Blocking Immune System Pathway Could Stop COVID-19 Infection, Finds Study
|
By HospiMedica International staff writers Posted on 14 Oct 2020 |
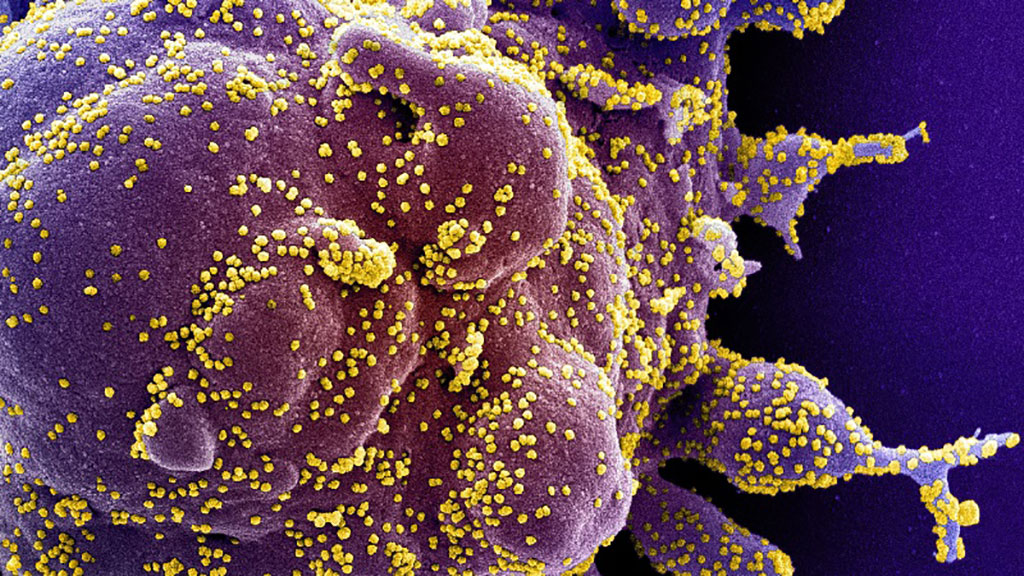
Image: Colorized scanning electron micrograph of a cell (purple) heavily infected with SARS-CoV-2 virus particles (yellow) (Photo courtesy of National Institute of Allergy and Infectious Diseases, National Institutes of Health)
A recent study has shown that blocking a specific protein in a biological pathway may prevent SARS-CoV-2 infection and keep the virus from misdirecting the immune system against healthy cells and organs.
While the world waits eagerly for a safe and effective vaccine to prevent infections from SARS-CoV-2, the virus behind the COVID-19 pandemic, researchers also are focusing on better understanding how SARS-CoV-2 attacks the body in the search for other means of stopping its devastating impact. The key to one possibility - blocking a protein that enables the virus to turn the immune system against healthy cells - has been identified in a recent study by a team of researchers at Johns Hopkins Medicine (Baltimore, MD, USA).
Scientists already know that spike proteins on the surface of the SARS-CoV-2 virus — making the pathogen look like the spiny ball from a medieval mace — are the means by which it attaches to cells targeted for infection. To do this, the spikes first grab hold of heparan sulfate, a large, complex sugar molecule found on the surface of cells in the lungs, blood vessels and smooth muscle making up most organs. Facilitated by its initial binding with heparan sulfate, SARS-CoV-2 then uses another cell-surface component, the protein known as angiotensin-converting enzyme 2 (ACE2), as its doorway into the attacked cell.
The Johns Hopkins Medicine team discovered that when SARS-CoV-2 ties up heparan sulfate, it prevents factor H from using the sugar molecule to bind with cells. Factor H’s normal function is to regulate the chemical signals that trigger inflammation and keep the immune system from harming healthy cells. Without this protection, cells in the lungs, heart, kidneys and other organs can be destroyed by the defense mechanism nature intended to safeguard them.
“Previous research has suggested that along with tying up heparan sulfate, SARS-CoV-2 activates a cascading series of biological reactions - what we call the alternative pathway of complement, or APC - that can lead to inflammation and cell destruction if misdirected by the immune system at healthy organs,” said study senior author Robert Brodsky, M.D., director of the hematology division at the Johns Hopkins University School of Medicine. “The goal of our study was to discover how the virus activates this pathway and to find a way to inhibit it before the damage happens.”
The APC is one of three chain reaction processes involving the splitting and combining of more than 20 different proteins - known as complement proteins - that usually gets activated when bacteria or viruses invade the body. The end product of this complement cascade, a structure called membrane attack complex (MAC), forms on the surface of the invader and causes its destruction, either by creating holes in bacterial membranes or disrupting a virus’ outer envelope. However, MACs also can arise on the membranes of healthy cells. Fortunately, humans have a number of complement proteins, including factor H, that regulate the APC, keep it in check and therefore, protect normal cells from damage by MACs.
In a series of experiments, the Johns Hopkins researchers used normal human blood serum and three subunits of the SARS-CoV-2 spike protein to discover exactly how the virus activates the APC, hijacks the immune system and endangers normal cells. They discovered that two of the subunits, called S1 and S2, are the components that bind the virus to heparan sulfate - setting off the APC cascade and blocking factor H from connecting with the sugar - and in turn, disabling the complement regulation by which factor H deters a misdirected immune response. In turn, the resulting immune system response to chemicals released by the lysing of killed cells could be responsible for the organ damage and failures seen in severe cases of COVID-19. Most notably, the research team found by blocking another complement protein, known as factor D, which works immediately upstream in the pathway from factor H, they were able to stop the destructive chain of events triggered by SARS-CoV-2. Making the discovery even more exciting is that there may already be drugs in development and testing for other diseases that can do the required blocking. The researchers hope that their work will encourage more study into the potential use against COVID-19 of complement-inhibiting drugs already in the pipeline for other diseases.
Related Links:
Johns Hopkins Medicine
While the world waits eagerly for a safe and effective vaccine to prevent infections from SARS-CoV-2, the virus behind the COVID-19 pandemic, researchers also are focusing on better understanding how SARS-CoV-2 attacks the body in the search for other means of stopping its devastating impact. The key to one possibility - blocking a protein that enables the virus to turn the immune system against healthy cells - has been identified in a recent study by a team of researchers at Johns Hopkins Medicine (Baltimore, MD, USA).
Scientists already know that spike proteins on the surface of the SARS-CoV-2 virus — making the pathogen look like the spiny ball from a medieval mace — are the means by which it attaches to cells targeted for infection. To do this, the spikes first grab hold of heparan sulfate, a large, complex sugar molecule found on the surface of cells in the lungs, blood vessels and smooth muscle making up most organs. Facilitated by its initial binding with heparan sulfate, SARS-CoV-2 then uses another cell-surface component, the protein known as angiotensin-converting enzyme 2 (ACE2), as its doorway into the attacked cell.
The Johns Hopkins Medicine team discovered that when SARS-CoV-2 ties up heparan sulfate, it prevents factor H from using the sugar molecule to bind with cells. Factor H’s normal function is to regulate the chemical signals that trigger inflammation and keep the immune system from harming healthy cells. Without this protection, cells in the lungs, heart, kidneys and other organs can be destroyed by the defense mechanism nature intended to safeguard them.
“Previous research has suggested that along with tying up heparan sulfate, SARS-CoV-2 activates a cascading series of biological reactions - what we call the alternative pathway of complement, or APC - that can lead to inflammation and cell destruction if misdirected by the immune system at healthy organs,” said study senior author Robert Brodsky, M.D., director of the hematology division at the Johns Hopkins University School of Medicine. “The goal of our study was to discover how the virus activates this pathway and to find a way to inhibit it before the damage happens.”
The APC is one of three chain reaction processes involving the splitting and combining of more than 20 different proteins - known as complement proteins - that usually gets activated when bacteria or viruses invade the body. The end product of this complement cascade, a structure called membrane attack complex (MAC), forms on the surface of the invader and causes its destruction, either by creating holes in bacterial membranes or disrupting a virus’ outer envelope. However, MACs also can arise on the membranes of healthy cells. Fortunately, humans have a number of complement proteins, including factor H, that regulate the APC, keep it in check and therefore, protect normal cells from damage by MACs.
In a series of experiments, the Johns Hopkins researchers used normal human blood serum and three subunits of the SARS-CoV-2 spike protein to discover exactly how the virus activates the APC, hijacks the immune system and endangers normal cells. They discovered that two of the subunits, called S1 and S2, are the components that bind the virus to heparan sulfate - setting off the APC cascade and blocking factor H from connecting with the sugar - and in turn, disabling the complement regulation by which factor H deters a misdirected immune response. In turn, the resulting immune system response to chemicals released by the lysing of killed cells could be responsible for the organ damage and failures seen in severe cases of COVID-19. Most notably, the research team found by blocking another complement protein, known as factor D, which works immediately upstream in the pathway from factor H, they were able to stop the destructive chain of events triggered by SARS-CoV-2. Making the discovery even more exciting is that there may already be drugs in development and testing for other diseases that can do the required blocking. The researchers hope that their work will encourage more study into the potential use against COVID-19 of complement-inhibiting drugs already in the pipeline for other diseases.
Related Links:
Johns Hopkins Medicine
Latest COVID-19 News
- Low-Cost System Detects SARS-CoV-2 Virus in Hospital Air Using High-Tech Bubbles
- World's First Inhalable COVID-19 Vaccine Approved in China
- COVID-19 Vaccine Patch Fights SARS-CoV-2 Variants Better than Needles
- Blood Viscosity Testing Can Predict Risk of Death in Hospitalized COVID-19 Patients
- ‘Covid Computer’ Uses AI to Detect COVID-19 from Chest CT Scans
- MRI Lung-Imaging Technique Shows Cause of Long-COVID Symptoms
- Chest CT Scans of COVID-19 Patients Could Help Distinguish Between SARS-CoV-2 Variants
- Specialized MRI Detects Lung Abnormalities in Non-Hospitalized Long COVID Patients
- AI Algorithm Identifies Hospitalized Patients at Highest Risk of Dying From COVID-19
- Sweat Sensor Detects Key Biomarkers That Provide Early Warning of COVID-19 and Flu
- Study Assesses Impact of COVID-19 on Ventilation/Perfusion Scintigraphy
- CT Imaging Study Finds Vaccination Reduces Risk of COVID-19 Associated Pulmonary Embolism
- Third Day in Hospital a ‘Tipping Point’ in Severity of COVID-19 Pneumonia
- Longer Interval Between COVID-19 Vaccines Generates Up to Nine Times as Many Antibodies
- AI Model for Monitoring COVID-19 Predicts Mortality Within First 30 Days of Admission
- AI Predicts COVID Prognosis at Near-Expert Level Based Off CT Scans
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read more
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read moreSurgical Techniques
view channel
Ultrasound Technology Aims to Replace Invasive BPH Procedures
Benign prostatic hyperplasia (BPH) is a frequent cause of lower urinary tract symptoms in aging men and often requires invasive procedures or prolonged recovery. With prevalence expected to rise as populations... Read more
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel