Metabolic Surgery Reduces Incident Adverse CV Events
|
By HospiMedica International staff writers Posted on 26 Sep 2019 |
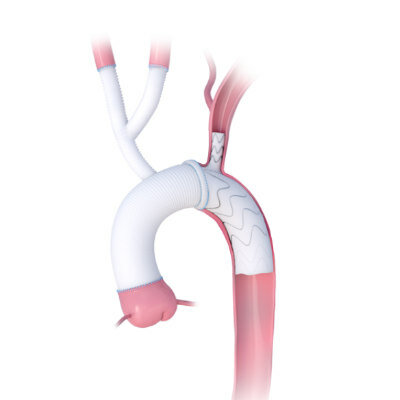
Metabolic surgery is associated with reduced incident major adverse cardiovascular events (MACE) in patients with type 2 diabetes (T2D) and obesity, according to a new study.
Researchers at the Cleveland Clinic (CC, OH, USA), Ohio State University (OSU, Columbus, USA), and other institutions conducted a retrospective cohort study of 13,722 patients to investigate the relationship between metabolic surgery and MACE in patients with T2D and obesity. In all, 2,287 study participants were matched 1:5 to nonsurgical patients, resulting in 11,435 control patients, with follow-up through December 2018. The primary outcome was incidence of extended MACE, a composite of six outcomes (all-cause mortality, heart failure, coronary artery events, cerebrovascular events, nephropathy, and atrial fibrillation).
The results revealed that at the end of the study period, 385 patients (30.8%) in the surgical group and 3,243 patients (47.7%) in the nonsurgical group experienced a primary end point, an absolute 8-year risk difference of 16.9%. All-cause mortality occurred in 112 patients (10%) in the metabolic surgery group and 1,111 patients (17.8%) in the nonsurgical group. Metabolic surgery was significantly associated with a lower risk of incident MACE, for a hazard ratio of 0.61. The study was published on September 2, 2019, in the Journal of the American Medical Association (JAMA).
“Although metabolic surgery, defined as procedures that influence metabolism by inducing weight loss and altering gastrointestinal physiology, significantly improves cardiometabolic risk factors, the effect on cardiovascular outcomes has been less well characterized,” concluded lead author Ali Aminian, MD, of the Cleveland Clinic, and colleagues. “The findings from this observational study must be confirmed in randomized clinical trials.”
Metabolic surgery, in contrast to bariatric surgery, is intended to specifically address T2D that fails to respond to lifestyle and medication changes, rather than obesity as such. Bariatric surgery is generally performed in those with a body mass index (BMI) of at least 40 kg/m2, compared to metabolic surgery, which includes participants with BMIs as low as 27 kg/m2. And whereas those undergoing bariatric surgery are relatively young and predominantly female, with few cardiometabolic abnormalities, those undergoing metabolic surgery are older, a higher proportion are men, and with more cardiometabolic comorbidities, and even overt cardiovascular disease.
Related Links:
Cleveland Clinic
Ohio State University
Researchers at the Cleveland Clinic (CC, OH, USA), Ohio State University (OSU, Columbus, USA), and other institutions conducted a retrospective cohort study of 13,722 patients to investigate the relationship between metabolic surgery and MACE in patients with T2D and obesity. In all, 2,287 study participants were matched 1:5 to nonsurgical patients, resulting in 11,435 control patients, with follow-up through December 2018. The primary outcome was incidence of extended MACE, a composite of six outcomes (all-cause mortality, heart failure, coronary artery events, cerebrovascular events, nephropathy, and atrial fibrillation).
The results revealed that at the end of the study period, 385 patients (30.8%) in the surgical group and 3,243 patients (47.7%) in the nonsurgical group experienced a primary end point, an absolute 8-year risk difference of 16.9%. All-cause mortality occurred in 112 patients (10%) in the metabolic surgery group and 1,111 patients (17.8%) in the nonsurgical group. Metabolic surgery was significantly associated with a lower risk of incident MACE, for a hazard ratio of 0.61. The study was published on September 2, 2019, in the Journal of the American Medical Association (JAMA).
“Although metabolic surgery, defined as procedures that influence metabolism by inducing weight loss and altering gastrointestinal physiology, significantly improves cardiometabolic risk factors, the effect on cardiovascular outcomes has been less well characterized,” concluded lead author Ali Aminian, MD, of the Cleveland Clinic, and colleagues. “The findings from this observational study must be confirmed in randomized clinical trials.”
Metabolic surgery, in contrast to bariatric surgery, is intended to specifically address T2D that fails to respond to lifestyle and medication changes, rather than obesity as such. Bariatric surgery is generally performed in those with a body mass index (BMI) of at least 40 kg/m2, compared to metabolic surgery, which includes participants with BMIs as low as 27 kg/m2. And whereas those undergoing bariatric surgery are relatively young and predominantly female, with few cardiometabolic abnormalities, those undergoing metabolic surgery are older, a higher proportion are men, and with more cardiometabolic comorbidities, and even overt cardiovascular disease.
Related Links:
Cleveland Clinic
Ohio State University
Latest Surgical Techniques News
- Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
- New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
- Robot-Assisted Brain Angiography Improves Procedural Outcomes
- Brain Mapping Technology Enhances Precision in Brain Tumor Resection
- Handheld Robotic System Expands Options for Total Knee Surgery
- VR Experience Reduces Patient Anxiety Before Kidney Stone Procedure
- Injectable Mini Livers Offer Hope for Patients Awaiting Transplant
- Pulsed Field Ablation Technology Cleared in Europe for Persistent AFib
- AI-Powered Imaging Brings Real-Time Margin Clarity to Breast Cancer Surgery
- Minimally Invasive Device Safely Treats Challenging Brain Aneurysms
- Surgical Robot Makes Complex Liver Tumor Surgery Safer and Less Invasive
- Neurostimulation Implant Reduces Seizure Burden in Drug-Resistant Epilepsy
- Minimally Invasive Procedure Effectively Treats Small Kidney Cancers
- Fluorescence Probe Paired with Engineered Enzymes Lights Up Tumors for Easier Surgical Removal
- Novel Hydrogel Could Become Bone Implant of the Future
- Skull Implant Design Could Shape Surgical Outcomes
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreCritical Care
view channel
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read more
First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
Pulmonary hypertension is a progressive, life‑threatening disease that is frequently missed early because symptoms such as dyspnea are nonspecific and diagnostic delays can exceed two years.... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel