ECMO Can Be Used as `Salvage Therapy` for COVID-19 Patients with Acute Respiratory Distress Syndrome, Finds New Study
|
By HospiMedica International staff writers Posted on 15 Apr 2021 |
Illustration
A large study has suggested survival benefit for severely ill COVID-19 patients treated with extracorporeal membrane oxygenation (ECMO).
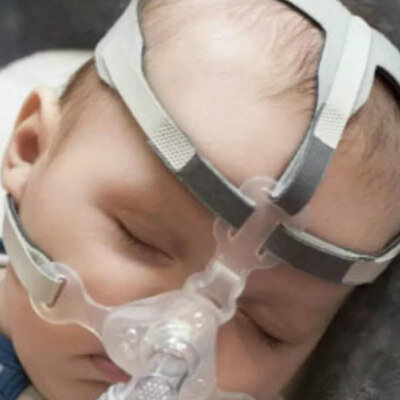
The findings of the study by researchers at University of California, Irvine Medical Center (UCIMC; Orange County, CA, USA) support the use of ECMO as "salvage therapy" for COVID-19 patients with acute respiratory distress syndrome (ARDS) or respiratory failure who do not improve with conventional mechanical ventilatory support. For critically ill COVID-19 patients treated with ECMO, the risk of death remains high - but is much lower than suggested by initial studies, according to the new research.
ECMO is a life-sustaining therapy for carefully selected patients with respiratory or circulatory failure. Requiring specialized equipment and highly trained professionals, ECMO is mainly provided at large medical centers. While some hospitals have been using ECMO therapy for COVID-19 patients with severe ARDS, there is a "paucity of data" on outcomes, according to the authors. Initial case series reported "exceedingly high" mortality rates: over 90%.
For their study, the researchers analyzed the outcomes of 11,182 patients with COVID-19 and ARDS who received ECMO between April and September 2020. The patients were treated at 155 US medical centers; numbers of patients treated with ECMO ranged from 1 to 38 per hospital. The majority of patients were under the age of 50 years (57.9%) with about 37% aged 51 to 64 years. Only about 5% were aged 65 years or older. For these ECMO-treated COVID-19 patients with ARDS, the overall rate of in-hospital death was 45.9%. Although high, that is roughly half the mortality rate reported in smaller ECMO studies from early in the pandemic. It's also comparable to the 39% death rate in a recent analysis of about 1,000 patients from the Extracorporeal Life Support Organization registry (largely treated at higher-volume ECMO centers).
For patients in the new study, average length of hospital stay was lengthy: 37 days, including 29 days in the intensive care unit. The in-hospital mortality rate increased with age: from about 25% for patients aged up to 30 years, to 42% for those aged 31 to 50 years, 53% for those aged 51 to 64, and 74% for those aged 65 or older. The researchers performed a subset analysis comparing patients aged 18 to 64 who were treated with (1,113 patients) or without ECMO (16,343 patients). In-hospital mortality was 44.6% for the ECMO-treated patients compared to 37.9% for those treated without ECMO.
"Our findings refute previous reports of futility for ECMO therapy in the setting of COVID-19," said Fabio Sagebin, MD, of the UCIMC Division of Cardiothoracic Surgery. "Our data showed that patients with COVID-19 and ARDS treated with conventional ventilatory support had a high risk of death and patients selected for ECMO, which is a higher risk group, had a similarly high rate of death. The data suggests that in appropriately selected patients, we can save lives with this therapy."
Related Links:
UCIMC
The findings of the study by researchers at University of California, Irvine Medical Center (UCIMC; Orange County, CA, USA) support the use of ECMO as "salvage therapy" for COVID-19 patients with acute respiratory distress syndrome (ARDS) or respiratory failure who do not improve with conventional mechanical ventilatory support. For critically ill COVID-19 patients treated with ECMO, the risk of death remains high - but is much lower than suggested by initial studies, according to the new research.
ECMO is a life-sustaining therapy for carefully selected patients with respiratory or circulatory failure. Requiring specialized equipment and highly trained professionals, ECMO is mainly provided at large medical centers. While some hospitals have been using ECMO therapy for COVID-19 patients with severe ARDS, there is a "paucity of data" on outcomes, according to the authors. Initial case series reported "exceedingly high" mortality rates: over 90%.
For their study, the researchers analyzed the outcomes of 11,182 patients with COVID-19 and ARDS who received ECMO between April and September 2020. The patients were treated at 155 US medical centers; numbers of patients treated with ECMO ranged from 1 to 38 per hospital. The majority of patients were under the age of 50 years (57.9%) with about 37% aged 51 to 64 years. Only about 5% were aged 65 years or older. For these ECMO-treated COVID-19 patients with ARDS, the overall rate of in-hospital death was 45.9%. Although high, that is roughly half the mortality rate reported in smaller ECMO studies from early in the pandemic. It's also comparable to the 39% death rate in a recent analysis of about 1,000 patients from the Extracorporeal Life Support Organization registry (largely treated at higher-volume ECMO centers).
For patients in the new study, average length of hospital stay was lengthy: 37 days, including 29 days in the intensive care unit. The in-hospital mortality rate increased with age: from about 25% for patients aged up to 30 years, to 42% for those aged 31 to 50 years, 53% for those aged 51 to 64, and 74% for those aged 65 or older. The researchers performed a subset analysis comparing patients aged 18 to 64 who were treated with (1,113 patients) or without ECMO (16,343 patients). In-hospital mortality was 44.6% for the ECMO-treated patients compared to 37.9% for those treated without ECMO.
"Our findings refute previous reports of futility for ECMO therapy in the setting of COVID-19," said Fabio Sagebin, MD, of the UCIMC Division of Cardiothoracic Surgery. "Our data showed that patients with COVID-19 and ARDS treated with conventional ventilatory support had a high risk of death and patients selected for ECMO, which is a higher risk group, had a similarly high rate of death. The data suggests that in appropriately selected patients, we can save lives with this therapy."
Related Links:
UCIMC
Latest COVID-19 News
- Low-Cost System Detects SARS-CoV-2 Virus in Hospital Air Using High-Tech Bubbles
- World's First Inhalable COVID-19 Vaccine Approved in China
- COVID-19 Vaccine Patch Fights SARS-CoV-2 Variants Better than Needles
- Blood Viscosity Testing Can Predict Risk of Death in Hospitalized COVID-19 Patients
- ‘Covid Computer’ Uses AI to Detect COVID-19 from Chest CT Scans
- MRI Lung-Imaging Technique Shows Cause of Long-COVID Symptoms
- Chest CT Scans of COVID-19 Patients Could Help Distinguish Between SARS-CoV-2 Variants
- Specialized MRI Detects Lung Abnormalities in Non-Hospitalized Long COVID Patients
- AI Algorithm Identifies Hospitalized Patients at Highest Risk of Dying From COVID-19
- Sweat Sensor Detects Key Biomarkers That Provide Early Warning of COVID-19 and Flu
- Study Assesses Impact of COVID-19 on Ventilation/Perfusion Scintigraphy
- CT Imaging Study Finds Vaccination Reduces Risk of COVID-19 Associated Pulmonary Embolism
- Third Day in Hospital a ‘Tipping Point’ in Severity of COVID-19 Pneumonia
- Longer Interval Between COVID-19 Vaccines Generates Up to Nine Times as Many Antibodies
- AI Model for Monitoring COVID-19 Predicts Mortality Within First 30 Days of Admission
- AI Predicts COVID Prognosis at Near-Expert Level Based Off CT Scans
Channels
Artificial Intelligence
view channel
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read more
New AI Approach Monitors Brain Health Using Passive Wearable Data
Brain health spans cognitive and emotional functions and can fluctuate even in adults without diagnosed disease. Detecting early changes remains difficult in routine care and burdens specialty services... Read moreCritical Care
view channel
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read more
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read moreSurgical Techniques
view channel
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read more
New Approach Enables Customized Muscle Tissue Without Biomaterial Scaffolds
Volumetric muscle loss is a traumatic loss of skeletal muscle that often leads to permanent functional impairment and limited reconstructive options. Current experimental strategies struggle to deliver... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel