New Self-Learning AI-Based Algorithm Reads Electrocardiograms to Spot Unseen Signs of Heart Failure
|
By HospiMedica International staff writers Posted on 20 Oct 2021 |
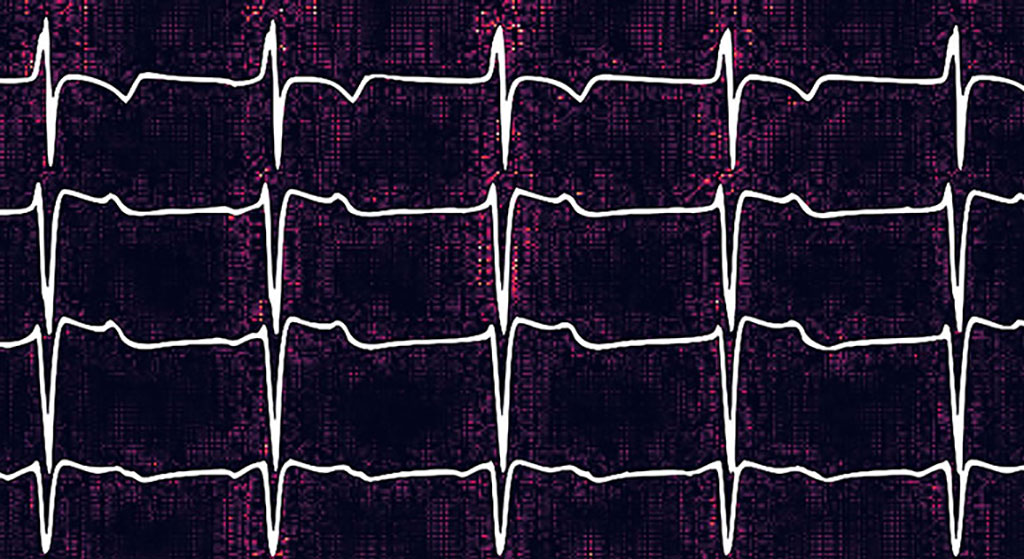
A new self-learning algorithm can detect blood pumping problems by reading electrocardiograms (also known as ECGs or EKGs) to predict whether a patient was experiencing heart failure.
The special artificial intelligence (AI)-based computer algorithm created by researchers at Mount Sinai (New York, NY, USA) was able to learn how to identify subtle changes in electrocardiograms (also known as ECGs or EKGs) to predict whether a patient was experiencing heart failure. Heart failure, or congestive heart failure, occurs when the heart pumps less blood than the body normally needs. For years, doctors have relied heavily on an imaging technique called an echocardiogram to assess whether a patient may be experiencing heart failure. While helpful, echocardiograms can be labor-intensive procedures that are only offered at select hospitals.
However, recent breakthroughs in AI suggest that electrocardiograms - a widely used electrical recording device - could be a fast and readily available alternative in these cases. For instance, many studies have shown how a “deep-learning” algorithm can detect weakness in the heart’s left ventricle, which pushes freshly oxygenated blood out to the rest of the body. In this study, the researchers described the development of an algorithm that not only assessed the strength of the left ventricle but also the right ventricle, which takes deoxygenated blood streaming in from the body and pumps it to the lungs.
Typically, an electrocardiogram involves a two-step process. Wire leads are taped to different parts of a patient’s chest and within minutes a specially designed, portable machine prints out a series of squiggly lines, or waveforms, representing the heart’s electrical activity. These machines can be found in most hospitals and ambulances and require minimal training to operate. For this study, the researchers programmed a computer to read patient electrocardiograms along with data extracted from written reports summarizing the results of corresponding echocardiograms taken from the same patients. In this situation, the written reports acted as a standard set of data for the computer to compare with the electrocardiogram data and learn how to spot weaker hearts.
Natural language processing programs helped the computer extract data from the written reports. Meanwhile, special neural networks capable of discovering patterns in images were incorporated to help the algorithm learn to recognize pumping strengths. The computer then read more than 700,000 electrocardiograms and echocardiogram reports obtained from 150,000 Mount Sinai Health System patients from 2003 to 2020. Data from four hospitals was used to train the computer, whereas data from a fifth one was used to test how the algorithm would perform in a different experimental setting. Initial results suggested that the algorithm was effective at predicting which patients would have either healthy or very weak left ventricles. Here strength was defined by left ventricle ejection fraction, an estimate of how much fluid the ventricle pumps out with each beat as observed on echocardiograms. Healthy hearts have an ejection fraction of 50% or greater while weak hearts have ones that are equal to or below 40%.
The algorithm was 94% accurate at predicting which patients had a healthy ejection fraction and 87% accurate at predicting those who had an ejection fraction that was below 40%. However the algorithm was not as effective at predicting which patients would have slightly weakened hearts. In this case, the program was 73% accurate at predicting the patients who had an ejection fraction that was between 40% and 50%. Further results suggested that the algorithm also learned to detect right valve weaknesses from the electrocardiograms. In this case, weakness was defined by more descriptive terms extracted from the echocardiogram reports. Here the algorithm was 84% accurate at predicting which patients had weak right valves. Finally, additional analysis suggested that the algorithm may be effective at detecting heart weakness in all patients, regardless of race and gender.
“We showed that deep-learning algorithms can recognize blood pumping problems on both sides of the heart from ECG waveform data,” said Benjamin S. Glicksberg, PhD, Assistant Professor of Genetics and Genomic Sciences, a member of the Hasso Plattner Institute for Digital Health at Mount Sinai, and a senior author of the study published in the Journal of the American College of Cardiology: Cardiovascular Imaging. “Ordinarily, diagnosing these type of heart conditions requires expensive and time-consuming procedures. We hope that this algorithm will enable quicker diagnosis of heart failure.”
“This study represents an exciting step forward in finding information hidden within the ECG data which can lead to better screening and treatment paradigms using a relatively simple and widely available test,” said Girish N. Nadkarni, MD, MPH, CPH, Associate Professor of Medicine at the Icahn School of Medicine at Mount Sinai, Chief of the Division of Data-Driven and Digital Medicine (D3M), and a senior author of the study. “A potential advantage of this study is that it involved one of the largest collections of ECGs from one of the most diverse patient populations in the world.”
Related Links:
Mount Sinai
Latest Health IT News
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
- Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
- Smartwatches Could Detect Congestive Heart Failure
- Versatile Smart Patch Combines Health Monitoring and Drug Delivery
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read more
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read moreSurgical Techniques
view channel
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreBusiness
view channel





















