiomatrix compared with the clinical documentation was 86% overall, and 100% among a subset of patients with no history of AF. For the five false-positive and five false-negative cases, expert overview disagreed with the clinical documentation and confirmed the electrocardiomatrix-based diagnosis. The study was published on July 1, 2019, in Stroke.
“Electrocardiomatrix goes further than standard cardiac telemetry by examining large amounts of telemetry data in a way that's so detailed it's impractical for individual clinicians to attempt,” said senior author and electrocardiomatrix co-inventor Jimo Borjigin, PhD, of the department of molecular and integrative physiology at U-M Medical School. “Importantly, the electrocardiomatrix identification method was highly accurate for the 212 patients who did not have a history of AF. This group is most clinically relevant, because of the importance of determining whether stroke patients have previously undetected AF.”
“After a stroke, neurologists are tasked with identifying which risk factors may have contributed in order to do everything possible to prevent another event. That makes detecting irregular heartbeat an urgent concern for these patients,” said lead author professor of neurology Devin Brown, MD. “As a physician can't reasonably review every single heartbeat, current monitoring technology flags heart rates that are too high. More accurate identification of AF should translate into more strokes prevented.”
Related Links:
University of Michigan
Latest Critical Care News
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
- Combined Infection Control Strategy Limits Drug-Resistant Outbreak in NICU
- AI Helps Predict Which Heart-Failure Patients Will Worsen Within a Year
- Algorithm Allows Paramedics to Predict Brain Damage Risk After Cardiac Arrest
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreSurgical Techniques
view channel
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read more
New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
Volumetric muscle loss is a traumatic loss of skeletal muscle that often leads to permanent functional impairment and limited reconstructive options. Current experimental strategies struggle to deliver... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel