Autofluorescent Bandage Detects Pathogenic Bacteria 
|
By HospiMedica International staff writers Posted on 04 Apr 2016 |
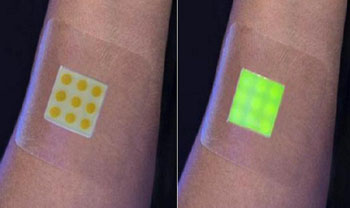
Image: The prototype of the ‘smart’ wound dressing: not infected (L), infected (R) (Photo courtesy of the University of Bath).
An intelligent hydrogel wound dressing glows green when it detects the presence of harmful bacteria in wound biofilms, potentially reducing the use of antibiotics.
Developed by researchers at the University of Bath (United Kingdom), the University of Brighton (United Kingdom), and other institutions, the prototype wound dressing combines tiny vesicles containing a fluorescent dye mixed with agarose, which are then dispersed within a hydrogel matrix. When toxic bacteria come in contact with the vesicles within the hydrated agarose film, a reaction occurs that releases a dye that fluoresces, alerting attending healthcare professionals that the wound is infected.
The researchers tested the dressing in both static and dynamic models of wound biofilms, using clinical strains of Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, and Enterococcus faecalis, which were used to establish a biofilm on a nanoporous polycarbonate membrane for periods of 24, 48, and 72 hours. The results indicated a clear fluorescent response within four hours, which was only observed when in contact with biofilms produced by a pathogenic strain. Similar responses were demonstrated on an ex-vivo porcine skin model of burn wound infection.
The sensitivity of the dressing to biofilms was dependent on the species and strain types of the bacterial pathogens involved, but a relatively higher response was observed in strains considered good biofilm formers. The researchers also found a clear difference in the levels of response when the dressings were tested on bacteria grown in biofilm or in planktonic cultures, suggesting that the level of expression of virulence factors is different depending of the growth mode. The study describing to prototype dressing was published in the February 2016 issue of ACS Applied Materials & Interfaces.
“The nanocapsules mimic skin cells in that they only break open when toxic bacteria are present; they aren’t affected by the harmless bacteria that normally live on healthy skin,” said senior author biophysical chemist Toby Jenkins, PhD, of the University of Brighton. “Using this dressing will allow clinicians to quickly identify infections without removing it, meaning that patients can be diagnosed and treated faster. It could really help to save lives.”
Related Links:
University of Bath
University of Brighton
Developed by researchers at the University of Bath (United Kingdom), the University of Brighton (United Kingdom), and other institutions, the prototype wound dressing combines tiny vesicles containing a fluorescent dye mixed with agarose, which are then dispersed within a hydrogel matrix. When toxic bacteria come in contact with the vesicles within the hydrated agarose film, a reaction occurs that releases a dye that fluoresces, alerting attending healthcare professionals that the wound is infected.
The researchers tested the dressing in both static and dynamic models of wound biofilms, using clinical strains of Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, and Enterococcus faecalis, which were used to establish a biofilm on a nanoporous polycarbonate membrane for periods of 24, 48, and 72 hours. The results indicated a clear fluorescent response within four hours, which was only observed when in contact with biofilms produced by a pathogenic strain. Similar responses were demonstrated on an ex-vivo porcine skin model of burn wound infection.
The sensitivity of the dressing to biofilms was dependent on the species and strain types of the bacterial pathogens involved, but a relatively higher response was observed in strains considered good biofilm formers. The researchers also found a clear difference in the levels of response when the dressings were tested on bacteria grown in biofilm or in planktonic cultures, suggesting that the level of expression of virulence factors is different depending of the growth mode. The study describing to prototype dressing was published in the February 2016 issue of ACS Applied Materials & Interfaces.
“The nanocapsules mimic skin cells in that they only break open when toxic bacteria are present; they aren’t affected by the harmless bacteria that normally live on healthy skin,” said senior author biophysical chemist Toby Jenkins, PhD, of the University of Brighton. “Using this dressing will allow clinicians to quickly identify infections without removing it, meaning that patients can be diagnosed and treated faster. It could really help to save lives.”
Related Links:
University of Bath
University of Brighton
Latest Critical Care News
- Novel Cannula Delivery System Enables Targeted Delivery of Imaging Agents and Drugs
- Ingestible Smart Capsule for Chemical Sensing in the Gut Moves Closer to Market
- Novel Intrabronchial Method Delivers Cell Therapies in Critically Ill Patients on External Lung Support
- Generative AI Technology Detects Heart Disease Earlier Than Conventional Methods
- Wearable Technology Predicts Cardiovascular Risk by Continuously Monitoring Heart Rate Recovery
- Wearable Health Monitoring Device Measures Gases Emitted from and Absorbed by Skin
- Groundbreaking Technology Rapidly Detects Airborne Influenza Viruses
- Handheld Device Could Transform Heart Disease Screening
- Flexible Semi-Autonomous Robot Could Deliver Medicine Inside Body

- Neurorestorative Treatment Strategies Hold Promise for Most Severe Forms of Epilepsy
- Gene Discovery Could Help Grow New Heart Arteries
- Study Discovers Invisible Transmission of Common Hospital-Associated Infection
- Non-Invasive Neuro-Ophthalmology Techniques Could Detect Brain Tumors Earlier
- Mass Manufactured Nanoparticles to Deliver Cancer Drugs Directly to Tumors
- World’s Smallest Pacemaker Fits Inside Syringe Tip

- AI-Powered, Internet-Connected Medical Devices to Revolutionize Healthcare, Finds Study
Channels
Surgical Techniques
view channel
Pioneering Sutureless Coronary Bypass Technology to Eliminate Open-Chest Procedures
In patients with coronary artery disease, certain blood vessels may be narrowed or blocked, requiring a stent or a bypass (also known as diversion) to restore blood flow to the heart. Bypass surgeries... Read more
Intravascular Imaging for Guiding Stent Implantation Ensures Safer Stenting Procedures
Patients diagnosed with coronary artery disease, which is caused by plaque accumulation within the arteries leading to chest pain, shortness of breath, and potential heart attacks, frequently undergo percutaneous... Read more
World's First AI Surgical Guidance Platform Allows Surgeons to Measure Success in Real-Time
Surgeons have always faced challenges in measuring their progress toward surgical goals during procedures. Traditionally, obtaining measurements required stepping out of the sterile environment to perform... Read morePatient Care
view channel
Portable Biosensor Platform to Reduce Hospital-Acquired Infections
Approximately 4 million patients in the European Union acquire healthcare-associated infections (HAIs) or nosocomial infections each year, with around 37,000 deaths directly resulting from these infections,... Read moreFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read moreHealth IT
view channel
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read more
Smartwatches Could Detect Congestive Heart Failure
Diagnosing congestive heart failure (CHF) typically requires expensive and time-consuming imaging techniques like echocardiography, also known as cardiac ultrasound. Previously, detecting CHF by analyzing... Read moreBusiness
view channel
Expanded Collaboration to Transform OR Technology Through AI and Automation
The expansion of an existing collaboration between three leading companies aims to develop artificial intelligence (AI)-driven solutions for smart operating rooms with sophisticated monitoring and automation.... Read more