Hypothermia During Surgery Affects Recovery
|
By HospiMedica International staff writers Posted on 02 Feb 2015 |
Transient and mild intraoperative hypothermia during surgery contributes to adverse outcomes, according to a new study.
Researchers at the Cleveland Clinic (OH, USA), Chiang Mai University (Thailand), and other institutions conducted a study to evaluate body temperature patterns in warmed surgical patients, and determine whether even short periods of low temperature increased blood loss or prolong hospital stays. The researchers measured intraoperative core body temperature patterns in 58,814 adults in surgery lasting more than one hour who were warmed with forced air. Independent associations between hypothermic exposure and transfusion requirement and duration of hospitalization were evaluated.
The results showed that 64% of surgical patients became hypothermic, with core temperatures below 36 °C during the first hour of anesthesia. Nearly half of the patients had a continuous core temperature less than 36 °C for more than one hour, and 20% of the patients had a continuous core temperature below 36 °C for more than two hours. Core temperatures then gradually increased, and most patients had normal temperatures by the end of surgery. The patients who became most hypothermic were most likely to need blood transfusions. The study was published in the February 2015 issue of Anesthesiology.
“Hypothermia is common during surgery because anesthetics disrupt normal control of body temperature and because operating rooms are kept cool,” said lead author Prof. Daniel Sessler, MD. “Consequently, body temperature typically decreases about four degrees Fahrenheit in unwarmed surgical patients. This sort of moderate hypothermia can cause serious complications including blood loss and wound infections.”
Forced-air warming utilizes the properties of convection and radiation to transfer heat from the movement of warm air across the surface of the patient’s skin. For more than 20 years, forced-air warming has been regarded as the standard of care to help prevent surgical site infections (SSIs) and other serious complications of unintended hypothermia, including increased blood loss, morbid myocardial events, and reduced resistance to surgical wound infections.
Related Links:
Cleveland Clinic
Chiang Mai University
Researchers at the Cleveland Clinic (OH, USA), Chiang Mai University (Thailand), and other institutions conducted a study to evaluate body temperature patterns in warmed surgical patients, and determine whether even short periods of low temperature increased blood loss or prolong hospital stays. The researchers measured intraoperative core body temperature patterns in 58,814 adults in surgery lasting more than one hour who were warmed with forced air. Independent associations between hypothermic exposure and transfusion requirement and duration of hospitalization were evaluated.
The results showed that 64% of surgical patients became hypothermic, with core temperatures below 36 °C during the first hour of anesthesia. Nearly half of the patients had a continuous core temperature less than 36 °C for more than one hour, and 20% of the patients had a continuous core temperature below 36 °C for more than two hours. Core temperatures then gradually increased, and most patients had normal temperatures by the end of surgery. The patients who became most hypothermic were most likely to need blood transfusions. The study was published in the February 2015 issue of Anesthesiology.
“Hypothermia is common during surgery because anesthetics disrupt normal control of body temperature and because operating rooms are kept cool,” said lead author Prof. Daniel Sessler, MD. “Consequently, body temperature typically decreases about four degrees Fahrenheit in unwarmed surgical patients. This sort of moderate hypothermia can cause serious complications including blood loss and wound infections.”
Forced-air warming utilizes the properties of convection and radiation to transfer heat from the movement of warm air across the surface of the patient’s skin. For more than 20 years, forced-air warming has been regarded as the standard of care to help prevent surgical site infections (SSIs) and other serious complications of unintended hypothermia, including increased blood loss, morbid myocardial events, and reduced resistance to surgical wound infections.
Related Links:
Cleveland Clinic
Chiang Mai University
Latest Surgical Techniques News
- Total Robotic Metabolic and Bariatric Surgery Proves More Beneficial than Conventional Laparoscopy
- Wirelessly Activated Robotic Device Aids Digestion in Patients with Compromised Organs

- Glowing Dye Helps Surgeons to Remove Hidden Prostate Cancer Cells in Real-Time
- Early Minimally Invasive Surgery Improves Intracerebral Hemorrhage Stroke Outcomes
- Early EVD Insertion Improves Surgical Outcome in Traumatic Brain Injury
- New Machine Learning Method Better Predicts Spine Surgery Outcomes
- New Research Platform Assesses Brain Cancer Mutations during Surgery
- Off-The-Shelf Surgical Device to Help Avoid Total Knee Replacement
- Study Warns Against Dangerous Smoke Levels Produced During Endoscopic Gastrointestinal Procedures
- New Hydrogel Sealant Effective at Sealing Dural Defects and Preventing Postoperative Adhesion
- MRI-Guided Multi-Stage Robotic Positioner Enhances Stereotactic Neurosurgery Precision

- AR Visualization System Improves Surgeons’ Capabilities and Spatial Awareness
- New Adhesive Hydrogel Coatings to Prolong Lifespan of Pacemakers and Medical Implants
- Maneuvering System Empowers Surgeons with Enhanced Control during Laparoscopic Procedures
- New Two-Dimensional Material Paves Way for Safer, More Effective Implantable Medical Devices
- Portable MRI Compatible Surgical Robot Improves Patients Outcomes for Neurosurgery
Channels
Critical Care
view channel.jpg)
GPS-Like Smart Pills with AI Provide Real-Time 3D Monitoring Of Gastrointestinal Health
Gas produced in the intestines when bacteria digest food can provide valuable information about a person's health. Currently, to measure gastrointestinal (GI) tract gases, physicians use methods such as... Read more
Soft Robots with Electronic Skins and Artificial Muscles to Provide Medical Treatment
Researchers have developed advanced soft robots that are equipped with electronic skins and artificial muscles, enabling them to detect their environment and modify their actions in real time.... Read morePatient Care
view channelFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read moreHealth IT
view channel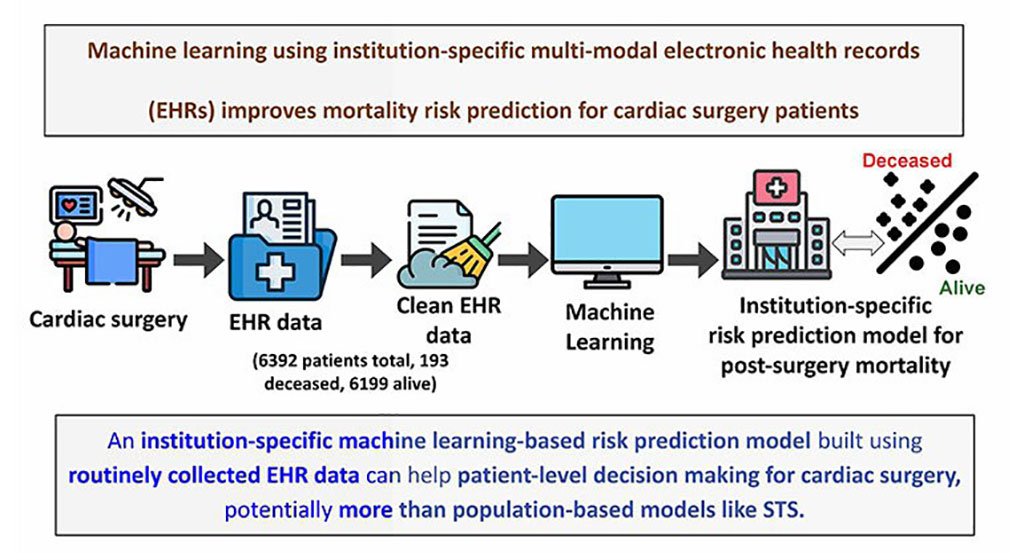
Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
Machine learning algorithms have been deployed to create predictive models in various medical fields, with some demonstrating improved outcomes compared to their standard-of-care counterparts.... Read more
Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
Top industry experts have underscored the immediate requirement for healthcare systems and hospitals to respond to severe cost and margin pressures. Close to half of U.S. hospitals ended 2022 in the red... Read more
AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
For healthcare organizations, optimizing operating room (OR) utilization during prime time hours is a complex challenge. Surgeons and clinics face difficulties in finding available slots for booking cases,... Read more
AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
Screening for common cancers like breast, cervix, and prostate cancer relies on relatively simple and highly effective techniques, such as mammograms, Pap smears, and blood tests. These methods have revolutionized... Read morePoint of Care
view channel
POCT for Infectious Diseases Delivers Laboratory Equivalent Pathology Results
On-site pathology tests for infectious diseases in rural and remote locations can achieve the same level of reliability and accuracy as those conducted in hospital laboratories, a recent study suggests.... Read more
Cartridge-Based Hemostasis Analyzer System Enables Faster Coagulation Testing
Quickly assessing a patient's total hemostasis status can be critical to influencing clinical outcomes and using blood products. Haemonetics Corporation (Boston, MA, USA) has now obtained 510(k) clearance... Read more
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read moreBusiness
view channel
BD Acquires Edwards Lifesciences' Critical Care Product Group for USD 4.2 Billion
BD (Becton, Dickinson and Company, Franklin Lakes, NJ, USA) and Edwards Lifesciences (Irvine, CA, USA) have entered into a definitive agreement under which BD will acquire Edwards' Critical Care product... Read more