Headache after Childbirth Epidural Could Indicate Subdural Hematoma
|
By HospiMedica International staff writers Posted on 29 Oct 2019 |
Women who experience headaches following neuraxial anesthesia prior to giving birth have a greater risk of developing intracranial subdural hematoma (ISH), according to a new study.
Researchers at McGill University (Montreal, Canada) and the University of Toronto (UT; Canada) reviewed the outcomes of 22,130,815 patients and deliveries in the United States between January 2010 and December 2016 in order to determine the association of post–dural puncture headache with postpartum ISH. Patients were included if they had two months of follow-up data, and did not receive a diagnostic lumbar puncture. The main outcome was ISH in the two-month postpartum period, with secondary outcomes including in-hospital mortality and occurrence of neurosurgery.
In all, there were 68,374 post–dural puncture headaches, for an overall rate of 309 per 100,000. There were 342 cases of ISH identified, indicating an incidence rate of 1.5 per 100,000 women. Of these, 100 cases were in women with post–dural puncture headache, indicating a rate of 147 hematoma cases per 100,000 deliveries in this subgroup. After adjustment for maternal age, cesarean delivery, hypertension, preeclampsia, and other co-morbidities, post–dural puncture headache had an odds ratio for subdural hematoma of 199, and an adjusted absolute risk increase of 130 per 100,000 deliveries. The study was published on September 16, 2019, in JAMA Neurology.
“When a patient has a post-dural puncture headache, they are at risk for a subdural hematoma, which can result in serious morbidity and increased mortality, and needs to be considered by any clinician looking after these patients,” said lead author Albert Moore, MD, of McGill University. “The risk is higher in patients who have coagulopathy, previous cerebral arteriovenous malformations, and hypertensive disease, and there is also a possibility that delaying a blood patch may increase the risk of developing a subdural hematoma.”
Post–dural puncture headache is thought to be caused by decreased intracranial pressure attributable to the leakage of cerebrospinal fluid (CSF) through the dural disruption, which places traction on pain-sensitive structures. Treatment often involves a blood patch, which is the injection of autologous whole blood into the epidural space. As pregnant women frequently receive neuraxial anesthesia for childbirth, they may develop symptoms of a post–dural puncture headache after their hospital discharge.
Related Links:
McGill University
University of Toronto
Researchers at McGill University (Montreal, Canada) and the University of Toronto (UT; Canada) reviewed the outcomes of 22,130,815 patients and deliveries in the United States between January 2010 and December 2016 in order to determine the association of post–dural puncture headache with postpartum ISH. Patients were included if they had two months of follow-up data, and did not receive a diagnostic lumbar puncture. The main outcome was ISH in the two-month postpartum period, with secondary outcomes including in-hospital mortality and occurrence of neurosurgery.
In all, there were 68,374 post–dural puncture headaches, for an overall rate of 309 per 100,000. There were 342 cases of ISH identified, indicating an incidence rate of 1.5 per 100,000 women. Of these, 100 cases were in women with post–dural puncture headache, indicating a rate of 147 hematoma cases per 100,000 deliveries in this subgroup. After adjustment for maternal age, cesarean delivery, hypertension, preeclampsia, and other co-morbidities, post–dural puncture headache had an odds ratio for subdural hematoma of 199, and an adjusted absolute risk increase of 130 per 100,000 deliveries. The study was published on September 16, 2019, in JAMA Neurology.
“When a patient has a post-dural puncture headache, they are at risk for a subdural hematoma, which can result in serious morbidity and increased mortality, and needs to be considered by any clinician looking after these patients,” said lead author Albert Moore, MD, of McGill University. “The risk is higher in patients who have coagulopathy, previous cerebral arteriovenous malformations, and hypertensive disease, and there is also a possibility that delaying a blood patch may increase the risk of developing a subdural hematoma.”
Post–dural puncture headache is thought to be caused by decreased intracranial pressure attributable to the leakage of cerebrospinal fluid (CSF) through the dural disruption, which places traction on pain-sensitive structures. Treatment often involves a blood patch, which is the injection of autologous whole blood into the epidural space. As pregnant women frequently receive neuraxial anesthesia for childbirth, they may develop symptoms of a post–dural puncture headache after their hospital discharge.
Related Links:
McGill University
University of Toronto
Latest Critical Care News
- Eye Imaging AI Identifies Elevated Cardiovascular Risk
- Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
- Combined Infection Control Strategy Limits Drug-Resistant Outbreak in NICU
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreSurgical Techniques
view channel
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel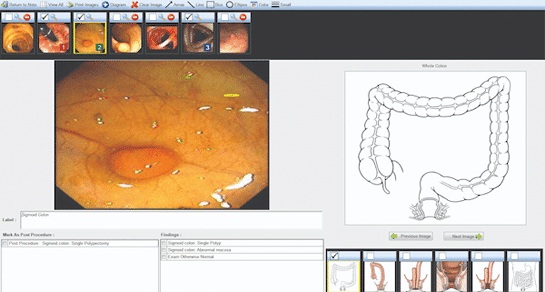
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel