Liquid Rhinoplasty Offers a Non-Surgical Cosmetic Alternative
|
By HospiMedica International staff writers Posted on 12 Mar 2020 |
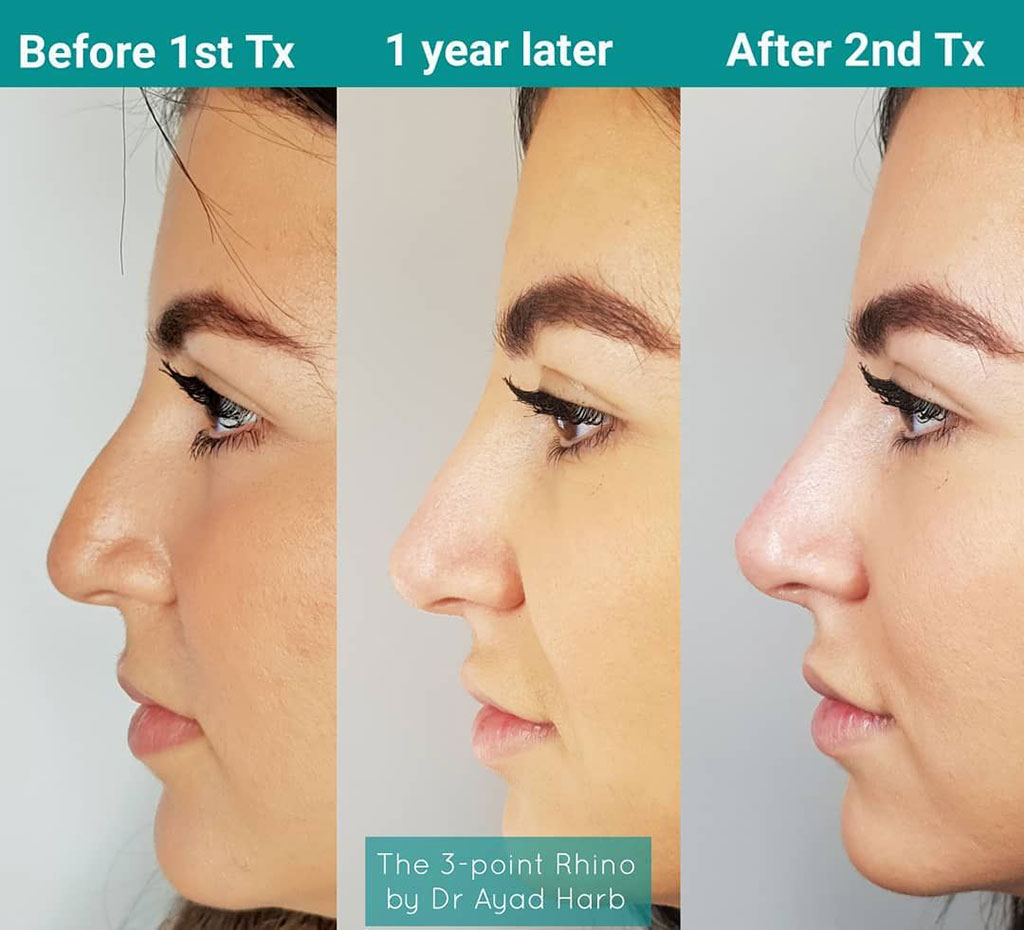
Image: An example of liquid rhinoplasty (Photo courtesy of Dr. Ayad Harb)
Nonsurgical rhinoplasty using dermal fillers is a safe procedure with positive aesthetic results when performed by an experienced clinician, claims a new study.
Ayad Harb, FRCSPlast, a consultant plastic surgeon and world authority on liquid rhinoplasty, and Colin Brewster, MRes, of Queen Elizabeth Hospital (Gateshead, United Kingdom), conducted a study of nonsurgical rhinoplasty in 5,000 patients (mean age 27 years, mostly female), who were treated between March 2016 and January 2019 by Dr. Harb. Study parameters included patient demographics, indications, treatment details, and outcomes. Average procedure time was 12 minutes, with the average filler injected about 0.72 mL.
The most common patient complaint was a dorsal hump (44%), with about 20% of patients seeking to refine the results after a previous rhinoplasty surgery. Liquid rhinoplasty was also used to treat other patient concerns, such as drooping nasal tip (15%), lack of definition (almost nine percent), frontal asymmetry (seven percent) and bulbous tip (six percent). Hyaluronic acid was the preferred filler due to its reversibility in the event of vascular occlusion. Another benefit is that it can be pre-mixed with local anesthetic, avoiding the need for pre-procedural local anesthetic, which can distort or mask subtle deformities.
The results showed that erythema and swelling were a common observation in the first five days, but generally settled with time; other complications were infrequent. A small number of patients (0.5%) showed signs of vascular occlusion; in most cases, blood flow was restored with simple measures. If not, a hyaluronidase enzyme injection was performed to immediately dissolve the dermal filler. The results lasted for 9-12 months, with approximately 32% returning at 12 months, most of whom were treated again. The study was published the March 2020 issue of Plastic and Reconstructive Surgery.
“The injections are carried out at the radix and move caudally with a micro-droplet technique of boluses of no more than 0.1 mL at any one point. Frequently, and especially nearer the tip, deposits of filler can be as small as 0.02 mL,” concluded Dr. Harb. “With each injection point, the gel implant is massaged into place and can be maneuverer to produce a smooth and symmetrical surface. The injections continue in the midline until the tip is reached; the tip is injected perpendicular to the skin to improve projection and definition.”
Nonsurgical rhinoplasty with injectable dermal fillers has become an increasingly popular alternative to surgical procedures, in view of its relative low cost, convenience and rapid recovery, and low risk profile. Although the procedure is not intended to replace surgical rhinoplasty, it has proven beneficial in discrete cases of inadequate tip projection, dorsal hump, and low radix. Nonsurgical rhinoplasty has also been used to improve functionality of the nose by splinting the nasal valves.
Related Links:
Queen Elizabeth Hospital
Ayad Harb, FRCSPlast, a consultant plastic surgeon and world authority on liquid rhinoplasty, and Colin Brewster, MRes, of Queen Elizabeth Hospital (Gateshead, United Kingdom), conducted a study of nonsurgical rhinoplasty in 5,000 patients (mean age 27 years, mostly female), who were treated between March 2016 and January 2019 by Dr. Harb. Study parameters included patient demographics, indications, treatment details, and outcomes. Average procedure time was 12 minutes, with the average filler injected about 0.72 mL.
The most common patient complaint was a dorsal hump (44%), with about 20% of patients seeking to refine the results after a previous rhinoplasty surgery. Liquid rhinoplasty was also used to treat other patient concerns, such as drooping nasal tip (15%), lack of definition (almost nine percent), frontal asymmetry (seven percent) and bulbous tip (six percent). Hyaluronic acid was the preferred filler due to its reversibility in the event of vascular occlusion. Another benefit is that it can be pre-mixed with local anesthetic, avoiding the need for pre-procedural local anesthetic, which can distort or mask subtle deformities.
The results showed that erythema and swelling were a common observation in the first five days, but generally settled with time; other complications were infrequent. A small number of patients (0.5%) showed signs of vascular occlusion; in most cases, blood flow was restored with simple measures. If not, a hyaluronidase enzyme injection was performed to immediately dissolve the dermal filler. The results lasted for 9-12 months, with approximately 32% returning at 12 months, most of whom were treated again. The study was published the March 2020 issue of Plastic and Reconstructive Surgery.
“The injections are carried out at the radix and move caudally with a micro-droplet technique of boluses of no more than 0.1 mL at any one point. Frequently, and especially nearer the tip, deposits of filler can be as small as 0.02 mL,” concluded Dr. Harb. “With each injection point, the gel implant is massaged into place and can be maneuverer to produce a smooth and symmetrical surface. The injections continue in the midline until the tip is reached; the tip is injected perpendicular to the skin to improve projection and definition.”
Nonsurgical rhinoplasty with injectable dermal fillers has become an increasingly popular alternative to surgical procedures, in view of its relative low cost, convenience and rapid recovery, and low risk profile. Although the procedure is not intended to replace surgical rhinoplasty, it has proven beneficial in discrete cases of inadequate tip projection, dorsal hump, and low radix. Nonsurgical rhinoplasty has also been used to improve functionality of the nose by splinting the nasal valves.
Related Links:
Queen Elizabeth Hospital
Latest Surgical Techniques News
- Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
- Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
- Ultrasound Technology Aims to Replace Invasive BPH Procedures
- Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
- New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
- Robot-Assisted Brain Angiography Improves Procedural Outcomes
- Brain Mapping Technology Enhances Precision in Brain Tumor Resection
- Handheld Robotic System Expands Options for Total Knee Surgery
- VR Experience Reduces Patient Anxiety Before Kidney Stone Procedure
- Injectable Mini Livers Offer Hope for Patients Awaiting Transplant
- Pulsed Field Ablation Technology Cleared in Europe for Persistent AFib
- AI-Powered Imaging Brings Real-Time Margin Clarity to Breast Cancer Surgery
- Minimally Invasive Device Safely Treats Challenging Brain Aneurysms
- Surgical Robot Makes Complex Liver Tumor Surgery Safer and Less Invasive
- Neurostimulation Implant Reduces Seizure Burden in Drug-Resistant Epilepsy
- Minimally Invasive Procedure Effectively Treats Small Kidney Cancers
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel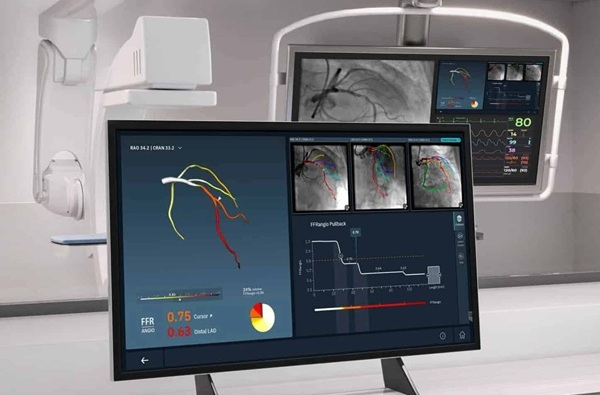
Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
Accurately determining whether a coronary stenosis limits blood flow is essential to guide percutaneous coronary intervention, yet wire-based physiologic testing remains underused due to added procedural... Read more
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel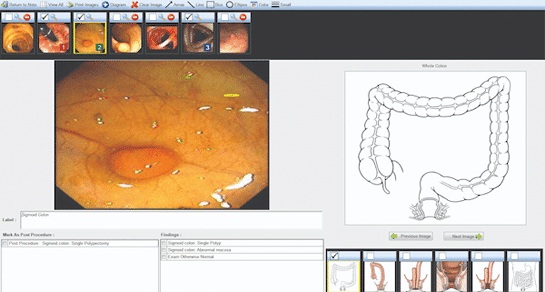
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel