Oversensitive COVID-19 Tests Detecting Dead Coronavirus Cells, Driving False Positives and Reinfections
|
By HospiMedica International staff writers Posted on 07 Sep 2020 |

Illustration
A study by the Oxford University’s Centre for Evidence-Based Medicine (Oxford, England) suggests that the current COVID-19 diagnostic tests could be too sensitive and may be detecting dead coronavirus cells, leading to overestimated infections.
According to the researchers, the tests used to diagnose COVID-19 are so sensitive that they may be indicating people are infected with SARS-CoV-2 even when they had the virus 70 days ago. Prof Carl Heneghan, director of the Centre for Evidence-Based Medicine, believes that eight days after contracting COVID-19, the chances of an infected person passing on the virus to others become zero if there are no symptoms. However, fragments of the coronavirus can still remain in the body for several weeks afterwards.
Polymerase chain reaction (PCR) tests currently used to detect SARS-CoV-2 have technical limitations as they cannot distinguish whether the virus in the patient is alive or dead. The researchers analyzed 25 studies on PCR tests and found that such tests can suggest people are infected even after their bodies’ immune system has already fought off the coronavirus because these tests only provide a ‘yes’ or ‘no’ as to whether the virus material is in the body. This means such people would test positive even though the coronavirus in their bodies may be harmless and non-infectious.
"After about day eight, you can still find the RNA fragments," Prof Heneghan told BBC Radio 4's Today program. "Some studies have reported up to 70 days that you intermittently shed. You can understand the importance of this, because what you want to do is find those with active infection and not those with the RNA fragments."
“Evidence is mounting that a good proportion of ‘new’ mild cases and people re-testing positive after quarantine or discharge from hospital are not infectious, but are simply clearing harmless virus particles which their immune system has efficiently dealt with,” added Prof Heneghan.
Earlier, a team of South Korean researchers had revealed that reports of recovered coronavirus patients testing positive for SARS-CoV-2 infection a second time round were most likely due to dead-virus fragments. They found that 260 people who had recovered and were declared virus-free tested positive again in South Korea but had little or no contagiousness at all. This meant that they were incapable of transmitting the virus to others, based on virus culture cells that all failed to find live viruses in the recovered patients.
“PCR testing that amplifies genetics of the virus is used in Korea to test COVID-19, and relapse cases are due to technical limits of the PCR testing. The respiratory epithelial cell has a half-life of up to three months, and RNA virus in the cell can be detected with PCR testing one to two months after the elimination of the cell,” said Oh Myoung-don, who spearheads the central clinical committee for emerging disease control in South Korea.
Related Links:
Oxford University’s Centre for Evidence-Based Medicine
According to the researchers, the tests used to diagnose COVID-19 are so sensitive that they may be indicating people are infected with SARS-CoV-2 even when they had the virus 70 days ago. Prof Carl Heneghan, director of the Centre for Evidence-Based Medicine, believes that eight days after contracting COVID-19, the chances of an infected person passing on the virus to others become zero if there are no symptoms. However, fragments of the coronavirus can still remain in the body for several weeks afterwards.
Polymerase chain reaction (PCR) tests currently used to detect SARS-CoV-2 have technical limitations as they cannot distinguish whether the virus in the patient is alive or dead. The researchers analyzed 25 studies on PCR tests and found that such tests can suggest people are infected even after their bodies’ immune system has already fought off the coronavirus because these tests only provide a ‘yes’ or ‘no’ as to whether the virus material is in the body. This means such people would test positive even though the coronavirus in their bodies may be harmless and non-infectious.
"After about day eight, you can still find the RNA fragments," Prof Heneghan told BBC Radio 4's Today program. "Some studies have reported up to 70 days that you intermittently shed. You can understand the importance of this, because what you want to do is find those with active infection and not those with the RNA fragments."
“Evidence is mounting that a good proportion of ‘new’ mild cases and people re-testing positive after quarantine or discharge from hospital are not infectious, but are simply clearing harmless virus particles which their immune system has efficiently dealt with,” added Prof Heneghan.
Earlier, a team of South Korean researchers had revealed that reports of recovered coronavirus patients testing positive for SARS-CoV-2 infection a second time round were most likely due to dead-virus fragments. They found that 260 people who had recovered and were declared virus-free tested positive again in South Korea but had little or no contagiousness at all. This meant that they were incapable of transmitting the virus to others, based on virus culture cells that all failed to find live viruses in the recovered patients.
“PCR testing that amplifies genetics of the virus is used in Korea to test COVID-19, and relapse cases are due to technical limits of the PCR testing. The respiratory epithelial cell has a half-life of up to three months, and RNA virus in the cell can be detected with PCR testing one to two months after the elimination of the cell,” said Oh Myoung-don, who spearheads the central clinical committee for emerging disease control in South Korea.
Related Links:
Oxford University’s Centre for Evidence-Based Medicine
Latest COVID-19 News
- Low-Cost System Detects SARS-CoV-2 Virus in Hospital Air Using High-Tech Bubbles
- World's First Inhalable COVID-19 Vaccine Approved in China
- COVID-19 Vaccine Patch Fights SARS-CoV-2 Variants Better than Needles
- Blood Viscosity Testing Can Predict Risk of Death in Hospitalized COVID-19 Patients
- ‘Covid Computer’ Uses AI to Detect COVID-19 from Chest CT Scans
- MRI Lung-Imaging Technique Shows Cause of Long-COVID Symptoms
- Chest CT Scans of COVID-19 Patients Could Help Distinguish Between SARS-CoV-2 Variants
- Specialized MRI Detects Lung Abnormalities in Non-Hospitalized Long COVID Patients
- AI Algorithm Identifies Hospitalized Patients at Highest Risk of Dying From COVID-19
- Sweat Sensor Detects Key Biomarkers That Provide Early Warning of COVID-19 and Flu
- Study Assesses Impact of COVID-19 on Ventilation/Perfusion Scintigraphy
- CT Imaging Study Finds Vaccination Reduces Risk of COVID-19 Associated Pulmonary Embolism
- Third Day in Hospital a ‘Tipping Point’ in Severity of COVID-19 Pneumonia
- Longer Interval Between COVID-19 Vaccines Generates Up to Nine Times as Many Antibodies
- AI Model for Monitoring COVID-19 Predicts Mortality Within First 30 Days of Admission
- AI Predicts COVID Prognosis at Near-Expert Level Based Off CT Scans
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel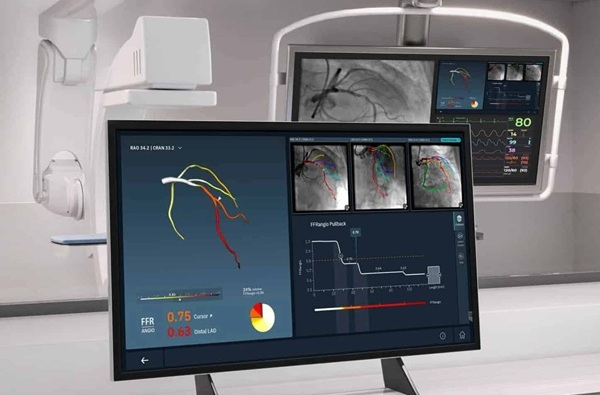
Angiography-Based FFR Approach Matches Gold Standard Results Without Wires
Accurately determining whether a coronary stenosis limits blood flow is essential to guide percutaneous coronary intervention, yet wire-based physiologic testing remains underused due to added procedural... Read more
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read moreSurgical Techniques
view channel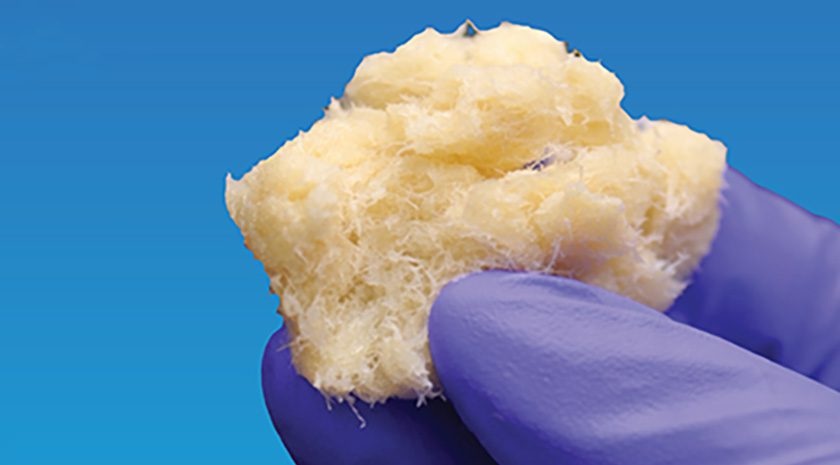
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more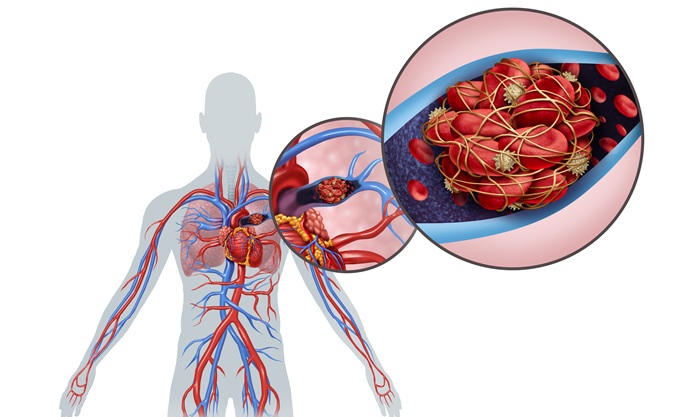
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel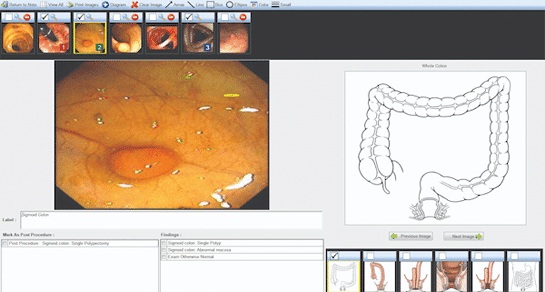
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel























