Plant-Based Vaccine for COVID-19 Could Prevent Novel Coronavirus Spread
|
By HospiMedica International staff writers Posted on 24 Mar 2020 |
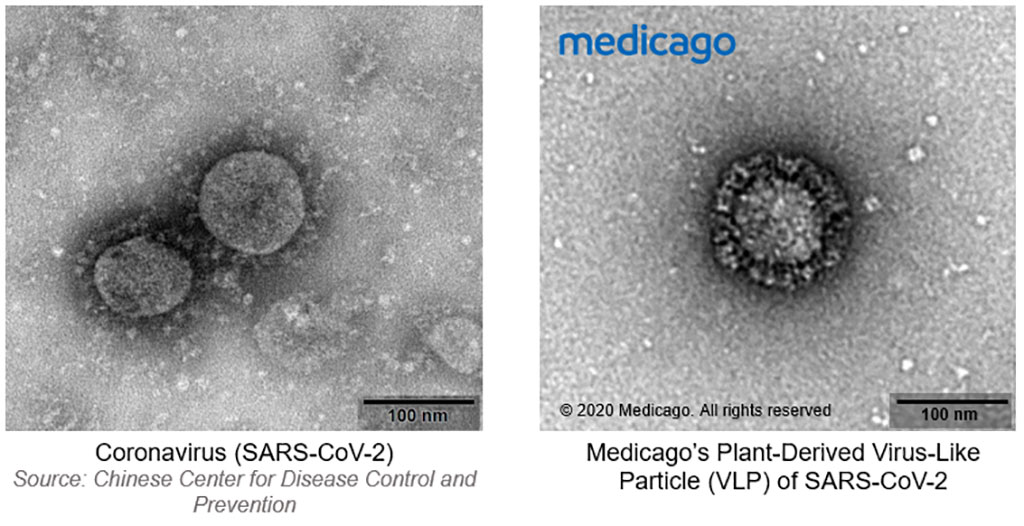
Image: Plant-based vaccine for COVID-19 could prevent novel coronavirus spread (Photo courtesy of Medicago, Inc.)
Medicago, Inc. (Quebec City, Canada), a biopharmaceutical company, has successfully produced a Virus-Like Particle (VLP) of the coronavirus just 20 days after obtaining the SARS-CoV-2 (virus causing the COVID-19 disease) gene. The production of the VLP is the first step in developing a vaccine for COVID-19 which will now undergo preclinical testing for safety and efficacy. Once this is completed, Medicago expects to discuss with the appropriate health agencies to initiate human trials of the vaccine by July-August 2020.
Medicago uses a proprietary plant-based technology to develop protein-based therapeutics. Unlike traditional vaccination development, the company does not use animal products or live viruses to create its products. Instead, it uses VLPs that mimic the shape and dimensions of a virus, which allows the body to recognize them and create an immune response in a non-infectious way. Clinical trial data suggest that VLPs have a multi-modal mechanism of action that is different from that of inactivated vaccines, activating both arms of the immune system – antibody and cell-mediated responses. Medicago’s proprietary technology is rapid, versatile, and scalable. As soon as the genetic sequence of a virus is made available, Medicago can develop a clinical-grade vaccine candidate in only a few weeks. Its recombinant technology allows the production of a vaccine that precisely matches the circulating strains, such as in the case of seasonal influenza. The technology is easily scalable, allowing the company to increase volume of production by simply increasing the number of plants it uses.
Medicago has previously demonstrated its capability as a first responder in a flu pandemic. In 2009, the company produced a research-grade vaccine candidate against H1N1 in just 19 days. In 2012, Medicago manufactured 10 million doses of a monovalent influenza vaccine within one month for the Defense Advanced Research Projects Agency (DARPA), part of the US Department of Defense. In 2015, Medicago also demonstrated that it could rapidly produce an anti-Ebola monoclonal antibody cocktail for the Biomedical Advanced Research and Development Authority (BARDA), part of the US Department of Health and Human Services. Medicago’s first product, a seasonal recombinant quadrivalent VLP vaccine for active immunization against influenza, is currently under review by Health Canada following the completion of a robust safety and efficacy clinical program involving over 25,000 patients.
Medicago is also using its technology platform to develop antibodies against SARS-CoV-2 in collaboration with the Laval University’s Infectious Disease Research Centre headed by Dr. Gary Kobinger, Professor in the Department of Microbiology and Infectious Diseases and the Director of the Infectious Disease Research Centre at Laval University, who helped develop a vaccine and treatment for Ebola. These SARS-CoV-2 antibodies could potentially be used to treat people infected by the virus.
“The pace of our initial progress in COVID-19 is attributable to the capability of our plant-based platform which is able to produce vaccine and antibody solutions to counteract this global public health threat. The ability to produce a candidate vaccine within 20 days after obtaining the gene is a critical differentiator for our proven technology. This technology enables scale-up at unprecedented speed to potentially combat COVID-19,” said Dr. Bruce Clark, CEO of Medicago.
“The collaborative efforts established between the research team at Laval University and Medicago have been very successful in developing unique antibodies against infectious diseases such as RSV and HMPV and that experience gives us confidence for successful identification of therapeutic antibodies against SARS-CoV-2,” said Dr. Gary Kobinger.
Related Links:
Medicago, Inc.
Medicago uses a proprietary plant-based technology to develop protein-based therapeutics. Unlike traditional vaccination development, the company does not use animal products or live viruses to create its products. Instead, it uses VLPs that mimic the shape and dimensions of a virus, which allows the body to recognize them and create an immune response in a non-infectious way. Clinical trial data suggest that VLPs have a multi-modal mechanism of action that is different from that of inactivated vaccines, activating both arms of the immune system – antibody and cell-mediated responses. Medicago’s proprietary technology is rapid, versatile, and scalable. As soon as the genetic sequence of a virus is made available, Medicago can develop a clinical-grade vaccine candidate in only a few weeks. Its recombinant technology allows the production of a vaccine that precisely matches the circulating strains, such as in the case of seasonal influenza. The technology is easily scalable, allowing the company to increase volume of production by simply increasing the number of plants it uses.
Medicago has previously demonstrated its capability as a first responder in a flu pandemic. In 2009, the company produced a research-grade vaccine candidate against H1N1 in just 19 days. In 2012, Medicago manufactured 10 million doses of a monovalent influenza vaccine within one month for the Defense Advanced Research Projects Agency (DARPA), part of the US Department of Defense. In 2015, Medicago also demonstrated that it could rapidly produce an anti-Ebola monoclonal antibody cocktail for the Biomedical Advanced Research and Development Authority (BARDA), part of the US Department of Health and Human Services. Medicago’s first product, a seasonal recombinant quadrivalent VLP vaccine for active immunization against influenza, is currently under review by Health Canada following the completion of a robust safety and efficacy clinical program involving over 25,000 patients.
Medicago is also using its technology platform to develop antibodies against SARS-CoV-2 in collaboration with the Laval University’s Infectious Disease Research Centre headed by Dr. Gary Kobinger, Professor in the Department of Microbiology and Infectious Diseases and the Director of the Infectious Disease Research Centre at Laval University, who helped develop a vaccine and treatment for Ebola. These SARS-CoV-2 antibodies could potentially be used to treat people infected by the virus.
“The pace of our initial progress in COVID-19 is attributable to the capability of our plant-based platform which is able to produce vaccine and antibody solutions to counteract this global public health threat. The ability to produce a candidate vaccine within 20 days after obtaining the gene is a critical differentiator for our proven technology. This technology enables scale-up at unprecedented speed to potentially combat COVID-19,” said Dr. Bruce Clark, CEO of Medicago.
“The collaborative efforts established between the research team at Laval University and Medicago have been very successful in developing unique antibodies against infectious diseases such as RSV and HMPV and that experience gives us confidence for successful identification of therapeutic antibodies against SARS-CoV-2,” said Dr. Gary Kobinger.
Related Links:
Medicago, Inc.
Latest COVID-19 News
- Low-Cost System Detects SARS-CoV-2 Virus in Hospital Air Using High-Tech Bubbles
- World's First Inhalable COVID-19 Vaccine Approved in China
- COVID-19 Vaccine Patch Fights SARS-CoV-2 Variants Better than Needles
- Blood Viscosity Testing Can Predict Risk of Death in Hospitalized COVID-19 Patients
- ‘Covid Computer’ Uses AI to Detect COVID-19 from Chest CT Scans
- MRI Lung-Imaging Technique Shows Cause of Long-COVID Symptoms
- Chest CT Scans of COVID-19 Patients Could Help Distinguish Between SARS-CoV-2 Variants
- Specialized MRI Detects Lung Abnormalities in Non-Hospitalized Long COVID Patients
- AI Algorithm Identifies Hospitalized Patients at Highest Risk of Dying From COVID-19
- Sweat Sensor Detects Key Biomarkers That Provide Early Warning of COVID-19 and Flu
- Study Assesses Impact of COVID-19 on Ventilation/Perfusion Scintigraphy
- CT Imaging Study Finds Vaccination Reduces Risk of COVID-19 Associated Pulmonary Embolism
- Third Day in Hospital a ‘Tipping Point’ in Severity of COVID-19 Pneumonia
- Longer Interval Between COVID-19 Vaccines Generates Up to Nine Times as Many Antibodies
- AI Model for Monitoring COVID-19 Predicts Mortality Within First 30 Days of Admission
- AI Predicts COVID Prognosis at Near-Expert Level Based Off CT Scans
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read more
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read moreSurgical Techniques
view channel
Ultrasound Technology Aims to Replace Invasive BPH Procedures
Benign prostatic hyperplasia (BPH) is a frequent cause of lower urinary tract symptoms in aging men and often requires invasive procedures or prolonged recovery. With prevalence expected to rise as populations... Read more
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel