Trauma Center Closure Increases Mortality Risk
|
By HospiMedica International staff writers Posted on 09 Apr 2014 |
A new study reveals a strong association between closure of trauma centers and increased mortality for patients with injuries.
Researchers at the University of California, San Francisco (UCSF; USA) performed a retrospective study of all adult patient visits for injuries at Level I and II to nonfederal trauma centers in California (USA) between 1999 and 2009, to examine the impact of three trauma center closures. The researchers compared the in-hospital mortality of 5,122 patients who lived in ZIP [US postal] codes where their drive time to that nearest trauma center increased as the result of a nearby closure to 228,236 patients whose drive time did not change, and 37,787 patients whose travel time decreased as the result of a trauma center opening. They also tested whether this effect was limited to a two-year period following a closure.
The results showed that decreased travel time to the closest trauma center was associated with 17% lower odds of in-hospital mortality compared to the group experiencing no change, while increased travel time was associated with 14% higher odds of in-hospital mortality. These effects were intensified in the first two years following a closure. Injured patients with decreased travel times to the nearest trauma center had 16% lower odds of death, while injured patients affected by a closure had 26% higher odds of death. The article was published in the March 2014 issue of the Journal of Trauma and Acute Care Surgery.
“This study confirms that when trauma centers close, people who live in the surrounding areas are more likely to die following an injury,” said lead author Renee Hsia, MD, an associate professor of emergency medicine at UCSF. “Affected patients were more likely to be young and low income, to identify as part of a racial or ethnic minority group, and have medical insurance.”
Trauma centers are an effective but costly element of the US health care infrastructure. Some Level I and II trauma centers regularly incur financial losses when these high fixed costs are coupled with high burdens of uncompensated care for disproportionately young and uninsured trauma patients. As a result, they are at risk of reducing their services or closing.
Related Links:
University of California, San Francisco
Researchers at the University of California, San Francisco (UCSF; USA) performed a retrospective study of all adult patient visits for injuries at Level I and II to nonfederal trauma centers in California (USA) between 1999 and 2009, to examine the impact of three trauma center closures. The researchers compared the in-hospital mortality of 5,122 patients who lived in ZIP [US postal] codes where their drive time to that nearest trauma center increased as the result of a nearby closure to 228,236 patients whose drive time did not change, and 37,787 patients whose travel time decreased as the result of a trauma center opening. They also tested whether this effect was limited to a two-year period following a closure.
The results showed that decreased travel time to the closest trauma center was associated with 17% lower odds of in-hospital mortality compared to the group experiencing no change, while increased travel time was associated with 14% higher odds of in-hospital mortality. These effects were intensified in the first two years following a closure. Injured patients with decreased travel times to the nearest trauma center had 16% lower odds of death, while injured patients affected by a closure had 26% higher odds of death. The article was published in the March 2014 issue of the Journal of Trauma and Acute Care Surgery.
“This study confirms that when trauma centers close, people who live in the surrounding areas are more likely to die following an injury,” said lead author Renee Hsia, MD, an associate professor of emergency medicine at UCSF. “Affected patients were more likely to be young and low income, to identify as part of a racial or ethnic minority group, and have medical insurance.”
Trauma centers are an effective but costly element of the US health care infrastructure. Some Level I and II trauma centers regularly incur financial losses when these high fixed costs are coupled with high burdens of uncompensated care for disproportionately young and uninsured trauma patients. As a result, they are at risk of reducing their services or closing.
Related Links:
University of California, San Francisco
Latest Hospital News News
- Nurse Tracking System Improves Hospital Workflow
- New Children’s Hospital Transforms California Healthcare
- Noisy Hospitals Face Threat of Decreased Federal Compensation
- Orthopedics Centre of Excellence Planned for Guy’s Hospital
- Research Suggests Avoidance of Low-Value Surgical Procedures
- U.S. Federal Readmission Fines Linked to Higher Mortality
- Columbia China to Build New Hospital in Jiaxing
- Dubai Debuts Second Robotic Pharmacy Service
- Seattle Hospital Network Shifts Away from Overlapping Surgeries
- ACC to Launch Valvular Heart Disease Program in China
- Mortality Rates Lower at Major Teaching Hospitals
- South Australia to Inaugurate Upscale Hospital
- Raffles to Launch Second Hospital Project in China
- Research Center Tackles Antimicrobial Drugs Challenge
- Miami Cardiac & Vascular Institute Completes Expansion Project
- Hospital Antibiotic Policies Improve Prescription Practices
Channels
Artificial Intelligence
view channel
AI Tool Predicts Unplanned Care and Symptom Burden in Cancer Survivors
Unplanned emergency visits and hospitalizations remain common in cancer survivorship, when routine clinical contact often tapers while new symptoms emerge. These events reflect unmet needs and disrupt... Read more
Automated Phone Speech Test Identifies Alzheimer’s Pathology for Prescreening
Alzheimer’s disease assessment and trial recruitment often rely on costly, invasive biomarker testing and clinic-based cognitive evaluations, limiting scalability as populations age. Providers and trial... Read moreCritical Care
view channel
Ring-Type Cuffless Monitor Becomes First Added to Official Hypertension Guidelines
Detecting nocturnal and morning hypertension often requires out-of-office assessment, but conventional cuff-type monitors can disrupt sleep. New national guidance in South Korea expands 24-hour monitoring... Read more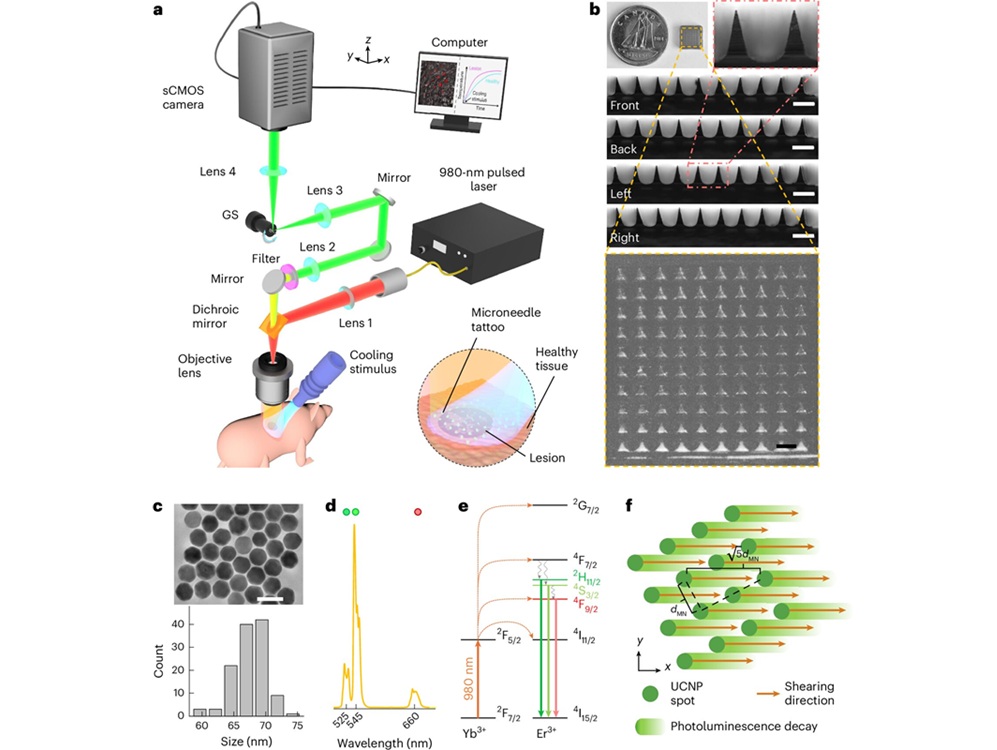
“Intelligent Tattoo” Method Detects Early Melanoma Signals
Melanoma is a lethal skin cancer in which earlier detection drives better outcomes. Current evaluation relies on visual inspection followed by biopsy, which can miss nascent lesions and lead to unnecessary... Read more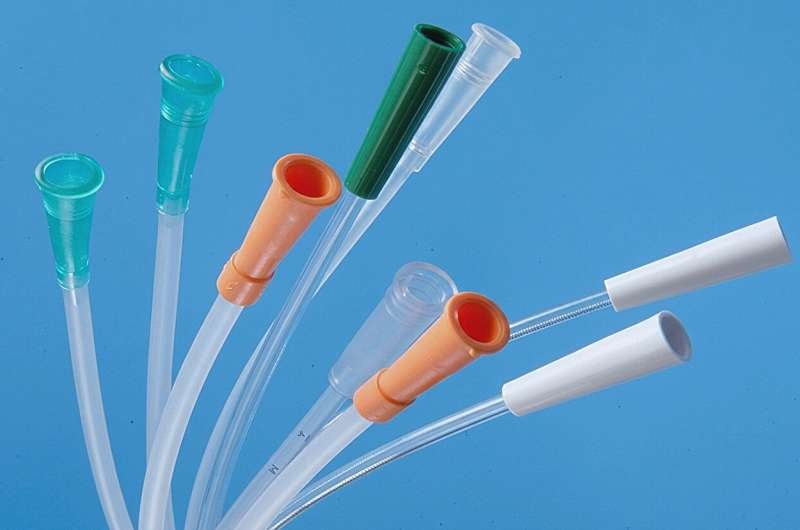
Reusable Intermittent Catheters Reduce Antibiotic Use Without Increasing Urinary Tract Infections
Intermittent self-catheterization, used to empty the bladder several times a day, can leave patients vulnerable to recurrent urinary tract infections and repeated antibiotic use. Reliance on single-use... Read moreSurgical Techniques
view channel
Fracture Plating System Combines Anatomical Fit with Streamlined Instrumentation
Fracture management involves diverse anatomies and injury patterns that can make plate fit and fixation strategy challenging. Surgeons need both intraoperative efficiency and flexibility, while hospitals... Read more
Pink Noise Stimulation Approach Could Support Safer Anesthesia
Maintaining stable unconsciousness during general anesthesia while minimizing drug exposure remains a core perioperative challenge. Sudden nociceptive surges can disrupt anesthetic depth, increasing neurological... Read morePatient Care
view channel
AI Avatar Doctor Improves Patient Understanding Before Radiotherapy
Radiation oncology consultations require patients to grasp complex concepts quickly, yet anxiety and information overload often undermine understanding and informed consent. Poor comprehension can also... Read more
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read moreHealth IT
view channel
AI-Native EHR Achieves EU Medical Device Certification
InterSystems (Boston, MA, USA) announced that its IntelliCare electronic health record (EHR) solutions have been certified as Class IIa medical devices under the European Union Medical Device Regulation... Read more
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read morePoint of Care
view channel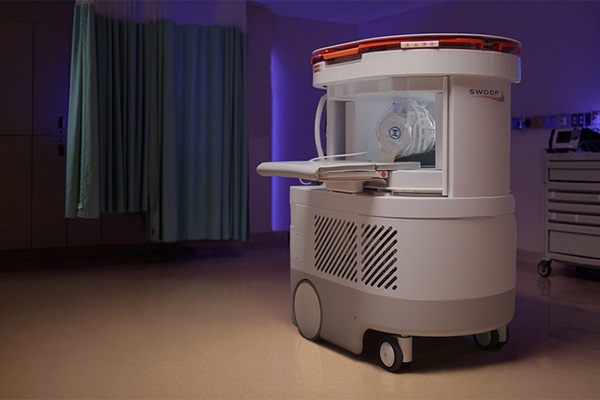
Portable MRI System Accelerates Emergency Brain Imaging and Triage
Emergency departments frequently face delays accessing conventional magnetic resonance imaging (MRI) for patients with suspected neurological emergencies. Such waits can slow triage, prolong boarding,... Read more