Patients Who Survive COVID-19 May Have Long-Term Brain Deficits
|
By HospiMedica International staff writers Posted on 05 Jun 2020 |

Illustration
To date, the focus on COVID-19 patients has been more on keeping them alive and less on examining the impact the disease on their long-term health, although neurological issues in patients who suffer from COVID-19 call for better assessments to shape treatments.
Dr. Majid Fotuhi, MD, PhD, a Harvard- and Johns Hopkins-trained neurologist and neuroscientist, has warned about neurological issues in patients who suffer from COVID-19 and is encouraging more study of the neurological effects of the disease to promote better treatments.
According to Fotuhi, medical director of NeuroGrow Brain Fitness Center, COVID-19’s neurological manifestation can be grouped into three stages. In NeuroCovid Stage I, the virus damage is limited to epithelial cells of nose and mouth. In NeuroCovid Stage II, patients may experience blood clots in their brain or have auto-antibodies that damage their peripheral nerves and muscles. In this stage, the virus can trigger a flood of inflammatory markers, called cytokine storm, which begin in the lungs and travel throughout all body organs. This may lead to blood clots resulting in a series of strokes that can kill neurons. In NeuroCovid Stage III, the blood brain barrier, a protective insulation in blood vessels of the brain, is damaged and patients may develop seizures or encephalopathy. In this rare late stage, the virus particles themselves may invade the brain directly, including the brain region that controls breathing.
Fotuhi has pointed out that many patients with COVID-19 may have no noticeable neurological symptoms at first; but in some cases, patients may present with neurological symptoms even before they have fever, cough, or shortness of breath. He stresses that having an MRI while at the hospital will be an important tool in developing an optimal treatment strategy for these patients. In addition, patients will need to be monitored in a few months after their hospitalization as they may have new symptoms not experienced early in their disease process.
“Our experience with other forms of respiratory viruses that affect the brain suggest that in the long-term patients may develop depression, insomnia, Parkinson’s disease, memory loss, or accelerated aging in the brain,” said Fotuhi.
Dr. Majid Fotuhi, MD, PhD, a Harvard- and Johns Hopkins-trained neurologist and neuroscientist, has warned about neurological issues in patients who suffer from COVID-19 and is encouraging more study of the neurological effects of the disease to promote better treatments.
According to Fotuhi, medical director of NeuroGrow Brain Fitness Center, COVID-19’s neurological manifestation can be grouped into three stages. In NeuroCovid Stage I, the virus damage is limited to epithelial cells of nose and mouth. In NeuroCovid Stage II, patients may experience blood clots in their brain or have auto-antibodies that damage their peripheral nerves and muscles. In this stage, the virus can trigger a flood of inflammatory markers, called cytokine storm, which begin in the lungs and travel throughout all body organs. This may lead to blood clots resulting in a series of strokes that can kill neurons. In NeuroCovid Stage III, the blood brain barrier, a protective insulation in blood vessels of the brain, is damaged and patients may develop seizures or encephalopathy. In this rare late stage, the virus particles themselves may invade the brain directly, including the brain region that controls breathing.
Fotuhi has pointed out that many patients with COVID-19 may have no noticeable neurological symptoms at first; but in some cases, patients may present with neurological symptoms even before they have fever, cough, or shortness of breath. He stresses that having an MRI while at the hospital will be an important tool in developing an optimal treatment strategy for these patients. In addition, patients will need to be monitored in a few months after their hospitalization as they may have new symptoms not experienced early in their disease process.
“Our experience with other forms of respiratory viruses that affect the brain suggest that in the long-term patients may develop depression, insomnia, Parkinson’s disease, memory loss, or accelerated aging in the brain,” said Fotuhi.
Latest COVID-19 News
- Low-Cost System Detects SARS-CoV-2 Virus in Hospital Air Using High-Tech Bubbles
- World's First Inhalable COVID-19 Vaccine Approved in China
- COVID-19 Vaccine Patch Fights SARS-CoV-2 Variants Better than Needles
- Blood Viscosity Testing Can Predict Risk of Death in Hospitalized COVID-19 Patients
- ‘Covid Computer’ Uses AI to Detect COVID-19 from Chest CT Scans
- MRI Lung-Imaging Technique Shows Cause of Long-COVID Symptoms
- Chest CT Scans of COVID-19 Patients Could Help Distinguish Between SARS-CoV-2 Variants
- Specialized MRI Detects Lung Abnormalities in Non-Hospitalized Long COVID Patients
- AI Algorithm Identifies Hospitalized Patients at Highest Risk of Dying From COVID-19
- Sweat Sensor Detects Key Biomarkers That Provide Early Warning of COVID-19 and Flu
- Study Assesses Impact of COVID-19 on Ventilation/Perfusion Scintigraphy
- CT Imaging Study Finds Vaccination Reduces Risk of COVID-19 Associated Pulmonary Embolism
- Third Day in Hospital a ‘Tipping Point’ in Severity of COVID-19 Pneumonia
- Longer Interval Between COVID-19 Vaccines Generates Up to Nine Times as Many Antibodies
- AI Model for Monitoring COVID-19 Predicts Mortality Within First 30 Days of Admission
- AI Predicts COVID Prognosis at Near-Expert Level Based Off CT Scans
Channels
Artificial Intelligence
view channel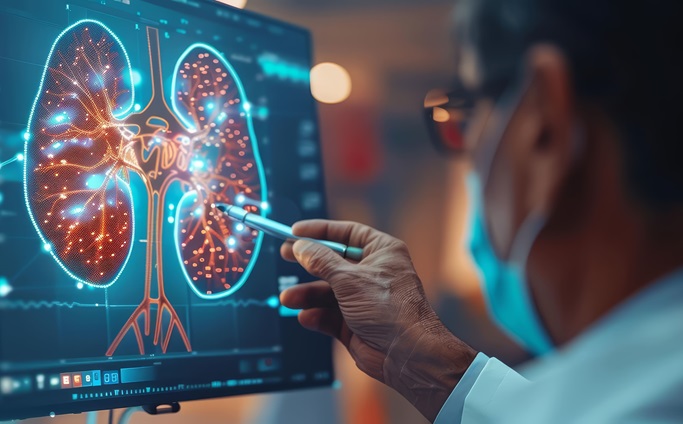
Innovative Risk Score Predicts Heart Attack or Stroke in Kidney Transplant Candidates
Heart researchers have utilized an innovative risk assessment score to accurately predict whether patients being evaluated for kidney transplants are at risk for future major cardiac events, such as a... Read more
AI Algorithm Detects Early-Stage Metabolic-Associated Steatotic Liver Disease Using EHRs
Liver disease, which is treatable when detected early, often goes unnoticed until it reaches advanced stages. Metabolic-associated steatotic liver disease (MASLD), the most prevalent form of liver disease,... Read moreCritical Care
view channel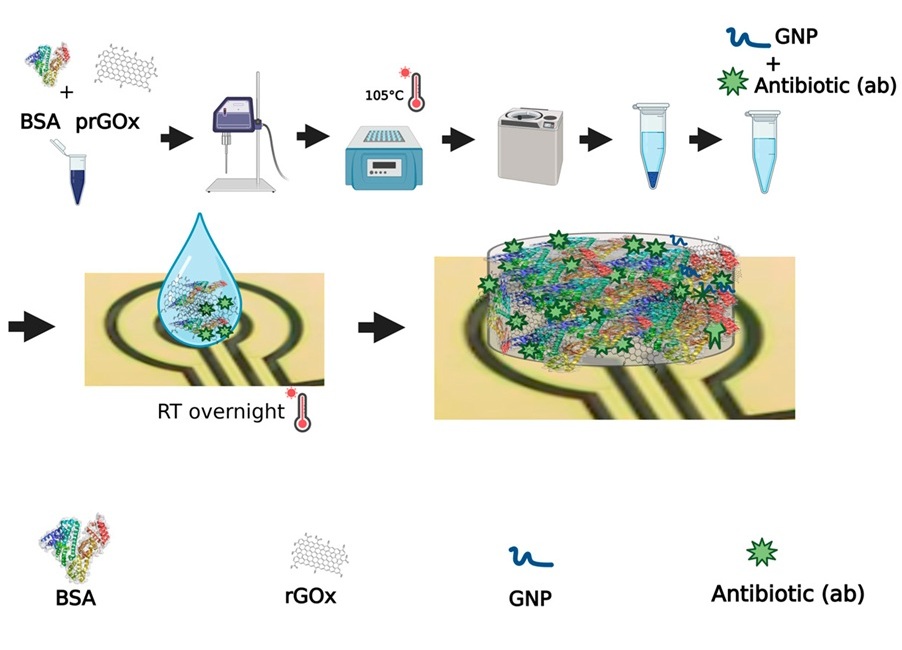
Novel Coating Significantly Extends Longevity of Implantable Biosensors
Wearable and implantable biosensors capable of accurately detecting biological molecules in a non-invasive or minimally invasive way offer enormous potential for monitoring patients’ health and their responses... Read more
Nanogel-Based Drug Delivery Technology to Improve UTI Treatment
Urinary tract infections (UTIs) are not only widespread and costly but also highly debilitating, significantly impacting the quality of life for those affected. The antibiotics commonly used to treat UTIs... Read more
New IV Pole Improves Safety and Ease of Administering IV Medications at Hospital Bedside
Preventable medication errors affect around 500,000 hospitalized patients in the U.S. every year. A significant portion of these errors occur with intravenous (IV) smart pumps, which require a precise... Read moreSurgical Techniques
view channel
Easy-To-Apply Gel Could Prevent Formation of Post-Surgical Abdominal Adhesions
Surgical adhesions are a frequent and often life-threatening complication following open or laparoscopic abdominal surgery. These adhesions develop in the weeks following surgery as the body heals.... Read more
Groundbreaking Leadless Pacemaker to Prevent Invasive Surgeries for Children
Leadless pacemakers marked a significant advancement in cardiac care, primarily because traditional pacemakers are dependent on leads, which are prone to breakage over time. Currently, two FDA-approved... Read morePatient Care
view channel
Portable Biosensor Platform to Reduce Hospital-Acquired Infections
Approximately 4 million patients in the European Union acquire healthcare-associated infections (HAIs) or nosocomial infections each year, with around 37,000 deaths directly resulting from these infections,... Read moreFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read moreHealth IT
view channel
Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
The future of medicine is likely to focus on the personalization of healthcare—understanding exactly what an individual requires and delivering the appropriate combination of nutrients, metabolites, and... Read more
Smartwatches Could Detect Congestive Heart Failure
Diagnosing congestive heart failure (CHF) typically requires expensive and time-consuming imaging techniques like echocardiography, also known as cardiac ultrasound. Previously, detecting CHF by analyzing... Read morePoint of Care
view channel
Handheld, Sound-Based Diagnostic System Delivers Bedside Blood Test Results in An Hour
Patients who go to a doctor for a blood test often have to contend with a needle and syringe, followed by a long wait—sometimes hours or even days—for lab results. Scientists have been working hard to... Read more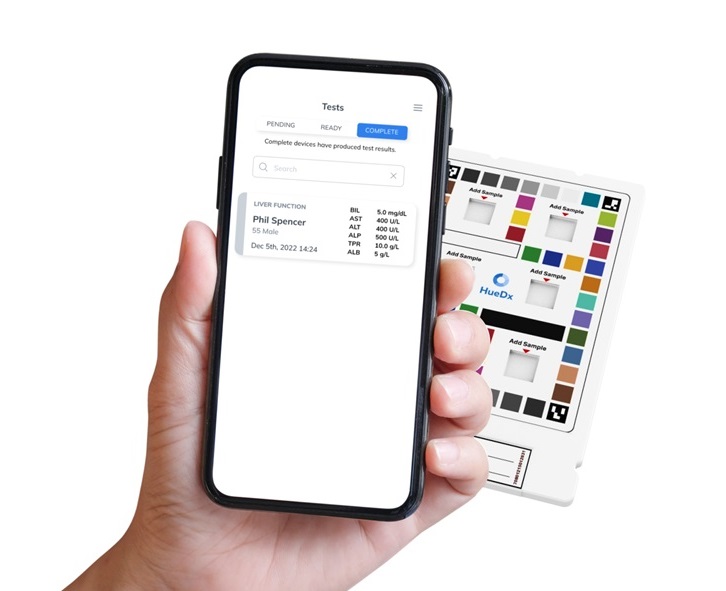
Smartphone-Enabled, Paper-Based Quantitative Diagnostic Platform Transforms POC Testing
Point-of-care diagnostics are crucial for public health, offering rapid, on-site testing that enables prompt diagnosis and treatment. This is especially valuable in remote or underserved regions where... Read moreBusiness
view channel
Becton Dickinson to Spin Out Biosciences and Diagnostic Solutions Business
Becton, Dickinson and Company (BD, Franklin Lakes, NJ, USA), has announced that its board of directors has unanimously authorized BD management to pursue a plan to separate BD's Biosciences and Diagnostic... Read more