New AI Algorithm Crunches Massive Amounts of Real-World Data to Find New Uses for Existing Medications
|
By HospiMedica International staff writers Posted on 12 Jan 2021 |
Illustration
Scientists have developed a machine-learning method that crunches massive amounts of data to help determine which existing medications could improve outcomes in diseases for which they are not prescribed.
The aim of this work by researchers at The Ohio State University (Columbus, OH, USA) is to speed up drug repurposing. In order to deem that a drug effective for one disorder will be useful as a treatment for something else, scientists need to conduct time-consuming and expensive randomized clinical trials. Drug repurposing is an attractive pursuit because it could lower the risk associated with safety testing of new medications and dramatically reduce the time it takes to get a drug into the marketplace for clinical use.
Randomized clinical trials are the gold standard for determining a drug’s effectiveness against a disease, although machine learning can account for hundreds – or thousands – of human differences within a large population that could influence how medicine works in the body. These factors, or confounders, ranging from age, sex and race to disease severity and the presence of other illnesses, function as parameters in the deep learning computer algorithm on which the framework is based. That information comes from “real-world evidence,” which is longitudinal observational data about millions of patients captured by electronic medical records or insurance claims and prescription data.
The Ohio State University researchers created a framework that combines enormous patient care-related datasets with high-powered computation to arrive at repurposed drug candidates and the estimated effects of those existing medications on a defined set of outcomes. The research team used insurance claims data on nearly 1.2 million heart-disease patients, which provided information on their assigned treatment, disease outcomes and various values for potential confounders. The deep learning algorithm also has the power to take into account the passage of time in each patient’s experience – for every visit, prescription and diagnostic test. The model input for drugs is based on their active ingredients.
Applying what is called causal inference theory, the researchers categorized, for the purposes of this analysis, the active drug and placebo patient groups that would be found in a clinical trial. The model tracked patients for two years – and compared their disease status at that end point to whether or not they took medications, which drugs they took and when they started the regimen.
Their hypothesis: that the model would identify drugs that could lower the risk for heart failure and stroke in coronary artery disease patients. The model yielded nine drugs considered likely to provide those therapeutic benefits, three of which are currently in use – meaning the analysis identified six candidates for drug repurposing. Among other findings, the analysis suggested that a diabetes medication, metformin, and escitalopram, used to treat depression and anxiety, could lower risk for heart failure and stroke in the model patient population. As it turns out, both of those drugs are currently being tested for their effectiveness against heart disease.
“This work shows how artificial intelligence can be used to ‘test’ a drug on a patient, and speed up hypothesis generation and potentially speed up a clinical trial,” said senior author Ping Zhang, assistant professor of computer science and engineering and biomedical informatics at Ohio State. “But we will never replace the physician – drug decisions will always be made by clinicians.”
Related Links:
The Ohio State University
The aim of this work by researchers at The Ohio State University (Columbus, OH, USA) is to speed up drug repurposing. In order to deem that a drug effective for one disorder will be useful as a treatment for something else, scientists need to conduct time-consuming and expensive randomized clinical trials. Drug repurposing is an attractive pursuit because it could lower the risk associated with safety testing of new medications and dramatically reduce the time it takes to get a drug into the marketplace for clinical use.
Randomized clinical trials are the gold standard for determining a drug’s effectiveness against a disease, although machine learning can account for hundreds – or thousands – of human differences within a large population that could influence how medicine works in the body. These factors, or confounders, ranging from age, sex and race to disease severity and the presence of other illnesses, function as parameters in the deep learning computer algorithm on which the framework is based. That information comes from “real-world evidence,” which is longitudinal observational data about millions of patients captured by electronic medical records or insurance claims and prescription data.
The Ohio State University researchers created a framework that combines enormous patient care-related datasets with high-powered computation to arrive at repurposed drug candidates and the estimated effects of those existing medications on a defined set of outcomes. The research team used insurance claims data on nearly 1.2 million heart-disease patients, which provided information on their assigned treatment, disease outcomes and various values for potential confounders. The deep learning algorithm also has the power to take into account the passage of time in each patient’s experience – for every visit, prescription and diagnostic test. The model input for drugs is based on their active ingredients.
Applying what is called causal inference theory, the researchers categorized, for the purposes of this analysis, the active drug and placebo patient groups that would be found in a clinical trial. The model tracked patients for two years – and compared their disease status at that end point to whether or not they took medications, which drugs they took and when they started the regimen.
Their hypothesis: that the model would identify drugs that could lower the risk for heart failure and stroke in coronary artery disease patients. The model yielded nine drugs considered likely to provide those therapeutic benefits, three of which are currently in use – meaning the analysis identified six candidates for drug repurposing. Among other findings, the analysis suggested that a diabetes medication, metformin, and escitalopram, used to treat depression and anxiety, could lower risk for heart failure and stroke in the model patient population. As it turns out, both of those drugs are currently being tested for their effectiveness against heart disease.
“This work shows how artificial intelligence can be used to ‘test’ a drug on a patient, and speed up hypothesis generation and potentially speed up a clinical trial,” said senior author Ping Zhang, assistant professor of computer science and engineering and biomedical informatics at Ohio State. “But we will never replace the physician – drug decisions will always be made by clinicians.”
Related Links:
The Ohio State University
Latest Business News
- GE HealthCare Leads Major European Initiative to Advance Cardio-Oncology Care
- Medtronic and GE HealthCare Broaden Alliance Across Monitoring and Care Solutions
- Quantum Surgical Acquires NeuWave from Johnson & Johnson
- Medtronic to Acquire Coronary Artery Medtech Company CathWorks
- Medtronic and Mindray Expand Strategic Partnership to Ambulatory Surgery Centers in the U.S.
- FDA Clearance Expands Robotic Options for Minimally Invasive Heart Surgery
- WHX in Dubai (formerly Arab Health) to debut specialised Biotech & Life Sciences Zone as sector growth accelerates globally
- WHX in Dubai (formerly Arab Health) to bring together key UAE government entities during the groundbreaking 2026 edition
- Interoperability Push Fuels Surge in Healthcare IT Market
- Philips and Masimo Partner to Advance Patient Monitoring Measurement Technologies
- B. Braun Acquires Digital Microsurgery Company True Digital Surgery
- CMEF 2025 to Promote Holistic and High-Quality Development of Medical and Health Industry
- Bayer and Broad Institute Extend Research Collaboration to Develop New Cardiovascular Therapies
- Medtronic Partners with Corsano to Expand Acute Care & Monitoring Portfolio in Europe
- Expanded Collaboration to Transform OR Technology Through AI and Automation
- Becton Dickinson to Spin Out Biosciences and Diagnostic Solutions Business
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
Accurately determining whether a coronary stenosis limits blood flow is essential to guide percutaneous coronary intervention, yet wire-based physiologic testing remains underused due to added procedural... Read more
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read moreSurgical Techniques
view channel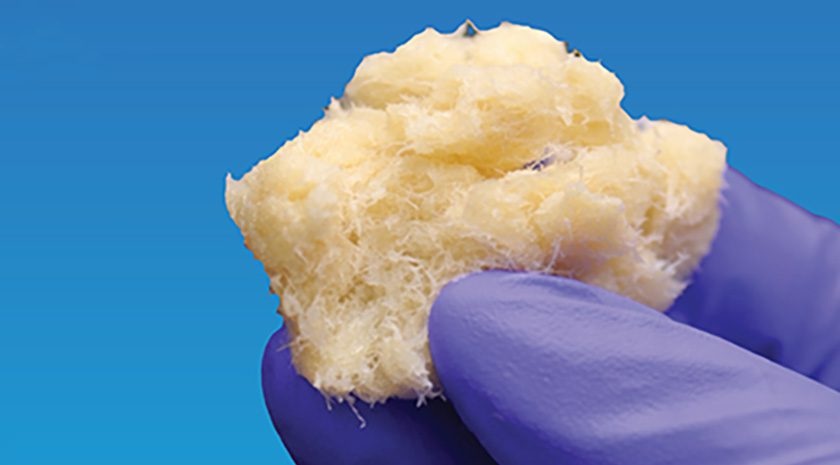
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel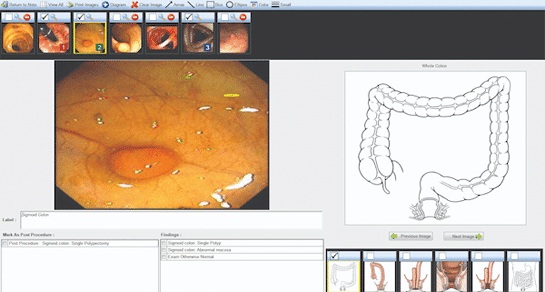
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more