Siemens Collaborates with CDC to Develop Process for Standardizing SARS-CoV-2 Assays
|
By HospiMedica International staff writers Posted on 16 Sep 2020 |
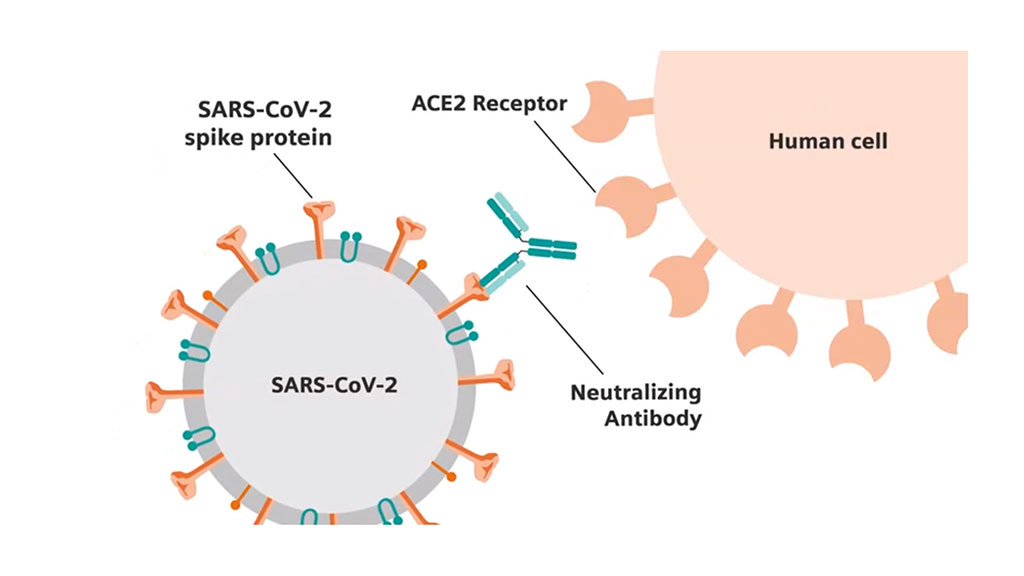
Image: Siemens’ collaboration with the CDC and the JRC will develop a novel process for standardizing SARS-CoV-2 assays by anchoring each protein to a neutralization antibody titer - a level of antibody present to block virus from entering cells in laboratory experiments (Photo courtesy of Siemens Healthineers)
Siemens Healthineers (Erlangen, Germany) has entered into a collaboration with the US Centers for Disease Control and Prevention (CDC Atlanta, GA, USA) and the JRC (Joint Research Centre) of the European Commission on a research project to develop a novel process for standardizing SARS-CoV-2 assays.
Antibody tests differ among test manufacturers and currently cannot be analytically compared because they target different SARS-CoV-2 proteins. These include the spike protein, S1/S2, S1 RBD, and N protein, which are found in different parts of the SARS-CoV-2 virus. As the pandemic has evolved, antibody test results have progressed from qualitative positive/negative results to more recent assays capable of numerical measurements that gauge the level of IgG antibodies in a patient’s blood sample. The reportable numerical patient results of the current semi-quantitative assays are expressed in units that are not actual concentrations of antibodies, but rather the antibody activity to the virus. Because comparing test results across manufacturers has not been possible, establishing immunity associated with these tests has been challenging.
Siemens’ collaboration with the CDC and the JRC will develop a novel process for standardizing SARS-CoV-2 assays by anchoring each protein to a neutralization antibody titer - a level of antibody present to block virus from entering cells in laboratory experiments. The thresholds displayed in the standardized unit of measure for IgG - arising either from natural infection or vaccination - may likely contribute to a standardized interpretation of immunity through test results. Developing a standardized process will define which concentration confers neutralization for different manufacturers’ antigen targets. Each manufacturer currently standardizes their assays independently with internal standards that are not linked to a common reference. The results of this collaborative research project will support the JRC's production of a reference material. This reference material with assigned concentrations of antibody specific to each viral protein will allow manufacturers to refer to standardized values.
With an international standard established and adopted by manufacturers, clinicians would be positioned to track their patients' antibody concentrations, regardless of the test method or manufacturer used. This capability is expected to improve patient care by enabling long-term antibody level comparison - clinical information that is important for verifying natural immunity acquired by patient’s infection with the virus, as well as for determining the effectiveness of vaccines.
"One barrier to antibody test adoption is we don't currently have an established process to determine immunity," said Deepak Nath, PhD, President of Laboratory Diagnostics, Siemens Healthineers. "Different SARS-CoV-2 antibody targets produce different levels of neutralization. Our R&D team recognized that if you could define a level at which neutralization is conferred for different targets, you could create a common ground to standardize assays—not just on antibody production, but their ability to provide immunity. Our collaboration with the CDC and JRC will develop the framework that all antibody test manufacturers would be expected to adopt moving forward for greater benefit to patient care as the pandemic evolves."
Antibody tests differ among test manufacturers and currently cannot be analytically compared because they target different SARS-CoV-2 proteins. These include the spike protein, S1/S2, S1 RBD, and N protein, which are found in different parts of the SARS-CoV-2 virus. As the pandemic has evolved, antibody test results have progressed from qualitative positive/negative results to more recent assays capable of numerical measurements that gauge the level of IgG antibodies in a patient’s blood sample. The reportable numerical patient results of the current semi-quantitative assays are expressed in units that are not actual concentrations of antibodies, but rather the antibody activity to the virus. Because comparing test results across manufacturers has not been possible, establishing immunity associated with these tests has been challenging.
Siemens’ collaboration with the CDC and the JRC will develop a novel process for standardizing SARS-CoV-2 assays by anchoring each protein to a neutralization antibody titer - a level of antibody present to block virus from entering cells in laboratory experiments. The thresholds displayed in the standardized unit of measure for IgG - arising either from natural infection or vaccination - may likely contribute to a standardized interpretation of immunity through test results. Developing a standardized process will define which concentration confers neutralization for different manufacturers’ antigen targets. Each manufacturer currently standardizes their assays independently with internal standards that are not linked to a common reference. The results of this collaborative research project will support the JRC's production of a reference material. This reference material with assigned concentrations of antibody specific to each viral protein will allow manufacturers to refer to standardized values.
With an international standard established and adopted by manufacturers, clinicians would be positioned to track their patients' antibody concentrations, regardless of the test method or manufacturer used. This capability is expected to improve patient care by enabling long-term antibody level comparison - clinical information that is important for verifying natural immunity acquired by patient’s infection with the virus, as well as for determining the effectiveness of vaccines.
"One barrier to antibody test adoption is we don't currently have an established process to determine immunity," said Deepak Nath, PhD, President of Laboratory Diagnostics, Siemens Healthineers. "Different SARS-CoV-2 antibody targets produce different levels of neutralization. Our R&D team recognized that if you could define a level at which neutralization is conferred for different targets, you could create a common ground to standardize assays—not just on antibody production, but their ability to provide immunity. Our collaboration with the CDC and JRC will develop the framework that all antibody test manufacturers would be expected to adopt moving forward for greater benefit to patient care as the pandemic evolves."
Latest COVID-19 News
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read more
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read moreSurgical Techniques
view channel
Ultrasound Technology Aims to Replace Invasive BPH Procedures
Benign prostatic hyperplasia (BPH) is a frequent cause of lower urinary tract symptoms in aging men and often requires invasive procedures or prolonged recovery. With prevalence expected to rise as populations... Read more
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel
























