Machine Learning Approach Predicts Surgery Duration
|
By HospiMedica International staff writers Posted on 01 Aug 2019 |
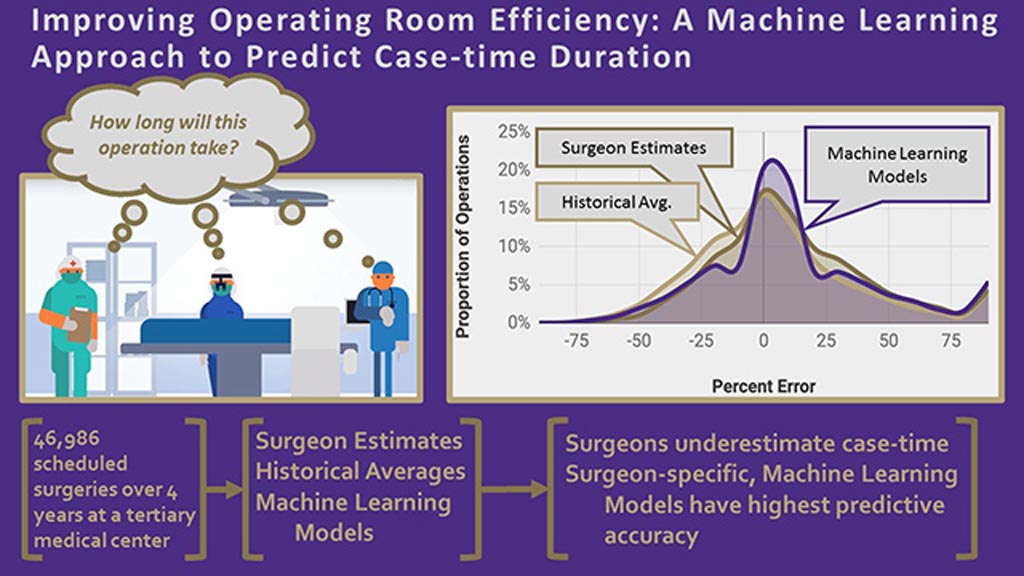
Image: A graphical abstract of the OR AI algorithm (Photo courtesy of UW).
A novel artificial intelligence (AI) based statistical model uses large retrospective datasets to improve estimation of surgical procedures duration.
Researchers at the University of Washington (UW; Seattle, USA) and Perimatics (Bellevue, WA, USA) used a dataset that included 46,986 scheduled surgeries performed by 92 surgeons at UW between January 2014 and December 2017 in order to develop, test, and train machine learning (ML) statistical models that could improve operating room (OR) efficiency by better predicting case-time duration. The models were developed on a training dataset that included 80% of the dataset, and validated on a testing dataset of the remaining 20%.
The predictions derived by ML were then compared to average historical procedure times and surgeon estimates, with individual models created for each surgical service and surgeon, respectively. The results showed that the ML algorithm could predict case times within a 10% threshold. Surgeon-specific models were able to improve accuracy from 30% (based on a surgeon's estimate) to 39%, and among the top one-third of surgeons, accuracy improved to more than 50%. The study was published on July 18, 2019, in the Journal of the American College of Surgeons (JACS).
“OR scheduling is a five billion dollar problem. To optimize the OR, you have to answer a fundamental question: How long does each surgery take? Underutilization means fewer patients get surgical care and the hospital has excess capacity. Overutilization results in cancelled operations and overtime expenses,” said study co-lead author Rajeev Saxena, MD, of the UW School of Medicine. “You can change an entire organizational culture by taking a data-forward approach and engaging key stakeholders.”
Many variables need to be considered when attempting to optimize surgical scheduling, including case duration, patient waiting time for surgery, and the number of blocks of OR time given to each surgeon or surgical service, as determined by OR committees. A utilization threshold of 75% is appropriate for most ORs, but if a hospital can strengthen OR utilization, it can grow revenue by increasing total case volume.
Related Links:
University of Washington
Perimatics
Researchers at the University of Washington (UW; Seattle, USA) and Perimatics (Bellevue, WA, USA) used a dataset that included 46,986 scheduled surgeries performed by 92 surgeons at UW between January 2014 and December 2017 in order to develop, test, and train machine learning (ML) statistical models that could improve operating room (OR) efficiency by better predicting case-time duration. The models were developed on a training dataset that included 80% of the dataset, and validated on a testing dataset of the remaining 20%.
The predictions derived by ML were then compared to average historical procedure times and surgeon estimates, with individual models created for each surgical service and surgeon, respectively. The results showed that the ML algorithm could predict case times within a 10% threshold. Surgeon-specific models were able to improve accuracy from 30% (based on a surgeon's estimate) to 39%, and among the top one-third of surgeons, accuracy improved to more than 50%. The study was published on July 18, 2019, in the Journal of the American College of Surgeons (JACS).
“OR scheduling is a five billion dollar problem. To optimize the OR, you have to answer a fundamental question: How long does each surgery take? Underutilization means fewer patients get surgical care and the hospital has excess capacity. Overutilization results in cancelled operations and overtime expenses,” said study co-lead author Rajeev Saxena, MD, of the UW School of Medicine. “You can change an entire organizational culture by taking a data-forward approach and engaging key stakeholders.”
Many variables need to be considered when attempting to optimize surgical scheduling, including case duration, patient waiting time for surgery, and the number of blocks of OR time given to each surgeon or surgical service, as determined by OR committees. A utilization threshold of 75% is appropriate for most ORs, but if a hospital can strengthen OR utilization, it can grow revenue by increasing total case volume.
Related Links:
University of Washington
Perimatics
Latest AI News
- Machine Learning Approach Enhances Liver Cancer Risk Stratification
- New AI Approach Monitors Brain Health Using Passive Wearable Data
- AI Tool Maps Early Risk Patterns in Bloodstream Infections
- AI Model Identifies Rare Endocrine Disorder from Hand Images
- AI Tool Promises to Reduce Length of Hospital Stays and Free Up Beds
- Machine Learning Model Cuts Canceled Liver Transplants By 60%
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreCritical Care
view channel
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read more
First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
Pulmonary hypertension is a progressive, life‑threatening disease that is frequently missed early because symptoms such as dyspnea are nonspecific and diagnostic delays can exceed two years.... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel