Digital Health Interventions Reduce Risk of Cardiovascular Disease
|
By HospiMedica International staff writers Posted on 18 May 2015 |
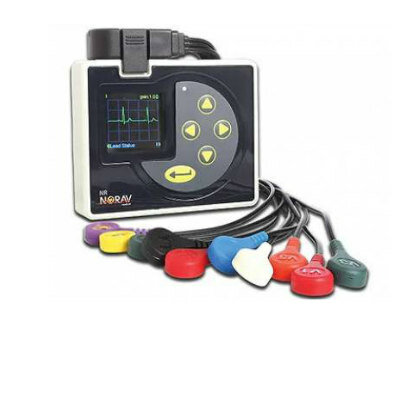
Digital health interventions (DHIs), such as telemedicine and text message reminders, reduce the relative risk of cardiovascular disease (CVD) by 40%, according to a new study.
Researchers at the Mayo Clinic (Rochester, MN, USA) conducted a systematic search of PubMed, MEDLINE, EMBASE, the Cochrane Central Register of Controlled Trials, and other sources for articles that examined elements of DHI and CVD outcomes or risk factors. The authors extracted CVD outcomes and data on risk factors for CVD such as weight, body mass index (BMI), blood pressure (BP), and lipid levels from 51 full-text articles that met validity and inclusion criteria.
The results showed that DHI significantly reduced CVD outcomes. Web-based strategies, email, mobile phones, mobile applications, text messaging, and monitoring sensors reduced the absolute risk of CVD by about 7%, more than use of statins, aspirin, or anti-hypertension drugs. Concomitant reductions were seen in weight and BMI, but not blood pressure. They found that some DHIs are more effective than others, with internet-based modalities, text messages, and telemedicine lowering risk more than emails and data monitoring. The study was published in the April 2015 issue of Mayo Clinic Proceedings.
“Because DHI use does not directly reduce CVD risk, these observed benefits likely reflect increased adherence to evidence-based preventive therapies such as statins, aspirin, or β-blockers,” concluded lead author R. Jay Widmer, MD, PhD, and colleagues of the division of cardiovascular diseases. “DHIs tend to trigger behavioral changes, while drugs treat the condition directly. A combination of the two could be optimal.”
“With nearly 50,000 health care–related apps now available for download and numerous internet-based digital health intervention solutions available, the benefit of digital health interventions on cardiovascular disease prevention and outcomes, both primary and secondary, merits reexamination,” suggested the authors.
Related Links:
Mayo Clinic
Researchers at the Mayo Clinic (Rochester, MN, USA) conducted a systematic search of PubMed, MEDLINE, EMBASE, the Cochrane Central Register of Controlled Trials, and other sources for articles that examined elements of DHI and CVD outcomes or risk factors. The authors extracted CVD outcomes and data on risk factors for CVD such as weight, body mass index (BMI), blood pressure (BP), and lipid levels from 51 full-text articles that met validity and inclusion criteria.
The results showed that DHI significantly reduced CVD outcomes. Web-based strategies, email, mobile phones, mobile applications, text messaging, and monitoring sensors reduced the absolute risk of CVD by about 7%, more than use of statins, aspirin, or anti-hypertension drugs. Concomitant reductions were seen in weight and BMI, but not blood pressure. They found that some DHIs are more effective than others, with internet-based modalities, text messages, and telemedicine lowering risk more than emails and data monitoring. The study was published in the April 2015 issue of Mayo Clinic Proceedings.
“Because DHI use does not directly reduce CVD risk, these observed benefits likely reflect increased adherence to evidence-based preventive therapies such as statins, aspirin, or β-blockers,” concluded lead author R. Jay Widmer, MD, PhD, and colleagues of the division of cardiovascular diseases. “DHIs tend to trigger behavioral changes, while drugs treat the condition directly. A combination of the two could be optimal.”
“With nearly 50,000 health care–related apps now available for download and numerous internet-based digital health intervention solutions available, the benefit of digital health interventions on cardiovascular disease prevention and outcomes, both primary and secondary, merits reexamination,” suggested the authors.
Related Links:
Mayo Clinic
Latest Health IT News
- Machine Learning Model Improves Mortality Risk Prediction for Cardiac Surgery Patients
- Strategic Collaboration to Develop and Integrate Generative AI into Healthcare
- AI-Enabled Operating Rooms Solution Helps Hospitals Maximize Utilization and Unlock Capacity
- AI Predicts Pancreatic Cancer Three Years before Diagnosis from Patients’ Medical Records
- First Fully Autonomous Generative AI Personalized Medical Authorizations System Reduces Care Delay
- Electronic Health Records May Be Key to Improving Patient Care, Study Finds
- AI Trained for Specific Vocal Biomarkers Could Accurately Predict Coronary Artery Disease
- First-Ever AI Test for Early Diagnosis of Alzheimer’s to Be Expanded to Diagnosis of Parkinson’s Disease
- New Self-Learning AI-Based Algorithm Reads Electrocardiograms to Spot Unseen Signs of Heart Failure
- Autonomous Robot Performs COVID-19 Nasal Swab Tests

- Statistical Tool Predicts COVID-19 Peaks Worldwide
- Wireless-Controlled Soft Neural Implant Stimulates Brain Cells
- Tiny Polymer Stent Could Treat Pediatric Urethral Strictures
- Human Torso Simulator Helps Design Brace Innovations
- 3D Bioprinting Rebuilds the Human Heart
Channels
Artificial Intelligence
view channel
AI-Powered Algorithm to Revolutionize Detection of Atrial Fibrillation
Atrial fibrillation (AFib), a condition characterized by an irregular and often rapid heart rate, is linked to increased risks of stroke and heart failure. This is because the irregular heartbeat in AFib... Read more
AI Diagnostic Tool Accurately Detects Valvular Disorders Often Missed by Doctors
Doctors generally use stethoscopes to listen for the characteristic lub-dub sounds made by heart valves opening and closing. They also listen for less prominent sounds that indicate problems with these valves.... Read moreCritical Care
view channel
Powerful AI Risk Assessment Tool Predicts Outcomes in Heart Failure Patients
Heart failure is a serious condition where the heart cannot pump sufficient blood to meet the body's needs, leading to symptoms like fatigue, weakness, and swelling in the legs and feet, and it can ultimately... Read more
Peptide-Based Hydrogels Repair Damaged Organs and Tissues On-The-Spot
Scientists have ingeniously combined biomedical expertise with nature-inspired engineering to develop a jelly-like material that holds significant promise for immediate repairs to a wide variety of damaged... Read more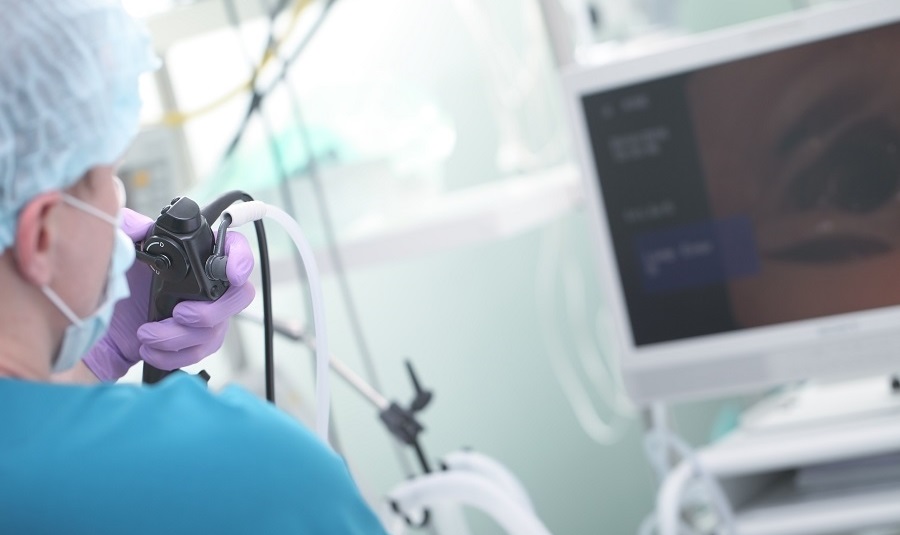
One-Hour Endoscopic Procedure Could Eliminate Need for Insulin for Type 2 Diabetes
Over 37 million Americans are diagnosed with diabetes, and more than 90% of these cases are Type 2 diabetes. This form of diabetes is most commonly seen in individuals over 45, though an increasing number... Read moreSurgical Techniques
view channel
Miniaturized Implantable Multi-Sensors Device to Monitor Vessels Health
Researchers have embarked on a project to develop a multi-sensing device that can be implanted into blood vessels like peripheral veins or arteries to monitor a range of bodily parameters and overall health status.... Read more
Tiny Robots Made Out Of Carbon Could Conduct Colonoscopy, Pelvic Exam or Blood Test
Researchers at the University of Alberta (Edmonton, AB, Canada) are developing cutting-edge robots so tiny that they are invisible to the naked eye but are capable of traveling through the human body to... Read more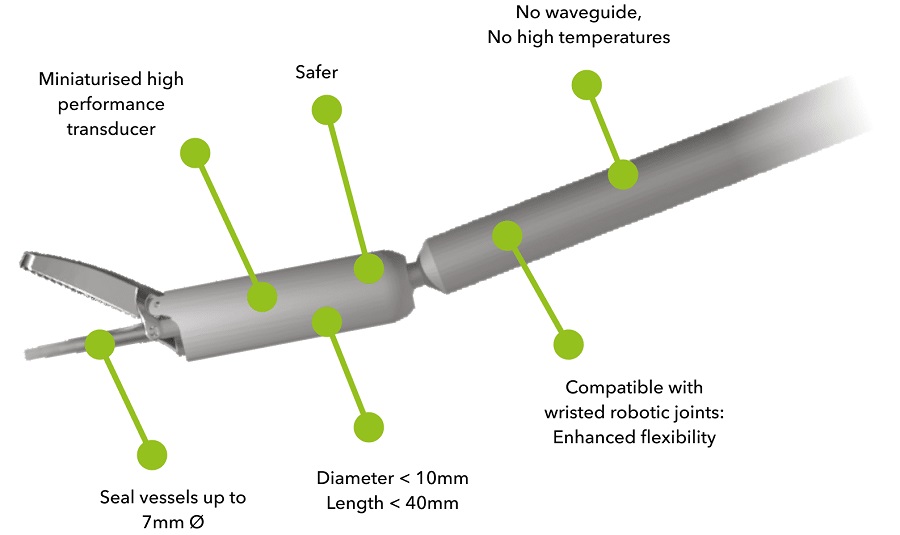
Miniaturized Ultrasonic Scalpel Enables Faster and Safer Robotic-Assisted Surgery
Robot-assisted surgery (RAS) has gained significant popularity in recent years and is now extensively used across various surgical fields such as urology, gynecology, and cardiology. These surgeries, performed... Read morePatient Care
view channelFirst-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
Reducing healthcare-acquired infections (HAIs) remains a pressing issue within global healthcare systems. In the United States alone, 1.7 million patients contract HAIs annually, leading to approximately... Read more
Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
An innovative solution has the capability to transform surgical capacity utilization by targeting the root cause of surgical block time inefficiencies. Fujitsu Limited’s (Tokyo, Japan) Surgical Capacity... Read more
Game-Changing Innovation in Surgical Instrument Sterilization Significantly Improves OR Throughput
A groundbreaking innovation enables hospitals to significantly improve instrument processing time and throughput in operating rooms (ORs) and sterile processing departments. Turbett Surgical, Inc.... Read morePoint of Care
view channel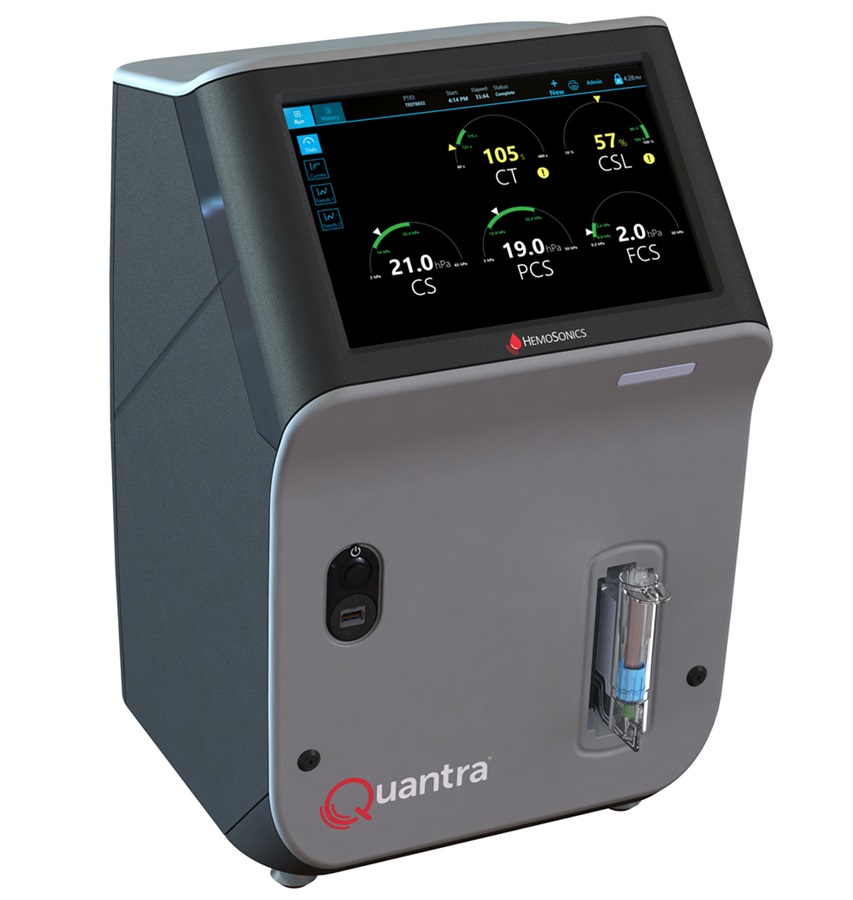
Critical Bleeding Management System to Help Hospitals Further Standardize Viscoelastic Testing
Surgical procedures are often accompanied by significant blood loss and the subsequent high likelihood of the need for allogeneic blood transfusions. These transfusions, while critical, are linked to various... Read more
Point of Care HIV Test Enables Early Infection Diagnosis for Infants
Early diagnosis and initiation of treatment are crucial for the survival of infants infected with HIV (human immunodeficiency virus). Without treatment, approximately 50% of infants who acquire HIV during... Read more
Whole Blood Rapid Test Aids Assessment of Concussion at Patient's Bedside
In the United States annually, approximately five million individuals seek emergency department care for traumatic brain injuries (TBIs), yet over half of those suspecting a concussion may never get it checked.... Read more
New Generation Glucose Hospital Meter System Ensures Accurate, Interference-Free and Safe Use
A new generation glucose hospital meter system now comes with several features that make hospital glucose testing easier and more secure while continuing to offer accuracy, freedom from interference, and... Read moreBusiness
view channel
Johnson & Johnson Acquires Cardiovascular Medical Device Company Shockwave Medical
Johnson & Johnson (New Brunswick, N.J., USA) and Shockwave Medical (Santa Clara, CA, USA) have entered into a definitive agreement under which Johnson & Johnson will acquire all of Shockwave’s... Read more