Replacement Valve That Grow Inside the Body to Revolutionize Heart Treatment
|
By HospiMedica International staff writers Posted on 01 Feb 2024 |

Heart valve replacement surgery, a life-saving procedure, has been available for over six decades. However, it comes with significant medical limitations, whether the valves used are mechanical or biological. Patients with mechanical heart valves need lifelong medication to prevent blood clotting. Biological valves, in contrast, have a lifespan of only 10 to 15 years. The situation is even more complex for children with congenital heart defects, as their growing bodies necessitate multiple valve replacements before they reach adulthood. Now, recent research suggests that the natural repair mechanisms in humans can be leveraged to build a living heart valve that grows inside the body along with the patient.
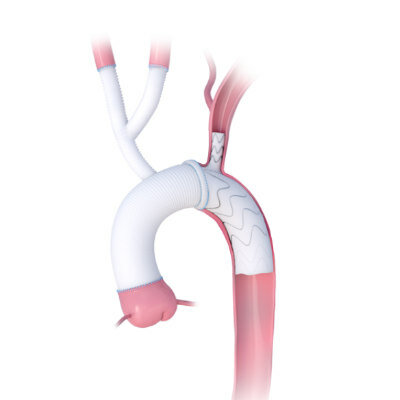
The new approach developed by researchers at Imperial College London (London, UK) involves a procedure that begins with a nanofibrous polymeric valve created from a biodegradable polymer scaffold, unlike the durable plastic that is typically used. Once implanted, this scaffold recruits cells and guides their development, turning the body into a bioreactor for new tissue growth. Over time, the scaffold is naturally replaced by the body's own tissues. At the heart of this innovation is the scaffold material, designed to attract, house, and direct the patient's cells, thereby encouraging tissue growth while preserving valve functionality.
The research team conducted laboratory validation studies and reported the initial results from animal tests. The valves, transplanted into sheep, were observed for up to six months. They functioned effectively throughout this period and demonstrated promising cellular regeneration. Notably, the study highlighted the scaffold's ability to attract blood cells that transform into functional tissues through a process known as endothelial-to-mesenchymal transformation (EndMT). Additionally, nerve and fatty tissue growth within the scaffold was observed, mirroring what one would expect in a normal valve. Concurrently, the polymer scaffold underwent degradation, paving the way for new tissue growth. This degradation was monitored using gel permeability chromatography (GPC) at the Agilent Measurement Suite (AMS) in Imperial’s Molecular Sciences Research Hub in White City, which is equipped with sophisticated analytical tools.
Further research is needed to fully understand the mechanisms behind the polymer's degradation and its correlation with tissue regeneration. The next phase involves extending animal studies to monitor tissue regeneration over longer periods. This data will be vital for obtaining regulatory approval for the first human clinical trials, expected within the next five years. Additionally, refining the manufacturing processes of the valves is necessary. As the project progresses, the team plans to seek commercial partners for later-stage clinical trials. Although currently focused on heart valve replacement, this technology has potential applications in other areas, such as treating vascular conditions, repairing blood vessels damaged by dialysis, and creating cardiac patches for heart repair.
“The aim of the concept we’ve developed is to produce a living valve in the body, which would be able to grow with the patient,” said Dr. Yuan-Tsan Tseng, a biomaterials scientist. “Once you have the scaffold, it becomes a platform technology that you can use to engineer other tissues.”
Related Links:
Imperial College London
Latest Surgical Techniques News
- Noninvasive Cardiac Radiotherapy Reduces Ventricular Tachycardia Events
- Augmented Reality System for Knee Replacement Receives FDA Clearance
- New AI Tool Predicts Complications Before Lung Cancer Surgery
- First Automated Insulin Delivery System Cleared for Type 1 Diabetes in Pregnancy
- Novel Ablation Technology Reduces Ventricular Tachycardia Recurrence
- Dual-Energy Ablation and Conduction System Pacing Show Positive Early Outcomes
- Less Invasive Microcurrent Cardiac Device Improves Heart Failure Outcomes
- Partial Heart Transplantation Enables Growing Valve Replacement for Children
- Torqueable Microcatheters Enhance Navigation in Complex Coronary Lesions
- Early “Heart Training” Surgery Promotes Regeneration in Pediatric Heart Failure
- Transcatheter Venous Arterialization Improves Outcomes in No-Option Limb Ischemia Patients
- CE-Marked Stapler Designed to Improve Staple Line Integrity
- Smart Fracture Implant Monitors Healing and Delivers Adaptive Support
- Pulsed Field Ablation Technology Showcases One-Year AF Outcomes
- Novel GERD Device Demonstrates Long-Term Safety in Real-World Study
- Flexible Graphene Cortical Interface Enables Real-Time Mapping During Tumor Surgery
Channels
Artificial Intelligence
view channel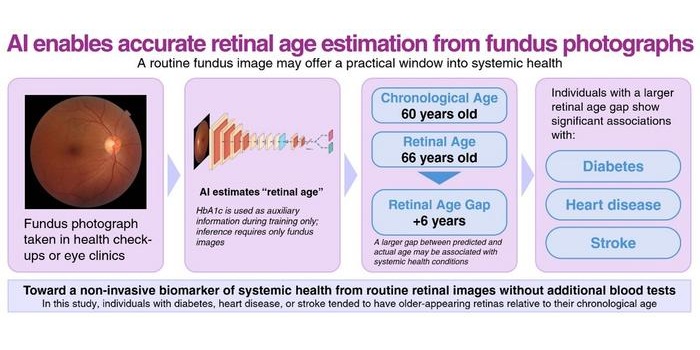
AI Model Uses Eye Imaging to Identify Risk of Major Systemic Diseases
Early detection of systemic disease risk remains a persistent challenge in population health screening. Cardiometabolic conditions such as diabetes, heart disease, and stroke often progress without symptoms... Read more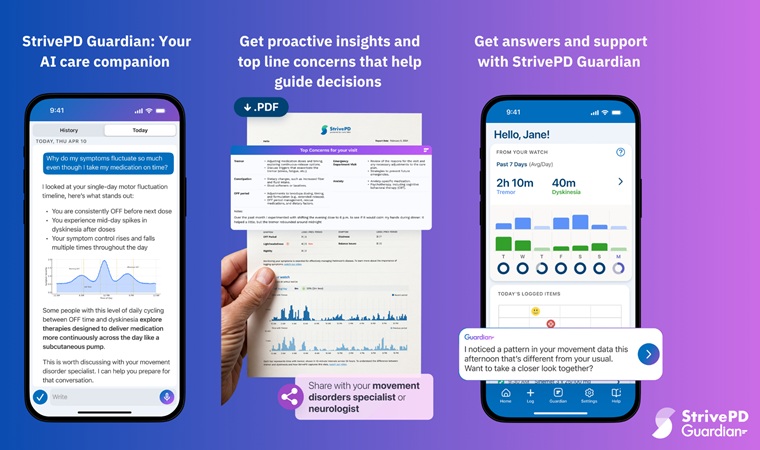
AI Platform Interprets Real-Time Wearable Data for Parkinson’s Management
Parkinson’s disease presents fluctuating motor and non-motor symptoms that complicate day-to-day self-management and clinical decision-making. Care teams require timely, longitudinal insight into medication... Read moreCritical Care
view channel
Blood-Filtering Device May Prolong Pregnancy in Severe Early Preeclampsia
Preeclampsia is a hypertensive disorder of pregnancy that can progress rapidly and threaten the lives of both mother and fetus. In its severe early form, often before 34 weeks’ gestation, clinicians frequently... Read more
AI Tool Predicts In-Hospital Cardiac Arrest Minutes in Advance
Sudden cardiac arrest, the abrupt loss of heart function, often arises without clear warning in hospitalized patients. Clinicians must sift through faint signals from routine monitoring while limiting... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channelBusiness
view channel
Johnson & Johnson Launches AI-Driven Cardiac Mapping System
Johnson & Johnson has introduced the CARTOSOUND SONATA Module for the CARTO System at the Heart Rhythm Society (HRS) 2026 meeting in Chicago. The module uses artificial intelligence with the CARTO... Read more