Children's Hospitals Are Being Fined Unequally for Readmissions
|
By HospiMedica International staff writers Posted on 01 Mar 2016 |
A new study finds that pay-for-performance (P4P) measures might penalize hospitals treating children from deprived or ethnically backward minorities in an unequal way, due to factors beyond their control.
Researchers at the University of Colorado (Aurora, USA), the Children’s Hospital Association (Overland Park, KS, USA), and other institutions conducted a retrospective cohort study of 43 free-standing children’s hospitals within the Pediatric Health Information System database to determine whether risk adjustment for commonly available social determinants of health (SDH) affects the readmissions-based P4P penalty status of children’s hospitals in the United States.
The researchers examined hospital discharges from 2013 that met criteria for potentially preventable readmissions, and evaluated two risk-adjustment models. The first was a baseline model adjusted for severity of illness. The second was an SDH-enhanced model that adjusted for severity of illness and a set of four variables that included race, ethnicity, payer, and the median household income for the patient’s home zip code. The main outcome was the change in a hospital’s potentially preventable readmissions penalty status.
Data from 179,400 hospital discharges at the 43 hospitals showed that SDH variables were distributed per 39.2% nonwhite, 17.9% Hispanic, and 58.7% publicly insured; median household income for the patient’s home zip code was USD 40,674. When compared with the baseline model, adjustment for SDH resulted in a change in penalty status for three hospitals within the 15-day readmission window, and five hospitals within the 30-day window. The study was published on February 15, 2016, in JAMA Pediatrics.
“Studies like ours show that patients who are poorer or are minorities are readmitted at higher rates than other patients,” said lead author Marion Sills, MD, of the University of Colorado, “which raises concern that the readmissions penalties punish hospitals for the type of patients that they serve, rather than purely for the quality of care they provide.”
Medicare (Baltimore, MD, USA) launched the penalty program in 2012 in an attempt to combat a perverse financial incentive, wherein hospitals earned more money if patients were readmitted to health deterioration after they are discharged, because they can be paid for two stays instead of one. In 2013 Medicare levied fines of USD 227 million against 2,225 hospitals that had their payments reduced by up to 2% the following year.
Related Links:
University of Colorado
Children’s Hospital Association
Medicare
Researchers at the University of Colorado (Aurora, USA), the Children’s Hospital Association (Overland Park, KS, USA), and other institutions conducted a retrospective cohort study of 43 free-standing children’s hospitals within the Pediatric Health Information System database to determine whether risk adjustment for commonly available social determinants of health (SDH) affects the readmissions-based P4P penalty status of children’s hospitals in the United States.
The researchers examined hospital discharges from 2013 that met criteria for potentially preventable readmissions, and evaluated two risk-adjustment models. The first was a baseline model adjusted for severity of illness. The second was an SDH-enhanced model that adjusted for severity of illness and a set of four variables that included race, ethnicity, payer, and the median household income for the patient’s home zip code. The main outcome was the change in a hospital’s potentially preventable readmissions penalty status.
Data from 179,400 hospital discharges at the 43 hospitals showed that SDH variables were distributed per 39.2% nonwhite, 17.9% Hispanic, and 58.7% publicly insured; median household income for the patient’s home zip code was USD 40,674. When compared with the baseline model, adjustment for SDH resulted in a change in penalty status for three hospitals within the 15-day readmission window, and five hospitals within the 30-day window. The study was published on February 15, 2016, in JAMA Pediatrics.
“Studies like ours show that patients who are poorer or are minorities are readmitted at higher rates than other patients,” said lead author Marion Sills, MD, of the University of Colorado, “which raises concern that the readmissions penalties punish hospitals for the type of patients that they serve, rather than purely for the quality of care they provide.”
Medicare (Baltimore, MD, USA) launched the penalty program in 2012 in an attempt to combat a perverse financial incentive, wherein hospitals earned more money if patients were readmitted to health deterioration after they are discharged, because they can be paid for two stays instead of one. In 2013 Medicare levied fines of USD 227 million against 2,225 hospitals that had their payments reduced by up to 2% the following year.
Related Links:
University of Colorado
Children’s Hospital Association
Medicare
Latest Hospital News News
- Nurse Tracking System Improves Hospital Workflow
- New Children’s Hospital Transforms California Healthcare
- Noisy Hospitals Face Threat of Decreased Federal Compensation
- Orthopedics Centre of Excellence Planned for Guy’s Hospital
- Research Suggests Avoidance of Low-Value Surgical Procedures
- U.S. Federal Readmission Fines Linked to Higher Mortality
- Columbia China to Build New Hospital in Jiaxing
- Dubai Debuts Second Robotic Pharmacy Service
- Seattle Hospital Network Shifts Away from Overlapping Surgeries
- ACC to Launch Valvular Heart Disease Program in China
- Mortality Rates Lower at Major Teaching Hospitals
- South Australia to Inaugurate Upscale Hospital
- Raffles to Launch Second Hospital Project in China
- Research Center Tackles Antimicrobial Drugs Challenge
- Miami Cardiac & Vascular Institute Completes Expansion Project
- Hospital Antibiotic Policies Improve Prescription Practices
Channels
Artificial Intelligence
view channelFacial Image Analysis Tracks Biological Aging, Predicts Cancer Outcomes
Biological aging is the progressive loss of physiological function that may diverge from chronological age. In cancer care, clinicians need simple tools that reflect dynamic changes in patient resilience... Read more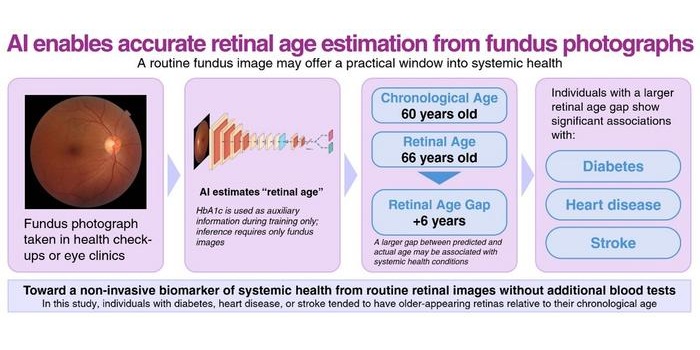
AI Model Uses Eye Imaging to Identify Risk of Major Systemic Diseases
Early detection of systemic disease risk remains a persistent challenge in population health screening. Cardiometabolic conditions such as diabetes, heart disease, and stroke often progress without symptoms... Read moreCritical Care
view channel
AI-Enhanced ECG Screens for Heart Failure Risk in Resource-Limited Settings
Heart failure, a chronic condition in which the heart cannot pump enough blood to meet the body’s needs, is increasing worldwide. In sub-Saharan Africa, patients often develop the disease at younger ages... Read more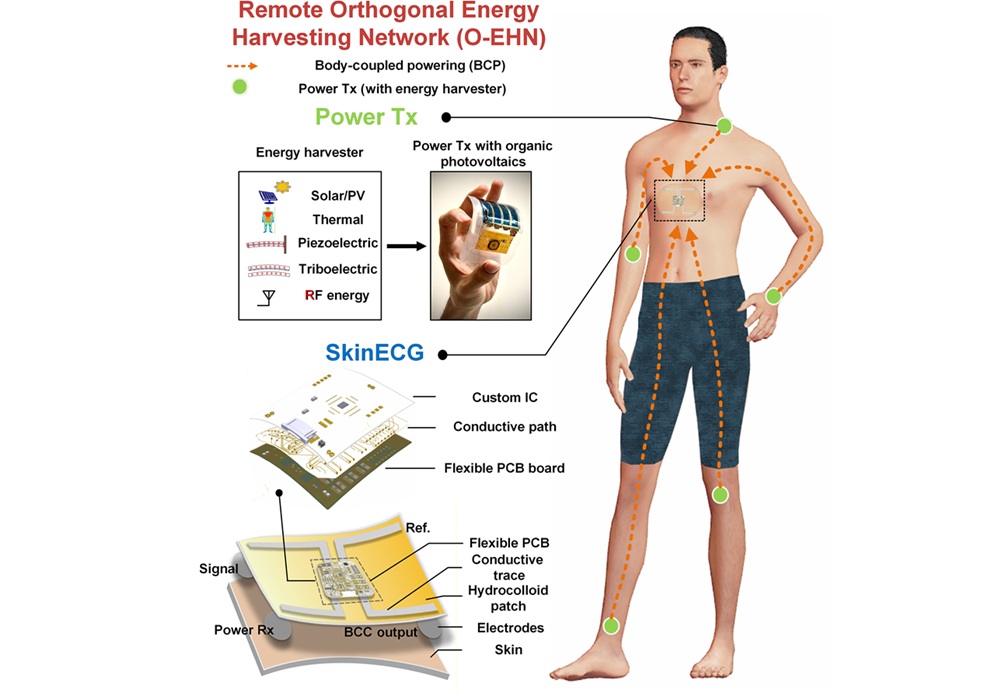
Battery-Free ECG Patch Enables Continuous Arrhythmia Monitoring
Continuous electrocardiogram (ECG) monitoring supports early detection of arrhythmias and enables timely intervention, yet many wearables depend on bulky batteries that interrupt care when depleted.... Read moreSurgical Techniques
view channel
Smart Soft Sensors Provide Real-Time Force Feedback in Minimally Invasive Surgery
Minimally invasive surgery reduces recovery time and postoperative pain but limits tactile feedback for surgeons. Loss of force perception can increase the risk of tissue injury and complicate delicate... Read more
Ultrasonic Fine-Needle Biopsy Tool Improves Salivary Gland Tumor Diagnosis
Accurate tissue sampling is central to cancer work-ups, yet fine-needle aspiration often yields too little material for a reliable diagnosis in head and neck lesions. Core needle biopsy can recover tissue... Read more
Patient-Specific 3D-Printed Guide Improves Precision in Breast-Conserving Surgery
Achieving clear margins during breast-conserving surgery remains challenging, especially when poorly defined tumor edges lead to repeat operations. Positive margins occur in about 20% of cases and in 30–40%... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EHR-Integrated Screening Workflow Detects Cognitive Impairment at Admission
Cognitive impairment involves difficulties with thinking, learning, memory, and decision-making, and is more common in older adults. In U.S. hospitals, more than 40% of admitted older adults have dementia,... Read more
AI System Detects and Quantifies Chronic Subdural Hematoma
Viz.ai (San Francisco, CA, USA) announced a strategic commercialization collaboration with Johnson & Johnson (New Brunswick, NJ, USA) to expand access in the United States to the Viz Subdural solution... Read more
Continuous Monitoring Platform Detects Infection Risk Across Care Transitions
Patients leaving skilled nursing facilities often lose continuous physiologic monitoring, increasing the risk of undetected infection and delayed intervention. Nursing home residents are seven times more... Read more
Automated System Classifies and Tracks Cardiogenic Shock Across Hospital Settings
Cardiogenic shock remains a difficult, time-sensitive emergency, with delayed identification driving poor outcomes and persistently high mortality. Many cases go undocumented even at advanced stages, hindering... Read morePoint of Care
view channel
Point-of-Care Viscoelastic Testing System Supports Obstetric Bleeding Management
HemoSonics (Durham, NC, USA) announced on May 5, 2026 that the company's Quantra Hemostasis System for Obstetric Procedures won Silver in the 2026 Edison Awards in the Women’s Health and Reproductive Innovations... Read moreBusiness
view channel
Olympus Partnership Aims to Expand Access to Robot-Assisted Endoscopic Therapy
Olympus has signed an exclusive global distribution agreement with EndoRobotics Co., Ltd., under which robot-assisted technologies developed by EndoRobotics will be distributed worldwide as part of the... Read more