New Children’s Hospital Transforms California Healthcare
|
By HospiMedica International staff writers Posted on 02 Jan 2018 |

Image: The new Lucile Packard Children’s Hospital main building (Photo courtesy of Stanford Health).
The new Lucile Packard Children’s Hospital (Palo Alto, CA, USA) expansion is set to transform the patient experience through a family-centered design and technological innovation, while setting new standards for sustainability in hospital design.
Nearly a decade in the making, the new pediatric and obstetric hospital campus will more than double the size of the existing campus by linking the original hospital (now called the West building) with the new Main building, bringing the total hospital space to measure 78,410 m2. The new Main building adds 149 patient beds, for a total of 361 beds in the Palo Alto campus, thus enabling the hospital to serve more patients than ever before, and permitting management to deploy awaited renovation plans for the existing hospital building.
With 13 surgical suites, the new hospital will have more operating rooms than any other children’s hospital in Northern California, reducing scheduling delays and long waits when surgeries take longer than planned. A neuro-hybrid surgery suite will feature a state-of-the-art diagnostic MRI, direct access to angiography imaging equipment, and a full operating room that will enable surgeons to view updated images during surgery and reimage patients before closure of the surgical incision, reducing the amount of time a young patient will spend under anesthesia.
A new imaging center features the only PET/MRI exclusively dedicated to pediatric patients in Northern California, which will shorten the time of imaging studies and significantly decreases the radiation dose delivered to the patient by close to 80%. The imaging center is part of a larger treatment center that encompasses surgery, radiology, imaging, interventional suites and catheterization labs, and a dedicated isotope radiation therapy room for nuclear medicine. Both the surgical suites and neuro-interventional and catheterization labs are still under construction, and are slated to open mid-year 2018.
“This will be the nation’s most technologically advanced, environmentally sustainable, and family-friendly hospital for children and expectant mothers,” said Christopher Dawes, CEO of Stanford Children’s Heath. “In our 25 years, we’ve become leaders in providing the best care for children and expectant mothers. Keeping pace with the growing needs of our patients was the catalyst for this transformation. We’ll continue to build world-renowned programs as part of Stanford Medicine and advance research in every pediatric and obstetric specialty.”
“When my mother founded this hospital, she envisioned a place where children and families could receive truly healing care,” said Susan Packard Orr. “She saw the power that nature had to heal and uplift. I’m proud that we have carried her vision forward, with world-class sustainability and holistic elements throughout the new hospital. Everything we do at this hospital will have an eye to ensuring that generations to come will be healthier.”
The new building will also allow for a transformative renovation of much of the existing hospital’s space, including the Johnson Center for Pregnancy and Newborn Services into mostly private obstetrics rooms. Some major programs will grow and transition into the new Main building, including the Bass Center for Childhood Cancer and Blood Diseases, the Pediatric Transplant Center, and the Betty Irene Moore Children’s Heart Center.
Related Links:
Lucile Packard Children’s Hospital
Nearly a decade in the making, the new pediatric and obstetric hospital campus will more than double the size of the existing campus by linking the original hospital (now called the West building) with the new Main building, bringing the total hospital space to measure 78,410 m2. The new Main building adds 149 patient beds, for a total of 361 beds in the Palo Alto campus, thus enabling the hospital to serve more patients than ever before, and permitting management to deploy awaited renovation plans for the existing hospital building.
With 13 surgical suites, the new hospital will have more operating rooms than any other children’s hospital in Northern California, reducing scheduling delays and long waits when surgeries take longer than planned. A neuro-hybrid surgery suite will feature a state-of-the-art diagnostic MRI, direct access to angiography imaging equipment, and a full operating room that will enable surgeons to view updated images during surgery and reimage patients before closure of the surgical incision, reducing the amount of time a young patient will spend under anesthesia.
A new imaging center features the only PET/MRI exclusively dedicated to pediatric patients in Northern California, which will shorten the time of imaging studies and significantly decreases the radiation dose delivered to the patient by close to 80%. The imaging center is part of a larger treatment center that encompasses surgery, radiology, imaging, interventional suites and catheterization labs, and a dedicated isotope radiation therapy room for nuclear medicine. Both the surgical suites and neuro-interventional and catheterization labs are still under construction, and are slated to open mid-year 2018.
“This will be the nation’s most technologically advanced, environmentally sustainable, and family-friendly hospital for children and expectant mothers,” said Christopher Dawes, CEO of Stanford Children’s Heath. “In our 25 years, we’ve become leaders in providing the best care for children and expectant mothers. Keeping pace with the growing needs of our patients was the catalyst for this transformation. We’ll continue to build world-renowned programs as part of Stanford Medicine and advance research in every pediatric and obstetric specialty.”
“When my mother founded this hospital, she envisioned a place where children and families could receive truly healing care,” said Susan Packard Orr. “She saw the power that nature had to heal and uplift. I’m proud that we have carried her vision forward, with world-class sustainability and holistic elements throughout the new hospital. Everything we do at this hospital will have an eye to ensuring that generations to come will be healthier.”
The new building will also allow for a transformative renovation of much of the existing hospital’s space, including the Johnson Center for Pregnancy and Newborn Services into mostly private obstetrics rooms. Some major programs will grow and transition into the new Main building, including the Bass Center for Childhood Cancer and Blood Diseases, the Pediatric Transplant Center, and the Betty Irene Moore Children’s Heart Center.
Related Links:
Lucile Packard Children’s Hospital
Latest Hospital News News
- Nurse Tracking System Improves Hospital Workflow
- Noisy Hospitals Face Threat of Decreased Federal Compensation
- Orthopedics Centre of Excellence Planned for Guy’s Hospital
- Research Suggests Avoidance of Low-Value Surgical Procedures
- U.S. Federal Readmission Fines Linked to Higher Mortality
- Columbia China to Build New Hospital in Jiaxing
- Dubai Debuts Second Robotic Pharmacy Service
- Seattle Hospital Network Shifts Away from Overlapping Surgeries
- ACC to Launch Valvular Heart Disease Program in China
- Mortality Rates Lower at Major Teaching Hospitals
- South Australia to Inaugurate Upscale Hospital
- Raffles to Launch Second Hospital Project in China
- Research Center Tackles Antimicrobial Drugs Challenge
- Miami Cardiac & Vascular Institute Completes Expansion Project
- Hospital Antibiotic Policies Improve Prescription Practices
- USC Virtual Care Clinic to Employ Avatar Doctors
Channels
Artificial Intelligence
view channelAI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
Accurately identifying long-term cardiovascular disease risk in asymptomatic adults remains challenging for clinicians. Missed or underestimated risk delays preventive therapy and increases the chance... Read more
Machine Learning Approach Enhances Liver Cancer Risk Stratification
Hepatocellular carcinoma, the most common form of primary liver cancer, is often detected late despite targeted surveillance programs. Current screening guidelines emphasize patients with known cirrhosis,... Read moreCritical Care
view channel
Eye Imaging AI Identifies Elevated Cardiovascular Risk
Many adults at risk for atherosclerotic cardiovascular disease are not identified until they undergo formal primary care assessment. Delayed risk recognition can postpone initiation of statins and lifestyle... Read more
Noninvasive Monitoring Device Enables Earlier Intervention in Heart Failure
Hospitalizations for heart failure with preserved ejection fraction (HFpEF) remain common because lung congestion often worsens before symptoms prompt treatment changes. Missed early decompensation... Read moreSurgical Techniques
view channel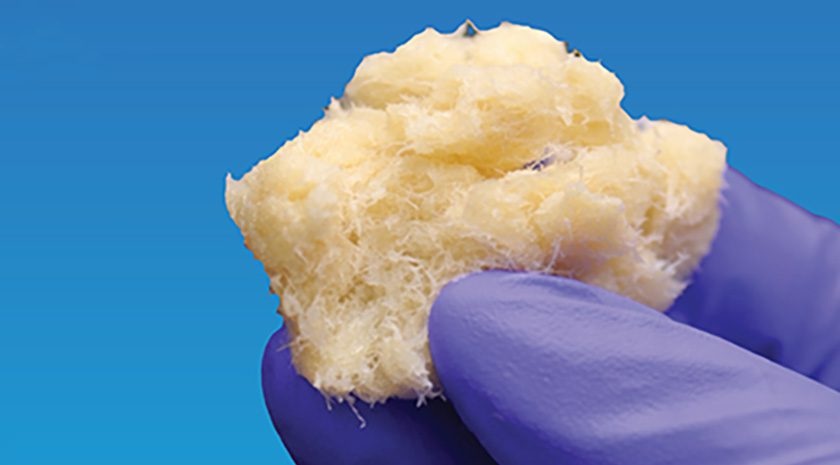
Fiber-Form Bone Graft Expands Intraoperative Options for Spinal Fusion
Spinal and orthopedic fusion procedures often require bone graft materials that handle predictably and support bone formation. Surgeons face added complexity in difficult anatomy and challenging fusion environments.... Read more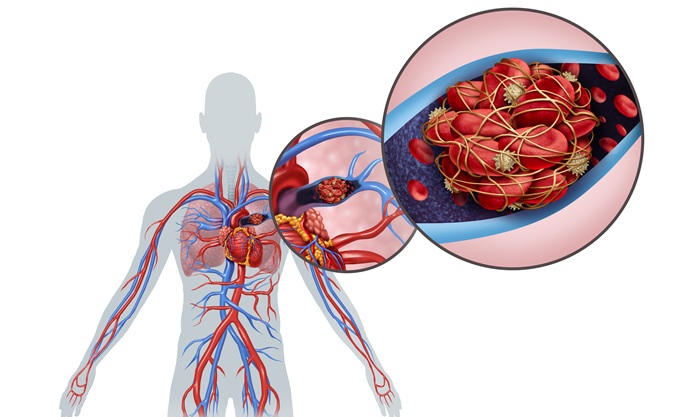
Ultrasound‑Aided Catheter Treatment Cuts Early Collapse in Pulmonary Embolism
Acute pulmonary embolism can cause rapid hemodynamic deterioration and early death in hospitalized and emergency patients. Systemic thrombolysis can dissolve clots but is limited by a high risk of major... Read morePatient Care
view channel
Wearable Sleep Data Predict Adherence to Pulmonary Rehabilitation
Chronic obstructive pulmonary disease (COPD) is a long-term lung disorder that makes breathing difficult and often disturbs sleep, reducing energy for daily activities. Limited engagement in pulmonary... Read more
Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
More than 80% of in-hospital patients receive intravenous (IV) therapy. Every dose of IV medicine delivered in a small volume (<250 mL) infusion bag should be followed by subsequent flushing to ensure... Read moreHealth IT
view channel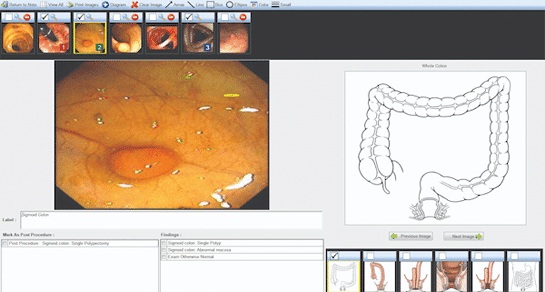
Voice-Driven AI System Enables Structured GI Procedure Documentation
Documentation during gastrointestinal (GI) procedures often competes with real-time clinical decision-making and imposes a significant cognitive burden on physicians. Manual data entry and post-procedure... Read more
EMR-Based Tool Predicts Graft Failure After Kidney Transplant
Kidney transplantation offers patients with end-stage kidney disease longer survival and better quality of life than dialysis, yet graft failure remains a major challenge. Although a successful transplant... Read more
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read moreBusiness
view channel





















