AI Algorithm for Blood Sugar Management Reduces Risk of Serious Complications in Diabetic COVID-19 Patients
|
By HospiMedica International staff writers Posted on 14 Aug 2020 |

Illustration
Preliminary observations of COVID-19 patients with diabetes has inspired researchers from the University of Michigan (Ann Arbor, MI, USA) to develop an algorithm for glucose monitoring that could help combat the virus’ serious complications.
After preliminary observations of 200 COVID-19 patients with severe hyperglycemia, the Michigan Medicine team has discovered why high blood sugar may trigger worse outcomes in people infected with the virus. The researchers have also developed a blood sugar management tool that could potentially reduce the risk of secondary infections, kidney issues and intensive care stays in people with diabetes, prediabetes or obesity who get COVID-19.
According to the researchers, the low grade, inflammatory nature of diabetes and hyperglycemia promotes the virus’ inflammatory surge, resulting in insulin resistance and severe hyperglycemia. Specifically, these patients are at an increased risk for mechanical ventilation, kidney replacement therapy due to kidney failure and requiring medications known as vasopressors to stop dangerously low blood pressure or steroids to combat acute respiratory distress syndrome.
Based on their findings, the research team has developed a tool to identify and manage high blood sugar in COVID-19 patients, placing them into certain risk categories that looked at hyperglycemia severity, presence of obesity, level of insulin resistance, extent of kidney dysfunction and evidence of rapid changes in inflammatory markers. The newly created hyperglycemia management teams set out to find a way to monitor patients’ diabetes without having to use more personal protective equipment to visit the rooms all the time. It also aims to reduce the health care provider’s exposure to the virus as much as possible.
Although typically accurate, a continuous glucose monitor wouldn’t be as helpful because a patient’s low blood pressure and the use of blood pressure medications could falsely elevate blood sugar levels. The new protocol called for insulin delivery every six hours, and at the same time a nurse would check in on the patient. Some patients who were on ventilators or receiving high doses of Vitamin C would get their arterial or venous blood sugar levels checked, replacing the need for the team’s blood sugar check. For those with the highest blood sugar levels and severe hyperglycemia, insulin infusions were an option for patients until their levels fell between a normal range. The result of these efforts helped successfully lower blood sugar levels without increasing nurse contact or the overall burden on primary care teams and PPE usage.
“Improving blood sugar control was important in reducing the amount of secondary infections and kidney issues this cohort of patients are susceptible to,” said first author Roma Gianchandani, M.D., a professor of internal medicine in the Michigan Medicine division of metabolism, endocrinology and diabetes. “This might help shorten ICU stays and lessen the amount of patients that need a ventilator.”
Related Links:
University of Michigan
After preliminary observations of 200 COVID-19 patients with severe hyperglycemia, the Michigan Medicine team has discovered why high blood sugar may trigger worse outcomes in people infected with the virus. The researchers have also developed a blood sugar management tool that could potentially reduce the risk of secondary infections, kidney issues and intensive care stays in people with diabetes, prediabetes or obesity who get COVID-19.
According to the researchers, the low grade, inflammatory nature of diabetes and hyperglycemia promotes the virus’ inflammatory surge, resulting in insulin resistance and severe hyperglycemia. Specifically, these patients are at an increased risk for mechanical ventilation, kidney replacement therapy due to kidney failure and requiring medications known as vasopressors to stop dangerously low blood pressure or steroids to combat acute respiratory distress syndrome.
Based on their findings, the research team has developed a tool to identify and manage high blood sugar in COVID-19 patients, placing them into certain risk categories that looked at hyperglycemia severity, presence of obesity, level of insulin resistance, extent of kidney dysfunction and evidence of rapid changes in inflammatory markers. The newly created hyperglycemia management teams set out to find a way to monitor patients’ diabetes without having to use more personal protective equipment to visit the rooms all the time. It also aims to reduce the health care provider’s exposure to the virus as much as possible.
Although typically accurate, a continuous glucose monitor wouldn’t be as helpful because a patient’s low blood pressure and the use of blood pressure medications could falsely elevate blood sugar levels. The new protocol called for insulin delivery every six hours, and at the same time a nurse would check in on the patient. Some patients who were on ventilators or receiving high doses of Vitamin C would get their arterial or venous blood sugar levels checked, replacing the need for the team’s blood sugar check. For those with the highest blood sugar levels and severe hyperglycemia, insulin infusions were an option for patients until their levels fell between a normal range. The result of these efforts helped successfully lower blood sugar levels without increasing nurse contact or the overall burden on primary care teams and PPE usage.
“Improving blood sugar control was important in reducing the amount of secondary infections and kidney issues this cohort of patients are susceptible to,” said first author Roma Gianchandani, M.D., a professor of internal medicine in the Michigan Medicine division of metabolism, endocrinology and diabetes. “This might help shorten ICU stays and lessen the amount of patients that need a ventilator.”
Related Links:
University of Michigan
Latest AI News
- AI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
- Machine Learning Approach Enhances Liver Cancer Risk Stratification
- New AI Approach Monitors Brain Health Using Passive Wearable Data
- AI Tool Maps Early Risk Patterns in Bloodstream Infections
- AI Model Identifies Rare Endocrine Disorder from Hand Images
- AI Tool Promises to Reduce Length of Hospital Stays and Free Up Beds
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel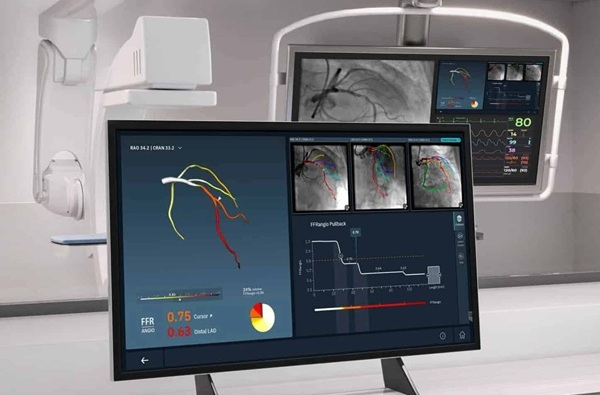
Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
Accurately determining whether a coronary stenosis limits blood flow is essential to guide percutaneous coronary intervention, yet wire-based physiologic testing remains underused due to added procedural... Read more
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read moreSurgical Techniques
view channel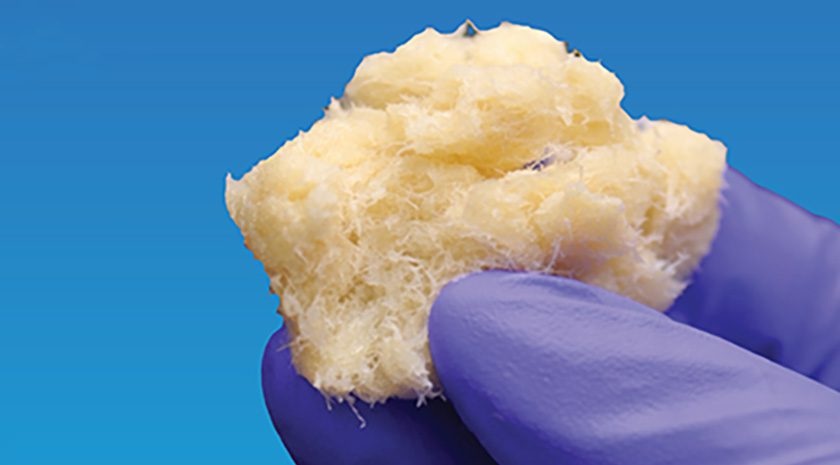
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more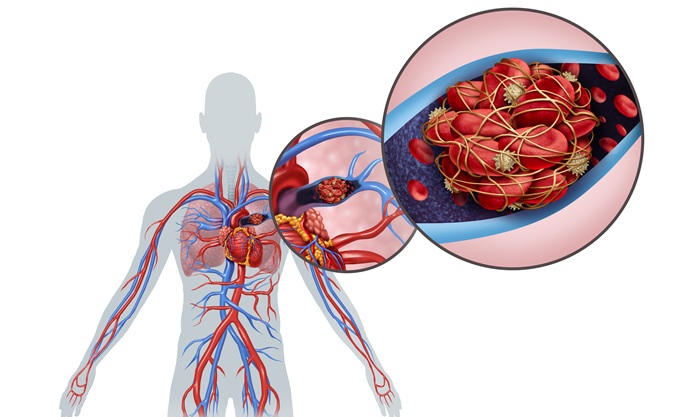
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel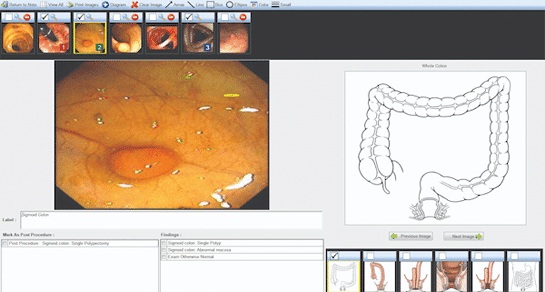
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel





















