Operating Room Waste Incurs Heavy Financial Burden
|
By HospiMedica International staff writers Posted on 19 Sep 2016 |
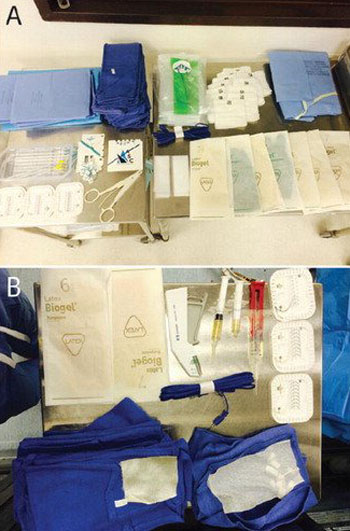
Image: Two images of wasted surgical supplies after a UCSF neurosurgery procedure (Photo courtesy of Christopher Moriates/ UCSF).
A new study reveals that on average, almost USD 1,000 of disposable operating room (OR) supplies go unused, and are discarded after surgery.
Researchers at the University of California, San Francisco (UCSF; USA) and Brown University (Providence, RI, USA) conducted a study to quantify the utilization of disposable supplies and the costs associated with opened (but unused) items in 58 neurosurgical procedures (36 cranial, 22 spinal) completed at the UCSF Medical Center by 14 different surgeons. Every wasted disposable supply was quantified in USD, as determined from the supply catalog, and statistical analyses were performed.
The results revealed that the average cost of unused supplies was USD 653, or 13.1% of the total surgical supply cost. Case type (cranial versus spinal), case category (vascular, tumor, functional, instrumented, and noninstrumented spine), and surgeon were important predictors of the percentage of unused surgical supply cost. Conversely, case length and years of surgical training had no effect. Among the most discarded supplies were sponges, blue towels, and gloves. The most expensive item wasted was surgifoam, a sponge used to stop bleeding, which can cost close to USD 4,000 each.
When taking into consideration case distribution, the authors estimate approximately USD 968 per case, or USD 2.9 million per year of OR waste is generated in the UCSF neurosurgical department alone. They therefore recommend price transparency, education about OR waste to surgeons and nurses, preference card reviews for each surgeon, and clarification of supplies that should be opened, versus available as needed, all in order to reduce waste. The study was published on May 6, 2016, in the Journal of Neurosurgery.
“Operating rooms in the U.S. produce more than 2,000 tons of waste per day; some of it is biological and must be safely disposed of,” said co-lead author Seungwon Yoon, of Brown University. “Part of the research involved identifying which surgeries generated the most waste. Spinal procedures, for example, are among the most wasteful. There is little agreement on how hospitals should address operating room wastefulness; each hospital or hospital system handles waste in its own way.”
“All three of UCSF’s hospitals have been working to reduce waste. Some medical devices, whether used or unused during surgery, can be reprocessed by an FDA-approved third party company and sold back to the hospital for about half the original sales price,” commented Gail Lee, director of sustainability for UCSF hospitals and campus. “This allows hospitals to save money and cut down on the volume of disposable supplies that end up in landfill. This strategy saved UCSF hospitals about USD 1.1 million over the past year.”
Related Links:
University of California, San Francisco
Brown University
Researchers at the University of California, San Francisco (UCSF; USA) and Brown University (Providence, RI, USA) conducted a study to quantify the utilization of disposable supplies and the costs associated with opened (but unused) items in 58 neurosurgical procedures (36 cranial, 22 spinal) completed at the UCSF Medical Center by 14 different surgeons. Every wasted disposable supply was quantified in USD, as determined from the supply catalog, and statistical analyses were performed.
The results revealed that the average cost of unused supplies was USD 653, or 13.1% of the total surgical supply cost. Case type (cranial versus spinal), case category (vascular, tumor, functional, instrumented, and noninstrumented spine), and surgeon were important predictors of the percentage of unused surgical supply cost. Conversely, case length and years of surgical training had no effect. Among the most discarded supplies were sponges, blue towels, and gloves. The most expensive item wasted was surgifoam, a sponge used to stop bleeding, which can cost close to USD 4,000 each.
When taking into consideration case distribution, the authors estimate approximately USD 968 per case, or USD 2.9 million per year of OR waste is generated in the UCSF neurosurgical department alone. They therefore recommend price transparency, education about OR waste to surgeons and nurses, preference card reviews for each surgeon, and clarification of supplies that should be opened, versus available as needed, all in order to reduce waste. The study was published on May 6, 2016, in the Journal of Neurosurgery.
“Operating rooms in the U.S. produce more than 2,000 tons of waste per day; some of it is biological and must be safely disposed of,” said co-lead author Seungwon Yoon, of Brown University. “Part of the research involved identifying which surgeries generated the most waste. Spinal procedures, for example, are among the most wasteful. There is little agreement on how hospitals should address operating room wastefulness; each hospital or hospital system handles waste in its own way.”
“All three of UCSF’s hospitals have been working to reduce waste. Some medical devices, whether used or unused during surgery, can be reprocessed by an FDA-approved third party company and sold back to the hospital for about half the original sales price,” commented Gail Lee, director of sustainability for UCSF hospitals and campus. “This allows hospitals to save money and cut down on the volume of disposable supplies that end up in landfill. This strategy saved UCSF hospitals about USD 1.1 million over the past year.”
Related Links:
University of California, San Francisco
Brown University
Latest Hospital News News
- Nurse Tracking System Improves Hospital Workflow
- New Children’s Hospital Transforms California Healthcare
- Noisy Hospitals Face Threat of Decreased Federal Compensation
- Orthopedics Centre of Excellence Planned for Guy’s Hospital
- Research Suggests Avoidance of Low-Value Surgical Procedures
- U.S. Federal Readmission Fines Linked to Higher Mortality
- Columbia China to Build New Hospital in Jiaxing
- Dubai Debuts Second Robotic Pharmacy Service
- Seattle Hospital Network Shifts Away from Overlapping Surgeries
- ACC to Launch Valvular Heart Disease Program in China
- Mortality Rates Lower at Major Teaching Hospitals
- South Australia to Inaugurate Upscale Hospital
- Raffles to Launch Second Hospital Project in China
- Research Center Tackles Antimicrobial Drugs Challenge
- Miami Cardiac & Vascular Institute Completes Expansion Project
- Hospital Antibiotic Policies Improve Prescription Practices
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read more
Automated IV Labeling Solution Improves Infusion Safety and Efficiency
Medication administration in high-acuity settings is often complicated by multiple concurrent infusions, making accurate line identification essential. In a 10-hospital intensive care unit study, 60% of... Read moreSurgical Techniques
view channel
Ultrasound Technology Aims to Replace Invasive BPH Procedures
Benign prostatic hyperplasia (BPH) is a frequent cause of lower urinary tract symptoms in aging men and often requires invasive procedures or prolonged recovery. With prevalence expected to rise as populations... Read more
Continuous Monitoring with Wearables Enhances Postoperative Patient Safety
Postoperative hypoxemia on general surgical wards is common and often missed by intermittent vital sign checks. Undetected low oxygen levels can delay recovery and raise the risk of complications that... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel