Vagus Nerve Stimulation Accelerates Stroke Recovery
|
By HospiMedica International staff writers Posted on 12 Apr 2018 |
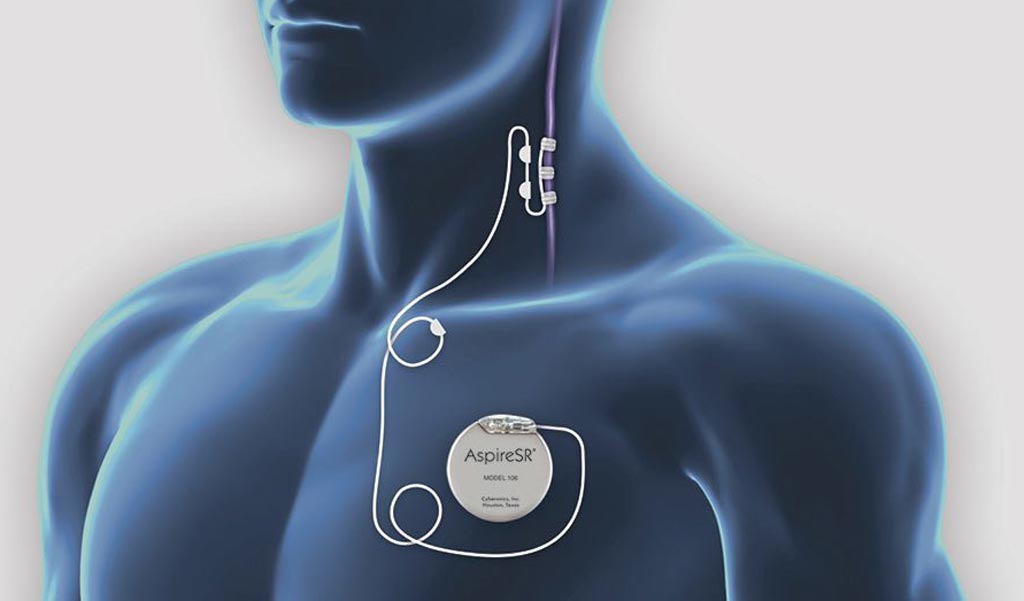
Image: A new study asserts vagus nerve stimulation can speed up stroke recovery (Photo courtesy of LivaNova).
A new study suggests that combining vagus nerve stimulation (VNS) with physical therapy doubles long-term stroke recovery rate, relative to current methods.
Researchers at the University of Texas at Dallas (UTD; Richardson, USA) and the Texas Biomedical Device Center (TxBDC; Richardson, USA) conducted a study in rats to determine if VNS could promote generalization, long-lasting recovery, and structural plasticity in motor function after stroke. The rats were first trained on a fully automated, quantitative task that measures forelimb supination. Once the rats achieved task proficiency, unilateral cortical and subcortical ischemic lesions were administered.
One week later, the rats were randomly assigned to receive a total of six weeks of rehabilitative training on the learned supination task, with or without VNS. The rats additionally underwent four weeks of testing to assess forelimb strength as an indicator of generalization of recovery. The durability of VNS benefits were also tested on the supination task two months after cessation of VNS, with viral tracing performed in order to assess synaptic connectivity in motor networks.
The results revealed that VNS enhanced plasticity in corticospinal motor networks, with a threefold-to-fivefold increase in the number of engaged neurons. Synaptic connectivity to the musculature of the rehabilitated forelimb was also enhanced, more than doubling the benefit of rehabilitative training. The researchers also found that pairing VNS with supination training in previously unknown tasks resulted in significantly improved volitional forelimb strength, suggesting generalization of forelimb recovery. The study was published on January 25, 2018, in Stroke.
“Our experiment was designed to ask this new question: After a stroke, do you have to rehabilitate every single action? If VNS helps you, is it only helping with the exact motion or function you paired with stimulation?” said study co-author Michael Kilgard, MD, associate director of TxBDC. “What we found was that it also improves similar motor skills as well, and that those results were sustained months beyond the completion of VNS-paired therapy. If we use this approach on complicated motor skills, those improvements can filter down to improve simpler movements.”
“If you have a stroke, you may have a limited time with a therapist. So when we create guidelines for a therapist, we now know to advise doing one complex activity as many times as possible, as opposed to a variety of activities,” said senior author Seth Hays, PhD, director of preclinical research at TxBDC. “That was an important finding; it was exciting that not only do we improve the task that we trained on, but also relatively similar tasks. You are getting generalization to related things, and you're getting sustained improvement months down the line.”
The vagus nerve is the tenth cranial nerve, and interfaces with parasympathetic control of the heart, lungs, and digestive tract. It is the longest nerve of the autonomic nervous system, supplying motor parasympathetic fibers to all the organs (except the adrenal glands), from the neck down to the second segment of the transverse colon. It also innervates several skeletal muscles, including the cricothyroid, the superior, middle and inferior pharyngeal constrictors, and other muscles of the pharynx and larynx, thus controlling muscle movements in the mouth and speech.
Related Links:
University of Texas at Dallas
Texas Biomedical Device Center
Researchers at the University of Texas at Dallas (UTD; Richardson, USA) and the Texas Biomedical Device Center (TxBDC; Richardson, USA) conducted a study in rats to determine if VNS could promote generalization, long-lasting recovery, and structural plasticity in motor function after stroke. The rats were first trained on a fully automated, quantitative task that measures forelimb supination. Once the rats achieved task proficiency, unilateral cortical and subcortical ischemic lesions were administered.
One week later, the rats were randomly assigned to receive a total of six weeks of rehabilitative training on the learned supination task, with or without VNS. The rats additionally underwent four weeks of testing to assess forelimb strength as an indicator of generalization of recovery. The durability of VNS benefits were also tested on the supination task two months after cessation of VNS, with viral tracing performed in order to assess synaptic connectivity in motor networks.
The results revealed that VNS enhanced plasticity in corticospinal motor networks, with a threefold-to-fivefold increase in the number of engaged neurons. Synaptic connectivity to the musculature of the rehabilitated forelimb was also enhanced, more than doubling the benefit of rehabilitative training. The researchers also found that pairing VNS with supination training in previously unknown tasks resulted in significantly improved volitional forelimb strength, suggesting generalization of forelimb recovery. The study was published on January 25, 2018, in Stroke.
“Our experiment was designed to ask this new question: After a stroke, do you have to rehabilitate every single action? If VNS helps you, is it only helping with the exact motion or function you paired with stimulation?” said study co-author Michael Kilgard, MD, associate director of TxBDC. “What we found was that it also improves similar motor skills as well, and that those results were sustained months beyond the completion of VNS-paired therapy. If we use this approach on complicated motor skills, those improvements can filter down to improve simpler movements.”
“If you have a stroke, you may have a limited time with a therapist. So when we create guidelines for a therapist, we now know to advise doing one complex activity as many times as possible, as opposed to a variety of activities,” said senior author Seth Hays, PhD, director of preclinical research at TxBDC. “That was an important finding; it was exciting that not only do we improve the task that we trained on, but also relatively similar tasks. You are getting generalization to related things, and you're getting sustained improvement months down the line.”
The vagus nerve is the tenth cranial nerve, and interfaces with parasympathetic control of the heart, lungs, and digestive tract. It is the longest nerve of the autonomic nervous system, supplying motor parasympathetic fibers to all the organs (except the adrenal glands), from the neck down to the second segment of the transverse colon. It also innervates several skeletal muscles, including the cricothyroid, the superior, middle and inferior pharyngeal constrictors, and other muscles of the pharynx and larynx, thus controlling muscle movements in the mouth and speech.
Related Links:
University of Texas at Dallas
Texas Biomedical Device Center
Latest Critical Care News
- Automated IV Labeling Solution Improves Infusion Safety and Efficiency
- First-Of-Its-Kind AI Tool Detects Pulmonary Hypertension from Standard ECGs
- 4D Digital Twin Heart Model Improves CRT Outcomes
- AI Turns Glucose Data Into Actionable Insights for Diabetes Care
- Microscale Wireless Implant Tracks Brain Activity Over Time
- Smart Mask Delivers Continuous, Battery-Free Breath Monitoring
- Routine Blood Pressure Readings May Identify Risk of Future Cognitive Decline
- CGM-Based Algorithm Enhances Insulin Dose Adjustment in Type 2 Diabetes
- Fish Scale–Based Implants Offer New Approach to Corneal Repair
- Dual-Function Wound Patch Combines Infection Sensing and Treatment
- Smartwatch Signals and Blood Tests Team Up for Early Warning on Insulin Resistance
- Smart Fabric Technology Aims to Prevent Pressure Injuries in Hospital Care
- Standardized Treatment Algorithm Improves Blood Pressure Control
- Combined Infection Control Strategy Limits Drug-Resistant Outbreak in NICU
- AI Helps Predict Which Heart-Failure Patients Will Worsen Within a Year
- Algorithm Allows Paramedics to Predict Brain Damage Risk After Cardiac Arrest
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreSurgical Techniques
view channel
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read more
New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
Volumetric muscle loss is a traumatic loss of skeletal muscle that often leads to permanent functional impairment and limited reconstructive options. Current experimental strategies struggle to deliver... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel





















